Abstract
Purpose
To compare the safety and efficacy of PAE for the treatment of benign prostatic hyperplasia (BPH) in men ≥75 years, who we defined as elderly, to those <75 years.
Methods
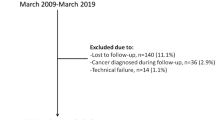
A total of 157 patients diagnosed with lower urinary tract symptoms (LUTS) due to BPH underwent PAE. Group A (n = 52) included patients ≥75 years, and group B (n = 105) included patients <75 years. Follow-up was performed using the International Prostate Symptoms Score (IPSS), quality of life (QoL), peak urinary flow rate (Q max), post-void residual volume (PVR), the International Index of Erectile Function short form (IIEF-5), prostatic-specific antigen (PSA), and prostate volume (PV), at 1, 3, 6, and every 6 months thereafter.
Results
More coexistent systemic diseases were identified in group A than in group B (P < 0.05). Technical success rate of PAE was 90.4 % in group A and 95.2 % in group B (P = 0.06). A total of 147 patients had completed the follow-up with a mean of 20 months. Compared with the baseline, there were significant improvements in IPSS, QoL, Q max, PV, PVR, and PSA in both groups after PAE. There were no significant differences in the changes of IPSS, Q max, PVR, PSA, and IIEF-5 between groups after PAE. No major complications were noted.
Conclusion
PAE could be used as an effective, safe, and well tolerable method in the treatment of elderly symptomatic BPH patients, similarly to younger patients, and it may play an important role in patients in whom medical therapy has failed, who are at high surgical and anesthetic risk or who refuse the standard surgical therapy.




Similar content being viewed by others
References
Pisco J, Campos Pinheiro L, Bilhim T, Duarte M, Rio Tinto H, Fernandes L, Vaz Santos V, Oliveira AG (2013) Prostatic arterial embolization for benign prostatic hyperplasia: short- and intermediate-term results. Radiology 266(2):668–677
Carnevale FC, da Motta-Leal-Filho JM, Antunes AA, Baroni RH, Marcelino AS, Cerri LM, Yoshinaga EM, Cerri GG, Srougi M (2013) Quality of life and clinical symptom improvement support prostatic artery embolization for patients with acute urinary retention caused by benign prostatic hyperplasia. J Vasc Interv Radiol 24(4):535–542
Bagla S, Martin CP, van Breda A, Sheridan MJ, Sterling KM, Papadouris D, Rholl KS, Smirniotopoulos JB, van Breda A (2014) Early results from a United States trial of prostatic artery embolization in the treatment of benign prostatic hyperplasia. J Vasc Interv Radiol 25(1):47–52
Gao YA, Huang Y, Zhang R, Yang YD, Zhang Q, Hou M, Wang Y (2014) Benign prostatic hyperplasia: prostatic arterial embolization versus transurethral resection of the prostate—a prospective, randomized, and controlled clinical trial. Radiology 270(3):920–928
Abt D, Mordasini L, Hechelhammer L, Kessler TM, Schmid HP, Engeler DS (2014) Prostatic artery embolization versus conventional TUR-P in the treatment of benign prostatic hyperplasia: protocol for a prospective randomized non-inferiority trial. BMC Urol 14:94
Kurbatov D, Russo GI, Lepetukhin A, Dubsky S, Sitkin I, Morgia G, Rozhivanov R, Cimino S, Sansalone S (2014) Prostatic artery embolization for prostate volume greater than 80 cm3: results from a single-center prospective study. Urology 84(2):400–404
Jones P, Rai BP, Nair R, Somani BK (2015) Current status of prostate artery embolization for lower urinary tract symptoms: review of world literature. Urology 86(4):676–681
Russo GI, Kurbatov D, Sansalone S, Lepetukhin A, Dubsky S, Sitkin I, Salamone C, Fiorino L, Rozhivanov R, Cimino S, Morgia G (2015) Prostatic arterial embolization vs open prostatectomy: a 1-year matched-pair analysis of functional outcomes and morbidities. Urology 86(2):343–348
Wang MQ, Guo LP, Zhang GD, Yuan K, Li K, Duan F, Yan JY, Wang Y, Kang HY, Wang ZJ (2015) Prostatic arterial embolization for the treatment of lower urinary tract symptoms due to large (>80 mL) benign prostatic hyperplasia: results of midterm follow-up from Chinese population. BMC Urol 15:33
Mitropoulos D, Artibani W, Graefen M, Remzi M, Rouprêt M, Truss M, European Association of Urology Guidelines Panel (2012) Reporting and grading of complications after urologic surgical procedures: an ad hoc EAU guidelines panel assessment and recommendations. Eur Urol 61(2):341–349
Carnevale FC, Antunes AA (2013) Prostatic artery embolization for enlarged prostates due to benign prostatic hyperplasia. How I do it. Cardiovasc Intervent Radiol 36(6):1452–1463
Bilhim T, Pisco J, Rio Tinto H, Fernandes L, Campos Pinheiro L, Duarte M, Pereira JA, Oliveira AG, O’Neill J (2013) Unilateral versus bilateral prostatic arterial embolization for lower urinary tract symptoms in patients with prostate enlargement. Cardiovasc Intervent Radiol 36(2):403–411
Pisco JM, Rio-Tinto H, Campos-Pinheiro L, Bilhim T (2013) Embolisation of prostatic arteries as treatment of moderate to severe lower urinary symptoms (LUTS) secondary to benign hyperplasia: results of short- and mid-term follow-up. Eur Radiol 23(9):2561–2572
McWilliams JP, Kuo MD, Rose SC, Bagla S, Caplin DM, Cohen EI, Faintuch S, Spies JB, Saad WE, Nikolic B, Society of Interventional Radiology (2014) Society of interventional radiology position statement: prostate artery embolization for treatment of benign disease of the prostate. J Vasc Interv Radiol 25(9):1349–1351
Grosso M, Balderi A, Arnò M, Sortino D, Antonietti A, Pedrazzini F, Giovinazzo G, Vinay C, Maugeri O, Ambruosi C, Arena G (2015) Prostatic artery embolization in benign prostatic hyperplasia: preliminary results in 13 patients. Radiol Med 120(4):361–368
Wang M, Guo L, Duan F, Yuan K, Zhang G, Li K, Yan J, Wang Y, Kang H, Wang Z (2015) Prostatic arterial embolization for the treatment of lower urinary tract symptoms as a result of large benign prostatic hyperplasia: a prospective single-center investigation. Int J Urol 22(8):766–772
Antunes AA, Carnevale FC, da Motta Leal Filho JM, Yoshinaga EM, Cerri LM, Baroni RH, Marcelino AS, Cerri GG, Srougi M (2013) Clinical, laboratorial, and urodynamic findings of prostatic artery embolization for the treatment of urinary retention related to benign prostatic hyperplasia. A prospective single-center pilot study. Cardiovasc Intervent Radiol 36(4):978–986
Lebdai S, Delongchamps NB, Sapoval M, Robert G, Amouyal G, Thiounn N, Karsenty G, Ruffion A, de La Taille A, Descazeaud A, Mathieu R (2015) Early results and complications of prostatic arterial embolization for benign prostatic hyperplasia. World J Urol [Epub ahead of print, PMID: 26276151]. doi: 10.1007/s00345-015-1665-6
Acknowledgments
This work was supported by grants from the National Scientific Foundation Committee of China (No. 81471769), the central health research project (2013BJ09), and Chinese PLA Scientific Foundation of the Twelve-Five Programme (BWS11J028).
Funding
This work was supported by grants from the National Scientific Foundation Committee of China (No. 81471769), the central health research project (2013BJ09), and Chinese PLA Scientific Foundation of the Twelve-Five Programme (BWS11J028).
Authors’ contributions
Wang MQ and Wang Y involved in project development and wrote the manuscript. Wang Y and Yuan K involved in data collection. Zhang GD and Duan F involved in the literature research. Wang MQ and Yan JY involved in data analysis and statistical analysis. Wang MQ and Kai Li reviewed the manuscript. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have declared that no competing interests exist.
Ethical statement
This study was approved by the hospital ethics committee and has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Additional information
M. Q. Wang is the article guarantor. M. Q. Wang, Y. Wang, and J. Y. Yan contributed equally to this work and are joint first authors on this article.
Rights and permissions
About this article
Cite this article
Wang, M.Q., Wang, Y., Yan, J.Y. et al. Prostatic artery embolization for the treatment of symptomatic benign prostatic hyperplasia in men ≥75 years: a prospective single-center study. World J Urol 34, 1275–1283 (2016). https://doi.org/10.1007/s00345-016-1771-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-016-1771-0