Abstract
Background
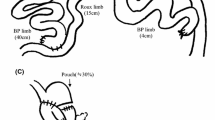
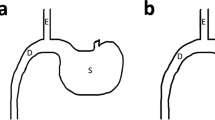
Despite the beneficial hypoglycemic and potentially curative effects in type 2 diabetes, large stomach volume deficits caused by Roux-en-Y gastrointestinal bypass (RYGB) surgery increase complications. Hypoglycemic effects of Braun surgery and RYGB surgery, both modified to maximally preserve stomach volume, were compared in rat type 2 diabetes models.
Methods
Three-month-old, male Goto-Kakizaki (GK) rats (n = 40) were randomly divided into equal groups and not treated (control) or treated with sham surgery (sham group), modified stomach-preserving Braun gastrointestinal bypass (Braun group), or modified RYGB (RYGB group). Pre- and postoperative body weight and water intake were recorded, along with operative and defecation times. Fasting blood glucose at 12 h, and blood glucose 180 min after intragastric glucose administration, were measured at weeks 1, 2, 3, 4, 10, and 11 along with glycosylated hemoglobin (preoperatively, week 11).
Results
Statistically similar (P > 0.05) increased body weight and decreased water intake, fasting blood glucose, blood glucose after intragastric glucose administration, and glycosylated hemoglobin were observed in Braun and RYGB groups compared with control and sham groups (P < 0.05). By week 1, RYGB and Braun groups exhibited sustained reductions in fasting blood glucose from 13.0 ± 4.1 to 6.9 ± 1.4 mmol/L and 12.4 ± 4.4 to 7.3 ± 0.9 mmol/L, respectively (P < 0.05); mean operative times were 139.1 ± 4.9 and 81.6 ± 6.4 min, respectively; and postoperative defecation times were 74.3 ± 3.1 and 29.4 ± 4.1 h, respectively (P < 0.05).
Conclusions
Stomach volume-preserving Braun gastrointestinal bypass surgery was faster and produced hypoglycemic effects similar to RYGB bypass surgery, potentially minimizing metabolic disruption.






Similar content being viewed by others
References
Narayan KM, Gregg EW, Fagot-Campagna A, et al. Diabetes—a common, growing, serious, costly, and potentially preventable public health problem. Diabetes Res Clin Pract. 2000;50 Suppl 2:S77–84.
Hofso D, Jenssen T, Hager H, et al. Fasting plasma glucose in the screening for type 2 diabetes in morbidly obese subjects. Obes Surg. 2010;20:302–7.
Liebl A, Mata M, Eschwege E. Evaluation of risk factors for development of complications in type II diabetes in Europe. Diabetologia. 2002;45:S23–8.
Dixon JB, le Roux CW, Rubino F, et al. Bariatric surgery for type 2 diabetes. Lancet. 2012;379:2300–11.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med. 2012;366:1577–85.
Shukla AP, Moreira M, Dakin G, et al. Medical versus surgical treatment of type 2 diabetes: the search for level 1 evidence. Surg Obes Relat Dis. 2012;8:476–82.
Rubino F, R’Bibo SL, del Genio F, et al. Metabolic surgery: the role of the gastrointestinal tract in diabetes mellitus. Nat Rev Endocrinol. 2010;6:102–9.
Ahn SM, Pomp A, Rubino F. Metabolic surgery for type 2 diabetes. Ann N Y Acad Sci. 2010;1212:E37–45.
Rubino F, Kaplan LM, Schauer PR, et al. The diabetes surgery summit consensus conference: recommendations for the evaluation and use of gastrointestinal surgery to treat type 2 diabetes mellitus. Ann Surg. 2010;251:399–405.
Dixon JF, Zimmet P, Alberti KG, et al. Bariatric surgery: an IDF statement for obese type 2 diabetes. Diabet Med. 2011;28(6):628–42.
Nathan DM, Buse JB, Davidson MB, et al. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy. A consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2009;32(1):193–203.
Brolin RE. Update: NIH consensus conference. Gastrointestinal surgery for severe obesity. Nutrition. 1996;12:403–4.
Seyfried F, Lannoo M, Gsell W, et al. Roux-en-Y gastric bypass in mice—surgical technique and characterisation. Obes Surg. 2012;22(7):1117–25.
Mingrone G. Role of the incretin system in the remission of type 2 diabetes following bariatric surgery. Nutr Metab Cardiovasc Dis. 2008;18:574–9.
Nguyen NT, Gelfand DV, Zainabadi K. Laparoscopic Roux-en-Y gastric bypass vs. laparoscopic adjustable gastric banding for treatment of morbid obesity. Surg Technol Int. 2004;12:111–9.
Lee TI, Chen JH, Weng TC, et al. Gastric bypass and diabetes: past, present and future. Curr Diabetes Rev. 2011;7:305–12.
Ballantyne GH, Wasielewski A, Saunders JK. The surgical treatment of type II diabetes mellitus: changes in homa insulin resistance in the first year following laparoscopic Roux-en-Y gastric bypass (LRYGB) and laparoscopic adjustable gastric banding (LAGB). Obes Surg. 2009;19:1297–303.
Guidone C, Manco M, Valera-Mora E, et al. Mechanisms of recovery from type 2 diabetes after malabsorptive bariatric surgery. Diabetes. 2006;55:2025–31.
Diniz MD, Beleigoli AM, Coelho AL, et al. Type 2 diabetes mellitus 5 to 10 years after Roux-en-Y gastric bypass: remission and relapses—a longitudinal prospective study. Surg Obes Relat Dis. 2013;9(3):487–8.
Tait LF, Ortega G, Tran DD, et al. Resolution of uncontrolled type 2 diabetes after laparoscopic truncal vagotomy, subtotal gastrectomy, and Roux-en-Y gastrojejunostomy for a patient with intractable gastric ulcers. Case Rep Surg. 2012;2012:102752.
Lakdawala M, Shaikh S, Bandukwala S, et al. Roux-en-Y gastric bypass stands the test of time: 5-year results in low body mass index (30–35 kg/m(2)) Indian patients with type 2 diabetes mellitus. Surg Obes Relat Dis. 2013;9(3):370–8.
Graessler J, Qin Y, Zhong H, et al. Metagenomic sequencing of the human gut microbiome before and after bariatric surgery in obese patients with type 2 diabetes: correlation with inflammatory and metabolic parameters. Pharmacogenomics J. 2012. doi:10.1038/tpj.2012.43.
Gautier T, Sarcher T, Contival N, et al. Indications and mid-term results of conversion from sleeve gastrectomy to Roux-en-Y gastric bypass. Obes Surg. 2013;23:212–5.
Jimenez A, Casamitjana R, Flores L, et al. Long-term effects of sleeve gastrectomy and Roux-en-Y gastric bypass surgery on type 2 diabetes mellitus in morbidly obese subjects. Ann Surg. 2012;256:1023–9.
Dorman RB, Rasmus NF, al-Haddad BJ, et al. Benefits and complications of the duodenal switch/biliopancreatic diversion compared to the Roux-en-Y gastric bypass. Surgery. 2012;152:758–65. discussion 765–757.
Henneman D, Lagarde S, Geubbels N, et al. Complications after laparoscopic Roux-en-Y gastric bypass: a diagnostic challenge. Report of three cases and review of the literature. G Chir. 2012;33:209–17.
Hoya Y, Mitsumori N, Yanaga K. The advantages and disadvantages of a Roux-en-Y reconstruction after a distal gastrectomy for gastric cancer. Surg Today. 2009;39:647–51.
Lindecken KD, Salm B. The effectiveness of Braun’s anastomosis in billroth ii surgery. The role of hepatobiliary sequence scintigraphy (HBSS) in the diagnosis of bile flow following stomach resection. Rofo. 1993;159:158–60.
Nakao K, Fujiwara Y, Itoh R, et al. Afferent loop obstruction with pancreatitis after distal partial gastrectomy with B-II reconstruction added Braun anastomosis for cancer of the stomach. Hepatogastroenterology. 2003;50:893–6.
Pan Y, Li Q, Wang DC, et al. Beneficial effects of jejunal continuity and duodenal food passage after total gastrectomy: a retrospective study of 704 patients. Eur J Surg Oncol. 2008;34:17–22.
Naslund E, Backman L, Holst JJ, et al. Importance of small bowel peptides for the improved glucose metabolism 20 years after jejunoileal bypass for obesity. Obes Surg. 1998;8:253–60.
Poulos JE, Leggett-Frazier N, Khazanie P, et al. Circulating insulin-like growth factor I concentrations in clinically severe obese patients with and without NIDDM in response to weight loss. Horm Metab Res. 1994;26:478–80.
Kellum JM, Kuemmerle JF, O’Dorisio TM, et al. Gastrointestinal hormone responses to meals before and after gastric bypass and vertical banded gastroplasty. Ann Surg. 1990;211:763–70. discussion 770–761.
Rubino F, Gagner M. Potential of surgery for curing type 2 diabetes mellitus. Ann Surg. 2002;236:554–9.
Mason EE. Ileal [correction of ilial] transposition and enteroglucagon/glp-1 in obesity (and diabetic?) surgery. Obes Surg. 1999;9:223–8.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222:339–50. discussion 350–332.
Pories WJ, Albrecht RJ. Etiology of type II diabetes mellitus: role of the foregut. World J Surg. 2001;25:527–31.
Conflict of Interest
The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sun, W., Dai, X., Li, J. et al. Braun Gastrointestinal Bypass Surgery Exerts Similar Hypoglycemic Effects, with Minimal Operation Time and Earlier Functional Recovery, than Roux-en-Y Bypass in Type 2 Diabetic Rats. OBES SURG 24, 171–178 (2014). https://doi.org/10.1007/s11695-013-1102-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-013-1102-0