Abstract
Purpose
Long-term outcomes of patients with T1 colorectal carcinoma (CRC) treated by endoscopic resection (ER) or surgical resection are unclear in relation to the curative criteria in the Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines. The aim of this study was to retrospectively compare the long-term outcomes among patients with T1 CRC in relation to the treatment methods.
Methods
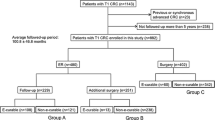
We examined 322 T1 CRC cases treated between January 1992 and August 2008 at Hiroshima University Hospital. Patients who did not meet the curative criteria in the JSCCR guidelines were defined as “non-endoscopically curable” and classified into three groups: underwent ER alone (group A: 45 patients), underwent additional surgery after ER (group B: 106 patients), and underwent surgical resection alone (group C: 92 patients).
Results
Of the 322 T1 CRC patients, 79 were categorized as endoscopically curable and 243 as non-endoscopically curable. Among the endoscopically curable T1 CRC patients, recurrence and 5-year OS rates were 0 and 94.2 %, respectively. In groups A, B, and C, recurrence rates were 4.4, 6.6, and 4.3 %, and OS rates were 85.6, 95.1, and 96.3 %, respectively (p < 0.05). Local recurrence or distant/lymph node metastasis was observed in 13 patients (group A: 2; group B: 7; group C: 4). Death due to primary CRC occurred in six patients (group B: 4; group C: 2).
Conclusion
Long-term outcomes support the curative criteria according to the JSCCR guidelines. ER for T1 CRC did not worsen clinical outcomes in cases that required additional surgical resection.



Similar content being viewed by others
References
Muto T, Oya M (2003) Recent advances in diagnosis and treatment of colorectal T1 carcinoma. Dis Colon Rectum 46:S89–S93
Kyzer S, Begin LR, Gordon PH et al (1992) The care of patients with colorectal polyps that contain invasive adenocarcinoma: endoscopic polypectomy or colectomy? Cancer 70:2044–2050
Asayama N, Oka S, Tanaka S et al (2015) Endoscopic submucosal dissection as total excisional biopsy for clinical T1 colorectal carcinoma. Digestion 91:64–69
Tanaka S, Yokota T, Saito D et al (1995) Clinicopathologic features of early rectal carcinoma and indications for endoscopic treatment. Dis Colon Rectum 38:959–963
Tanaka S, Haruma K, Teixeira CR et al (1995) Endoscopic treatment of submucosal invasive colorectal carcinoma with special reference. J Gastroenterol 30:710–717
Kobayashi H, Mochizuki H, Morita T et al (2011) Characteristics of recurrence after curative resection for T1 colorectal cancer: Japanese multicenter study. J Gastroenterol 46:203–211
Ueno H, Mochizuki H, Hashiguchi Y et al (2004) Risk factors for an adverse outcome in early invasive colorectal carcinoma. Gastroenterology 127:385–394
Nakadoi K, Tanaka S, Kanao H et al (2012) Management of T1 colorectal carcinoma with special reference to criteria for curative endoscopic resection. J Gastroenterol Hepatol 27:1057–1062
Colacchio TA, Forde KA, Scantlebury VP (1981) Endoscopic polypectomy: inadequate treatment for invasive colorectal carcinoma. Ann Surg 194:704–707
Watanabe T, Itabashi M, Shimada Y, Japanese Society for Cancer of the Colon and Rectum et al (2012) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol 17:1–29
Watanabe T, Itabashi M, Shimada Y, Japanese Society for Cancer of the Colon and Rectum et al (2015) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2014 for the treatment of colorectal cancer. Int J Clin Oncol 20:207–239
Kitajima K, Fujimori T, Fujii S et al (2004) Correlations between lymph node metastasis and depth of submucosal invasion in submucosal invasive colorectal carcinoma: a Japanese collaborative study. J Gastroenterol 39:534–543
Yoshii S, Nojima M, Nosho K et al (2014) Factors associated with risk for colorectal cancer recurrence after endoscopic resection of T1 tumors. Clin Gastroenterol Hepatol 2:292–302
Ikematsu H, Yoda Y, Matsuda T et al (2013) Long-term outcomes after resection for submucosal invasive colorectal cancers. Gastroenterology 144:551–559
Yoda Y, Ikematsu H, Matsuda T et al (2013) A large-scale multicenter study of long-term outcomes after endoscopic resection for submucosal invasive colorectal cancer. Endoscopy 45:718–724
Kikuchi R, Takano M, Takagi K et al (1995) Management of early invasive colorectal cancer. Risk of recurrence and clinical guidelines. Dis Colon Rectum 38:1286–1295
Kobayashi H, Higuchi T, Uetake H et al (2012) Resection with en bloc removal of regional lymph node after endoscopic resection for T1 colorectal cancer. Ann Surg Oncol 19:4161–4167
Iida S, Hasegawa H, Okabayashi K et al (2012) Risk factors for postoperative recurrence in patients with pathologically T1 colorectal cancer. World J Surg 3:424–430
Okabe S, Shia J, Nash G et al (2004) Lymph node metastasis in T1 adenocarcinoma of the colon and rectum. J Gastrointest Surg 8:1032–1039
Choi DH, Sohn DK, Chang HJ et al (2009) Indications for subsequent surgery after endoscopic resection of submucosally invasive colorectal carcinomas: a prospective cohort study. Dis Colon Rectum 52:438–445
Tateishi Y, Nakanishi Y, Taniguchi H et al (2010) Pathological prognostic factors predicting lymph node metastasis in submucosal invasive (T1) colorectal carcinoma. Mod Pathol 23:1068–1072
Di Gregorio C, Bonetti LR, de Gaetani C et al (2014) Clinical outcome of low- and high-risk malignant colorectal polyps: results of a population- based study and meta-analysis of the available literature. Intern Emerg Med 9:151–160
Kunihiro M, Tanaka S, Haruma K et al (2000) Electrocautery snare resection stimulates the cellular proliferation of residual colorectal tumor: an increasing gene expression related to tumor growth. Dis Colon Rectum 43:1107–1115
Kawamura YJ, Sugamata Y, Yoshino K et al (1999) Endoscopic resection for submucosally invasive colorectal cancer: is it feasible? Surg Endosc 13:224–227
Oka S, Tanaka S, Kanao H et al (2011) Mid-term prognosis after endoscopic resection for submucosal colorectal carcinoma: summary of a multicenter questionnaire survey conducted by the colorectal endoscopic resection standardization implementation working group in Japanese Society for Cancer of the Colon and Rectum. Dig Endosc 23:190–194
Rickert A, Aliyev R, Belle S et al (2014) Oncologic colorectal resection after endoscopic treatment of malignant polyps: Does endoscopy have an adverse effect on oncologic and surgical outcomes? Gastrointest Endosc 79:951–960
Ozawa S, Tanaka S, Hayashi N et al (2013) Risk factors for vertical incomplete resection in endoscopic submucosal dissection as total excisional biopsy for submucosal invasive colorectal carcinoma. Int J Colorectal Dis 28:1247–1256
Matsumoto A, Tanaka S, Oba S et al (2010) Outcome of endoscopic submucosal dissection for colorectal tumors accompanied by fibrosis. Scand J Gastroenterol 45:1329–1337
Terasaki M, Tanaka S, Shigita K et al (2014) Risk factors for delayed bleeding after endoscopic submucosal dissection for colorectal neoplasms. Int J Colorectal Dis 29:877–882
Tanaka S, Tamegai Y, Tsuda S et al (2010) Multicenter questionnaire survey on the current situation of colorectal endoscopic submucosal dissection in Japan. Dig Endosc 22:S2–8
Tanaka S, Kaltenbach T, Chayama K et al (2006) High-magnification colonoscopy (with videos). Gastrointest Endosc 64:604–613
Kanao H, Tanaka S, Oka S et al (2009) Narrow-band imaging magnification predicts the histology and invasion depth of colorectal tumors. Gastrointest Endosc 69:631–636
Acknowledgments
The authors thank Professor Fumio Shimamoto at the Faculty of Human Culture and Science, Prefectural University of Hiroshima for advice on diagnosis of T1 CRC according to pathology.
Author contributions
NA, SO, and ST contributed to the study concept and design, statistical analysis and interpretation of data, and drafting of the manuscript. NA, YN, YT, KS, NH, HE, TH, and HO contributed to the acquisition of data. KA gave advice on diagnosis of T1 CRC according to pathology. All the authors participated in the critical revision of the article for important intellectual content and final approval of the article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study protocol was approved by the Ethics Committee of Hiroshima University and was in keeping with the guidelines of the relevant government agency. All patients gave their informed consent before all procedures.
Conflict of interest
The authors declare that they have no competing interests.
Sources of funding
None
Additional information
Category
Colorectal neoplasia.
Rights and permissions
About this article
Cite this article
Asayama, N., Oka, S., Tanaka, S. et al. Long-term outcomes after treatment for T1 colorectal carcinoma. Int J Colorectal Dis 31, 571–578 (2016). https://doi.org/10.1007/s00384-015-2473-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-015-2473-6