Abstract
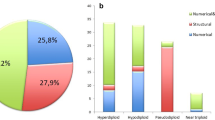
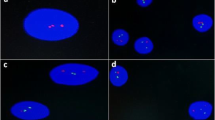
We investigated bone marrow cells of 70 acute lymphoblastic leukemia children by conventional cytogenetics (CC), fluorescence in situ hybridization (FISH), and reverse transcription polymerase chain reaction (RT-PCR) methods. CC and RT-PCR for fusion genes BCR/ABL, MLL/AF4, E2A/PBX1, TEL/AML1 were performed at diagnosis in each patient. FISH was performed to verify the presence of fusion genes and MLL rearrangements and to estimate the percentage of abnormal cells. Karyotypes were obtained in 59 (84%) of 70 cases. Thirty-five (59%) of 59 cases revealed chromosome aberrations. Hyperdiploidy >50 chromosomes was present in nine cases, hyperdiploidy 47–50 chromosomes in six, pseudodiploidy in 15, and hypodiploidy in five. BCR/ABL was present in two cases, PBX1/E2A in two, and TEL/AML1 in 14. MLL/AF4 was not found, but the rearrangements of MLL gene were present in five children. The addition of RT-PCR and FISH to CC was of the utmost importance. One of two Ph translocations and one of two t(1;19) were first revealed by RT-PCR. Moreover, FISH showed the percentage of TEL/AML1(+) cells that turned to be an important prognostic factor. The outcome was the best for the children with hyperdiploidy >50 chromosomes without structural changes. It was also good for those with TEL/AML1 present in ≥80% of cells without chromosome aberrations. The presence of pseudodiploidy correlated with poor outcome. The outcome for patients with t(9;22)–BCR/ABL or 11q23–MLL rearrangement was the worst in study group. The presence of BCR/ABL caused eight times increase of risk of death; MLL rearrangements caused 12 times increase.








Similar content being viewed by others
References
Arico M, Valsecchi MG, Camitta B, Schrappe M (2000) Outcome of treatment in children with Philadelphia chromosome-positive acute lymphoblastic leukemia. N Engl J Med 342:998–1007 doi:10.1056/NEJM200004063421402
Campana D, Behm GB (2000) Immunophenotyping of leukemia. J Immunol Methods 243:59–75 doi:10.1016/S0022-1759(00)00228-3
Carroll WL, Bhojwani D, Min DJ, Raetz E, Relling M, Davies S et al (2003) Pediatric acute lymphoblastic leukemia. Hematology 102–130 doi:10.1182/asheducation-2003.1.102
Cimino G, Elia L, Rapanotti MC, Sprovieri T, Mancini M, Cuneo A et al (2000) A prospective study of residual disease monitoring of the ALL/AF4 transcript in patients with t(4;11) acute lymphoblastic leukemia. Blood 95:96–101
Douet-Guilbert N, Morel F, Le Bris M-J, Herry A, Le Calvez G, Marion V et al (2004) Cytogenetic studies in T-cell acute lymphoblastic leukemia. Leuk Lymphoma 45:287–290 doi:10.1080/10428190310001603911
Ford A, Fasching K, Panzer-Grumayer ER, Koening M, Haas OA, Greaves MF (2001) Origins of late relapse in childhood acute lymphoblastic leukemia with TEL-AML1 fusion genes. Blood 98:558–564 doi:10.1182/blood.V98.3.558
Forestier E, Johansson B, Gustafsson G, Borgström G, Kerndrup G, Johannsson J, Heim S (2000) Prognostic impact of karyotypic findings in childhood acute lymphoblastic leukemia: a Nordic series comparing two treatment periods. Br J Haematol 110:147–153 doi:10.1046/j.1365-2141.2000.02153.x
Friedmann AM, Weinstein HJ (2000) The role of prognostic features in the treatment of childhood acute lymphoblastic leukemia. Oncologist 5:321–328 doi:10.1634/theoncologist.5-4-321
Harrison CJ (2001) Detection and significance of chromosomal abnormalities in childhood acute lymphoblastic leukemia. Blood Rev 15:49–59 doi:10.1054/blre.2001.0150
Heerema NA, Nachman JB, Sather HN, Sensel MG, Lee MK, Hutchinson R et al (1999) Hypodiploidy with less than 45 chromosomes confers adverse risk in childhood acute lymphoblastic leukemia: a report from the Children’s Cancer Group. Blood 94:4036–4046
Hoelzer D, Gokbuget N, Ottmannn O, Pui CH, Relling MV, Appelbaum FR et al (2002) Acute lymphoblastic leukemia. Hematology 162–192 doi:10.1182/asheducation-2002.1.162
Hunger SP, Fall MZ, Camitta BM, Carroll AJ, Link MP, Lauer SJ et al (1998) E2A–PBX1 chimeric transcript status at end of consolidation is not predictive of treatment in childhood acute lymphoblastic leukemias with a t(1;19)(q23;p13): A Pediatric Oncology Group Study. Blood 91:1021–1028
ISCN (2005) An international system for human cytogenetic nomenclature. Karger, Basel
Johansson B, Moorman AV, Haas OA, Watmore AE, Cheung KL, Swanton S et al (1998) Hematologic malignances with t(4;11)(q21;q23)—a cytogenetic, morphologic, immunophenotypic and clinical study of 183 cases. Leukemia 12:779–787 doi:10.1038/sj.leu.2401012
Kager L, Lion T, Attarbaschi A, Koenig M, Strehl S, Haas OA et al (2007) Incidence and outcome of TCF3-PBX1-positive acute lymphoblastic leukemia in Australian children. Haematologica 92:1561–1564 doi:10.3324/haematol.11239
Kearney L (1999) The impact of new FISH technologies on the cytogenetics of the haematological malignancies. Br J Haematol 104:648–658 doi:10.1046/j.1365-2141.1999.01181.x
Kohlmann A, Schoch C, Dugas M, Hiddemann W, Kern W, Haferlach T (2004) Pediatric acute lymphoblastic leukemia (ALL) gene expression signatures classify an independent cohort of adult ALL patients. Leukemia 18:63–71 doi:10.1038/sj.leu.2403167
Kubicka M, Soszynska K, Mucha B, Rafinska B, Kolodziej B, Haus O et al (2007) Unusual profile of pediatric acute lymphoblastic leukemia with MLL gene rearrangement. Leuk Lymphoma 48:2083–2086
Lee A, Kirk J, Edmands S, Radich J (1995) Multiplex PCR of bcr–abl fusion transcripts in Philadelphia positive acute lymphoblastic leukemia. PCR Methods Appl 4:283–287
Pui CH, Chessells JM, Camitta B, Baruchel A, Biondi A, Boyett JM et al (2003) Clinical heterogeneity in childhood acute lymphoblastic leukemia with 11q23 rearrangements. Leukemia 17:700–706 doi:10.1038/sj.leu.2402883
Pui CH (2001) Risk assessment in acute lymphoblastic leukemia: beyond leukemia cell characteristics. J Pediatr Hematol Oncol 23:405–407 doi:10.1097/00043426-200110000-00002
Raimondi SC, Shurtleff SA, Downing JR, Rubnitz J, Mathew S, Hancock M et al (1997) 12p abnormalities and the TEL gene (ETV6) in childhood acute lymphoblastic leukemia. Blood 90:4559–4566
Raynaud SD, Dastugue N, Zoccola D, Shurtleff SA, Mathew S, Raimondi SC (1999) Cytogenetic abnormalities associated with the t(12;21): a collaborative study of 169 children with t(12;21) positive acute lymphoblastic leukemia. Leukemia 13:1325–1330 doi:10.1038/sj/leu/2401506
Sawinska M, Ładon D (2004) Mechanism, detection and clinical significance of the reciprocal translocation t(12;21)(p12;q21) in the children suffering from acute lymphoblastic leukaemia. Leuk Res 28:35–42 doi:10.1016/S0145-2126(03)00160-7
Schrappe M, Arico M, Harbott J, Biondi A, Zimmermann M, Conter V, Reiter A, Valsecchi MG, Gadner H, Basso G, Bartram CR, Lampert F, Riehm H, Masera G, for the German–Austrian–Swiss BFM Study Group and the Associazione Italiana di Ematologia ed Oncologia Pediatrica (AIEOP) (1998) Philadelphia chromosome-positive (Ph+) childhood acute lymphoblastic leukemia: good initial steroid allows early prediction of favorable treatment outcome. Blood 92:2730–2741
Uckun FM, Sensel MG, Sather HN, Gaynon PS, Arthur DC, Lange BJ et al (1998) Clinical significance of translocation t(1;19) in childhood acute lymphoblastic leukemia in the context of contemporary therapies: a report from the Children’s Cancer Group. J Clin Oncol 16:527–535
Uckun FM, Sensel MG, Sun L, Steinhertz PG, Trigg ME, Heerema NA et al (1998) Biology and treatment of childhood T-lineage acute lymphoblastic leukemia. Blood 91:735–746
van der Burg M, Poulsen TS, Hunger SP, Baverloo HB, Smit EME, Vang-Nielsen K et al (2004) Split-signal FISH for detection of chromosome aberrations in acute lymphoblastic leukemia. Leukemia 18:895–908 doi:10.1038/sj.leu.2403340
van Dongen JJM, Macintyre EA, Gabert JA, Delabesse E, Rossi V, Saglio S et al (1999) Standardized RT-PCR analysis of fusion gene transcripts from chromosome aberrations in acute leukemia for detection of minimal residual disease. Report of the BIOMED-1 Concerted Action. Leukemia 13:1901–1928 doi:10.1038/sj/leu/2401592
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Soszynska, K., Mucha, B., Debski, R. et al. The application of conventional cytogenetics, FISH, and RT-PCR to detect genetic changes in 70 children with ALL. Ann Hematol 87, 991–1002 (2008). https://doi.org/10.1007/s00277-008-0540-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-008-0540-6