Abstract
Purpose
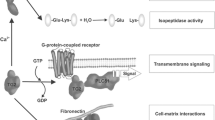
Celiac disease is an autoimmune-mediated enteropathy characterized by adaptive and innate immune responses to dietary gluten in wheat, rye and barley in genetically susceptible individuals. Gluten-derived gliadin peptides are deamidated by transglutaminase 2 (TG2), leading to an immune response in the small-intestinal mucosa. TG2 inhibitors have therefore been suggested as putative drugs for celiac disease. In this proof-of-concept study we investigated whether two TG2 inhibitors, cell-impermeable R281 and cell-permeable R283, can prevent the toxic effects of gliadin in vitro and ex vivo.
Methods
Intestinal epithelial Caco-2 cells were treated with peptic-tryptic-digested gliadin (PT-gliadin) with or without TG2 inhibitors and thereafter direct toxic effects (transepithelial resistance, cytoskeletal rearrangement, junction protein expression and phoshorylation of extracellular-signal-regulated kinase 1/2) were determined. In an organ culture of celiac-patient-derived small-intestinal biopsies we measured secretion of TG2-autoantibodies into the culture medium and the densities of CD25- and interleukin (IL) 15-positive cells, forkhead box P3 (FOXP3)-positive regulatory T cells (Tregs) and Ki-67-positive proliferating crypt cells.
Results
Both TG2 inhibitors evinced protective effects against gliadin-induced detrimental effects in Caco-2 cells but the cell-impermeable R281 seemed slightly more potent. In addition, TG2 inhibitor R281 modified the gluten-induced increase in CD25- and IL15-positive cells, Tregs and crypt cell proliferation, but had no effect on antibody secretion in celiac-patient-derived biopsies.
Conclusions
Our results suggest that TG2 inhibitors are able to reduce certain gliadin-induced effects related to responses in vitro and ex vivo.





Similar content being viewed by others
References
Sulkanen S, Halttunen T, Laurila K, et al. Tissue transglutaminase autoantibody enzyme-linked immunosorbent assay in detecting celiac disease. Gastroenterology. 1998;115:1322–8.
Kaukinen K, Collin P, Laurila K, Kaartinen T, Partanen J, Mäki M. Resurrection of gliadin antibodies in coeliac disease. Deamidated gliadin peptide antibody test provides additional diagnostic benefit. Scand J Gastroenterol. 2007;42:1428–33.
Hallert C, Granno C, Hulten S, Midhagen G, Strom M, Svensson H, Valdimarsson T. Living with coeliac disease: controlled study of the burden of illness. Scand J Gastroenterol. 2002;37:39–42.
Sollid LM, Khosla C. Novel therapies for coeliac disease. J Intern Med. 2011;269:604–13.
Gundemir S, Colak G, Tucholski J, Johnson GV. Transglutaminase 2: a molecular Swiss army knife. Biochim Biophys Acta. 2012;1823:406–19.
Jones RA, Nicholas B, Mian S, Davies PJ, Griffin M. Reduced expression of tissue transglutaminase in a human endothelial cell line leads to changes in cell spreading, cell adhesion and reduced polymerisation of fibronectin. J Cell Sci. 1997;110:2461–72.
Griffin M, Casadio R, Bergamini CM. Transglutaminases: nature's biological glues. Biochem J. 2002;368:377–96.
Molberg O, Mcadam SN, Korner R, et al. Tissue transglutaminase selectively modifies gliadin peptides that are recognized by gut-derived T cells in celiac disease. Nat Med. 1998;4:713–7.
Frisullo G, Nociti V, Iorio R, et al. Increased CD4 + CD25 + Foxp3+ T cells in peripheral blood of celiac disease patients: correlation with dietary treatment. Hum Immunol. 2009;70:430–5.
Gianfrani C, Levings MK, Sartirana C, et al. Gliadin-specific type 1 regulatory T cells from the intestinal mucosa of treated celiac patients inhibit pathogenic T cells. J Immunol. 2006;177:4178–86.
Maiuri L, Ciacci C, Ricciardelli I, et al. Association between innate response to gliadin and activation of pathogenic T cells in coeliac disease. Lancet. 2003;362:30–7.
Sander GR, Cummins AG, Henshall T, Powell BC. Rapid disruption of intestinal barrier function by gliadin involves altered expression of apical junctional proteins. FEBS Lett. 2005;579:4851–5.
Giovannini C, Maiuri L, De Vincenzi M. Cytotoxic effect of prolamin-derived peptides on in vitro cultures of cell line Caco-2: Implications for coeliac disease. Toxicol In Vitro. 1995;9:251–5.
Browning TH, Trier JS. Organ culture of mucosal biopsies of human small intestine. J Clin Invest. 1969;48:1423–32.
Stenman SM, Lindfors K, Korponay-Szabo IR, et al. Secretion of celiac disease autoantibodies after in vitro gliadin challenge is dependent on small-bowel mucosal transglutaminase 2-specific IgA deposits. BMC Immunol. 2008;9:6.
Lindfors K, Blomqvist T, Juuti-Uusitalo K, Stenman S, Venäläinen J, Mäki M, Kaukinen K. Live probiotic Bifidobacterium lactis bacteria inhibit the toxic effects induced by wheat gliadin in epithelial cell culture. Clin Exp Immunol. 2008;152:552–8.
Juuti-Uusitalo K, Lindfors K, Mäki M, Patrikainen M, Isola J, Kaukinen K. Inhibition of epithelial growth factor receptor signalling does not preserve epithelial barrier function after in vitro gliadin insult. Scand J Gastroenterol. 2009;44:820–5.
Griffin M, Mongeot A, Collighan R, Saint RE, Jones RA, Coutts IG, Rathbone DL. Synthesis of potent water-soluble tissue transglutaminase inhibitors. Bioorg Med Chem Lett. 2008;18:5559–62.
Baumgartner W, Golenhofen N, Weth A, Hiiragi T, Saint R, Griffin M, Drenckhahn D. Role of transglutaminase 1 in stabilisation of intercellular junctions of the vascular endothelium. Histochem Cell Biol. 2004;122:17–25.
Rauhavirta T, Qiao SW, Jiang Z, et al. Epithelial transport and deamidation of gliadin peptides: a role for coeliac disease patient immunoglobulin A. Clin Exp Immunol. 2011;164:127–36.
Maiuri L, Ciacci C, Ricciardelli I, et al. Unexpected role of surface transglutaminase type II in celiac disease. Gastroenterology. 2005;129:1400–13.
Jones RA, Kotsakis P, Johnson TS, Chau DY, Ali S, Melino G, Griffin M. Matrix changes induced by transglutaminase 2 lead to inhibition of angiogenesis and tumor growth. Cell Death Differ. 2006;13:1442–53.
Stenman SM, Venalainen JI, Lindfors K, et al. Enzymatic detoxification of gluten by germinating wheat proteases: implications for new treatment of celiac disease. Ann Med. 2009;41:390–400.
Thomas S, Brightman F, Gill H, Lee S, Pufong B. Simulation modelling of human intestinal absorption using Caco-2 permeability and kinetic solubility data for early drug discovery. J Pharm Sci. 2008;97:4557–74.
Molberg O, McAdam S, Lundin KE, Kristiansen C, Arentz-Hansen H, Kett K, Sollid LM. T cells from celiac disease lesions recognize gliadin epitopes deamidated in situ by endogenous tissue transglutaminase. Eur J Immunol. 2001;31:1317–23.
Zanzi D, Stefanile R, Santagata S, et al. IL-15 interferes with suppressive activity of intestinal regulatory T cells expanded in Celiac disease. Am J Gastroenterol. 2011;106:1308–17.
Tiittanen M, Westerholm-Ormio M, Verkasalo M, Savilahti E, Vaarala O. Infiltration of forkhead box P3-expressing cells in small intestinal mucosa in coeliac disease but not in type 1 diabetes. Clin Exp Immunol. 2008;152:498–507.
Vorobjova T, Uibo O, Ojakivi I, Teesalu K, Panarina M, Heilman K, Uibo R. Lower expression of tight junction protein 1 gene and increased FOXP3 expression in the small bowel mucosa in coeliac disease and associated type 1 diabetes mellitus. Int Arch Allergy Immunol. 2011;156:451–61.
Maiuri L, Ciacci C, Auricchio S, Brown V, Quaratino S, Londei M. Interleukin 15 mediates epithelial changes in celiac disease. Gastroenterology. 2000;119:996–1006.
Barone MV, Zanzi D, Maglio M, et al. Gliadin-mediated proliferation and innate immune activation in celiac disease are due to alterations in vesicular trafficking. PLoS One. 2011;6:e17039.
Ciccocioppo R, Finamore A, Ara C, Di Sabatino A, Mengheri E, Corazza GR. Altered expression, localization, and phosphorylation of epithelial junctional proteins in celiac disease. Am J Clin Pathol. 2006;125:502–11.
Barone MV, Gimigliano A, Castoria G, et al. Growth factor-like activity of gliadin, an alimentary protein: implications for coeliac disease. Gut. 2007;56:480–8.
Koval M, Ward C, Findley MK, Roser-Page S, Helms MN, Roman J. Extracellular matrix influences alveolar epithelial claudin expression and barrier function. Am J Respir Cell Mol Biol. 2010;42:172–80.
Dieterich W, Esslinger B, Trapp D, et al. Cross linking to tissue transglutaminase and collagen favours gliadin toxicity in coeliac disease. Gut. 2006;55:478–84.
Lammers KM, Lu R, Brownley J et al. Gliadin induces an increase in intestinal permeability and zonulin release by binding to the chemokine receptor CXCR3. Gastroenterology. 2008;135:194–204.e3.
Acknowledgements
The Celiac Disease Study Group has been financially supported by the Academy of Finland, the SalWe Research Program for Intelligent Monitoring of Health and Wellbeing (Tekes—the Finnish Funding Agency for Technology and Innovation grant 648/10), the Pirkanmaa Regional Fund of the Finnish Cultural Foundation, the Sigrid Juselius Foundation, the Competitive Research Funding of Tampere University Hospital, the Research Fund of the Finnish Celiac Society, the European Commission IAPP grant TRANSCOM (Contract number PIA-GA-2010-251506) and Elna Kaarina Savolainen’s Legacy Allocated for the Development of Cancer Treatment.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rauhavirta, T., Oittinen, M., Kivistö, R. et al. Are Transglutaminase 2 Inhibitors Able to Reduce Gliadin-Induced Toxicity Related to Celiac Disease? A Proof-of-Concept Study. J Clin Immunol 33, 134–142 (2013). https://doi.org/10.1007/s10875-012-9745-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-012-9745-5