Abstract
Introduction
The expression of excision repair cross-complementation group 1 (ERCC1) is reported to be correlated with resistance to platinum-based drugs. Class III β-tubulin is reported to be correlated with resistance to taxanes.
Methods
In the present study, we evaluated whether ERCC1 and class III β-tubulin expression could be used to predict progression-free and/or overall survival in 34 patients with locally advanced non-small cell lung cancer (NSCLC) receiving concurrent chemoradiation therapy with cisplatin and docetaxel, and immunohistochemistry was used to examine the expression of these two proteins in tumor samples obtained from the patients.
Results
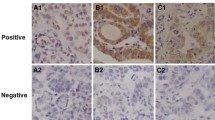
Immunostaining for ERCC1 and class III β-tubulin was positive in 16 and 12 patients, respectively. A significant correlation was observed between ERCC1 expression and response to chemotherapy (P = 0.012), and between class III β-tubulin expression and histology (P = 0.029). Patients negative for ERCC1 had a significantly longer median progression-free (62.5 vs. 36 weeks, P = 0.009), but not overall (171 vs. 50.5 weeks, P = 0.208), survival than those positive for ERCC1. Expression of class III β-tubulin was not correlated with progression-free or overall survival (P = 0.563 and P = 0.265, respectively). Multivariate analysis adjusting for possible confounding factors showed that negative ERCC1 expression (hazard ratio = 3.972, P = 0.009) was a significantly favorable factor for progression-free survival.
Conclusions
This retrospective study indicates that immunostaining for ERCC1 may be useful for predicting survival in NSCLC patients receiving concurrent chemoradiotherapy with cisplatin and docetaxel, and can provide information critical for planning personalized chemotherapy.


Similar content being viewed by others
Abbreviations
- NSCLC:
-
Non-small cell lung cancer
- ERCC1:
-
Excision repair cross-complementation group 1
- p-stage:
-
Pathological stage
- RECIST:
-
Response evaluation criteria in solid tumors
References
Kiura K, Ueoka H, Segawa Y et al (2003) PhaseI/II study of docetaxel and cisplatin with concurrent thoracic radiation therapy for locally advanced non-small-cell lung cancer. Br J Cancer 89:795–802
Lord RV, Brabender J, Gandara D et al (2002) Low ERCC1 expression correlates with prolonged survival after cisplatin plus gemcitabine chemotherapy in non-small cell lung cancer. Clin Cancer Res 8:2286–2291
Ceppi P, Volante M, Novello S et al (2006) ERCC1 and RRM1 gene expressions but not EGFR are predictive of shorter survival in advanced non-small-cell lung cancer treated with cisplatin and gemcitabine. Ann Oncol 17:1818–1825
Olaussen KA, Dunant A, Fouret P et al (2006) DNA repair by ERCC1 in non-small-cell lung cancer and cisplatin-based adjuvant chemotherapy. New Engl J Med 355:983–991
Azuma K, Komohara Y, Sasada T et al (2007) Excision repair cross-complementation group 1 predicts progression-free and overall survival in non-small cell lung cancer patients treated with platinum-based chemotherapy. Cancer Sci 98:1336–1343
Dabholkar M, Vionnet J, Bostick-Burton F et al (1994) Messenger RNA levels of XPAC and ERCC1 in ovarian cancer tissue correlate with response to platinum-based chemotherapy. J Clin Invest 94:703–708
Park DJ, Lenz HJ (2006) Determinants of chemosensitivity in gastric cancer. Curr Opin Pharmacol 6:337–344
Shirota Y, Stoehlmacher J, Brabender J et al (2001) ERCC1 and thymidylate synthase mRNA levels predict survival for colorectal cancer patients receiving combination oxaliplatin and fluorouracil chemotherapy. J Clin Oncol l19:4298–4304
Seve P, Dumontet C (2008) Is class III beta-tubulin a predictive factor in patients receiving tubulin-binding agents? Lancet Oncol 9:168–175
Gan P, Pasquier E, Kavallris M (2007) Class III β-tubulin mediates sensitivity to chemotherapeutic drugs in non-small cell lung cancer. Cancer Res 67:9356–9363
Seve P, Mackey J, Isac S et al (2005) Class III β-tubulin expression in tumor cells predicts response and outcome in patients with non-small cell lung cancer receiving paclitaxel. Mol Cancer Ther 4:2001–2007
Mozzetti S, Ferlini C, Concolino P et al (2005) ClassIII β-tubulin overexpression is a prominent mechanism of paclitaxel resistance in ovarian cancer patients. Clin Cancer Res 11:298–305
Tommasi S, Mangia A, Lacalamita R et al (2007) Cytoskeleton and paclitaxel sensitivity in breast cancer: the role of β-tubulins. Int J Cancer 120:2078–2085
Liu B, Staren ED, Iwamura T et al (2001) Mechanisms of taxotere-related drug resistance in pancreatic carcinoma. J Surg Res 99:179–186
Therasse P, Arbuck SG, Eisenhauer EA et al (2000) New guidelines to evaluate the response to treatment in solid tumors. J Natl Cancer Inst 92:205–216
Cobo M, Isla D, Massuti B et al (2007) Customizing cisplatin based on quantitative excision repair cross-complementing 1 mRNA expression: a phase III trial in non-small-cell lung cancer. J Clin Oncol 25:2747–2754
Simon G, Sharma A, Li X et al (2007) Feasibility and efficacy of molecular analysis-directed individualized therapy in advanced non-small-cell lung cancer. J Clin Oncol 25:2741–2746
Zheng Z, Chen T, Li X et al (2007) DNA synthesis and repair genes RRM1 and ERCC1 in lung cancer. New Engl J Med 356:800–808
Azuma K, Sasada T, Kawahara A et al. Expression of ERCC1 and class III β-tubulin in non-small cell lung cancer patients treated with carboplatin and paclitaxel. Lung Cancer (in press)
Acknowledgments
This study was supported in part by Grants-in-Aid from the 21st Century Centers of Excellence Program for Medical Science, Japan.
Conflict of interest statement
None of the authors has a financial relationship with a commercial entity that has an interest in the subject of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Azuma, K., Sasada, T., Kawahara, A. et al. Expression of ERCC1 and class III β-tubulin in non-small cell lung cancer patients treated with a combination of cisplatin/docetaxel and concurrent thoracic irradiation. Cancer Chemother Pharmacol 64, 565–573 (2009). https://doi.org/10.1007/s00280-008-0907-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-008-0907-3