Abstract
Introduction
Metamizole use has been limited because of its risk of agranulocytosis. However, more recent literature seems to support its safety. This prospective, randomised, double-blind study was conducted to compare the analgesic effects of intravenous metamizole or intravenous paracetamol in combination with morphine PCA during the first 24 h following total hip arthroplasty.
Materials and methods
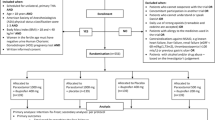
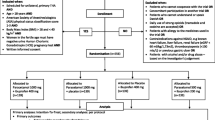
One hundred ten consecutive patients were selected for study. The two study groups were (A) metamizole, (B) paracetamol. Postoperative pain therapy was provided by Morphine PCA pump. In the first treatment group (A group), all patients received intravenous metamizole 1.5 g every 8 h during the first 24 postoperative hours. In the second treatment group (B group), all patients received intravenous paracetamol 1 g every 8 h during the first 24 postoperative hours. Postoperative pain intensity was measured 1, 2, 3, 4, 6, 8, 10, 14, 18, 22 h after the end of surgery by a VAS.
Results
Statistically significant differences in VAS pain values favoring metamizole were reported at 6-h (p = 0.038), 8-h (p = 0.036), 14-h (p = 0.011), 18-h (p < 0.001) and 22-h (p = 0.025) post-baseline. Mean cumulative pain values were 17.9 for metamizole and 30.6 for paracetamol.
Conclusions
In this study, we have also shown excellent efficacy of paracetamol and metamizole combined with opioids, but metamizole proved to be a better analgesic than paracetamol. It is also necessary to mention the financial aspect considering that intravenous paracetamol is about ten times more expensive than an equivalent analgesic doses of intravenous metamizole.


Similar content being viewed by others
References
Weis OF, Sriwatanakul K, Alloza JL, Weintraub M, Lasagna L (1983) Attitudes of patients, housestaff, and nurses toward postoperative analgesic care. Anesth Analg 62(1):70–74
Melzack R, Abbott FV, Zackon W, Mulder DS, Davis MW (1987) Pain on a surgical ward: a survey of the duration and intensity of pain and the effectiveness of medication. Pain 29(1):67–72
McQuay H, Moore A, Justins D (1997) Treating acute pain in hospital. BMJ 314(7093):1531–1535
Sinatra RS, Jahr JS, Reynolds LW, Viscusi ER, Groudine SB, Payen-Champenois C (2005) Efficacy and safety of single and repeated administration of 1 gram intravenous acetaminophen injection (paracetamol) for pain management after major orthopedic surgery. Anesthesiology 102(4):822–831
Holmer Pettersson P, Owall A, Jakobsson J (2004) Early bioavailability of paracetamol after oral or intravenous administration. Acta Anaesthesiol Scand 48(7):867–870. doi:10.1111/j.0001-5172.2004.00452.x
Flouvat B, Leneveu A, Fitoussi S, Delhotal-Landes B, Gendron A (2004) Bioequivalence study comparing a new paracetamol solution for injection and propacetamol after single intravenous infusion in healthy subjects. Int J Clin Pharmacol Ther 42(1):50–57
Sinatra RS, Jahr JS, Reynolds L, Groudine SB, Royal MA, Breitmeyer JB, Viscusi ER (2012) Intravenous acetaminophen for pain after major orthopedic surgery: an expanded analysis. Pain Pract 12(5):357–365. doi:10.1111/j.1533-2500.2011.00514.x
Macario A, Royal MA (2011) A literature review of randomized clinical trials of intravenous acetaminophen (paracetamol) for acute postoperative pain. Pain Pract 11(3):290–296. doi:10.1111/j.1533-2500.2010.00426.x
Hernandez-Palazon J, Tortosa JA, Martinez-Lage JF, Perez-Flores D (2001) Intravenous administration of propacetamol reduces morphine consumption after spinal fusion surgery. Anesth Analg 92(6):1473–1476
Peduto VA, Ballabio M, Stefanini S (1998) Efficacy of propacetamol in the treatment of postoperative pain. morphine-sparing effect in orthopedic surgery. Italian collaborative group on propacetamol. Acta Anaesthesiol Scand 42(3):293–298
Chaparro LE, Lezcano W, Alvarez HD, Joaqui W (2012) Analgesic effectiveness of dipyrone (metamizol) for postoperative pain after herniorrhaphy: a randomized, double-blind, dose-response study. Pain Pract 12(2):142–147. doi:10.1111/j.1533-2500.2011.00463.x
Fendrich Z (2000) Metamizol–a new effective analgesic with a long history. Overview of its pharmacology and clinical use. Cas Lek Cesk 139(14):440–444
Koster HT, Avis HJ, Stevens MF, Hollmann MW (2012) Metamizole in postoperative pain management. Ned Tijdschr Geneeskd 156(14):A4323
Hintze J (2008) PASS 2008. NCSS, LLC. http://www.ncss.com
Grundmann U, Wornle C, Biedler A, Kreuer S, Wrobel M, Wilhelm W (2006) The efficacy of the non-opioid analgesics parecoxib, paracetamol and metamizol for postoperative pain relief after lumbar microdiscectomy. Anesth Analg 103(1):217–222. doi:10.1213/01.ane.0000221438.08990.06 (table of contents)
Lydick E, Epstein RS, Himmelberger D, White CJ (1995) Area under the curve: a metric for patient subjective responses in episodic diseases. Qual Life Res 4(1):41–45
Saghaei M (2004) Random allocation software for parallel group randomized trials. BMC Med Res Methodol 4:26. doi:10.1186/1471-2288-4-26
Ohnesorge H, Bein B, Hanss R, Francksen H, Mayer L, Scholz J, Tonner PH (2009) Paracetamol versus metamizol in the treatment of postoperative pain after breast surgery: a randomized, controlled trial. Eur J Anaesthesiol 26(8):648–653. doi:10.1097/EJA.0b013e328329b0fd
Korkmaz Dilmen O, Tunali Y, Cakmakkaya OS, Yentur E, Tutuncu AC, Tureci E, Bahar M (2010) Efficacy of intravenous paracetamol, metamizol and lornoxicam on postoperative pain and morphine consumption after lumbar disc surgery. Eur J Anaesthesiol 27(5):428–432. doi:10.1097/EJA.0b013e32833731a4
Andrade SE, Martinez C, Walker AM (1998) Comparative safety evaluation of non-narcotic analgesics. J Clin Epidemiol 51(12):1357–1365
Maj S, Centkowski P (2004) A prospective study of the incidence of agranulocytosis and aplastic anemia associated with the oral use of metamizole sodium in Poland. Med Sci Monit 10(9):I93–I95
Backstrom M, Hagg S, Mjorndal T, Dahlqvist R (2002) Utilization pattern of metamizole in northern Sweden and risk estimates of agranulocytosis. Pharmacoepidemiol Drug Saf 11(3):239–245. doi:10.1002/pds.697
Zukowski M, Kotfis K (2009) Safety of metamizole and paracetamol for acute pain treatment. Anestezjol Intens Ter 41(3):170–175
Pergolizzi J, Boger RH, Budd K, Dahan A, Erdine S, Hans G, Kress HG, Langford R, Likar R, Raffa RB, Sacerdote P (2008) Opioids and the management of chronic severe pain in the elderly: consensus statement of an international expert panel with focus on the six clinically most often used World Health Organization step III opioids (buprenorphine, fentanyl, hydromorphone, methadone, morphine, oxycodone). Pain Pract 8(4):287–313. doi:10.1111/j.1533-2500.2008.00204.x
Lahtinen P, Kokki H, Hendolin H, Hakala T, Hynynen M (2002) Propacetamol as adjunctive treatment for postoperative pain after cardiac surgery. Anesth Analg 95(4):813–819
White PF (2005) The changing role of non-opioid analgesic techniques in the management of postoperative pain. Anesth Analg 101(5 Suppl):S5–S22
Mardani-Kivi M, Karimi Mobarakeh M, Haghighi M, Naderi-Nabi B, Sedighi-Nejad A, Hashemi-Motlagh K, Saheb-Ekhtiari K (2013) Celecoxib as a pre-emptive analgesia after arthroscopic knee surgery; a triple-blinded randomized controlled trial. Arch Orthop Trauma Surg 133(11):1561–1566. doi:10.1007/s00402-013-1852-0
Pandazi A, Kanellopoulos I, Kalimeris K, Batistaki C, Nikolakopoulos N, Matsota P, Babis GC, Kostopanagiotou G (2013) Periarticular infiltration for pain relief after total hip arthroplasty: a comparison with epidural and PCA analgesia. Arch Orthop Trauma Surg 133(11):1607–1612. doi:10.1007/s00402-013-1849-8
Scott CE, Streit J, Biant LC, Breusch SJ (2012) Periarticular infiltration in total hip replacement: effect on heterotopic ossification, analgesic requirements and outcome. Arch Orthop Trauma Surg 132(5):703–709. doi:10.1007/s00402-011-1453-8
Conflict of interest
The authors declare no conflict of interest. No financial support was received in preparation of the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Oreskovic, Z., Bicanic, G., Hrabac, P. et al. Treatment of postoperative pain after total hip arthroplasty: comparison between metamizol and paracetamol as adjunctive to opioid analgesics—prospective, double-blind, randomised study. Arch Orthop Trauma Surg (2014). https://doi.org/10.1007/s00402-014-1979-7
Received:
Published:
DOI: https://doi.org/10.1007/s00402-014-1979-7