Summary
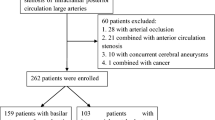
The curative efficacy of percutaneous transluminal angioplasty and stenting (PTAS) in the treatment of patients with ischemia cerebrovascular disease caused by artery stenosis was explored. The clinical data of 111 patients with ischemia cerebrovascular disease receiving PTAS in Guangdong Province General Hospital from Aug. 2007 to Nov. 2009 were retrospectively analyzed. In total 132 stents were implanted in the 111 patients. The mortality and rate of neural and non-neural complications were assessed perioperatively. Outcomes [including the frequency of transient ischemic attack (TIA), stroke, or death from vascular diseases) were assessed after operation. NIHSS rating was performed in all cases before and at first week, 6th month and 12th month after the operation. The PTAS success rate was 100%. The degree of stenosis was reduced after PTAS. The total complication rate during perioperative period was 15.3% (the rate of neural complications was 3.6%). Sixty-seven patients were followed up. Three patients (4.48%) developed cerebrovascular events within 1 month, containing one case of TIA, one case of ipsilateral mild stroke and one case of contralateral mild stroke. No severe stroke or death was observed. During a follow-up period of 12 months 7 patients had cerebrovascular events (10.44%), including 2 cases of ipsilateral TIA (2.99%), 2 cases of ipsilateral mild stroke and 2 cases of contralateral mild stroke (2.99%), one case of severe stroke (1.49%). In 13 patients receiving DSA re-examination one year after PTAS, 2 patients (15.38%) had in-stent restenosis. NIHSS scores were obviously decreased during a follow-up period as compared with those pre-operation (P<0.05). It was concluded that PTAS could significantly alleviate the neural function deficit of the patients with ischemia cerebrovascular disease. The success rate of PTAS was high, and the rate of complications was lower and the clinical outcomes were satisfactory. PTAS is a safe and effective therapeutic method, though the long-term outcomes need further study.
Similar content being viewed by others
References
Sacco RL, Kargman DE, Gu Q, et al. Race-ethnicity and determinants of intracranial atherosclerotic cerebral infarction. The Northern Manhattan Stroke Study. Stroke, 1995,26(1):14–20
Chimowitz MI, Lynn MJ, Howlett-Smith H, et al. Comparison of warfarin and aspirin for symptomatic intracranial arterial stenosis. N Engl J Med, 2005, 352(13):1305–1316
Kasner SE, Chimowitz MI, Lynn MJ, et al. Predictors of ischemic stroke in the territory of a symptomatic intracranial arterial stenosis. Circulation, 2006,113(4): 555–563
Wholey MH, Wholey M, Tan WA, et al. Management of neurologic complications of carotid artery stenting. J Endovasc Ther, 2001,8(4):341–353
Ascher E, Markevich N, Schutzer RW, et al. Cerebral hyperperfusion syndrome after carotid endarterectomy: Predictive factors and hemodynamic changes. J Vasc Surg, 2003,37(4):769–777
Endarterectomy for asymptomatic carotid artery stenosis. Executive Committee for the Asymptomatic Carotid Atherosclerosis Study. JAMA, 1995,273(18): 1421–1428
Mori T, Fukuoka M, Kazita K, et al. Follow-up study after intracranial percutaneous transluminal cerebral balloon angioplasty. AJNR, 1998,19(6):1525–1533
North American Symptomatic Carotid Endarterectomy Trial Collaborators. Beneficial effect of carotid endarterectomy in symptomatic patients with high grade carotid stenosis. N Engl J Med, 1991,325(7): 445–453
Samuels OB, Joseph JJ, Lynn MJ, et al. A standardized method for measuring intracranial arterial stenosis. AJNR, 2000,21(4):643–646
European Carotid Surgery Trial Collaborative Group. Randomized trial of endarterectomy for recently symptomatic carotid stenosis: final results of the MRC European Carotid Surgery Trial (ECST). Lancet, 1998,351(9113): 1379–1387
Barnett HJ, Taylor DW, Eliasziw M, et al. Benefit of carotid endarterectomy in patients with symptomatic moder ate or severe stenosis. North American Symptomatic Carotid Endarterectomy Trial Collaborators. N Engl J Med, 1998,339(20):1415–1425
O’Holleran LW, Kennelly MM, McClurken M, et al. Natural history of asymptomatic carotid plaque. Five year follow-up study. Am J Surg, 1987,154(6), 659–662
Reinhard M, Müller T, Roth M, et al. Bilateral severe carotid artery stenosis or occlusion-cerebral autoregulation dynamics and collateral flow patterns. Acta Neurochir (Wien), 2003,45(12):1053–1059
Gur AY, Bornstein NMRN. Cerebral vasomotor reactivity of bilateral severe carotid stenosis is stroke unavoidable? Eur J Neurol, 2006,13(2):183–186
Liistro Di-Mario C. Carotid artery sterning. Heart, 2003,89(8):944–948
Schumacher HC, Khaw AV, Meyers PM, et al. Intracranial angioplasty and stent placement for cerebral atherosclerosis. J Vasc Interv Radiol, 2004,15(1 Pt 2): S123–132
The SSYLV IA Study Investigators. Stenting of symptomatic atherosclerotic lesions in the vertebral or intracranial arteries (SSYLV IA) study results. Stroke, 2004,35(11): 1388–1392
Al-Mubarak N, Colombo A, Gaines PA, et al. Multicenter evaluation of carotid artery stenting with a filter protection system. J Am Coll Cardiol, 2002,39(5): 841–846
Nicholas GG, Hashemi H, Gee W, et al. The cerebral hyperperfusion syndrome diagnostic value of ocular pneumoplethysmography. J Vasc Surg, 1993,17(4): 690–695
Sbarigia E, Speziale F, Giannoni MF, et al. Post-carotid endarterectomy hyperperfusion syndrome: preliminary observations for identifying at risk patients by transcranial Doppler sonography and the acetazolamide test. Euro J Vasc Surg, 1993,7(3):252–256
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, X., Wang, W., Tang, Z. et al. Clinical study of PTAS therapy for patients with ischemia cerebrovascular disease caused by artery stenosis. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 31, 67–72 (2011). https://doi.org/10.1007/s11596-011-0152-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-011-0152-6