Background
This study examines 1,791 consecutive laparoscopic adjustable gastric banding (LAGB) procedures with up to 12 years follow-up. Long-term results of LAGB with a high follow-up rate are not common.
Methods
Between September 1993 and December 2005, 1,791 consecutive patients (75.1% women, mean age 38.7 years, mean weight 127.7 ± 24 kg, mean BMI 46.2 ± 7.7) underwent LAGB by the same surgical team. Perigastric dissection was used in 77.8% of the patients, while subsequently pars flaccida was used in 21.5% and a mixed approach in 0.8%. Data were analyzed according to co-morbidities, conversion, shortand long-term complications and weight loss. Fluoroscopy-guided band adjustments were performed and patients received intensive follow-up. The effects of LAGB on life expectancy were measured in a case/control study involving 821 surgically-treated patients versus 821 treated by medical therapy.
Results
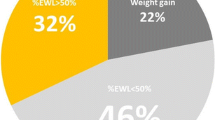
Most common baseline co-morbidities (%) were hypertension (35.6), osteoarthritis (57.8), diabetes (22), dyslipidemia (27.1), sleep apnea syndrome (31.4), depression (21.2), sweet eating (22.5) and binge eating (18.5). Conversion to open was 1.7%: due to technical difficulties (1.2) and due to intraoperative complications (0.5).Together with the re-positioning of the band, additional surgery was performed in 11.9% of the patients: hiatal hernia repair (2.4), cholecystectomy (7.8) and other procedures (1.7). There was no mortality. Reoperation was required in 106 patients (5.9%): band removal 55 (3.7%), band repositioning 50 (2.7%), and other 1 (0.05%). Port-related complications occurred in 200 patietns (11.2%). 41 patients (2.3%) underwent further surgery due to unsatisfactory results: removal of the band in 12 (0.7%), biliopancreatic diversion in 5 (0.27%) and a biliopancreatic diversion with gastric preservation (“bandinaro”) in 24 (1.3%). Weight in kg was 103.7 ± 21.6, 102.5 ± 22.5, 105.0 ± 23.6, 106.8 ± 24.3, 103.3 ± 26.2 and 101.4 ± 27.1 at 1, 3, 5, 7, 9, 11 years after LAGB. BMI at the same intervals was 37.7 ± 7.1, 37.2 ± 7.2, 38.1 ± 7.6, 38.5 ± 7.9, 37.5 ± 8.5 and 37.7 ± 9.1. The case/control study found a statistically significant difference in survival in favor of the surgically-treated group.
Conclusions
LAGB can achieve effective, safe and stable long-term weight loss. In experienced hands, the complication rate is low. Follow-up is paramount.
Similar content being viewed by others
References
Buchwald H, Williams SE. Bariatric surery worldwide 2003. Obes Surg 2004; 14: 1157–64.
Gastrointestinal surgery for severe obesity. National Institutes of Health Consensus Development Conference Draft Statement. Obes Surg 1991; 1: 257–65.
Favretti F, Cadiére G, Segato G et al. Laparoscopic banding: selection and technique in 830 patients. Obes Surg 2002: 12: 385–90.
Fielding G, Allen J. A step-by-step guide to placement of the Lap-Band adjustable gastric banding system. Am J Surg 2002; 184 (Suppl): 26S–30S.
Weiner S, Engert R, Weiner S. Outcome after laparoscopic adjustable gastric banding — 8 years experience. Obes Surg 2003; 13: 427–34.
Busetto L, Sergi G, Enzi G et al. Short term effects of weight loss on the cardiovascular risk factors in morbidly obese patients. Obes Res 2004; 12: 1–8.
Busetto L, Mazza M, Mirabelli D et al. Total mortality in morbid obese patients treated with laparoscopic adjustable gastric banding: a case-control study. Obes Metab 2006; 2 (Suppl): 365 (abst).
Cadiere GB, Favretti F, Himpens J et al. Anneau gastrique et derivation bilio-pancreatique par laparoscopie. Le Journal de Cielio-chirurgie 2001; 38: 32–5.
Fielding GA, Duncombe J. Clinical and radiological followup of laparoscopic adjustable gastric bands, 1998 and 2000: A comparison of two techniques. Obes Surg 2005; 15: 634–40.
O’Brien PE, Dixon JB, Laurie C et al. A prospective randomized trial of placement of the laparoscopic adjustable gastric band: comparison of the perigastric and pars flaccida pathways. Obes Surg 2005’ 15: 820–6.
Dargent J. Pouch dilatation and slippage after adjustable gastric banding: Is it still an issue? Obes Surg 2003; 13: 111–5.
Chevallier J-M, Zinzindohoue F, Douard R et al. Complications after laparoscopic adjustable gastric banding for morbid obesity: experience with 1,000 patients over 7 years. Obes Surg 2004; 14: 407–14.
Parikh MS, Fielding GA, Ren CJ. U.S. experience with 749 laparoscopic adjustable gastric bands: intermediate outcomes. Surg Endosc 2005; 19: 1631–5.
Ponce J, Paynter S, Fromm R. Laparoscopic adjustable gastric banding: 1,014 consecutive cases. J Am Coll Surg 2005; 201: 529–35.
O’Brien P, Dixon J. Weight loss and early and late complications — the international experience. Am J Surg 2002; 184: 42S–45S.
Favretti F, Cadiere G, Segato G et al. Laparoscopic adjustable silicone gastric banding (Lap-Band®): How to avoid complications. Obes Surg 1997; 7: 352–8.
Niville E, Dams A, Van Der Speeten K et al. Results of lap rebanding procedures after Lap-Band removal for band erosion — a mid-term evaluation. Obes Surg 2005; 15: 630–3.
Dargent J. Surgical treatment of morbid obesity by adjustable gastric band: the case for a conservative strategy in the case of failure — a 9-year series. Obes Surg 2004; 14: 986–90.
Belachew M, Belva PH, Desaive C. Long-term results of laparoscopic adjustable gastric banding for the treatment of morbid obesity. Obes Surg 2002; 12: 564–8.
Angrisani L, Alkilani M, Basso N. Laparoscopic Italian experience with the Lap-Band®. Obes Surg 2001; 11: 307–10.
Busetto L, Segato G, De Luca M et al. Preoperative weight loss by intragastric balloon in super-obese patients treated with laparoscopic gastric banding: a case-control study. Obes Surg 2004; 14: 1–6.
Deitel M, Greenstein RJ. Recommendations for reporting weight loss. Obes Surg 2003; 13: 159–60.
Goldstein DJ. Beneficial health effects of modest weight loss. Int J Obes 1992; 16: 397–415.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Favretti, F., Segato, G., Ashton, D. et al. Laparoscopic Adjustable Gastric Banding in 1,791 Consecutive Obese Patients: 12-Year Results. OBES SURG 17, 168–175 (2007). https://doi.org/10.1007/s11695-007-9043-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9043-0