Abstract
Background
Studies concerning the relationship between distal radius fracture malunion and a persistent arm-related disability have produced conflicting results.
Questions/purposes
We investigated (1) how arm-related disability changes during the first 2 years after a fracture and (2) whether fracture malunion causes persistent disability.
Methods
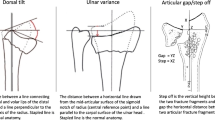
One hundred twenty-three patients with distal radius fractures, treated with closed reduction and casts or external or percutaneous pin fixations, completed the DASH questionnaire at baseline, 3 months, 6 months, 1 year, and 2 years after fracture. Radiographic measurements were made at 1 year. Using a definition of malunion as ulnar variance of 1 mm or more and dorsal tilt greater than 10°, the patients were classified into three groups: no malunion (n = 35), malunion involving either ulnar variance or dorsal tilt (n = 65), and malunion involving ulnar variance and dorsal tilt (n = 23). The changes in the DASH scores with time (baseline to 2 years), in relation to malunion, were analyzed using generalized estimating equations adjusted for age, sex, fracture type (extraarticular or intraarticular), and treatment method.
Results
The mean change in DASH scores from baseline to 2 years was worse for patients with malunions involving ulnar variance and dorsal tilt than for patients with no malunions (mean difference, 13; 95% CI, 1.4–25) and for patients with malunions involving either ulnar variance or dorsal tilt (mean difference, 13; 95% CI, 2.2–24).
Conclusion
After distal radius fracture, arm-related disabilities are more likely to persist at least 2 years in patients with fractures that healed with shortening and dorsal angulation than in patients with only shortening or dorsal angulation or without malunion.
Level of evidence
Level II, prognostic study. See Guidelines for Authors for a complete description of levels of evidence.

Similar content being viewed by others
References
Abramo A, Kopylov P, Tagil M. Evaluation of a treatment protocol in distal radius fractures: a prospective study in 581 patients using DASH as outcome. Acta Orthop. 2008;79:376–385.
Altissimi M, Antenucci R, Fiacca C, Mancini GB. Long-term results of conservative treatment of fractures of the distal radius. Clin Orthop Relat Res. 1986;206:202–210.
Arora R, Lutz M, Deml C, Krappinger D, Haug L, Gabl M. A prospective randomized trial comparing nonoperative treatment with volar locking plate fixation for displaced and unstable distal radial fractures in patients sixty-five years of age and older. J Bone Joint Surg Am. 2011;93:2146–2153.
Atroshi I, Gummesson C, Andersson B, Dahlgren E, Johansson A. The Disabilities of the Arm, Shoulder and Hand (DASH) outcome questionnaire: reliability and validity of the Swedish version evaluated in 176 patients. Acta Orthop Scand. 2000;71:613–618.
Batra S, Gupta A. The effect of fracture-related factors on the functional outcome at 1 year in distal radius fractures. Injury. 2002;33:499–502.
Brogren E, Hofer M, Petranek M, Wagner P, Dahlin LB, Atroshi I. Relationship between distal radius fracture malunion and arm-related disability: a prospective population-based cohort study with 1-year follow-up. BMC Musculoskelet Disord. 2011;12:9.
Chung KC, Kotsis SV, Kim HM. Predictors of functional outcomes after surgical treatment of distal radius fractures. J Hand Surg Am. 2007;32:76–83.
Edwards BJ, Song J, Dunlop DD, Fink HA, Cauley JA. Functional decline after incident wrist fractures—Study of Osteoporotic Fractures: prospective cohort study. BMJ. 2010;341:c3324.
Egol KA, Walsh M, Romo-Cardoso S, Dorsky S, Paksima N. Distal radial fractures in the elderly: operative compared with nonoperative treatment. J Bone Joint Surg Am. 2010;92:1851–1857.
Flinkkila T, Raatikainen T, Hamalainen M. AO and Frykman’s classifications of Colles’ fracture: no prognostic value in 652 patients evaluated after 5 years. Acta Orthop Scand. 1998;69:77–81.
Foldhazy Z, Tornkvist H, Elmstedt E, Andersson G, Hagsten B, Ahrengart L. Long-term outcome of nonsurgically treated distal radius fractures. J Hand Surg Am. 2007;32:1374–1384.
Gliatis JD, Plessas SJ, Davis TR. Outcome of distal radial fractures in young adults. J Hand Surg Br. 2000;25:535–543.
Gummesson C, Atroshi I, Ekdahl C. The Disabilities of the Arm, Shoulder and Hand (DASH) outcome questionnaire: longitudinal construct validity and measuring self-rated health change after surgery. BMC Musculoskelet Disord. 2003;4:11.
Hudak PL, Amadio PC, Bombardier C. Development of an upper extremity outcome measure: the DASH (disabilities of the arm, shoulder and hand) [corrected]. The Upper Extremity Collaborative Group (UECG). Am J Ind Med. 1996;29:602–608.
Hunsaker FG, Cioffi DA, Amadio PC, Wright JG, Caughlin B. The American Academy of Orthopaedic Surgeons outcomes instruments: normative values from the general population. J Bone Joint Surg Am. 2002;84:208–215.
Jupiter JB, Masem M. Reconstruction of post-traumatic deformity of the distal radius and ulna. Hand Clin. 1988;4:377–390.
Karnezis IA, Panagiotopoulos E, Tyllianakis M, Megas P, Lambiris E. Correlation between radiological parameters and patient-rated wrist dysfunction following fractures of the distal radius. Injury. 2005;36:1435–1439.
Kopylov P, Johnell O, Redlund-Johnell I, Bengner U. Fractures of the distal end of the radius in young adults: a 30-year follow-up. J Hand Surg Br. 1993;18:45–49.
Little RJ, D’Agostino R, Cohen ML, Dickersin K, Emerson SS, Farrar JT, Frangakis C, Hogan JW, Molenberghs G, Murphy SA, Neaton JD, Rotnitzky A, Scharfstein D, Shih WJ, Siegel JP, Stern H. The prevention and treatment of missing data in clinical trials. N Engl J Med. 2012;367:1355–1360.
MacDermid JC, Richards RS, Donner A, Bellamy N, Roth JH. Responsiveness of the Short Form-36, Disability of the Arm, Shoulder, and Hand questionnaire, Patient-Rated Wrist Evaluation, and physical impairment measurements in evaluating recovery after a distal radius fracture. J Hand Surg Am. 2000;25:330–340.
MacDermid JC, Roth JH, Richards RS. Pain and disability reported in the year following a distal radius fracture: a cohort study. BMC Musculoskelet Disord. 2003;4:24.
McQueen M, Caspers J. Colles fracture: does the anatomical result affect the final function? J Bone Joint Surg Br. 1988;70:649–651.
Nygaard M, Nielsen NS, Bojsen-Moller F. A biomechanical evaluation of the relative load change in the joints of the wrist with ulnar shortening: a “handbag” model. J Hand Surg Eur Vol. 2009;34:724–729.
Scheer JH, Adolfsson LE. Radioulnar laxity and clinical outcome do not correlate after a distal radius fracture. J Hand Surg Eur Vol. 2011;36:503–508.
Souer JS, Lozano-Calderon SA, Ring D. Predictors of wrist function and health status after operative treatment of fractures of the distal radius. J Hand Surg Am. 2008;33:157–163.
Taleisnik J, Watson HK. Midcarpal instability caused by malunited fractures of the distal radius. J Hand Surg Am. 1984;9:350–357.
Villar RN, Marsh D, Rushton N, Greatorex RA. Three years after Colles’ fracture: a prospective review. J Bone Joint Surg Br. 1987;69:635–638.
Young BT, Rayan GM. Outcome following nonoperative treatment of displaced distal radius fractures in low-demand patients older than 60 years. J Hand Surg Am. 2000;25:19–28.
Acknowledgments
We thank Mats Billsten for help with data acquisition and Gunilla Persson for administrative assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she, or a member of his or her immediate family, has no funding or commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Each author certifies that his or her institution approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent for participation in the study was obtained.
This work was performed at the Department of Orthopedics Hässleholm-Krisitianstad, Hässleholm Hospital, Hässleholm, Sweden.
About this article
Cite this article
Brogren, E., Wagner, P., Petranek, M. et al. Distal Radius Malunion Increases Risk of Persistent Disability 2 Years After Fracture: A Prospective Cohort Study. Clin Orthop Relat Res 471, 1691–1697 (2013). https://doi.org/10.1007/s11999-012-2767-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-012-2767-8