Abstract
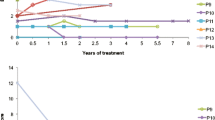
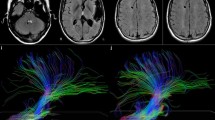
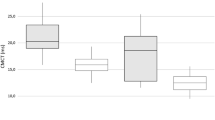
Cerebrotendinous xanthomatosis (CTX) is a rare neurometabolic disease due to defective activity of sterol 27-hydroxylase, with plasma and tissue cholestanol storage. Clinical phenotype is characterized by both systemic manifestations and neurological signs. Therapy with chenodeoxycholic acid (CDCA) suppresses abnormal bile acid synthesis. The purpose of the study was to assess the frequency and clinical relevance of spasticity in the CTX phenotype and to study the usefulness of transcranial magnetic stimulation (TMS) in detecting corticospinal tract damage and monitoring the effects of replacement therapy. Twenty-four CTX patients underwent clinical evaluation including general disability scores, pyramidal and cerebellar function scales, assessment of serum cholestanol and TMS. Nine patients who started CDCA therapy at baseline received clinical and neurophysiological follow up. All patients showed signs of pyramidal damage which were relevant for clinical disability in 18 out of 24 cases (75%), resulting in spastic paraparesis. TMS revealed corticospinal alterations even in subjects with mild clinical signs of corticospinal tract involvement. After CDCA treatment, serum cholestanol decreased to normal concentrations in all patients. Clinical picture was unchanged in seven out of nine cases; in two others pyramidal signs disappeared. A reduction in abnormal neurophysiological parameters was found. Spastic paraparesis is the most frequent and relevant neurological feature in CTX patients. Replacement treatment with CDCA can prevent the progression of pyramidal damage, especially if started early in the course of the disease. TMS represents a sensitive indicator of corticospinal tract dysfunction and subclinical improvements in pyramidal function after CDCA therapy.
Similar content being viewed by others
References
Björkhem I, Boberg KM, Leitersdorf E (2001) Inborn errors in bile acid biosynthesis and storage of sterols other than cholesterol. In: Scriver CR, Beaudet AL, Sly WS, Valle D (eds) The metabolic and molecular basis of inherited disease, 8th edn. McGraw-Hill, New York, pp 2961–2988
Lee MH, Hazard S, Carpten JD et al (2001) Fine-mapping, mutation analysis, and structural mapping of cerebrotendinous xanthomatosis in U.S. pedigrees. J Lipid Res 42:159–169
Cali JJ, Russell DW (1991) Characterization of human sterol 27-hydroxylase. A mitochondrial cytochrome P-450 that catalyzes multiple oxidation reaction in bile acid biosynthesis. J Biol Chem 266:7774–7778
Salen G, Shefer S, Tint GS et al (1985) Biosynthesis of bile acids in cerebrotendinous xanthomatosis. Relationship of bile acid pool sizes and synthesis rates to hydroxylations at C-12, C-25, and C-26. J Clin Invest 76:744–751
Federico A, Dotti MT (2003) Cerebrotendinous xanthomatosis: clinical manifestations, diagnostic criteria, pathogenesis, and therapy. J Child Neurol 18:633–638
Cruysberg JR (2002) Cerebrotendinous xanthomatosis: juvenile cataract and chronic diarrhea before the onset of neurologic disease. Arch Neurol 59:1975
Federico A, Dotti MT, Loré F, Nuti R (1993) Cerebrotendinous xanthomatosis: pathophysiological study on bone metabolism. J Neurol Sci 115:67–70
Arlazoroff A, Roitberg B, Werber E et al (1991) Epileptic seizure as a presenting symptom of cerebrotendinous xanthomatosis. Epilepsia 32:657–661
Dotti MT, Federico A, Garuti R, Calandra S (2000) Cerebrotendinous xanthomatosis with predominant parkinsonian syndrome: further confirmation of the clinical heterogeneity. Mov Disord 15:1017–1019
Alcalay R, Wu S, Patel S, Frucht S (2009) Oromandibular dystonia as a complication of cerebrotendinous xanthomatosis. Mov Disord 24(9):1397–1399
Siebner HR, Berndt S, Conrad B (1996) Cerebrotendinous xanthomatosis without tendon xanthomas mimicking Marinesco–Sjoegren syndrome: a case report. J Neurol Neurosurg Psychiatry 60(5):582–585
Gilad R, Lampl Y, Lev D, Sadeh M (1999) Cerebrotendinous xanthomatosis without xanthomas. Clin Genet 56:405–406
Verrips A, van Engelen BG, Wevers RA et al (2000) Presence of diarrhea and absence of tendon xanthomas in patients with cerebrotendinous xanthomatosis. Arch Neurol 57:520–524
Campdelacreu J, Munoz E, Cervera A et al (2002) Cerebrotendinous xanthomatosis without tendinous xanthomas: presentation of two cases. Neurologia 17:647–650
Okuma H, Kitagawa Y, Tokuoka K, Takagi S (2007) Cerebrotendinous xanthomatosis with cerebellar ataxia as the chief symptom. Intern Med 46:1259–1261
Barkhof F, Verrips A, Wesseling P et al (2000) Cerebrotendinous xanthomatosis: the spectrum of imaging findings and the correlation with neuropathologic findings. Radiology 217:869–876
De Stefano N, Dotti MT, Mortilla M, Federico A (2001) Magnetic resonance imaging and spectroscopic changes in brains of patients with cerebrotendinous xanthomatosis. Brain 124:121–131
Berginer VM, Salen G, Shefer S (1984) Long-term treatment of cerebrotendinous xanthomatosis with chenodeoxycholic acid. N Engl J Med 311:1649–1652
Berginer VM, Gross B, Morad K et al (2009) Chronic diarrhea and juvenile cataracts: think cerebrotendinous xanthomatosis and treat. Pediatrics 123(1):143–147
van Swieten JC, Koudstaal PJ, Visser MC et al (1988) Interobserver agreement for the assessment of handicap in stroke patients. Stroke 19:604–607
Kurtzke JF (1983) Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 33:1444–1452
Koopman BJ, van der Molen JC, Wolthers BG et al (1984) Capillary gas chromatographic determination of cholestanol/cholesterol ratio in biological fluids. Its potential usefulness for the follow-up of some liver diseases and its lack of specificity in diagnosing CTX (cerebrotendinous xanthomatosis). Clin Chim Acta 137(3):305–315
Federico A, Dotti MT (1996) Cerebrotendinous xanthomatosis. In: Moser HW (ed) Handbook of Clinical Neurology 22(66):599–613
Rossini PM, Rossi S (1998) Clinical applications of motor evoked potentials. Electroencephalogr Clin Neurophysiol 106:180–194
Kobayashi M, Pascual-Leone A (2003) Transcranial magnetic stimulation in neurology. Lancet Neurol 2:145–156
Hallett M (2007) Transcranial magnetic stimulation: a primer. Neuron 55:187–199
Rossini PM, Barker AT, Berardelli A et al (1994) Non-invasive electrical and magnetic stimulation of the brain, spinal cord and roots: basic principles and procedures for routine clinical application. Report of an IFCN committee. Electroencephalogr Clin Neurophysiol 91(2):79–92
Passero S, Rossi S, Giannini F, Nuti D (2001) Brain-stem compression in vertebrobasilar dolichoectasia. A multimodal electrophysiological study. Clin Neurophysiol 112:1531–1539
Centonze D, Koch G, Versace V et al (2007) Repetitive transcranial magnetic stimulation of the motor cortex ameliorates spasticity in multiple sclerosis. Neurology 68(13):1045–1050
Knikou M (2008) The H-reflex as a probe: pathways and pitfalls. J Neurosci Methods 171(1):1–12
Verrips A, Hoefsloot LH, Steenbergen GC et al (2000) Clinical and molecular genetic characteristics of patients with cerebrotendinous xanthomatosis. Brain 123(Pt 5):908–919
Verrips A, Nijeholt GJ, Barkhof F et al (1999) Spinal xanthomatosis: a variant of cerebrotendinous xanthomatosis. Brain 122(Pt 8):1589–1595
Clemen CS, Spottke EA, Lütjohann D et al (2005) Cerebrotendinous xanthomatosis: a treatable ataxia. Neurology 64:1476
Mukherjee AA, Chawla BP, Rathi SS, Puthran RS (2007) Cerebrotendinous xanthomatosis: a treatable cause of metabolic ataxia. J Assoc Physicians India 55:655–657
Guerrera S, Stromillo ML, Mignarri A et al (2010) Clinical relevance of brain volume changes in patients with cerebrotendinous xanthomatosis. J Neurol Neurosurg Psychiatry 81(11):1189–1193
Rossini PM, Rossi S (2007) Transcranial magnetic stimulation. Diagnostic, therapeutic and research potential. Neurology 68:484–488
Ugawa Y, Kohara N, Shimpo T, Mannen T (1988) Central motor and sensory conduction in adrenoleukomyeloneuropathy, cerebrotendinous xanthomatosis, HTLV-1-associated myelopathy and tabes dorsalis. J Neurol Neurosurg Psychiatry 51:1069–1074
Mondelli M, Rossi A, Scarpini C et al (1992) Evoked potentials in cerebrotendinous xanthomatosis and effect induced by chenodeoxycholic acid. Arch Neurol 49:469–475
Restuccia D, Di Lazzaro V, Servidei S et al (1992) Somatosensory and motor evoked potentials in the assessment of cerebrotendinous xanthomatosis before and after treatment with chenodeoxycholic acid: a preliminary study. J Neurol Sci 112:139–146
Mondelli M, Sicurelli F, Scarpini C et al (2001) Cerebrotendinous xanthomatosis: 11-year treatment with chenodeoxycholic acid in five patients. An electrophysiological study. J Neurol Sci 190:29–33
Acknowledgments
Authors thank Benito Vecchiarelli for his excellent technical assistance during some of the neurophysiological recordings.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mignarri, A., Rossi, S., Ballerini, M. et al. Clinical relevance and neurophysiological correlates of spasticity in cerebrotendinous xanthomatosis. J Neurol 258, 783–790 (2011). https://doi.org/10.1007/s00415-010-5829-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-010-5829-4