ABSTRACT
OBJECTIVES
Despite the known adverse effects of sleep deprivation on recovery from illness, studies have shown that sleep deprivation remains an incompletely addressed problem among acutely ill inpatients. Behavioral interventions are recommended as first-line therapy prior to using pharmacologic therapy due to the side effects of sedative hypnotics. The objective of this systematic review was to identify non-pharmacologic interventions that have been used to improve sleep quality and quantity of non-intensive care unit (ICU) inpatients.
DATA SOURCES
PubMed, Embase, Web of Science, CINAHL, and Cochrane Library through January 2013; manual searches of reference lists.
STUDY ELIGIBILITY CRITERIA, PARTICIPANTS, INTERVENTIONS
Any study in which a non-pharmacologic intervention was conducted in a general inpatient setting, and nighttime sleep quantity or quality was assessed.
STUDY APPRAISAL AND SYNTHESIS METHODS
Information on study design, populations, interventions, comparators, outcomes, time frame, and risk of bias were independently abstracted by two investigators.
RESULTS
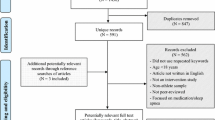
13 intervention studies with 1,154 participants were included. Four studies were randomized controlled trials. Seven studies had a low to medium risk of bias, and there was significant heterogeneity in the interventions. Relaxation techniques improved sleep quality 0–38 %, interventions to improve sleep hygiene or reduce sleep interruptions improved sleep quantity 5 %, and daytime bright light exposure improved sleep quantity 7–18 %.
LIMITATIONS
The heterogeneity in the types and dose of interventions, outcome measures, length of follow-up, differences in patient populations, and dearth of randomized trials may dilute effects seen or make it more difficult to draw conclusions.
CONCLUSIONS AND IMPLICATIONS OF KEY FINDINGS
There is insufficient to low strength of evidence that any non-pharmacologic intervention improves sleep quality or quantity of general inpatients. Further studies are needed in this area to guide clinicians.

Similar content being viewed by others
REFERENCES
Murphy WJ, Rui H, Longo DL. Effects of growth hormone and prolactin immune development and function. Life Sci. 1995;57(1):1–14.
Spiegel K, Follenius M, Simon C, Saini J, Ehrhart J, Brandenberger G. Prolactin secretion and sleep. Sleep. 1994;17(1):20–27.
Redwine LHR, Gillin JC, Irwin M. Effects of sleep and sleep deprivation on interleukin-6, growth hormone, cortisol, and melatonin levels in humans. J Clin Endocrinol Metabol. 2000;85(10):6.
Palmblad JPB, Wasserman J, Akerstedt T. Lymphocyte and Granulocyte Reactions during sleep deprivation. Psychosom Med. 1979;41(4):5.
Palmblad J, Cantell K, Strander H, et al. Stressor exposure and immunological response in man: interferon-producing capacity and phagocytosis. J Psychosom Res. 1976;20(3):193–199.
Van Cauter E. Review Article—Sleep disturbances and insulin resistance. Diabet Med. 2011;28(12):1455–1462.
Broussard JL, Erhrmann DA, Cauter EV, Tasali E, Brady MJ. Impaired insulin signaling in human adipocytes after experimental sleep restriction: A randomized, crossover study. Ann Intern Med. 2012;157(8):549–557.
Cappuccio FP, Miller MA. A new challenge to widely held views on the role of sleep. Ann Intern Med. 2012;157:593–594.
Arora VM, Fazal AZ, Zee PC, Knutson KL. Objective sleep duration and quality in hospitalized older adults: Associations with blood pressure and mood. J Am Geriatr Soc. 2011;59(11):2185–2186.
Smith MT, Klick B, Koachik S, et al. Sleep onset insomnia symptoms during hospitalization for major burn injury predict chronic pain. Pain. 2008;138(3):497–506.
Griffiths M, Peerson A. Risk factors for chronic insomnia following hospitalization. J Adv Nurs. 2005;49(3):245–253.
Gay P. Sleep and sleep-disordered breathing in the hospitalized patient. Respir Care. 2010;55(9):1240–1254.
Frighetto L, Marra C, Bandali S, Wilbur K, Naumann T, Jewesson P. An assessment of quality of sleep and the use of drugs with sedating properties in hospitalized adult patients. Health Qual Life Outcome. 2004;2:17.
Southwell MT, Wistow G. Sleep in hospitals at night: are patients’ needs being met? J Adv Nurs. 1995;21(6):1101–1109.
Raymond I, Ancoli-Israel S, Choiniere M. Sleep disturbances, pain and analgesia in adults hospitalized for burn injuries. Sleep Med. 2004;5(6):551–559.
Manabe K, Matsui T, Yamaya M, et al. Sleep patterns and mortality among elderly patients in a geriatric hospital. Gerontology. 2000;46(6):318–322.
Flaherty JH. Insomnia among hospitalized older persons. Clin Geriatr Med. 2008;24(1):51–67. vi.
Tranmer JE, Minard J, Fox LA, Rebelo L. The sleep experience of medical and surgical patients. Clin Nurs Res. 2003;12(2):159–173.
Topf M, Thompson S. Interactive relationships between hospital patients’ noise-induced stress and other stress with sleep. Heart Lung. 2001;30(4):237–243.
Young JS, Bourgeois JA, Hilty DM, Hardin KA. Sleep in hospitalized medical patients, part 1: factors affecting sleep. J Hosp Med. 2008;3(6):473–482.
Young JS, Bourgeois JA, Hilty DM, Hardin KA. Sleep in hospitalized medical patients, part 2: behavioral and pharmacological management of sleep disturbances. J Hosp Med. 2009;4(1):50–59.
Glass J, Lactot KL, Herrmann N, Sproule BA, Busto UE. Sedative hypnotics in older people with insomnia: meta-analysis of risks and benefits. Br Med J (Clin Res Ed). 2005;331:1169–1175.
Kolla BP, Lovely JK, Mansukhani MP, Morgenthaler TI. Zolpidem is independently associated with increased risk of inpatient falls. J Hosp Med. 2013;8(1):1–6.
Jarman H, Jacobs E, Walter R, Witney C, Zielinski V. Allowing the patients to sleep: flexible medication times in an acute hospital. Int J Nurs Pract. 2002;8(2):75–80.
Lenhart SE, Buysse DJ. Treatment of insomnia in hospitalized patients. Ann Pharmacother. 2001;35:1449–1457.
Blair B, Martin J. Toward a good night’s sleep: An approach to insomnia in older patients. Consultant. 2012;52(12):795–803.
Suggested risk of bias criteria for EPOC reviews. Cochrane Effective Practice and Organization of Care Group. Available at http://epoc.cochrane.org/epoc-resources. Accessed September 4, 2013.
Methods Guide for Effectiveness and Comparative Effectiveness Reviews. Agency for Healthcare Research and Quality. Available at http://effectivehealthcare.ahrq.gov/index.cfm/search-for-guides-reviews-and-reports/?productid=318&pageaction=displayproduct. Accessed September 4, 2013.
Owens DK, Lohr KN, Atkins D, et al. AHRQ Series Paper 5: Grading the strength of a body of evidence when comparing medical interventions. J Clin Epidemiol. 2010;63:513–523.
Lareau R, Benson L, Watcharotone K, Manguba G. Examining the feasibility of implementing specific nursing interventions to promote sleep in hospitalized elderly patients. Geriatr Nurs. 2008;29(3):197–206.
Soden K, Vincent K, Craske S, Lucas C, Ashley S. A randomized controlled trial of aromatherapy massage in a hospice setting. Palliat Med. 2004;2:87–92.
Toth M, Wolsko PM, Foreman J, et al. A pilot study for a randomized, controlled trial on the effect of guided imagery in hospitalized medical patients [5]. J Alternative Compl Med. 2007;13(2):194–197.
Zimmerman L, Nieveen J, Barnason S, Schmaderer M. The effects of music interventions on postoperative pain and sleep in coronary artery bypass graft (CABG) patients… including commentary by Miaskowski C. Sch Inq Nurs Pract. 1996;10(2):153–174.
Williamson JW. The effects of ocean sounds on sleep after coronary artery bypass graft surgery. Am J Crit Care. 1992;1(1):91–97.
McDowell JA, Mion LC, Lydon TJ, Inouye SK. A nonpharmacologic sleep protocol for hospitalized older patients. J Am Geriatr Soc. 1998;46(6):700–705.
Smith MC, Kemp J, Hemphill L, Vojir CP. Outcomes of therapeutic massage for hospitalized cancer patients. J Nurs Scholarsh. 2002;34(3):257–262.
Connell FEA, Tan G, Gupta I, Gompertz P, Bennett GCJ, Herzberg JL. Can aromatherapy promote sleep in elderly hospitalized patients? Geriatr Today. 2001;4(4):191–195.
Bartick MC, Thai X, Schmidt T, Altaye A, Solet JM. Decrease in as-needed sedative use by limiting nighttime sleep disruptions from hospital staff. J Hosp Med. 2010;5(3):E20–24.
Edinger JD, Lipper S, Wheeler B. Hospital ward policy and patients’ sleep patterns: a multiple baseline study. Rehabil Psychol. 1989;34(1):43–50.
Mishima K, Okawa M, Hishikawa Y, Hozumi S, Hori H, Takahashi K. Morning bright light therapy for sleep and behavior disorders in elderly patients with dementia. Acta Psychiatr Scand. 1994;89:1–7.
Wakamura T, Tokura H. Influence of bright light during daytime on sleep parameters in hospitalized elderly patients. J Physiol Anthropol Appl Human Sci. 2001;20(6):345–351.
Yamadera H, Ito T, Suzuki H, Asayama K, Ito R, Endo S. Effects of bright light on cognitive and sleep-wake (circadian) rhythm disturbances in Alzheimer-type dementia. Psychiatry Clin Neurosci. 2000;54:352–353.
Bonnett MHAD. Heart rate variability in insomniacs and matched normal sleepers. Psychosom Med. 1998;60(5):610–615.
Brown THMT. The Influence of PTSD, Sleep Fears, and Neighborhood Stress on Insomnia and Short Sleep Duration in Urban, Young Adult African Americans. Behav Sleep Med. 2013;11:1–9.
Kompier MATT, van Veldhoven M. Tossing and turning–insomnia in relation to occupational stress, rumination, fatigue, and well-being. Scan J Work Environ Health. 2012;38(3):238–246.
Gross CRKM, Reilly-Spong M, Wall M, Winbush NY, Patterson R, Mahowald M, Cramer-Bornemann M. Mindfulness-based stress reduction versus pharmacotherapy for chronic primary insomnia: a randomized controlled clinical trial. Explore. 2011;7(2):76–87.
Hoge EAML, Metcalf CA, Morris LK, Robinaugh DJ, Worthington JJ, Pollack MH, Simon NM. Randomized controlled trial of mindfulness meditation for generalized anxiety disorder: effects on anxiety and stress reactivity. J Clin Psychiatry. 2013;74.
Nakamura YLD, Kuhn R, Donaldson GW. Investigating efficacy of two brief mind-body intervention programs for managing sleep disturbance in cancer survivors: a pilot randomized controlled trial. J Cancer Surviv. 2013;7(2):165–182.
Czeisler CA, Richardson GS, Zimmerman JC, Moore-Ede MC, Weitzman ED. Entrainment of human circadian rhythms by light–dark cycles: a reassessment. Photochem Photobiol. 1981;34(2):239–247.
Acknowledgements
The authors thank Daniel J. Brotman, MD, Johns Hopkins University for his thoughtful comments during preparation of the manuscript. No compensation was given for his contributions. All authors had full access to the data in the study and take full responsibility for the integrity of the data and the accuracy of the analysis.
No funding was received for this work.
An earlier version of this work was presented at the Society of General Internal Medicine Annual Conference in Denver, CO in April 2013.
Author Contributions
All authors contributed to the collection, extraction, synthesis, and analysis of the data for this systematic review.
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author Contributions
All authors contributed to the collection, extraction, synthesis, and analysis of the data for this systematic review.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 124 kb)
Rights and permissions
About this article
Cite this article
Tamrat, R., Huynh-Le, MP. & Goyal, M. Non-Pharmacologic Interventions to Improve the Sleep of Hospitalized Patients: A Systematic Review. J GEN INTERN MED 29, 788–795 (2014). https://doi.org/10.1007/s11606-013-2640-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-013-2640-9