Abstract
Purpose
Malignant pleural mesothelioma (MPM) has a dismal prognosis. Treatment results may be improved by biomarker-directed therapy. We investigated the baseline expression and impact on outcome of predictive biomarkers ERCC1, BRCA1, and class III β-tubulin in a cohort of MPM patients treated with cisplatin–vinorelbine. We further explored the possibility of combining markers into a treatment-response profile to increase the predictive power.
Methods
Formalin-fixed paraffin-embedded tumor specimens from 54 MPM patients included in a phase II trial were evaluated for ERCC1, BRCA1, and class III β-tubulin by immunohistochemistry (IHC). Immunostaining was quantified by an H-score and dichotomized according to upper quartile values. The ERCC1- and class III β-tubulin-status classified patients as treatment resistant (ERCC1 positive + class III β-tubulin positive) or treatment responsive (ERCC1 negative + class III β-tubulin negative). The remaining marker combinations were considered inconclusive.
Results
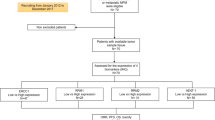
Fifty patients had tumor tissue available for IHC. Eleven had a responsive profile, and nine had a resistant profile. Thirty patients had an inconclusive profile. Median progression-free survival (PFS) was 6.7 months in the treatment-resistant group, 15.3 months in the treatment-responsive group, and 8.1 months in the inconclusive group (log-rank p = 0.03). Multivariate analysis revealed that treatment-resistant patients had a decreased PFS and overall survival (OS) compared with the treatment-responsive patients (HR 6.45, CI 95 % [2.02–20.64] p = 0.002 and HR 4.64, CI 95 % [1.56–13.79], p = 0.006, respectively). BRCA1 status was associated with neither PFS nor OS.
Conclusion
Combined negative ERCC1 and class III β-tubulin immunostaining is associated with significantly prolonged PFS and OS in MPM patients receiving cisplatin–vinorelbine therapy.



Similar content being viewed by others
References
Churg A, Roggli V, Galateau-Salle F et al (2004) Mesothelioma. In: Travis WD, Brambilla E, Müller-Hermelink HK et al (eds) Pathology and genetics of tumours of the lung, pleura, thymus and heart. IARC press, Lyon, pp 128–136
Sorensen JB (2008) Current concepts in chemotherapy for malignant pleural mesothelioma. Clin Respir J 2:74–79
Carlson RW, Allred DC, Anderson BO et al (2009) Breast cancer. Clinical practice guidelines in oncology. J Natl Compr Canc Netw 7:122–192
Gridelli C, De MF, Di MM et al (2011) Gefitinib as first-line treatment for patients with advanced non-small-cell lung cancer with activating epidermal growth factor receptor mutation: review of the evidence. Lung Cancer 71:249–257
Slamon DJ, Godolphin W, Jones LA et al (1989) Studies of the HER-2/neu proto-oncogene in human breast and ovarian cancer. Science 244:707–712
Marchetti A, Martella C, Felicioni L et al (2005) EGFR mutations in non-small-cell lung cancer: analysis of a large series of cases and development of a rapid and sensitive method for diagnostic screening with potential implications on pharmacologic treatment. J Clin Oncol 23:857–865
Siddik ZH (2003) Cisplatin: mode of cytotoxic action and molecular basis of resistance. Oncogene 22:7265–7279
Martin LP, Hamilton TC, Schilder RJ (2008) Platinum resistance: the role of DNA repair pathways. Clin Cancer Res 14:1291–1295
Vilmar AC, Santoni-Rugiu E, Sorensen JB (2010) ERCC1 and histopathology in advanced NSCLC patients randomized in a large multicenter phase III trial. Ann Oncol 21:1817–1824
Olaussen KA, Dunant A, Fouret P et al (2006) DNA repair by ERCC1 in non-small-cell lung cancer and cisplatin-based adjuvant chemotherapy. N Engl J Med 355:983–991
Steffensen KD, Waldstrom M, Jakobsen A (2009) The relationship of platinum resistance and ERCC1 protein expression in epithelial ovarian cancer. Int J Gynecol Cancer 19:820–825
Kim KH, Do IG, Kim HS et al (2010) Excision repair cross-complementation group 1 (ERCC1) expression in advanced urothelial carcinoma patients receiving cisplatin-based chemotherapy. APMIS 118:941–948
Kennedy RD, Quinn JE, Mullan PB et al (2004) The role of BRCA1 in the cellular response to chemotherapy. J Natl Cancer Inst 96:1659–1668
Cass I, Baldwin RL, Varkey T et al (2003) Improved survival in women with BRCA-associated ovarian carcinoma. Cancer 97:2187–2195
Taron M, Rosell R, Felip E et al (2004) BRCA1 mRNA expression levels as an indicator of chemoresistance in lung cancer. Hum Mol Genet 13:2443–2449
Tassone P, Blotta S, Palmieri C et al (2005) Differential sensitivity of BRCA1-mutated HCC1937 human breast cancer cells to microtubule-interfering agents. Int J Oncol 26:1257–1263
Stordal B, Davey R (2009) A systematic review of genes involved in the inverse resistance relationship between cisplatin and paclitaxel chemotherapy: role of BRCA1. Curr Cancer Drug Targets 9:354–365
Quinn JE, Kennedy RD, Mullan PB et al (2003) BRCA1 functions as a differential modulator of chemotherapy-induced apoptosis. Cancer Res 63:6221–6228
Mullan PB, Gorski JJ, Harkin DP (2006) BRCA1–a good predictive marker of drug sensitivity in breast cancer treatment? Biochim Biophys Acta 1766:205–216
Kavallaris M (2010) Microtubules and resistance to tubulin-binding agents. Nat Rev Cancer 10:194–204
Gan PP, Pasquier E, Kavallaris M (2007) Class III beta-tubulin mediates sensitivity to chemotherapeutic drugs in non small cell lung cancer. Cancer Res 67:9356–9363
Seve P, Dumontet C (2008) Is class III beta-tubulin a predictive factor in patients receiving tubulin-binding agents? Lancet Oncol 9:168–175
Seve P, Isaac S, Tredan O et al (2005) Expression of class III {beta}-tubulin is predictive of patient outcome in patients with non-small cell lung cancer receiving vinorelbine-based chemotherapy. Clin Cancer Res 11:5481–5486
Seve P, Mackey J, Isaac S et al (2005) Class III beta-tubulin expression in tumor cells predicts response and outcome in patients with non-small cell lung cancer receiving paclitaxel. Mol Cancer Ther 4:2001–2007
Vilmar AC, Santoni-Rugiu E, Sorensen JB (2011) Class III {beta}-tubulin in advanced NSCLC of adenocarcinoma subtype predicts superior outcome in a randomized trial. Clin Cancer Res 17:5205–5214
Tommasi S, Mangia A, Lacalamita R et al (2007) Cytoskeleton and paclitaxel sensitivity in breast cancer: the role of beta-tubulins. Int J Cancer 120:2078–2085
Seve P, Reiman T, Lai R et al (2007) Class III beta-tubulin is a marker of paclitaxel resistance in carcinomas of unknown primary site. Cancer Chemother Pharmacol 60:27–34
Zimling ZG, Sorensen JB, Gerds TA et al (2012) Low ERCC1 expression in malignant pleural mesotheliomas treated with cisplatin and vinorelbine predicts prolonged progression-free survival. J Thorac Oncol 7:249–256
Sorensen JB, Frank H, Palshof T (2008) Cisplatin and vinorelbine first-line chemotherapy in non-resectable malignant pleural mesothelioma. Br J Cancer 99:44–50
Rusch VW (1996) A proposed new international TNM staging system for malignant pleural mesothelioma from the International Mesothelioma Interest Group. Lung Cancer 14:1–12
Byrne MJ, Nowak AK (2004) Modified RECIST criteria for assessment of response in malignant pleural mesothelioma. Ann Oncol 15:257–260
Francart J, Legrand C, Sylvester R et al (2006) Progression-free survival rate as primary end point for phase II cancer clinical trials: application to mesothelioma—The EORTC Lung Cancer Group. J Clin Oncol 24:3007–3012
Miki Y, Swensen J, Shattuck-Eidens D et al (1994) A strong candidate for the breast and ovarian cancer susceptibility gene BRCA1. Science 266:66–71
Marquis ST, Rajan JV, Wynshaw-Boris A et al (1995) The developmental pattern of Brca1 expression implies a role in differentiation of the breast and other tissues. Nat Genet 11:17–26
Yoshikawa K, Honda K, Inamoto T et al (1999) Reduction of BRCA1 protein expression in Japanese sporadic breast carcinomas and its frequent loss in BRCA1-associated cases. Clin Cancer Res 5:1249–1261
Cicchillitti L, Penci R, Di MM et al (2008) Proteomic characterization of cytoskeletal and mitochondrial class III beta-tubulin. Mol Cancer Ther 7:2070–2079
D’Addario G, Fruh M, Reck M et al (2010) Metastatic non-small-cell lung cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 21(Suppl 5):v116–v119
Ohishi Y, Oda Y, Basaki Y et al (2007) Expression of beta-tubulin isotypes in human primary ovarian carcinoma. Gynecol Oncol 105:586–592
Reiman T, Lai R, Veillard AS et al (2012) Cross-validation study of class III beta-tubulin as a predictive marker for benefit from adjuvant chemotherapy in resected non-small-cell lung cancer: analysis of four randomized trials. Ann Oncol 23:86–93
Ikeda S, Takabe K, Suzuki K (2009) Expression of ERCC1 and class IIIbeta tubulin for predicting effect of carboplatin/paclitaxel in patients with advanced inoperable non-small cell lung cancer. Pathol Int 59:863–867
Azuma K, Sasada T, Kawahara A et al (2009) Expression of ERCC1 and class III beta-tubulin in non-small cell lung cancer patients treated with carboplatin and paclitaxel. Lung Cancer 64:326–333
Steele JP, Shamash J, Evans MT et al (2000) Phase II study of vinorelbine in patients with malignant pleural mesothelioma. J Clin Oncol 18:3912–3917
Camp RL, Chung GG, Rimm DL (2002) Automated subcellular localization and quantification of protein expression in tissue microarrays. Nat Med 8:1323–1327
Gustavson MD, Bourke-Martin B, Reilly D et al (2009) Standardization of HER2 immunohistochemistry in breast cancer by automated quantitative analysis. Arch Pathol Lab Med 133:1413–1419
Acknowledgments
Thanks to Lone Svendstrup, Anne Jørgensen, and Margit Bæksted for excellent technical assistance. Thanks to N.Z. Sroczynski, TopoTarget, Copenhagen, Denmark, for the kind donation of the A2780 cell pellet. Thanks to Heidi R. Hudlebusch, BRIC, Copenhagen Biocenter, Denmark, for kindly providing the SH-SY5Y cell pellet. This work was funded by The Danish Cancer Society, the Harboe foundation, the Danielsen foundation, and the Danish Lung Association.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zimling, Z.G., Sørensen, J.B., Gerds, T.A. et al. A biomarker profile for predicting efficacy of cisplatin–vinorelbine therapy in malignant pleural mesothelioma. Cancer Chemother Pharmacol 70, 743–754 (2012). https://doi.org/10.1007/s00280-012-1965-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-012-1965-0