Abstract
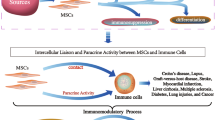
In addition to being multi-potent, mesenchymal stem cells (MSCs) possess immunomodulatory functions that have been investigated as potential treatments in various immune disorders. MSCs can robustly interact with cells of the innate and adaptive immune systems, either through direct cell–cell contact or through their secretome. In this review, we discuss current findings regarding the interplay between MSCs and different immune cell subsets. We also draw attention to the mechanisms involved.



Similar content being viewed by others
Abbreviations
- MSCs:
-
Mesenchymal stem cells;
- Sca-1:
-
Stem cell antigen-1
- ESCs:
-
Embryonic stem cells
- iPSCs:
-
Induced pluripotent stem cells
- Th:
-
T-helper
- TGF-β:
-
Transforming growth factor beta
- HGF:
-
Hepatocyte growth factor
- IFN:
-
Interferon
- Treg:
-
Regulatory T cell
- NK:
-
Natural killer
- DC:
-
Dendritic cell
- EAE:
-
Experimental autoimmune encephalomyelitis
- SLE:
-
Systemic lupus erythematosus
- GVHD:
-
Graft-versus-host disease
- TNF:
-
Tumor necrosis factor
- IL:
-
Interleukin
- iNOS:
-
Nitric oxide synthase
- COX:
-
Cyclooxygenase
- NO:
-
Nitric oxide
- PGE2:
-
Prostaglandin E2
- CXCR3:
-
CXC chemokine receptor3
- CCR5:
-
C-C chemokine receptor type 5
- ICAM-1:
-
Intercellular adhesion molecule 1
- VCAM-1:
-
Vascular cell adhesion molecule 1
- IDO:
-
Indoleamine 2,3-dioxygenase
- HLA-G5:
-
Human leukocyte antigen class I molecule G5
- EV:
-
Extracellular vesicle
- TSG6:
-
Tumor necrosis factor-induced protein 6
- Breg:
-
Regulatory B cell
- STAT3:
-
Signal transducer and activator of transcription 3
- Blimp1:
-
B lymphocyte-induced maturation protein 1
- IL-1Ra:
-
IL-1 receptor antagonist
- APC:
-
Antigen-presenting cell
- MIF:
-
Macrophage migration inhibitory factor.
References
Hass R, Kasper C, Bohm S, Jacobs R (2011) Different populations and sources of human mesenchymal stem cells (MSC): a comparison of adult and neonatal tissue-derived MSC. Cell Commun Signal 9:12. doi:10.1186/1478-811X-9-12
Elahi KC, Klein G, Avci-Adali M, Sievert KD, MacNeil S, Aicher WK (2016) Human mesenchymal stromal cells from different sources diverge in their expression of cell surface proteins and display distinct differentiation patterns. Stem Cells Int 2016:5646384. doi:10.1155/2016/5646384
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, Moorman MA, Simonetti DW, Craig S, Marshak DR (1999) Multilineage potential of adult human mesenchymal stem cells. Science 284(5411):143–147
Le Blanc K, Mougiakakos D (2012) Multipotent mesenchymal stromal cells and the innate immune system. Nat Rev Immunol 12(5):383–396. doi:10.1038/nri3209
Jiang Y, Jahagirdar BN, Reinhardt RL, Schwartz RE, Keene CD, Ortiz-Gonzalez XR, Reyes M, Lenvik T, Lund T, Blackstad M, Du J, Aldrich S, Lisberg A, Low WC, Largaespada DA, Verfaillie CM (2002) Pluripotency of mesenchymal stem cells derived from adult marrow. Nature 418(6893):41–49. doi:10.1038/nature00870
Keating A (2012) Mesenchymal stromal cells: new directions. Cell stem cell 10(6):709–716. doi:10.1016/j.stem.2012.05.015
Horwitz EM, Le Blanc K, Dominici M, Mueller I, Slaper-Cortenbach I, Marini FC, Deans RJ, Krause DS, Keating A, International Society for Cellular T (2005) Clarification of the nomenclature for MSC: the International Society for Cellular Therapy position statement. Cytotherapy 7(5):393–395. doi:10.1080/14653240500319234
Lv FJ, Tuan RS, Cheung KM, Leung VY (2014) Concise review: the surface markers and identity of human mesenchymal stem cells. Stem Cells 32(6):1408–1419. doi:10.1002/stem.1681
Houlihan DD, Mabuchi Y, Morikawa S, Niibe K, Araki D, Suzuki S, Okano H, Matsuzaki Y (2012) Isolation of mouse mesenchymal stem cells on the basis of expression of Sca-1 and PDGFR-alpha. Nat Protoc 7(12):2103–2111. doi:10.1038/nprot.2012.125
Gutierrez-Aranda I, Ramos-Mejia V, Bueno C, Munoz-Lopez M, Real PJ, Macia A, Sanchez L, Ligero G, Garcia-Parez JL, Menendez P (2010) Human induced pluripotent stem cells develop teratoma more efficiently and faster than human embryonic stem cells regardless the site of injection. Stem Cells 28(9):1568–1570. doi:10.1002/stem.471
Ben-David U, Benvenisty N (2011) The tumorigenicity of human embryonic and induced pluripotent stem cells. Nature Rev Cancer 11(4):268–277. doi:10.1038/nrc3034
Lo B, Parham L (2009) Ethical issues in stem cell research. Endocr Rev 30(3):204–213. doi:10.1210/er.2008-0031
Cho KA, Ju SY, Cho SJ, Jung YJ, Woo SY, Seoh JY, Han HS, Ryu KH (2009) Mesenchymal stem cells showed the highest potential for the regeneration of injured liver tissue compared with other subpopulations of the bone marrow. Cell Biol Int 33(7):772–777. doi:10.1016/j.cellbi.2009.04.023
Qian H, Yang H, Xui WR, Yan YM, Chen QL, Zhu W, Cao HL, Yin Q, Zhou HX, Mao F, Chen YC (2008) Bone marrow mesenchymal stem cells ameliorate rat acute renal failure by differentiation into renal tubular epithelial-like cells. Int J Mol Med 22(3):325–332. doi:10.3892/ijmm_00000026
Rose RA, Jiang H, Wang X, Helke S, Tsoporis JN, Gong N, Keating SC, Parker TG, Backx PH, Keating A (2008) Bone marrow-derived mesenchymal stromal cells express cardiac-specific markers, retain the stromal phenotype, and do not become functional cardiomyocytes in vitro. Stem Cells 26(11):2884–2892. doi:10.1634/stemcells.2008-0329
Han F, Wang CY, Yang L, Zhan SD, Zhang M, Tian K (2012) Contribution of murine bone marrow mesenchymal stem cells to pancreas regeneration after partial pancreatectomy in mice. Cell Biol Int 36(9):823–831. doi:10.1042/CBI20110680
Wang Y, Chen X, Cao W, Shi Y (2014) Plasticity of mesenchymal stem cells in immunomodulation: pathological and therapeutic implications. Nat Immunol 15(11):1009–1016. doi:10.1038/ni.3002
Munir H, McGettrick HM (2015) Mesenchymal stem cell therapy for autoimmune disease: risks and rewards. Stem Cells Dev 24(18):2091–2100. doi:10.1089/scd.2015.0008
Frenette PS, Pinho S, Lucas D, Scheiermann C (2013) Mesenchymal stem cell: keystone of the hematopoietic stem cell niche and a stepping-stone for regenerative medicine. Annu Rev Immunol 31:285–316. doi:10.1146/annurev-immunol-032712-095919
Koch U, Radtke F (2011) Mechanisms of T cell development and transformation. Annu Rev Cell Dev Biol 27:539–562. doi:10.1146/annurev-cellbio-092910-154008
Mueller DL, Jenkins MK, Schwartz RH (1989) Clonal expansion versus functional clonal inactivation: a costimulatory signalling pathway determines the outcome of T cell antigen receptor occupancy. Annu Rev Immunol 7:445–480. doi:10.1146/annurev.iy.07.040189.002305
June CH, Ledbetter JA, Gillespie MM, Lindsten T, Thompson CB (1987) T-cell proliferation involving the Cd28 pathway is associated with cyclosporine-resistant interleukin-2 gene-expression. Mol Cell Biol 7(12):4472–4481
O’Garra A (1998) Cytokines induce the development of functionally heterogeneous T helper cell subsets. Immunity 8(3):275–283
Soroosh P, Doherty TA (2009) Th9 and allergic disease. Immunology 127(4):450–458. doi:10.1111/j.1365-2567.2009.03114.x
Langrish CL, Chen Y, Blumenschein WM, Mattson J, Basham B, Sedgwick JD, McClanahan T, Kastelein RA, Cua DJ (2005) IL-23 drives a pathogenic T cell population that induces autoimmune inflammation. J Exp Med 201(2):233–240. doi:10.1084/jem.20041257
Hori S, Nomura T, Sakaguchi S (2003) Control of regulatory T cell development by the transcription factor Foxp3. Science 299(5609):1057–1061. doi:10.1126/science.1079490
Kaech SM, Cui WG (2012) Transcriptional control of effector and memory CD8(+) T cell differentiation. Nat Rev Immunol 12(11):749–761. doi:10.1038/nri3307
Dimeloe S, Burgener AV, Grahlert J, Hess C (2016) T-cell metabolism governing activation, proliferation and differentiation; a modular view. Immunology. doi:10.1111/imm.12655
Bartholomew A, Sturgeon C, Siatskas M, Ferrer K, McIntosh K, Patil S, Hardy W, Devine S, Ucker D, Deans R, Moseley A, Hoffman R (2002) Mesenchymal stem cells suppress lymphocyte proliferation in vitro and prolong skin graft survival in vivo. Exp Hematol 30(1):42–48
Di Nicola M, Carlo-Stella C, Magni M, Milanesi M, Longoni PD, Matteucci P, Grisanti S, Gianni AM (2002) Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli. Blood 99(10):3838–3843
Glennie S, Soeiro I, Dyson PJ, Lam EW, Dazzi F (2005) Bone marrow mesenchymal stem cells induce division arrest anergy of activated T cells. Blood 105(7):2821–2827. doi:10.1182/blood-2004-09-3696
Plumas J, Chaperot L, Richard MJ, Molens JP, Bensa JC, Favrot MC (2005) Mesenchymal stem cells induce apoptosis of activated T cells. Leukemia 19(9):1597–1604. doi:10.1038/sj.leu.2403871
Akiyama K, Chen C, Wang D, Xu X, Qu C, Yamaza T, Cai T, Chen W, Sun L, Shi S (2012) Mesenchymal-stem-cell-induced immunoregulation involves FAS-ligand-/FAS-mediated T cell apoptosis. Cell Stem Cell 10(5):544–555. doi:10.1016/j.stem.2012.03.007
Luz-Crawford P, Kurte M, Bravo-Alegria J, Contreras R, Nova-Lamperti E, Tejedor G, Noel D, Jorgensen C, Figueroa F, Djouad F, Carrion F (2013) Mesenchymal stem cells generate a CD4+CD25+Foxp3+ regulatory T cell population during the differentiation process of Th1 and Th17 cells. Stem Cell Res Ther 4(3):65. doi:10.1186/scrt216
Selmani Z, Naji A, Zidi I, Favier B, Gaiffe E, Obert L, Borg C, Saas P, Tiberghien P, Rouas-Freiss N, Carosella ED, Deschaseaux F (2008) Human leukocyte antigen-G5 secretion by human mesenchymal stem cells is required to suppress T lymphocyte and natural killer function and to induce CD4(+)CD25(high)FOXP3(+) regulatory T cells. Stem Cells 26(1):212–222. doi:10.1634/stemcells.2007-0554
Consentius C, Akyuz L, Schmidt-Lucke JA, Tschope C, Pinzur L, Ofir R, Reinke P, Volk HD, Juelke K (2015) Mesenchymal stromal cells prevent allostimulation in vivo and control checkpoints of Th1 priming: migration of human DC to lymph nodes and NK cell activation. Stem Cells 33(10):3087–3099. doi:10.1002/stem.2104
Lopez-Santalla M, Mancheno-Corvo P, Menta R, Lopez-Belmonte J, DelaRosa O, Bueren JA, Dalemans W, Lombardo E, Garin MI (2015) Human adipose-derived mesenchymal stem cells modulate experimental autoimmune arthritis by modifying early adaptive T cell responses. Stem Cells 33(12):3493–3503. doi:10.1002/stem.2113
Tasso R, Ilengo C, Quarto R, Cancedda R, Caspi RR, Pennesi G (2012) Mesenchymal stem cells induce functionally active T-regulatory lymphocytes in a paracrine fashion and ameliorate experimental autoimmune uveitis. Invest Ophthalmol Vis Sci 53(2):786–793. doi:10.1167/iovs.11-8211
Hsu WT, Lin CH, Chiang BL, Jui HY, Wu KK, Lee CM (2013) Prostaglandin E2 potentiates mesenchymal stem cell-induced IL-10+ IFN-gamma+ CD4+ regulatory T cells to control transplant arteriosclerosis. J Immunol 190(5):2372–2380. doi:10.4049/jimmunol.1202996
Ryu KH, Kim SY, Kim YR, Woo SY, Sung SH, Kim HS, Jung SC, Jo I, Park JW (2014) Tonsil-derived mesenchymal stem cells alleviate concanavalin A-induced acute liver injury. Exp Cell Res 326(1):143–154. doi:10.1016/j.yexcr.2014.06.007
Sun L, Akiyama K, Zhang H, Yamaza T, Hou Y, Zhao S, Xu T, Le A, Shi S (2009) Mesenchymal stem cell transplantation reverses multiorgan dysfunction in systemic lupus erythematosus mice and humans. Stem Cells 27(6):1421–1432. doi:10.1002/stem.68
Wu KH, Chan CK, Tsai C, Chang YH, Sieber M, Chiu TH, Ho M, Peng CT, Wu HP, Huang JL (2011) Effective treatment of severe steroid-resistant acute graft-versus-host disease with umbilical cord-derived mesenchymal stem cells. Transplantation 91(12):1412–1416. doi:10.1097/TP.0b013e31821aba18
Ren GW, Zhang LY, Zhao X, Xu GW, Zhang YY, Roberts AI, Zhao RC, Shi YF (2008) Mesenchymal stem cell-mediated immunosuppression occurs via concerted action of chemokines and nitric oxide. Cell Stem Cell 2(2):141–150. doi:10.1016/j.stem.2007.11.014
Ren GW, Zhao X, Zhang LY, Zhang JM, L’Huillier A, Ling WF, Roberts AI, Le AD, Shi ST, Shao CS, Shi YF (2010) Inflammatory cytokine-induced intercellular adhesion molecule-1 and vascular cell adhesion molecule-1 in mesenchymal stem cells are critical for immunosuppression. J Immunol 184(5):2321–2328. doi:10.4049/jimmunol.0902023
Crop MJ, Baan CC, Korevaar SS, Ijzermans JN, Pescatori M, Stubbs AP, van Ijcken WF, Dahlke MH, Eggenhofer E, Weimar W, Hoogduijn MJ (2010) Inflammatory conditions affect gene expression and function of human adipose tissue-derived mesenchymal stem cells. Clin Exp Immunol 162(3):474–486. doi:10.1111/j.1365-2249.2010.04256.x
Ma S, Xie N, Li W, Yuan B, Shi Y, Wang Y (2014) Immunobiology of mesenchymal stem cells. Cell Death Differ 21(2):216–225. doi:10.1038/cdd.2013.158
Li W, Ren G, Huang Y, Su J, Han Y, Li J, Chen X, Cao K, Chen Q, Shou P, Zhang L, Yuan ZR, Roberts AI, Shi S, Le AD, Shi Y (2012) Mesenchymal stem cells: a double-edged sword in regulating immune responses. Cell Death Differ 19(9):1505–1513. doi:10.1038/cdd.2012.26
Renner P, Eggenhofer E, Rosenauer A, Popp FC, Steinmann JF, Slowik P, Geissler EK, Piso P, Schlitt HJ, Dahlke MH (2009) Mesenchymal stem cells require a sufficient, ongoing immune response to exert their immunosuppressive function. Transplant Proc 41(6):2607–2611. doi:10.1016/j.transproceed.2009.06.119
Su J, Chen X, Huang Y, Li W, Li J, Cao K, Cao G, Zhang L, Li F, Roberts AI, Kang H, Yu P, Ren G, Ji W, Wang Y, Shi Y (2014) Phylogenetic distinction of iNOS and IDO function in mesenchymal stem cell-mediated immunosuppression in mammalian species. Cell Death Differ 21(3):388–396. doi:10.1038/cdd.2013.149
Ren G, Su J, Zhang L, Zhao X, Ling W, L’Huillie A, Zhang J, Lu Y, Roberts AI, Ji W, Zhang H, Rabson AB, Shi Y (2009) Species variation in the mechanisms of mesenchymal stem cell-mediated immunosuppression. Stem Cells 27(8):1954–1962. doi:10.1002/stem.118
Bogdan C (2001) Nitric oxide and the immune response. Nat Immunol 2(10):907–916. doi:10.1038/ni1001-907
Bouffi C, Bony C, Courties G, Jorgensen C, Noel D (2010) IL-6-dependent PGE2 secretion by mesenchymal stem cells inhibits local inflammation in experimental arthritis. PLoS One 5(12):e14247. doi:10.1371/journal.pone.0014247
Munn DH (2012) Blocking IDO activity to enhance anti-tumor immunity. Front Biosci (Elite Ed) 4:734–745
Meisel R, Zibert A, Laryea M, Gobel U, Daubener W, Dilloo D (2004) Human bone marrow stromal cells inhibit allogeneic T-cell responses by indoleamine 2,3-dioxygenase-mediated tryptophan degradation. Blood 103(12):4619–4621. doi:10.1182/blood-2003-11-3909
Ling W, Zhang J, Yuan Z, Ren G, Zhang L, Chen X, Rabson AB, Roberts AI, Wang Y, Shi Y (2014) Mesenchymal stem cells use IDO to regulate immunity in tumor microenvironment. Cancer Res 74(5):1576–1587. doi:10.1158/0008-5472.CAN-13-1656
Matysiak M, Orlowski W, Fortak-Michalska M, Jurewicz A, Selmaj K (2011) Immunoregulatory function of bone marrow mesenchymal stem cells in EAE depends on their differentiation state and secretion of PGE2. J Neuroimmunol 233(1–2):106–111. doi:10.1016/j.jneuroim.2010.12.004
Bruno S, Deregibus MC, Camussi G (2015) The secretome of mesenchymal stromal cells: role of extracellular vesicles in immunomodulation. Immunol Lett 168(2):154–158. doi:10.1016/j.imlet.2015.06.007
Burrello J, Monticone S, Gai C, Gomez Y, Kholia S, Camussi G (2016) Stem cell-derived extracellular vesicles and immune-modulation. Front Cell Dev Biol 4:83. doi:10.3389/fcell.2016.00083
Stephen J, Bravo EL, Colligan D, Fraser AR, Petrik J, Campbell JDM (2016) Mesenchymal stromal cells as multifunctional cellular therapeutics—a potential role for extracellular vesicles. Transfus Apher Sci 55(1):62–69. doi:10.1016/j.transci.2016.07.011
Di Trapani M, Bassi G, Midolo M, Gatti A, Kamga PT, Cassaro A, Carusone R, Adamo A, Krampera M (2016) Differential and transferable modulatory effects of mesenchymal stromal cell-derived extracellular vesicles on T, B and NK cell functions. Sci Rep UK 6. doi:10.1038/srep24120
Zhang B, Yin Y, Lai RC, Lim SK (2014) Immunotherapeutic potential of extracellular vesicles. Front Immunol 5:518. doi:10.3389/fimmu.2014.00518
Blazquez R, Sanchez-Margallo FM, de la Rosa O, Dalemans W, Alvarez V, Tarazona R, Casado JG (2014) Immunomodulatory potential of human adipose mesenchymal stem cells derived exosomes on in vitro stimulated T cells. Front Immunol 5:556. doi:10.3389/fimmu.2014.00556
Amarnath S, Foley JE, Farthing DE, Gress RE, Laurence A, Eckhaus MA, Metais JY, Rose JJ, Hakim FT, Felizardo TC, Cheng AV, Robey PG, Stroncek DE, Sabatino M, Battiwalla M, Ito S, Fowler DH, Barrett AJ (2015) Bone marrow-derived mesenchymal stromal cells harness purinergenic signaling to tolerize human Th1 cells in vivo. Stem Cells 33(4):1200–1212. doi:10.1002/stem.1934
Wang L, Gu Z, Zhao X, Yang N, Wang F, Deng A, Zhao S, Luo L, Wei H, Guan L, Gao Z, Li Y, Wang L, Liu D, Gao C (2016) Extracellular vesicles released from human umbilical cord-derived mesenchymal stromal cells prevent life-threatening acute graft-versus-host disease in a mouse model of allogeneic hematopoietic stem cell transplantation. Stem Cells Dev 25(24):1874–1883. doi:10.1089/scd.2016.0107
Favaro E, Carpanetto A, Caorsi C, Giovarelli M, Angelini C, Cavallo-Perin P, Tetta C, Camussi G, Zanone MM (2016) Human mesenchymal stem cells and derived extracellular vesicles induce regulatory dendritic cells in type 1 diabetic patients. Diabetologia 59(2):325–333. doi:10.1007/s00125-015-3808-0
Mokarizadeh A, Delirezh N, Morshedi A, Mosayebi G, Farshid AA, Mardani K (2012) Microvesicles derived from mesenchymal stem cells: potent organelles for induction of tolerogenic signaling. Immunol Lett 147(1–2):47–54. doi:10.1016/j.imlet.2012.06.001
Del Fattore A, Luciano R, Pascucci L, Goffredo BM, Giorda E, Scapaticci M, Fierabracci A, Muraca M (2015) Immunoregulatory effects of mesenchymal stem cell-derived extracellular vesicles on T lymphocytes. Cell Transplant 24(12):2615–2627. doi:10.3727/096368915X687543
Zhang B, Yin Y, Lai RC, Tan SS, Choo AB, Lim SK (2014) Mesenchymal stem cells secrete immunologically active exosomes. Stem Cells Dev 23(11):1233–1244. doi:10.1089/scd.2013.0479
Xu C, Yu P, Han X, Du L, Gan J, Wang Y, Shi Y (2014) TGF-beta promotes immune responses in the presence of mesenchymal stem cells. J Immunol 192(1):103–109. doi:10.4049/jimmunol.1302164
Sala E, Genua M, Petti L, Anselmo A, Arena V, Cibella J, Zanotti L, D’Alessio S, Scaldaferri F, Luca G, Arato I, Calafiore R, Sgambato A, Rutella S, Locati M, Danese S, Vetrano S (2015) Mesenchymal stem cells reduce colitis in mice via release of TSG6, independently of their localization to the intestine. Gastroenterology 149(1):163 e120–176 e120. doi:10.1053/j.gastro.2015.03.013
Choi JJ, Yoo SA, Park SJ, Kang YJ, Kim WU, Oh IH, Cho CS (2008) Mesenchymal stem cells overexpressing interleukin-10 attenuate collagen-induced arthritis in mice. Clin Exp Immunol 153(2):269–276. doi:10.1111/j.1365-2249.2008.03683.x
Pieper K, Grimbacher B, Eibel H (2013) B-cell biology and development. J Allergy Clin Immunol 131(4):959–971. doi:10.1016/j.jaci.2013.01.046
O’Connor BP, Vogel LA, Zhang WJ, Loo W, Shnider D, Lind EF, Ratliff M, Noelle RJ, Erickson LD (2006) Imprinting the fate of antigen-reactive B cells through the affinity of the B cell receptor. J Immunol 177(11):7723–7732
De Silva NS, Klein U (2015) Dynamics of B cells in germinal centres. Nat Rev Immunol 15(3):137–148. doi:10.1038/nri3804
Depoil D, Weber M, Treanor B, Fleire SJ, Carrasco YR, Harwood NE, Batista FD (2009) Early events of B cell activation by antigen. Sci Signal 2(63):pt1. doi:10.1126/scisignal.263pt1
Hayakawa K, Hardy RR, Herzenberg LA, Herzenberg LA (1985) Progenitors for Ly-1 B cells are distinct from progenitors for other B cells. J Exp Med 161(6):1554–1568
Yang M, Sun L, Wang S, Ko KH, Xu H, Zheng BJ, Cao X, Lu L (2010) Novel function of B cell-activating factor in the induction of IL-10-producing regulatory B cells. J Immunol 184(7):3321–3325. doi:10.4049/jimmunol.0902551
Corcione A, Benvenuto F, Ferretti E, Giunti D, Cappiello V, Cazzanti F, Risso M, Gualandi F, Mancardi GL, Pistoia V, Uccelli A (2006) Human mesenchymal stem cells modulate B-cell functions. Blood 107(1):367–372. doi:10.1182/blood-2005-07-2657
Tabera S, Perez-Simon JA, Diez-Campelo M, Sanchez-Abarca LI, Blanco B, Lopez A, Benito A, Ocio E, Sanchez-Guijo FM, Canizo C, San Miguel JF (2008) The effect of mesenchymal stem cells on the viability, proliferation and differentiation of B-lymphocytes. Haematologica 93(9):1301–1309. doi:10.3324/haematol.12857
Che N, Li X, Zhou S, Liu R, Shi D, Lu L, Sun L (2012) Umbilical cord mesenchymal stem cells suppress B-cell proliferation and differentiation. Cell Immunol 274(1–2):46–53. doi:10.1016/j.cellimm.2012.02.004
Asari S, Itakura S, Ferreri K, Liu CP, Kuroda Y, Kandeel F, Mullen Y (2009) Mesenchymal stem cells suppress B-cell terminal differentiation. Exp Hematol 37(5):604–615. doi:10.1016/j.exphem.2009.01.005
Rafei M, Hsieh J, Fortier S, Li M, Yuan S, Birman E, Forner K, Boivin MN, Doody K, Tremblay M, Annabi B, Galipeau J (2008) Mesenchymal stromal cell-derived CCL2 suppresses plasma cell immunoglobulin production via STAT3 inactivation and PAX5 induction. Blood 112(13):4991–4998. doi:10.1182/blood-2008-07-166892
Luz-Crawford P, Djouad F, Toupet K, Bony C, Franquesa M, Hoogduijn MJ, Jorgensen C, Noel D (2016) Mesenchymal stem cell-derived interleukin 1 receptor antagonist promotes macrophage polarization and inhibits B cell differentiation. Stem Cells 34(2):483–492. doi:10.1002/stem.2254
Conforti A, Scarsella M, Starc N, Giorda E, Biagini S, Proia A, Carsetti R, Locatelli F, Bernardo ME (2014) Microvescicles derived from mesenchymal stromal cells are not as effective as their cellular counterpart in the ability to modulate immune responses in vitro. Stem Cells Dev 23(21):2591–2599. doi:10.1089/scd.2014.0091
Schena F, Gambini C, Gregorio A, Mosconi M, Reverberi D, Gattorno M, Casazza S, Uccelli A, Moretta L, Martini A, Traggiai E (2010) Interferon-gamma-dependent inhibition of B cell activation by bone marrow-derived mesenchymal stem cells in a murine model of systemic lupus erythematosus. Arthritis Rheum 62(9):2776–2786. doi:10.1002/art.27560
Franquesa M, Mensah FK, Huizinga R, Strini T, Boon L, Lombardo E, DelaRosa O, Laman JD, Grinyo JM, Weimar W, Betjes MG, Baan CC, Hoogduijn MJ (2015) Human adipose tissue-derived mesenchymal stem cells abrogate plasmablast formation and induce regulatory B cells independently of T helper cells. Stem Cells 33(3):880–891. doi:10.1002/stem.1881
Peng Y, Chen X, Liu Q, Zhang X, Huang K, Liu L, Li H, Zhou M, Huang F, Fan Z, Sun J, Liu Q, Ke M, Li X, Zhang Q, Xiang AP (2015) Mesenchymal stromal cells infusions improve refractory chronic graft versus host disease through an increase of CD5+ regulatory B cells producing interleukin 10. Leukemia 29(3):636–646. doi:10.1038/leu.2014.225
Guo Y, Chan KH, Lai WH, Siu CW, Kwan SC, Tse HF, Wing-Lok Ho P, Wing-Man Ho J (2013) Human mesenchymal stem cells upregulate CD1dCD5(+) regulatory B cells in experimental autoimmune encephalomyelitis. Neuroimmunomodulation 20(5):294–303. doi:10.1159/000351450
Park MJ, Kwok SK, Lee SH, Kim EK, Park SH, Cho ML (2015) Adipose tissue-derived mesenchymal stem cells induce expansion of interleukin-10-producing regulatory B cells and ameliorate autoimmunity in a murine model of systemic lupus erythematosus. Cell Transplant 24(11):2367–2377. doi:10.3727/096368914X685645
Lee DS, Yi TG, Lee HJ, Kim SN, Park S, Jeon MS, Song SU (2014) Mesenchymal stem cells infected with Mycoplasma arginini secrete complement C3 to regulate immunoglobulin production in B lymphocytes. Cell Death Dis 5:e1192. doi:10.1038/cddis.2014.147
Che N, Li X, Zhang L, Liu R, Chen HF, Gao X, Shi ST, Chen WJ, Sun LY (2014) Impaired B cell inhibition by lupus bone marrow mesenchymal stem cells is caused by reduced CCL2 expression. J Immunol 193(10):5306–5314. doi:10.4049/jimmunol.1400036
Rasmusson I, Le Blanc K, Sundberg B, Ringden O (2007) Mesenchymal stem cells stimulate antibody secretion in human B cells. Scand J Immunol 65(4):336–343. doi:10.1111/j.1365-3083.2007.01905.x
Traggiai E, Volpi S, Schena F, Gattorno M, Ferlito F, Moretta L, Martini A (2008) Bone marrow-derived mesenchymal stem cells induce both polyclonal expansion and differentiation of B cells isolated from healthy donors and systemic lupus erythematosus patients. Stem Cells 26(2):562–569. doi:10.1634/stemeells.2007-0528
Healy ME, Bergin R, Mahon BP, English K (2015) Mesenchymal stromal cells protect against caspase 3-mediated apoptosis of CD19(+) peripheral B cells through contact-dependent upregulation of VEGF. Stem Cells Dev 24(20):2391–2402. doi:10.1089/scd.2015.0089
Franquesa M, Hoogduijn MJ, Bestard O, Grinyo JM (2012) Immunomodulatory effect of mesenchymal stem cells on B cells. Front Immunol 3. doi:10.3389/fimmu.2012.00212
Mildner A, Jung S (2014) Development and function of dendritic cell subsets. Immunity 40(5):642–656. doi:10.1016/j.immuni.2014.04.016
Zhang W, Ge W, Li C, You S, Liao L, Han Q, Deng W, Zhao RC (2004) Effects of mesenchymal stem cells on differentiation, maturation, and function of human monocyte-derived dendritic cells. Stem Cells Dev 13(3):263–271. doi:10.1089/154732804323099190
Jiang XX, Zhang Y, Liu B, Zhang SX, Wu Y, Yu XD, Mao N (2005) Human mesenchymal stem cells inhibit differentiation and function of monocyte-derived dendritic cells. Blood 105(10):4120–4126. doi:10.1182/blood-2004-02-0586
Nauta AJ, Kruisselbrink AB, Lurvink E, Willemze R, Fibbe WE (2006) Mesenchymal stem cells inhibit generation and function of both CD34+-derived and monocyte-derived dendritic cells. J Immunol 177(4):2080–2087
Li YP, Paczesny S, Lauret E, Poirault S, Bordigoni P, Mekhloufi F, Hequet O, Bertrand Y, Ou-Yang JP, Stoltz JF, Miossec P, Eljaafari A (2008) Human mesenchymal stem cells license adult CD34(+) hemopoietic progenitor cells to differentiate into regulatory dendritic cells through activation of the notch pathway. J Immunol 180(3):1598–1608
Chen HW, Chen HY, Wang LT, Wang FH, Fang LW, Lai HY, Chen HH, Lu J, Hung MS, Cheng Y, Chen MY, Liu SJ, Chong P, Lee OKS, Hsu SC (2013) Mesenchymal stem cells tune the development of monocyte-derived dendritic cells toward a myeloid-derived suppressive phenotype through growth-regulated oncogene chemokines. J Immunol 190(10):5065–5077. doi:10.4049/jimmunol.1202775
Abomaray FM, Al Jumah MA, Kalionis B, AlAskar AS, Al Harthy S, Jawdat D, Al Khaldi A, Alkushi A, Knawy BA, Abumaree MH (2015) Human chorionic villous mesenchymal stem cells modify the functions of human dendritic cells, and induce an anti-inflammatory phenotype in CD1+ dendritic cells. Stem Cell Rev 11(3):423–441. doi:10.1007/s12015-014-9562-8
English K, Barry FP, Mahon BP (2008) Murine mesenchymal stem cells suppress dendritic cell migration, maturation and antigen presentation. Immunol Lett 115(1):50–58. doi:10.1016/j.imlet.2007.10.002
Zhang B, Liu R, Shi D, Liu XX, Chen Y, Dou XW, Zhu XS, Lu CH, Liang W, Liao LM, Zenke M, Zhao RCH (2009) Mesenchymal stem cells induce mature dendritic cells into a novel Jagged-2-dependent regulatory dendritic cell population. Blood 113(1):46–57. doi:10.1182/blood-2008-04-154138
Liu X, Qu X, Chen Y, Liao L, Cheng K, Shao C, Zenke M, Keating A, Zhao RC (2012) Mesenchymal stem/stromal cells induce the generation of novel IL-10-dependent regulatory dendritic cells by SOCS3 activation. J Immunol 189(3):1182–1192. doi:10.4049/jimmunol.1102996
Cahill EF, Tobin LM, Carty F, Mahon BP, English K (2015) Jagged-1 is required for the expansion of CD4(+)CD25(+)FoxP3(+) regulatory T cells and tolerogenic dendritic cells by murine mesenchymal stromal cells. Stem Cell Res Ther 6. doi:10.1186/s13287-015-0021-5
Chiesa S, Morbelli S, Morando S, Massollo M, Marini C, Bertoni A, Frassoni F, Bartolome ST, Sambuceti G, Traggiai E, Uccelli A (2011) Mesenchymal stem cells impair in vivo T-cell priming by dendritic cells. P Natl Acad Sci USA 108(42):17384–17389. doi:10.1073/pnas.1103650108
Li H, Guo Z, Jiang X, Zhu H, Li X, Mao N (2008) Mesenchymal stem cells alter migratory property of T and dendritic cells to delay the development of murine lethal acute graft-versus-host disease. Stem Cells 26(10):2531–2541. doi:10.1634/stemcells.2008-0146
Zhang Y, Cai W, Huang Q, Gu Y, Shi Y, Huang J, Zhao F, Liu Q, Wei X, Jin M, Wu C, Xie Q, Zhang Y, Wan B, Zhang Y (2014) Mesenchymal stem cells alleviate bacteria-induced liver injury in mice by inducing regulatory dendritic cells. Hepatology 59(2):671–682. doi:10.1002/hep.26670
Liu XX, Ren SD, Ge CZ, Cheng K, Zenke M, Keating A, Zhao RCH (2015) Sca-1(+)Lin(−)CD117(−) mesenchymal stem/stromal sells induce the generation of novel IRF8-controlled regulatory dendritic cells through Notch-RBP-J signaling. J Immunol 194(9):4298–4308. doi:10.4049/jimmunol.1402641
Huang YF, Chen P, Zhang CB, Ko GJ, Ruiz M, Fiorina P, Hussain MA, Wasowska BA, Rabb H, Womer KL (2010) Kidney-derived mesenchymal stromal cells modulate dendritic cell function to suppress alloimmune responses and delay allograft rejection. Transplantation 90(12):1307–1311. doi:10.1097/TP.0b013e3181fdd9eb
Djouad F, Charbonnier LM, Bouffi C, Louis-Plence P, Bony C, Apparailly F, Cantos C, Jorgensen C, Noel D (2007) Mesenchymal stem cells inhibit the differentiation of dendritic cells through an interleukin-6-dependent mechanism. Stem Cells 25(8):2025–2032. doi:10.1634/stemcells.2006-0548
Deng Y, Yi S, Wang G, Cheng J, Zhang Y, Chen W, Tai Y, Chen S, Chen G, Liu W, Zhang Q, Yang Y (2014) Umbilical cord-derived mesenchymal stem cells instruct dendritic cells to acquire tolerogenic phenotypes through the IL-6-mediated upregulation of SOCS1. Stem Cells Dev 23(17):2080–2092. doi:10.1089/scd.2013.0559
Spaggiari GM, Abdelrazik H, Becchetti F, Moretta L (2009) MSCs inhibit monocyte-derived DC maturation and function by selectively interfering with the generation of immature DCs: central role of MSC-derived prostaglandin E2. Blood 113(26):6576–6583. doi:10.1182/blood-2009-02-203943
Ramasamy R, Fazekasova H, Lam EWF, Soeiro I, Lombardi G, Dazzi F (2007) Mesenchymal stem cells inhibit dendritic cell differentiation and function by preventing entry into the cell cycle. Transplantation 83(1):71–76. doi:10.1097/01.tp.0000244572.24780.54
Chia JJ, Zhu T, Chyou S, Dasoveanu DC, Carballo C, Tian S, Magro CM, Rodeo S, Spiera RF, Ruddle NH, McGraw TE, Browning JL, Lafyatis R, Gordon JK, Lu TT (2016) Dendritic cells maintain dermal adipose-derived stromal cells in skin fibrosis. J Clin Invest. doi:10.1172/JCI85740
Wynn TA, Vannella KM (2016) Macrophages in tissue repair, regeneration, and fibrosis. Immunity 44(3):450–462. doi:10.1016/j.immuni.2016.02.015
Perdiguero EG, Geissmann F (2016) The development and maintenance of resident macrophages. Nat Immunol 17(1):2–8. doi:10.1038/ni.3341
Schulz C, Gomez Perdiguero E, Chorro L, Szabo-Rogers H, Cagnard N, Kierdorf K, Prinz M, Wu B, Jacobsen SE, Pollard JW, Frampton J, Liu KJ, Geissmann F (2012) A lineage of myeloid cells independent of Myb and hematopoietic stem cells. Science 336(6077):86–90. doi:10.1126/science.1219179
Glass CK, Natoli G (2016) Molecular control of activation and priming in macrophages. Nat Immunol 17(1):26–33. doi:10.1038/ni.3306
Zhang QZ, Su WR, Shi SH, Wilder-Smith P, Xiang AP, Wong A, Nguyen AL, Kwon CW, Le AD (2010) Human gingiva-derived mesenchymal stem cells elicit polarization of M2 macrophages and enhance cutaneous wound healing. Stem Cells 28(10):1856–1868. doi:10.1002/stem.503
Cho DI, Kim MR, Jeong HY, Jeong HC, Jeong MH, Yoon SH, Kim YS, Ahn Y (2014) Mesenchymal stem cells reciprocally regulate the M1/M2 balance in mouse bone marrow-derived macrophages. Exp Mol Med 46. doi:10.1038/emm.2013.135
Francois M, Romieu-Mourez R, Li M, Galipeau J (2012) Human MSC suppression correlates with cytokine induction of indoleamine 2,3-dioxygenase and bystander M2 macrophage differentiation. Mol Ther 20(1):187–195. doi:10.1038/mt.2011.189
Selleri S, Bifsha P, Civini S, Pacelli C, Dieng MM, Lemieux W, Jin P, Bazin R, Patey N, Marincola FM, Moldovan F, Zaouter C, Trudeau LE, Benabdhalla B, Louis I, Beausejour C, Stroncek D, Le Deist F, Haddad E (2016) Human mesenchymal stromal cell-secreted lactate induces M2-macrophage differentiation by metabolic reprogramming. Oncotarget 7(21):30193–30210. doi:10.18632/oncotarget.8623
Nemeth K, Leelahavanichkul A, Yuen PST, Mayer B, Parmelee A, Doi K, Robey PG, Leelahavanichkul K, Koller BH, Brown JM, Hu XZ, Jelinek I, Star RA, Mezey E (2009) Bone marrow stromal cells attenuate sepsis via prostaglandin E-2-dependent reprogramming of host macrophages to increase their interleukin-10 production. Nat Med 15(1):42–49. doi:10.1038/nm.1905
Choi H, Lee RH, Bazhanov N, Oh JY, Prockop DJ (2011) Anti-inflammatory protein TSG-6 secreted by activated MSCs attenuates zymosan-induced mouse peritonitis by decreasing TLR2/NF-kappa B signaling in resident macrophages. Blood 118(2):330–338. doi:10.1182/blood-2010-12-327353
Wise AF, Williams TM, Kiewiet MBG, Payne NL, Siatskas C, Samuel CS, Ricardo SD (2014) Human mesenchymal stem cells alter macrophage phenotype and promote regeneration via homing to the kidney following ischemia-reperfusion injury. Am J Physiol Renal 306(10):F1222–F1235. doi:10.1152/ajprenal.00675.2013
Lee KC, Lin HC, Huang YH, Hung SC (2015) Allo-transplantation of mesenchymal stem cells attenuates hepatic injury through IL1Ra dependent macrophage switch in a mouse model of liver disease. J Hepatol 63(6):1405–1412. doi:10.1016/j.jhep.2015.09.007
Zullo JA, Nadel EP, Rabadi MM, Baskind MJ, Rajdev MA, Demaree CM, Vasko R, Chugh SS, Lamba R, Goligorsky MS, Ratliff BB (2015) The secretome of hydrogel-coembedded endothelial progenitor cells and mesenchymal stem cells instructs macrophage polarization in endotoxemia. Stem Cells Transl Med 4(7):852–861. doi:10.5966/sctm.2014-0111
Xie ZY, Hao HJ, Tong C, Cheng Y, Liu JJ, Pang YP, Si YL, Guo YL, Zang L, Mu YM, Han WD (2016) Human umbilical cord-derived mesenchymal stem cells elicit macrophages into an anti-inflammatory phenotype to alleviate insulin resistance in type 2 diabetic rats. Stem Cells 34(3):627–639. doi:10.1002/stem.2238
Braza F, Dirou S, Forest V, Sauzeau V, Hassoun D, Chesne J, Cheminant-Muller MA, Sagan C, Magnan A, Lemarchand P (2016) Mesenchymal stem cells induce suppressive mcrophages through phagocytosis in a mouse model of asthma. Stem Cells 34(7):1836–1845. doi:10.1002/stem.2344
Chaturvedi P, Gilkes DM, Takano N, Semenza GL (2014) Hypoxia-inducible factor-dependent signaling between triple-negative breast cancer cells and mesenchymal stem cells promotes macrophage recruitment. P Natl Acad Sci USA 111(20):E2120–E2129. doi:10.1073/pnas.1406655111
Liu WX, Zhang S, Gu SZ, Sang LX, Dai C (2015) Mesenchymal stem cells recruit macrophages to alleviate experimental colitis through TGF beta 1. Cell Physiol Biochem 35(3):858–865. doi:10.1159/000369743
Braza F, Dirou S, Forest V, Sauzeau V, Hassoun D, Chesne J, Cheminant-Muller MA, Sagan C, Magnan A, Lemarchand P (2016) Mesenchymal stem cells induce suppressive macrophages through phagocytosis in a mouse model of asthma. Stem Cells 34(7):1836–1845. doi:10.1002/stem.2344
Ylostalo JH, Bartosh TJ, Coble K, Prockop DJ (2012) Human mesenchymal stem/stromal cells cultured as spheroids are self-activated to produce prostaglandin E2 that directs stimulated macrophages into an anti-inflammatory phenotype. Stem Cells 30(10):2283–2296. doi:10.1002/stem.1191
Song XL, Xie SS, Lu K, Wang CH (2015) Mesenchymal stem cells alleviate experimental asthma by inducing polarization of alveolar macrophages. Inflammation 38(2):485–492. doi:10.1007/s10753-014-9954-6
Fathman JW, Bhattacharya D, Inlay MA, Seita J, Karsunky H, Weissman IL (2011) Identification of the earliest natural killer cell-committed progenitor in murine bone marrow. Blood 118(20):5439–5447. doi:10.1182/blood-2011-04-348912
Res P, MartinezCaceres E, Jaleco AC, Staal F, Noteboom E, Weijer K, Spits H (1996) CD34(+)CD38(dim) cells in the human thymus can differentiate into T, natural killer, and dendritic cells but are distinct from pluripotent stem cells. Blood 87(12):5196–5206
Pegram HJ, Andrews DM, Smyth MJ, Darcy PK, Kershaw MH (2011) Activating and inhibitory receptors of natural killer cells. Immunol Cell Biol 89(2):216–224. doi:10.1038/icb.2010.78
Childs RW, Carlsten M (2015) Therapeutic approaches to enhance natural killer cell cytotoxicity against cancer: the force awakens. Nat Rev Drug Discov 14(7):487–498. doi:10.1038/nrd4506
Fauriat C, Long EO, Ljunggren HG, Bryceson YT (2010) Regulation of human NK-cell cytokine and chemokine production by target cell recognition. Blood 115(11):2167–2176. doi:10.1182/blood-2009-08-238469
Aggarwal S, Pittenger MF (2005) Human mesenchymal stem cells modulate allogeneic immune cell responses. Blood 105(4):1815–1822. doi:10.1182/blood-2004-04-1559
Spaggiari GM, Capobianco A, Becchetti S, Mingari MC, Moretta L (2006) Mesenchymal stem cell-natural killer cell interactions: evidence that activated NK cells are capable of killing MSCs, whereas MSCs can inhibit IL-2-induced NK-cell proliferation. Blood 107(4):1484–1490. doi:10.1182/blood-2005-07-2775
Sotiropoulou PA, Perez SA, Gritzapis AD, Baxevanis CN, Papamichail M (2006) Interactions between human mesenchymal stem cells and natural killer cells. Stem Cells 24(1):74–85. doi:10.1634/stemcells.2004-0359
Spaggiari GM, Capobianco A, Abdelrazik H, Becchetti F, Mingari MC, Moretta L (2008) Mesenchymal stem cells inhibit natural killer-cell proliferation, cytotoxicity, and cytokine production: role of indoleamine 2,3-dioxygenase and prostaglandin E2. Blood 111(3):1327–1333. doi:10.1182/blood-2007-02-074997
Qu MM, Cui J, Zhu J, Ma YH, Yuan X, Shi JM, Guo DY, Li CY (2015) Bone marrow-derived mesenchymal stem cells suppress NK cell recruitment and activation in PolyI:C-induced liver injury. Biochem Biophys Res Commun 466(2):173–179. doi:10.1016/j.bbrc.2015.08.125
Michelo CM, Fasse E, Van Cranenbroek B, Linda K, van der Meer A, Abdelrazik H, Joosten I (2016) Added effects of dexamethasone and mesenchymal stem cells on early Natural Killer cell activation. Transpl Immunol 37:1–9. doi:10.1016/j.trim.2016.04.008
Chen X, Shao H, Zhi Y, Xiao Q, Su C, Dong L, Liu X, Li X, Zhang X (2016) CD73 pathway contributes to the immunosuppressive ability of mesenchymal stem cells in intraocular autoimmune responses. Stem Cells Dev 25(4):337–346. doi:10.1089/scd.2015.0227
Chatterjee D, Tufa DM, Baehre H, Hass R, Schmidt RE, Jacobs R (2014) Natural killer cells acquire CD73 expression upon exposure to mesenchymal stem cells. Blood 123(4):594–595. doi:10.1182/blood-2013-09-524827
El Omar R, Xiong Y, Dostert G, Louis H, Gentils M, Menu P, Stoltz JF, Velot E, Decot V (2016) Immunomodulation of endothelial differentiated mesenchymal stromal cells: impact on T and NK cells. Immunol Cell Biol 94(4):342–356. doi:10.1038/icb.2015.94
Lu Y, Liu J, Liu Y, Qin YR, Luo Q, Wang QL, Duan HF (2015) TLR4 plays a crucial role in MSC-induced inhibition of NK cell function. Biochem Biophys Res Commun 464(2):541–547. doi:10.1016/j.bbrc.2015.07.002
Boissel L, Tuncer HH, Betancur M, Wolfberg A, Klingemann H (2008) Umbilical cord mesenchymal stem cells increase expansion of cord blood natural killer cells. Biol Blood Marrow Transplant 14(9):1031–1038. doi:10.1016/j.bbmt.2008.06.016
Thomas H, Jager M, Mauel K, Brandau S, Lask S, Flohe SB (2014) Interaction with mesenchymal stem cells provokes natural killer cells for enhanced IL-12/IL-18-induced interferon-gamma secretion. Mediat Inflamm. doi:10.1155/2014/143463
Cui RT, Rekasi H, Hepner-Schefczyk M, Fessmann K, Petri RM, Bruderek K, Brandau S, Jager M, Flohe SB (2016) Human mesenchymal stromal/stem cells acquire immunostimulatory capacity upon cross-talk with natural killer cells and might improve the NK cell function of immunocompromised patients. Stem Cell Res Ther 7. doi:10.1186/s13287-016-0353-9
Almeida CR, Caires HR, Vasconcelos DP, Barbosa MA (2016) NAP-2 secreted by human NK cells can stimulate mesenchymal stem/stromal cell recruitment. Stem Cell Rep 6(4):466–473. doi:10.1016/j.stemcr.2016.02.012
Gotherstrom C, Lundqvist A, Duprez IR, Childs R, Berg L, le Blanc K (2011) Fetal and adult multipotent mesenchymal stromal cells are killed by different pathways. Cytotherapy 13(3):269–278. doi:10.3109/14653249.2010.523077
Kolaczkowska E, Kubes P (2013) Neutrophil recruitment and function in health and inflammation. Nat Rev Immunol 13(3):159–175. doi:10.1038/nri3399
Brinkmann V, Reichard U, Goosmann C, Fauler B, Uhlemann Y, Weiss DS, Weinrauch Y, Zychlinsky A (2004) Neutrophil extracellular traps kill bacteria. Science 303(5663):1532–1535. doi:10.1126/science.1092385
Raffaghello L, Bianchi G, Bertolotto M, Montecucco F, Busca A, Dallegri F, Ottonello L, Pistoia V (2008) Human mesenchymal stem cells inhibit neutrophil apoptosis: a model for neutrophil preservation in the bone marrow niche. Stem cells 26(1):151–162. doi:10.1634/stemcells.2007-0416
Cassatella MA, Mosna F, Micheletti A, Lisi V, Tamassia N, Cont C, Calzetti F, Pelletier M, Pizzolo G, Krampera M (2011) Toll-like receptor-3-activated human mesenchymal stromal cells significantly prolong the survival and function of neutrophils. Stem cells 29(6):1001–1011. doi:10.1002/stem.651
Brandau S, Jakob M, Hemeda H, Bruderek K, Janeschik S, Bootz F, Lang S (2010) Tissue-resident mesenchymal stem cells attract peripheral blood neutrophils and enhance their inflammatory activity in response to microbial challenge. J Leukoc Biol 88(5):1005–1015. doi:10.1189/jlb.0410207
Romieu-Mourez R, Francois M, Boivin MN, Bouchentouf M, Spaner DE, Galipeau J (2009) Cytokine modulation of TLR expression and activation in mesenchymal stromal cells leads to a proinflammatory phenotype. J Immunol 182(12):7963–7973. doi:10.4049/jimmunol.0803864
Yu PF, Huang Y, Han YY, Lin LY, Sun WH, Rabson AB, Wang Y, Shi YF (2016) TNFalpha-activated mesenchymal stromal cells promote breast cancer metastasis by recruiting CXCR2+ neutrophils. Oncogene. doi:10.1038/onc.2016.217
Isakova IA, Baker KC, Dufour J, Phinney DG (2016) Mesenchymal stem cells yield transient improvements in motor function in an infant rhesus macaque with severe early-onset krabbe disease. Stem Cells Transl Med. doi:10.5966/sctm.2015-0317
Brandau S, Jakob M, Bruderek K, Bootz F, Giebel B, Radtke S, Mauel K, Jager M, Flohe SB, Lang S (2014) Mesenchymal stem cells augment the anti-bacterial activity of neutrophil granulocytes. PLoS One 9(9):e106903. doi:10.1371/journal.pone.0106903
Jiang D, Muschhammer J, Qi Y, Kugler A, de Vries JC, Saffarzadeh M, Sindrilaru A, Beken SV, Wlaschek M, Kluth MA, Ganss C, Frank NY, Frank MH, Preissner KT, Scharffetter-Kochanek K (2016) Suppression of neutrophil-mediated tissue damage—a novel skill of mesenchymal stem cells. Stem Cells 34(9):2393–2406. doi:10.1002/stem.2417
Munir H, Luu NT, Clarke LS, Nash GB, McGettrick HM (2016) Comparative ability of mesenchymal stromal cells from different tissues to limit neutrophil recruitment to inflamed endothelium. PLoS One 11(5):e0155161. doi:10.1371/journal.pone.0155161
Zhu YG, Feng XM, Abbott J, Fang XH, Hao Q, Monsel A, Qu JM, Matthay MA, Lee JW (2014) Human mesenchymal stem cell microvesicles for treatment of Escherichia coli endotoxin-induced acute lung injury in mice. Stem Cells 32(1):116–125. doi:10.1002/stem.1504
Amin K (2012) The role of mast cells in allergic inflammation. Respir Med 106(1):9–14. doi:10.1016/j.rmed.2011.09.007
Theoharides TC, Alysandratos KD, Angelidou A, Delivanis DA, Sismanopoulos N, Zhang B, Asadi S, Vasiadi M, Weng Z, Miniati A, Kalogeromitros D (2012) Mast cells and inflammation. Biochim Biophys Acta 1822(1):21–33. doi:10.1016/j.bbadis.2010.12.014
Theoharides TC, Valent P, Akin C (2015) Mast cells, mastocytosis, and related disorders. N Engl J Med 373(2):163–172. doi:10.1056/NEJMra1409760
Brown JM, Nemeth K, Kushnir-Sukhov NM, Metcalfe DD, Mezey E (2011) Bone marrow stromal cells inhibit mast cell function via a COX2-dependent mechanism. Clin Exp Allergy 41(4):526–534. doi:10.1111/j.1365-2222.2010.03685.x
Kim HS, Yun JW, Shin TH, Lee SH, Lee BC, Yu KR, Seo Y, Lee S, Kang TW, Choi SW, Seo KW, Kang KS (2015) Human umbilical cord blood mesenchymal stem cell-derived PGE2 and TGF-beta1 alleviate atopic dermatitis by reducing mast cell degranulation. Stem Cells 33(4):1254–1266. doi:10.1002/stem.1913
Liu J, Kuwabara A, Kamio Y, Hu S, Park J, Hashimoto T, Lee JW (2016) Human mesenchymal stem cell-derived microvesicles prevent the rupture of intracranial aneurysm in part by suppression of mast cell activation via a PGE2-dependent mechanism. Stem Cells. doi:10.1002/stem.2448
Su W, Wan Q, Huang J, Han L, Chen X, Chen G, Olsen N, Zheng SG, Liang D (2015) Culture medium from TNF-alpha-stimulated mesenchymal stem cells attenuates allergic conjunctivitis through multiple antiallergic mechanisms. J Allergy Clin Immunol 136(2):423 e428–432 e428. doi:10.1016/j.jaci.2014.12.1926
Kim A, Yu HY, Heo J, Song M, Shin JH, Lim J, Yoon SJ, Kim Y, Lee S, Kim SW, Oh W, Choi SJ, Shin DM, Choo MS (2016) Mesenchymal stem cells protect against the tissue fibrosis of ketamine-induced cystitis in rat bladder. Sci Rep 6:30881. doi:10.1038/srep30881
Su WR, Zhang QZ, Shi SH, Nguyen AL, Le AD (2011) Human gingiva-derived mesenchymal stromal cells attenuate contact hypersensitivity via prostaglandin E2-dependent mechanisms. Stem Cells 29(11):1849–1860. doi:10.1002/stem.738
Allakhverdi Z, Comeau MR, Armant M, Agrawal R, Woodfolk JA, Sehmi R, Howie KJ, Gauvreau GM, Delespesse G (2013) Mast cell-activated bone marrow mesenchymal stromal cells regulate proliferation and lineage commitment of CD34(+) progenitor cells. Front Immunol 4:461. doi:10.3389/fimmu.2013.00461
Nazari M, Ni NC, Ludke A, Li SH, Guo J, Weisel RD, Li RK (2016) Mast cells promote proliferation and migration and inhibit differentiation of mesenchymal stem cells through PDGF. J Mol Cell Cardiol 94:32–42. doi:10.1016/j.yjmcc.2016.03.007
Le Blanc K, Rasmusson I, Sundberg B, Gotherstrom C, Hassan M, Uzunel M, Ringden O (2004) Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet 363(9419):1439–1441. doi:10.1016/S0140-6736(04)16104-7
Chen SL, Fang WW, Ye F, Liu YH, Qian J, Shan SJ, Zhang JJ, Chunhua RZ, Liao LM, Lin S, Sun JP (2004) Effect on left ventricular function of intracoronary transplantation of autologous bone marrow mesenchymal stem cell in patients with acute myocardial infarction. Am J Cardiol 94(1):92–95. doi:10.1016/j.amjcard.2004.03.034
He XW, He XS, Lian L, Wu XJ, Lan P (2012) Systemic infusion of bone marrow-derived mesenchymal stem cells for treatment of experimental colitis in mice. Dig Dis Sci 57(12):3136–3144. doi:10.1007/s10620-012-2290-5
Carlsson PO, Schwarcz E, Korsgren O, Le Blanc K (2015) Preserved beta-cell function in type 1 diabetes by mesenchymal stromal cells. Diabetes 64(2):587–592. doi:10.2337/db14-0656
Kurtzberg J, Prockop S, Teira P, Bittencourt H, Lewis V, Chan KW, Horn B, Yu L, Talano JA, Nemecek E, Mills CR, Chaudhury S (2014) Allogeneic human mesenchymal stem cell therapy (remestemcel-L, Prochymal) as a rescue agent for severe refractory acute graft-versus-host disease in pediatric patients. Biol Blood Marrow Transplant 20(2):229–235. doi:10.1016/j.bbmt.2013.11.001
Wohn DY (2012) Korea okays stem cell therapies despite limited peer-reviewed data. Nat Med 18(3):329–329. doi:10.1038/nm0312-329a
Allison M (2009) Genzyme backs Osiris, despite Prochymal flop. Nat Biotechnol 27(11):966–967. doi:10.1038/nbt1109-966
Yamout B, Hourani R, Salti H, Barada W, El-Hajj T, Al-Kutoubi A, Herlopian A, Baz EK, Mahfouz R, Khalil-Hamdan R, Kreidieh NM, El-Sabban M, Bazarbachi A (2010) Bone marrow mesenchymal stem cell transplantation in patients with multiple sclerosis: a pilot study. J Neuroimmunol 227(1–2):185–189. doi:10.1016/j.jneuroim.2010.07.013
Lazarus HM, Haynesworth SE, Gerson SL, Rosenthal NS, Caplan AI (1995) Ex vivo expansion and subsequent infusion of human bone marrow-derived stromal progenitor cells (mesenchymal progenitor cells): implications for therapeutic use. Bone Marrow Transplant 16(4):557–564
Chen M, Su W, Lin X, Guo Z, Wang J, Zhang Q, Brand D, Ryffel B, Huang J, Liu Z, He X, Le AD, Zheng SG (2013) Adoptive transfer of human gingiva-derived mesenchymal stem cells ameliorates collagen-induced arthritis via suppression of Th1 and Th17 cells and enhancement of regulatory T cell differentiation. Arthritis Rheum 65(5):1181–1193. doi:10.1002/art.37894
Acknowledgements
This study was done with the support of Grants from the China National Basic Research Program (JFYS 2016YFA0100203), the National Natural Science Foundation of China (31272518, 31572399), and the Program of the Shaanxi Province (2015NY157).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Li, N., Hua, J. Interactions between mesenchymal stem cells and the immune system. Cell. Mol. Life Sci. 74, 2345–2360 (2017). https://doi.org/10.1007/s00018-017-2473-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00018-017-2473-5