Abstract
Background
Variations in hospice use are not well understood.
Objective
Assess whether care before death, including the types of physicians seen, number of outpatient visits, and hospitalizations, was associated with hospice use and the timing of enrollment.
Design/setting
Observational study of a population-based sample of advanced breast cancer patients included in the Surveillance, Epidemiology, and End Results—Medicare database.
Patients
There were 4,455 women aged ≥65 diagnosed with stage III/IV breast cancer during 1992–1999 who died before the end of 2001.
Measurements
Hospice use and, among enrollees, enrollment within 2 weeks of death. Independent variables of interest included hospitalizations, outpatient visits, and physicians seen before death.
Results
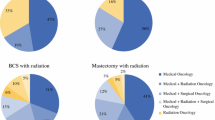
Adjusted hospice use rates were higher for hospitalized patients (45% if hospitalized for 1–7 days, 46% if 8–20 days, 35% if ≥21 days) than those not hospitalized (31%, P < 0.001). Adjusted rates were also higher among patients seeing a cancer specialist and primary care provider (PCP; 41%) and those seeing a cancer specialist and no PCP (38%) than among those seeing a PCP and no cancer specialist (30%) or neither type of physician (22%; P < 0.001). Hospice use also increased with increasing frequency of outpatient visits (P < 0.001). Hospitalizations, physicians seen, and visits were not associated with referral within 2 weeks of death (all P ≥ 0.10).
Discussion
Care before death is associated with hospice use among older women with advanced breast cancer. Additional research is needed to understand better how differences in patient characteristics and disease status influence cancer care before death and the role of various types of physicians in hospice referrals.
Similar content being viewed by others
References
Institute of Medicine, ed. Improving Palliative Care for Cancer. Washington, D.C.: National Academy Press; 2001.
Greer DS, Mor V. An overview of National Hospice Study findings. J Chronic Dis. 1986;39(1):5–7.
Greer DS, Mor V, Morris JN, Sherwood S, Kidder D, Birnbaum H. An alternative in terminal care: results of the National Hospice Study. J Chronic Dis. 1986;39(1):9–26.
Wallston KA, Burger C, Smith RA, Baugher RJ. Comparing the quality of death for hospice and non-hospice cancer patients. Med Care. 1988;26(2):177–82.
General Accounting Office. Medicare: More beneficiaries use hospice; many factors contribute to shorter periods of use. 2000 September 18, 2000.
Medicare Payment Advisory Commission (MedPAC). Report to the Congress: Medicare Beneficiaries’ Access to Hospice. 2002 May.
Medicare Payment Advisory Commission (MedPAC). Medicare’s hospice benefit: Recent trends and consideration of payment system refinements. 2006 Jun.
Berry ZS, Lynn J. Hospice medicine. JAMA. 1993;270(2):221–3.
Virnig BA, Kind S, McBean M, Fisher E. Geographic variation in hospice use prior to death. J Am Geriatr Soc. 2000;48(9):1117–25.
Lackan NA, Ostir GV, Freeman JL, Mahnken JD, Goodwin JS. Decreasing variation in the use of hospice among older adults with breast, colorectal, lung, and prostate cancer. Med Care. 2004;42(2):116–22.
Virnig BA, Persily NA, Morgan RO, DeVito CA. Do Medicare HMOs and Medicare FFS differ in their use of the Medicare hospice benefit? Hosp J. 1999;14(1):1–12.
Talamantes MA, Lawler WR, Espino DV. Hispanic American elders: caregiving norms surrounding dying and the use of hospice services. Hosp J. 1995;10(2):35–49.
Ngo-Metzger Q, McCarthy EP, Burns RB, Davis RB, Li FP, Phillips RS. Older Asian Americans and Pacific Islanders dying of cancer use hospice less frequently than older white patients. Am J Med. 2003;115(1):47–53.
Greiner KA, Perera S, Ahluwalia JS. Hospice usage by minorities in the last year of life: results from the National Mortality Followback Survey. J Am Geriatr Soc. 2003;51(7):970–8.
Lackan NA, Freeman JL, Goodwin JS. Hospice use by older women dying with breast cancer between 1991 and 1996. J Palliat Care. 2003;19(1):49–53.
Lackan NA, Ostir GV, Kuo YF, Freeman JL. The association of marital status and hospice use in the USA. Palliat Med. 2005;19(2):160–2.
McCarthy EP, Burns RB, Ngo-Metzger Q, Davis RB, Phillips RS. Hospice use among Medicare managed care and fee-for-service patients dying with cancer. JAMA. 2003;289(17):2238–45.
Virnig BA, Fisher ES, McBean AM, Kind S. Hospice use in Medicare managed care and fee-for-service systems. Am J Manag Care. 2001;7(8):777–86.
Iwashyna TJ, Chang VW, Zhang JX, Christakis NA. The lack of effect of market structure on hospice use. Health Serv Res. 2002;37(6):1531–51.
Wennberg JE, Fisher ES, Stukel TA, Skinner JS, Sharp SM, Bronner KK. Use of hospitals, physician visits, and hospice care during last six months of life among cohorts loyal to highly respected hospitals in the United States. BMJ. 2004;328(7440):607.
Earle CC, Neville BA, Landrum MB, Ayanian JZ, Block SD, Weeks JC. Trends in the aggressiveness of cancer care near the end of life. J Clin Oncol. 2004;22(2):315–21.
Keating NL, Herrinton L, Zaslavsky AM, Liu L, Ayanian JZ. Variations in hospice use among cancer patients. J Natl Cancer Inst. 2006;98:1053–9.
Navari RM, Stocking CB, Siegler M. Preferences of patients with advanced cancer for hospice care. JAMA. 2000;284(19):2449.
Bradley EH, Cramer LD, Bogardus ST, Jr., Kasl SV, Johnson-Hurzeler R, Horwitz SM. Physicians’ ratings of their knowledge, attitudes, and end-of-life-care practices. Acad Med. 2002;77(4):305–11.
Institute of Medicine, ed. Approaching death-improving care at the end of life. Washington, DC: National Academy Press; 1997.
Levinsky NG, Yu W, Ash A, et al. Influence of age on Medicare expenditures and medical care in the last year of life. JAMA. 2001;286(11):1349–55.
Christakis NA, Escarce JJ. Survival of Medicare patients after enrollment in hospice programs. N Engl J Med. 1996;335(3):172–8.
Christakis NA, Lamont EB. Extent and determinants of error in doctors’ prognoses in terminally ill patients: prospective cohort study. BMJ. 2000;320(7233):469–72.
Stillman MJ, Syrjala KL. Differences in physician access patterns to hospice care. J Pain Symptom Manage. 1999;17(3):157–63.
Lamont EB, Christakis NA. Physician factors in the timing of cancer patient referral to hospice palliative care. Cancer. 2002;94(10):2733–7.
Christakis NA, Iwashyna TJ. Impact of individual and market factors on the timing of initiation of hospice terminal care. Med Care. 2000;38(5):528–41.
Potosky AL, Riley GF, Lubitz JD, Mentnech RM, Kessler LG. Potential for cancer related health services research using a linked Medicare-tumor registry database. Med Care. 1993;31(8):732–48.
Ries LA, Wingo PA, Miller DS, et al. The annual report to the nation on the status of cancer, 1973–1997, with a special section on colorectal cancer. Cancer. 2000;88(10):2398–424.
Baldwin LM, Adamache W, Klabunde C, Kenward K, Dalhman C, Warren JL. Linking physician characteristics and Medicare claims data: issues in data availability, quality, and measurement. Med Care. 2002;40(8, Supplement):IV-82–IV-95.
American Joint Committee on Cancer. AJCC cancer staging manual, 5th edition New York, NY: Springer; 1997.
Ellis RP, Pope GC, Iezzoni LI, et al. Diagnosis-based risk adjustment for Medicare capitation payments. Health Care Financing Rev. 1996;17(3):101–28.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83.
Ash AS, Posner MA, Speckman J, Franco S, Yacht AC, Bramwell L. Using claims data to examine mortality trends following hospitalization for heart attack in Medicare. Health Serv Res. 2003;38(5):1253–62.
Baldwin LM, Klabunde CN, Green P, Barlow W, Wright G. In search of the perfect comorbidity measure for use with administrative claims data: does it exist? Med Care. 2006;44(8):745–53.
Little RJ. Direct standardization: a tool for teaching linear models for unbalanced data. Am Statistician. 1982;36:38–43.
Leape LL, Hilborne LH, Bell R, Kamberg C, Brook RH. Underuse of cardiac procedures: do women, ethnic minorities, and the uninsured fail to receive needed revascularization? Ann Intern Med. 1999;130:183–92.
Bradley EH, Fried TR, Kasl SV, Cicchetti DV, Johnson-Hurzeler R, Horwitz SM. Referral of terminally ill patients for hospice: frequency and correlates. J Palliat Care. 2000;16(4):20–6.
Iwashyna TJ, Christakis NA. Attitude and self-reported practice regarding hospice referral in a national sample of internists. J Palliat Med. 1998;1:241–8.
Warren JL, Klabunde CN, Schrag D, Bach PB, Riley GF. Overview of the SEER-Medicare data: content, research applications, and generalizability to the United States elderly population. Med Care. 2002;40(8 Suppl):IV-3–IV-18.
Locher JL, Kilgore ML, Morrisey MA, Ritchie CS. Patterns and predictors of home health and hospice use by older adults with cancer. J Am Geriatr Soc. 2006;54(8):1206–11.
Bach PB, Schrag D, Begg CB. Resurrecting treatment histories of dead patients: a study design that should be laid to rest. JAMA. 2004;292(22):2765–70.
Earle CC, Ayanian JZ. Looking back from death: the value of retrospective studies of end-of-life care. J Clin Oncol. 2006;24:838–40.
Acknowledgements
This study was funded by a Clinical Scientist Development Award from the Doris Duke Charitable Foundation.
This study used the linked SEER—Medicare database. The interpretation and reporting of these data are the sole responsibility of the authors. The authors acknowledge the efforts of the Applied Research Program, NCI; the Office of Research, Development and Information, CMS; Information Management Services (IMS), Inc.; and the Surveillance, Epidemiology, and End Results (SEER) Program tumor registries in the creation of the SEER—Medicare database.
The authors thank Laurie Meneades, M.S., for expert programming assistance.
Conflict of Interest Statement
Dr. Ayanian is a consultant to Research Triangle Institute and DxCG, Inc. on the development of DCG risk adjustment models. None of the other authors have any potential conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was funded by a Clinical Scientist Development Award to Dr. Keating from the Doris Duke Charitable Foundation. Dr. Ayanian is a consultant to Research Triangle Institute and DxCG, Inc. on the development of DCG risk adjustment models. The study was presented on April 26, 2007 at the 30th Annual Meeting of the Society of General Internal Medicine, Toronto, Ontario, Canada.
Appendix
Appendix
Current Procedure Technology codes used for identifying outpatient visits include codes 99201–99205, 99211–99215, 99241–99245, 99381–99387, 99391–99397, 99401–99404, 99411–99412, 99420–99429, 99354–99360.
Rights and permissions
About this article
Cite this article
Keating, N.L., Landrum, M.B., Guadagnoli, E. et al. Care in the Months before Death and Hospice Enrollment Among Older Women with Advanced Breast Cancer. J GEN INTERN MED 23, 11–18 (2008). https://doi.org/10.1007/s11606-007-0422-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-007-0422-y