Abstract
Background
This study aimed to determine and compare the opinions of trainees and trainers attending courses using two simulation models (fresh frozen cadavers or anaesthetized pigs) and to assess trainees’ degree of insight into both the difficulty of different procedures and their operative performance in the simulated environment.
Methods
Trainers and trainees attending the training courses completed questionnaires. Performance was evaluated using the Global Assessment Score (GAS).
Results
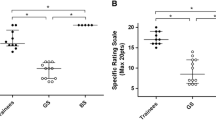
Data were collected over a 12-month period from 26 trainers and 77 trainees. The overall satisfaction was high after attendance at either course (4.50 vs. 4.49; p = 0.83). When the opinions of the trainees and trainers in cadaveric and animal courses were compared, the findings rated the animal model as superior in terms of tissue quality (3.97 vs. 3.55; p = 0.02), persistence of air leak (1.43 vs. 2.40; p < 0.001), and lack of disturbance by odor (4.24 vs. 3.41; p < 0.001). The cadaveric model provided more realistic simulation for port placement (4.02 vs. 3.11; p < 0.001) and anatomy (4.25 vs. 3.00; p < 0.001) and was perceived to be superior as a training model (4.53 vs. 3.61; p = 0.001). The trainees demonstrated good insight into procedure difficulty and their operative performance. The trainees and trainers were shown to have a good concordance of scores. The trainees were more inclined to underrate and the peers to overrate their performance.
Conclusions
Trainees appear to have a good insight into procedure difficulty and their ability. Both training models have advantages and disadvantages, but overall, the cadaveric model is perceived to have a higher fidelity and greater educational value.
Similar content being viewed by others
References
Derossis AM, Fried GM, Abrahamowicz M, Sigman HH, Barkun JS, Meakins JL (1998) Development of a model for training and evaluation of laparoscopic skills. Am J Surg 175:482–487
Miskovic D, Wyles SM, Ni M, Darzi AW, Hanna GB (2010) Mentoring and simulation in laparoscopic colorectal surgery. A systematic review. Ann Surg (in press)
Tichansky DS, Taddeucci RJ, Harper J, Madan AK (2008) Minimally invasive surgery fellows would perform a wider variety of cases in their “ideal” fellowship. Surg Endosc 22:650–654
JGt Bittner, Coverdill JE, Imam T, Deladisma AM, Edwards MA, Mellinger JD (2008) Do increased training requirements in gastrointestinal endoscopy and advanced laparoscopy necessitate a paradigm shift? A survey of program directors in surgery. J Surg Educ 65:418–430
LAPCO (2010). www.lapco.nhs.uk/about-the-programme.php. Accessed 11 July 2010
NICE. http://guidance.nice.org.uk/TA105. Accessed 11 July 2010
Giger U, Fresard I, Hafliger A, Bergmann M, Krahenbuhl L (2008) Laparoscopic training on Thiel human cadavers: a model to teach advanced laparoscopic procedures. Surg Endosc 22:901–906
Bohm B, Milsom JW (1994) Animal models as educational tools in laparoscopic colorectal surgery. Surg Endosc 8:707–713
Mutter D, Rubino F, Temporal MS, Marescaux J (2005) Surgical education and Internet-based simulation: the World Virtual University. Minim Invasive Ther Allied Technol 14:267–274
Suzuki S, Eto K, Hattori A, Yanaga K, Suzuki N (2007) Surgery simulation using patient-specific models for laparoscopic colectomy. Stud Health Technol Inform 125:464–466
Waseda M, Inaki N, Mailaender L, Buess GF (2005) An innovative trainer for surgical procedures using animal organs. Minim Invasive Ther Allied Technol 14:262–266
Ramshaw BJ, Young D, Garcha I, Shuler F, Wilson R, White JG, Duncan T, Mason E (2001) The role of multimedia interactive programs in training for laparoscopic procedures. Surg Endosc 15:21–27
Neary PC, Boyle E, Delaney CP, Senagore AJ, Keane FB, Gallagher AG (2008) Construct validation of a novel hybrid virtual-reality simulator for training and assessing laparoscopic colectomy: results from the first course for experienced senior laparoscopic surgeons. Surg Endosc 22:2301–2309
Ross HM, Simmang CL, Fleshman JW, Marcello PW (2008) Adoption of laparoscopic colectomy: results and implications of ASCRS hands-on course participation. Surg Innov 15:179–183
Pattana-arun J, Udomsawaengsup S, Sahakitrungruang C, Tansatit T, Tantiphlachiva K, Rojanasakul A (2005) The new laparoscopic proctocolectomy training (in soft cadaver). J Med Assoc Thai 88(Suppl 4):S65–S69
Lin E, Szomstein S, Addasi T, Galati-Burke L, Turner JW, Tiszenkel HI (2003) Model for teaching laparoscopic colectomy to surgical residents. Am J Surg 186:45–48
UK government (2010). www.opsi.gov.uk/si/si2008/uksi_20083067_en_1. Accessed 11 July 2010
Miskovic D, Wyles SM, Carter F, Coleman MG, Hanna GB (2010) Development, validation, and implementation of a monitoring tool for training in laparoscopic colorectal surgery in the English National Training Program. Surg Endosc. doi:10.1007/s00464-010-1329-y
Supe A, Dalvi A, Prabhu R, Kantharia C, Bhuiyan P (2005) Cadaver as a model for laparoscopic training. Indian J Gastroenterol 24:111–113
Byrne P (1994) Teaching laparoscopic surgery: practice on live animals is illegal. BMJ 308:1435
Clayden GS (1994) Teaching laparoscopic surgery: preliminary training on animals is essential. BMJ 309:342
Kirwan WO, Kaar TK, Waldron R (1991) Starting laparoscopic cholecystectomy: the pig as a training model. Ir J Med Sci 160:243–246
Royal College Surgeons England (2010). https://www.iscp.ac.uk/Default.aspx. Accessed 11 July 2010
Sidhu RS, Vikis E, Cheifetz R, Phang T (2006) Self-assessment during a 2-day laparoscopic colectomy course: can surgeons judge how well they are learning new skills? Am J Surg 191:677–681
Jamali FR, Soweid AM, Dimassi H, Bailey C, Leroy J, Marescaux J (2008) Evaluating the degree of difficulty of laparoscopic colorectal surgery. Arch Surg 143:762–767 (discussion 768)
Dochy F, Segers M, Sluijsmans D (1999) The use of self-, peer and co-assessment in higher education: a review. Stud Higher Educ 24:331–350
Acknowledgments
We acknowledge the following people from the various centers for their invaluable help, support, and facilitation of data collection during the training courses: University of Bristol (Bill Wrigley, Steve Gaze), Hamburg (Mark Thomas, Aline Ludolph), Newcastle Surgical Training Centre (Lorraine Waugh, Philip Jackson, Sian Gillinder, Jeff Potts), Nottingham University (Ryan Thachen-Cary, Giulia Miles, Paris (Fiona Morrison, Rodrigo Da Rocha Cararo), South West Laparoscopic Consortium (Elaine Cox).
Disclosures
Susannah M. Wyles, Danilo Miskovic, Zhifang Ni, Austin G. Acheson, Charles Maxwell-Armstrong, Robert Longman, Tom Cecil, Mark G. Coleman, Alan Horgan, and George B. Hanna have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was presented at the 18th International Congress of EAES, June 16–19, 2010, Geneva, Switzerland.
Rights and permissions
About this article
Cite this article
Wyles, S.M., Miskovic, D., Ni, Z. et al. Analysis of laboratory-based laparoscopic colorectal surgery workshops within the English National Training Programme. Surg Endosc 25, 1559–1566 (2011). https://doi.org/10.1007/s00464-010-1434-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-1434-y