Abstract
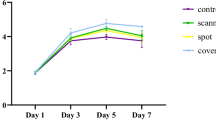
This study was designed to determine the laser dose for the stimulation, zero-bioactivation, and inhibition of normal and neoplastic cells in vitro. The medical use of laser biomodulation has been occurring for decades in the area of tissue healing and inflammatory conditions. The potential to modulate the regeneration and differentiation of early cellular precursors by laser photons is a valuable endeavor searching for novel and efficient methods. A 35-mW HeNe (632.8-nm) laser and power density of 1.25 mW/cm2 was used to irradiate tissue culture dishes seeded with 400 cells/dish of normal cells (CHO, CCL-226, 3 T3, and HSF) and neoplastic cells (EMT-6 and RIF-1). All cell lines were cultured using DMEM supplemented with 10% and 5% FBS, 2 mM glutamine and 100 U pen-strep antibiotic. Irradiation times of 16, 32, 48, 64, 80, 96, 112, 128, 144, and 160 s for three consecutive days to deliver cumulative doses of 60, 120, 180, 240, 300, 360, 420, 480, 540, and 600 mJ/cm2 were done, respectively. Cell cultures were stained and colony-forming efficiency was determined. Data analysis was done using Student’s t test, α = 0.05. A trend of stimulation, zero-bioactivation, and inhibition in all cell lines was observed except for CCL-226 which gave a pattern of inhibition, zero-bioactivation, and inhibition. The optimum biostimulatory dose was at 180 mJ/cm2 and bioinhibitory doses were from 420–600 mJ/cm2 cumulative doses. This study established the dose-dependency of cell growth to laser treatments, that the extent of cellular proliferation is influenced by the type of cells involved, and the risk when laser irradiation is performed on patients with undiagnosed neoplasms and during pregnancy. On the other hand, the ability of laser irradiation to regulate embryonic fibroblasts and human skin fibroblast in vitro suggests possible laser biomodulatory effects on embryonic and adult stem cells directed for tissue regeneration. Studies on the effects of light treatments exploring different laser parameters for the clonal expansion and differentiation of stem cells are recommended.

Similar content being viewed by others
References
Medrado A, Pugliese L, Reis S, Andrade Z (2003) Influence of low-level laser therapy on wound healing and its biological action upon myofibroblasts. Lasers Surg Med 32:239–244
Hopkins JT, McLoda TA, Seegmiller JG, Baxter DG (2004) Low-level laser therapy facilitates superficial wound healing in humans: a triple-blind, sham-controlled study. J Athl Train 39:223–229
Maiya GA, Kumar P, Rao L (2005) Effect of low intensity helium-neon (He-Ne) laser irradiation on diabetic wound healing dynamics. Photomed Laser Surg 23:187–190
Mendez TM, Pinheiro AL, Pacheco MT, Nascimento PM, Ramalho LM (2004) Dose and wavelength of laser light have influence on the repair of cutaneous wounds. J Clin Laser Med Surg 22:19–25
Bisht D, Mehrotra R, Singh PA, Atri SC, Kumar A (1999) Effect of helium-neon laser on wound healing. Indian J Exp Biol 37:187–189
Lyons RF, Abergel RP, White RA, Dwyer RM, Castel JC, Uitto J (1987) Biostimulation of wound healing in vivo by a helium-neon laser. Ann Plast Surg 18:47–50
Al-Watban FAH, Zhang XY, Andres BL (2007) Low-Level Laser Therapy enhances wound healing in diabetic rats: A comparison of Different Lasers. Photomed Laser Surg 2(25):72–77
Al-Watban FAH, Zhang XY, Andres BL, Al-Anize AA (2009) Visible lasers were better than invisible lasers in accelerating burn healing on diabetic rats. Photomed Laser Surg 2(27):269–272
Al-Watban FAH (2009) Laser therapy converts diabetic wound healing to normal healing. Photomed Laser Surg 1(27):127–135
Pereira AN, Eduardo Cde P, Matson E, Marques MM (2002) Effect of low-power laser irradiation on cell growth and procollagen synthesis of cultured fibroblasts. Lasers Surg Med 31:263–267
Allendorf JD, Bessler M, Huang J, Kayton ML, Laird D, Nowygrod R, Treat MR (1997) Helium-neon laser irradiation at fluences of 1, 2, and 4 J/cm2 failed to accelerate wound healing as assessed by both wound contracture rate and tensile strength. Lasers Surg Med 20:340–345
Anneroth G, Hall G, Ryden H, Zetterqvist L (1988) The effect of low-energy infra-red laser radiation on wound healing in rats. Br J Oral Maxillofac Surg 26:12–17
McCaughan JS Jr, Bethel BH, Johnston T, Janssen W (1985) Effect of low-dose argon irradiation on rate of wound closure. Lasers Surg Med 5:607–614
Hunter J, Leonard L, Wilson R, Snider G, Dixon J (1984) Effects of low energy laser on wound healing in a porcine model. Lasers Surg Med 3:285–290
Schlager A, Oehler K, Huebner K, Schmuth M, Spoetl L (2000) Healing of burns after treatment with 670-nanometer low-power laser light. Plast Reconstr Surg 105:1635–1639
Schlager A, Kronberger P, Petschke F, Ulmer H (2000) Low power laser light in the healing of burns: a comparison between two different wavelengths (635 nm and 690 nm) and a placebo group. Lasers Surg Med 27:39–42
Basford JR (1989) Low-energy laser therapy: controversies and new research findings. Lasers Surg Med 9:1–5
Al-Watban FAH, Gonzaga MVD, Andres BL, Zhang XY (2003) Laser as a wound healer: in comparison with pharmacological drugs, LED and conventional light sources. The Millenium Laser Book Trilogy, Lasers in Medicine Surgery and Dentistry, European Medical Laser Association Part Three 618–650.
Al-Watban FAH, Andres BL (2001) The effect of HeNe laser (632 nm) and Solcoseryl in vitro. Lasers Med Sci 16:267–275
Al-Watban FAH, Andres BL (2000) The effect of HeNe laser (632 nm) and Polygen™ in vitro. J Clin Laser Med Surg 3(18):145–150
Schafer FQ, Buettner GR (2001) Redox environment of the cell as viewed through the redox state of the glutathione disulfide/glutathione couple. Free Radic Biol Med 30:1191–1212
Liu H, Colavitti R, Rovira II, Finkel T (2005) Redox-dependent transcriptional regulation. Circ Res 97:967–974
Yang M, Nazhat NB, Jiang X, Kelsey SM, Blake DR, Newland AC, Morris CJ (1996) Adriamycin stimulates proliferation of human lymphoblastic leukaemic cells via a mechanism of hydrogen peroxide (H2O2) production. Br J Haematol 95:339–344
Kirlin WG, Cai J, Thompson SA, Diaz D, Kavanagh TJ, Jones DP (1999) Glutathione redox potential in response to differentiation and enzyme inducers. Free Radic Biol Med 27:1208–1218
Alaluf S, Muir-Howie H, Hu HL, Evans A, Green MR (2000) Atmospheric oxygen accelerates the induction of a post-mitotic phenotype in human dermal fibroblasts: the key protective role of glutathione. Differentiation 66:147–155
Karu T (1999) Primary and secondary mechanisms of action of visible to near-IR radiation on cells. J Photochem Photobiol B 49:1–17
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Al-Watban, F.A.H., Andres, B.L. Laser biomodulation of normal and neoplastic cells. Lasers Med Sci 27, 1039–1043 (2012). https://doi.org/10.1007/s10103-011-1040-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-011-1040-9