Abstract
Introduction/hypothesis
Sexual function in women with pelvic organ prolapse (POP) and stress urinary incontinence (SUI) is adversely affected, but data reporting sexual function following surgery are limited. We aimed to determine effect of pelvic reconstructive surgery on sexual function and to evaluate effect of additional continence procedures.
Methods
Women with POP or SUI were assessed using pelvic organ prolapse quantification (POP-Q) or videocystourethrography. Sexual function was assessed with Golombok Rust Inventory of Sexual Satisfaction (GRISS) and sexual domains on prolapse quality of life (P-QoL) questionnaire and King's Health questionnaire. Women were reviewed over 2 years using all these objective and subjective assessments.
Results
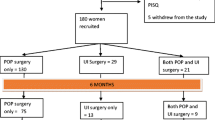
In total, 52 patients were followed up over 2 years. Sexual function measured using GRISS scores and sexual function domain scores of KHQ and P-QoL improved following surgery. A better supported pelvic floor (POP-Q) was associated with significantly improved GRISS scores.
Conclusions
These findings aid in pre-operative counselling of women with POP and SUI about potential improvement in sexual function post-operatively.




Similar content being viewed by others
References
Kelleher CJ, Cardozo LD, Khullar V, Salvatore S (1997) A new questionnaire to assess the quality of life of urinary incontinent women. Br J Obstet Gynaecol 104:1374–1379
Digesu GA, Khullar V, Cardozo L, Robinson D, Salvatore S (2005) P-QoL: a validated questionnaire to assess the symptoms and quality of life of women with urogenital prolapse. Int Urogynecol J Pelvic Floor Dysfunct 16:176–181
Swift SE (2000) The distribution of pelvic organ support in a population of female subjects seen for routine gynaecological health care. Am J Obstet Gynecol 183:277–285
Swift SE, Woodman P, O'Boyle A et al (2005) Pelvic Organ Support Study (POSST): the distribution, clinical definition and epidemiology of pelvic organ support defects. Am J Obstet Gynecol 192:795–806
Jolleys JV (1988) Reported prevalence of urinary incontinence in women in a general practice. Br Med J (Clin Res Ed) 296:1300–1302
Barber MD, Visco AG, Wyman JF, Fantl JA, Bump RC (2002) Sexual function in women with urinary incontinence and pelvic organ prolapse. Obstet Gynecol 99:281–289
Pauls RN, Segal JL, Silva WA, Kleeman SD, Karram MM (2006) Sexual function in patients presenting to a urogynecology practice. Int Urogynecol J Pelvic Floor Dysfunct 17:576–580
Rogers RG, Kammerer-Doak D, Darrow A et al (2006) Does sexual function change after surgery for stress urinary incontinence and/or pelvic organ prolapse? A multicenter prospective study. Am J Obstet Gynecol 195:e1–e4
Ghezzi F, Serati M, Cromi A, Uccella S, Triacca P, Bolis P (2005) Impact of tension-free vaginal tape on sexual function: results of a prospective study. Int Urogynecol J Pelvic Floor Dysfunct 17:54–59
Mazouni C, Karsenty G, Bretelle F, Bladou F, Gamerre M, Serment G (2004) Urinary complications and sexual function after the tension-free vaginal tape procedure. Acta Obstet Gynecol Scand 83:955–961
Helstrom L, Nilsson B (2005) Impact of vaginal surgery on sexuality and quality of life in women with urinary incontinence or genital descensus. Acta Obstet Gynecol Scand 84:79–84
Jha S, Radley S, Farkas A, Jones G (2009) The impact of TVT on sexual function. Int Urogynecol J Pelvic Floor Dysfunct 20(2):165–169
Pace G, Vicentini C (2008) Female sexual function evaluation of the tension-free vaginal tape (TVT) and transobturator suburethral tape (TOT) incontinence surgery: results of a prospective study. J Sex Med 5(2):387–393
Elzevier HW, Putter H, Delaere KP, Venema PL, Lycklama à Nijeholt AA, Pelger RC (2008) Female sexual function after surgery for stress urinary incontinence: transobturator suburethral tape vs. tension-free vaginal tape obturator. J Sex Med 5(2):400–406
Kuhn A, Brunnmayr G, Stadlmayr W, Kuhn P, Mueller MD (2009) Male and female sexual function after surgical repair of female organ prolapse. J Sex Med 6(5):1324–1334
Azar M, Noohi S, Radfar S, Radfar MH (2008) Sexual function in women after surgery for pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 19(1):53–57
Bump RC, Mattiasson A, Bo K et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Rust J, Golombok S (1986) The GRISS: a psychometric instrument for the assessment of sexual dysfunction. Arch Sex Behav 15(2):157–165
Rogers RG, Kammerer-Doak D, Villarreal A, Coates K, Qualls C (2001) A new instrument to measure sexual function in women with urinary incontinence or pelvic organ prolapse. Am J Obstet Gynecol 188:552–558
Kelleher CJ, Pleil AM, Reese PR, Burgess SM, Brodish PH (2004) How much is enough and who says so? BJOG 111(6):605–612
Meston CM, Derogatis LR (2002) Validated instruments for assessing female sexual function. J Sex Marital Ther 28(Suppl 1):155–164
Pauls RN, Silva WA, Rooney CM et al (2007) Sexual function after vaginal surgery for pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol 197:622.e1–622.e7
Lowenstein L, Gamble T, Sanses TV, van Raalte H, Carberry C, Jakus S, Pham T, Nguyen A, Hoskey K, Kenton K (2009) Changes in sexual function after treatment for prolapse are related to the improvement in body image perception. J Sex Med 7:1023–1028. doi:10.1111/j.1743-6109.2009.01586.x
Kahn MA, Stanton SL (1997) Posterior colporrhaphy: its effects on bowel and sexual function. Br J Obstet Gynaecol 104:82–86
Haase P, Skibsted L (1988) Influence of operations for stress incontinence and/or genital descensus on sexual life. Acta Obstet Gynecol Scand 67:659–661
Robinson D, Wadsworth S, Cardozo L, Bidmead J, Balmforth J (2003) Fascial posterior colpoperineorrhaphy: a 5 year follow up study. J Pelvic Med Surg 9(6):279–283
Blandon RE, Gebhart JB, Trabuco EC, Klingele CJ (2009) Complications from vaginally placed mesh in pelvic reconstructive surgery. Int Urogynecol J Pelvic Floor Dysfunct 20:523–531. doi:10.1007/s00192-009-0818-9
Carey M, Higgs P, Goh J, Lim J, Leong A, Krause H, Cornish A (2009) Vaginal repair with mesh versus colporrhaphy for prolapse: a randomised controlled trial. BJOG 116(10):1380–1386
Srikrishna S, Robinson D, Cardozo L (2009) Qualifying a quantitative approach to women's expectations of continence surgery. Int Urogynecol J Pelvic Floor Dysfunct 20(7):859–865, Epub 2009 Apr 7
Hartmann U, Philippsohn S, Heiser K, Ruffer-Hesse C (2004) Low sexual desire in midlife and older women: personality factors, psychosocial development, present sexuality. Menopause 11:726–740
Conflicts of interest
Sushma Srikrishna, Speaker Honorarium: Recordati, Astellas, SEP, Advisory board; Astellas. Dudley Robinson, Consultant: Astellas, Ferring, Gynaecare, Uroplasty, Pfizer, Recordati, Novo-Nordisk, Speaker Honorarium: Astellas, Ferring, Gynaecare, Uroplasty, Pfizer, Recordati, Trial participation: Astellas, Pfizer. Linda Cardozo, Consultant: Astellas, Pfizer, Rottapharm, Schering-Plough, SEP, Speaker Honorarium: Astellas, Pfizer, Rottapharm, Trial Participation: Astellas, Pfizer, Research grant: Pfizer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Srikrishna, S., Robinson, D., Cardozo, L. et al. Can sex survive pelvic floor surgery?. Int Urogynecol J 21, 1313–1319 (2010). https://doi.org/10.1007/s00192-010-1198-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-010-1198-x