ABSTRACT
BACKGROUND
Archetypal symptoms and signs are commonly absent in frail older people who are acutely unwell. This challenges both recognition of illness and monitoring of disease progression in people at high risk of prolonged hospital stays, institutionalization and death.
OBJECTIVE
To determine whether bedside assessment of balance and mobility could track acute changes in the health status of older people admitted to hospital.
DESIGN
Prospective cohort study.
PARTICIPANTS
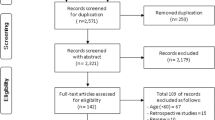
Four hundred nine patients, with a mean age of 81.8 years, admitted to general medical and rehabilitation wards at a tertiary care teaching hospital in Halifax, Nova Scotia. No patient refused assessment, and the only exclusion criterion was age.
INTERVENTIONS
The Hierarchical Assessment of Balance and Mobility (HABAM) was completed daily during the first 2 weeks of admission. For each patient, frailty status was measured on admission by a Frailty Index based on a Comprehensive Geriatric Assessment (FI-CGA).
MAIN MEASURES
Death and discharge destination.
KEY RESULTS
Poor performance in balance, transfers and mobility was associated with adverse outcomes. Forty-eight percent of patients with the lowest scores in all three domains died, compared with none with the highest scores. The relative risk of death for people who deteriorated during the first 48 h of admission was 17.1 (95% confidence interval: 4.9–60.3). Changes in HABAM scores were related to the discharge destination: patients discharged home showed the greatest rate of improvement, whereas those discharged to institutions stabilised at a lower level of performance. Fitter patients tended to have better performance on admission and faster recovery.
CONCLUSIONS
Daily bedside observation of mobility and balance allows assessment of acute changes in the health of older people. Frailty slows recovery of mobility and balance, and reduces recovery potential. By identifying patients most vulnerable to adverse outcomes, the HABAM and FI-CGA may facilitate risk stratification in older people admitted to hospital.




Similar content being viewed by others
REFERENCES
Janssens JP, Krause KH. Pneumonia in the very old. Lancet Infect Dis. 2004;4:112–24.
Matsuno O, Kataoka H, Takenaka R, et al. Influence of age on symptoms and laboratory findings at presentation in patients with influenza-associated pneumonia. Arch Gerontol Geriatr. 2009;49:322–5.
Chong CP, Street PR. Pneumonia in the elderly: a review of the epidemiology, pathogenesis, microbiology, and clinical features. South Med J. 2008;101:1141–5.
Basi SK, Marrie TJ, Huang JQ, Majumdar SR. Patients admitted to hospital with suspected pneumonia and normal chest radiographs: epidemiology, microbiology, and outcomes. Am J Med. 2004;117:305–11.
Inouye SK, Studenski S, Tinetti ME, Kuchel GA. Geriatric syndromes: clinical, research, and policy implications of a core geriatric concept. J Am Geriatr Soc. 2007;55:780–91.
Jarrett PG, Rockwood K, Carver D, Stolee P, Cosway S. Illness presentation in elderly patients. Arch Intern Med. 1995;155:1060–4.
Isaacs B. Some characteristics of geriatric patients. Scott Med J. 1969;14:243–51.
Cigolle CT, Langa KM, Kabeto MU, Tian Z, Blaum CS. Geriatric conditions and disability: the health and retirement study. Ann Intern Med. 2007;147:156–64.
Davis DHJ, Rockwood MRH, Mitnitski AB, Rockwood K. Impairments in mobility and balance in relation to frailty. Arch Gerontol Geriatr 2010; [In press]. PMID: 20678816.
Gill TM, Allore HG, Hardy SE, Guo Z. The dynamic nature of mobility disability in older persons. J Am Geriatr Soc. 2006;54:248–54.
MacKnight C, Rockwood K. A hierarchical assessment of balance and mobility. Age Ageing. 1995;24:126–30.
MacKnight C, Rockwood K. Rasch analysis of the hierarchical assessment of balance and mobility (HABAM). J Clin Epidemiol. 2000;53:1242–7.
Rockwood K, Rockwood MRH, Andrew MK, Mitnitski A. Reliability of the hierarchical assessment of balance and mobility in frail older adults. J Am Geriatr Soc. 2008;56:1213–7.
Jones DM, Song X, Rockwood K. Operationalizing a frailty index from a standardized comprehensive geriatric assessment. J Am Geriatr Soc. 2004;52:1929–33.
Jones D, Song X, Mitnitski A, Rockwood K. Evaluation of a frailty index based on a comprehensive geriatric assessment in a population based study of elderly Canadians. Aging Clin Exp Res. 2005;17:465–71.
Kelsey JL, Whittemore AS, Evans AS, Thomson WD. Methods in Observational Epidemiology. 2nd ed. Oxford: Oxford University Press; 1996.
Rockwood K, Andrew M, Mitnitski A. A comparison of two approaches to measuring frailty in elderly people. J Gerontol A Biol Sci Med Sci. 2007;62:738–43.
Rockwood K, Song X, MacKnight C, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173:489–95.
de Morton NA, Berlowitz DJ, Keating JL. A systematic review of mobility instruments and their measurement properties for older acute medical patients. Health Qual Life Outcomes. 2008;6:44.
Pérennou D, Decavel P, Manckoundia P, et al. Evaluation of balance in neurologic and geriatric disorders. Ann Readapt Med Phys. 2005;48:317–35.
de Morton NA, Davidson M, Keating JL. The de Morton Mobility Index (DEMMI): an essential health index for an ageing world. Health Qual Life Outcomes. 2008;6:63.
Guralnik JM, Simonsick EM, Ferrucci L, et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol. 1994;49:M85–94.
Mathias S, Nayak US, Isaacs B. Balance in elderly patients: the “get-up and go” test. Arch Phys Med Rehab. 1986;67:387–389.
Berg KO, Wood-Dauphinee SL, Williams JI, Gayton D. Measuring balance in the elderly: preliminary development of an instrument. Physiother Can. 1989;41:304–11.
Tinetti ME. Performance-oriented assessment of mobility problems in elderly patients. J Am Geriatr Soc. 1986;34:119–26.
Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol Biol Med Sci. 2001;56:M146–56.
Bandeen-Roche K, Xue QL, Ferrucci L, et al. Phenotype of frailty: characterization in the women’s health and aging studies. J Gerontol A Biol Sci Med Sci. 2006;61:262–6.
Gill TM, Gahbauer EA, Han L, Allore HG. Trajectories of disability in the last year of life. N Engl J Med. 2010;362:1173–80.
Gill TM, Allore HG, Gahbauer EA, Murphy TE. Change in disability after hospitalization or restricted activity in older persons. JAMA. 2010;304:1919–28.
Bauer JM, Sieber CC. Sarcopenia and frailty: a clinician’s controversial point of view. Exp Gerontol. 2008;43:674–8.
Rockwood K, Mitnitski A. Frailty in relation to the accumulation of deficits. J Gerontol A Biol Sci Med Sci. 2007;62:722–7.
Searle SD, Mitnitski A, Gahbauer EA, Gill TM, Rockwood K. A standard procedure for creating a frailty index. BMC Geriatr. 2008;8:24.
Mitnitski A, Song X, Skoog I, et al. Relative fitness and frailty of elderly men and women in developed countries and their relationship with mortality. J Am Geriatr Soc. 2005;53:2184–9.
Kulminski AM, Ukraintseva SV, Kulminskaya IV, et al. Cumulative deficits better characterize susceptibility to death in elderly people than phenotypic frailty: lessons from the cardiovascular health study. J Am Geriatr Soc. 2008;56:898–903.
Rockwood K, Rockwood MRH, Mitnitski A. Physiological redundancy in older adults in relation to the change with age in the slope of a frailty index. J Am Geriatr Soc. 2010;58:318–323.
Torres OH, Muñoz J, Ruiz D, et al. Outcome predictors of pneumonia in elderly patients: importance of functional assessment. J Am Geriatr Soc. 2004;52:1603–9.
Volpato S, Onder G, Cavalieri M, et al. Characteristics of nondisabled older patients developing new disability associated with medical illnesses and hospitalization. J Gen Intern Med. 2007;22:668–74.
Gu D, Dupre ME, Sautter J, Zhu H, Liu Y, Yi Z. Frailty and mortality among Chinese at advanced ages. J Gerontol B Psychol Sci Soc Sci. 2009;64:279–89.
Gavrilov LA, Gavrilova NS. Reliability theory of aging and longevity. In Handbook of the Biology of Aging. 6th Edition: Academic Press.
Nowak A, Hubbard RE. Falls and frailty: lessons from complex systems. J R Soc Med. 2009;102:98–102.
Funders
The study was supported by a grant from the Fountain Innovation Fund of the QEII Health Sciences Foundation. KR receives career support from the Dalhousie Medical Research Foundation as the Kathryn Allen Weldon Professor of Alzheimer Research. The sponsor had no role in the acquisition or interpretation of data, or the decision to publish. NF is supported by a postdoctoral fellowship of the Alzheimer’s Society of Canada.
Prior Presentations
This work was presented at the British Geriatrics Society Conference, November 2010.
Conflict of Interest
A commercial version of the FI-CGA, known as Videx, is being developed for semi-automated use on a handheld device. Otherwise, none of the authors has any conflicts to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hubbard, R.E., Eeles, E.M.P., Rockwood, M.R.H. et al. Assessing Balance and Mobility to Track Illness and Recovery in Older Inpatients. J GEN INTERN MED 26, 1471–1478 (2011). https://doi.org/10.1007/s11606-011-1821-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-011-1821-7