Abstract
Background
Integration of patient views in mental health service planning is in its infancy despite service provision being clearly dominated by narratives from professional consultations and medical records. We wished to clarify perceptions of uncertainty about mental health conditions from a range of provider and user perspectives (patients, carers, parents, mental health service providers) and understand the role of narratives in mental health research.
Aims
(1) To explore the utility of qualitative research methods, particularly narrative content analysis in mental health research, and (2) identify aspects of uncertainty in mental health service users and providers.
Material
Four hundred and six free text responses were considered as one element of an existing questionnaire about uncertainties about mental health treatments, collected from mental healthcare users and providers through charities, the Mental Health Research Network in Wales, health professionals and websites. Free text responses were analysed using narrative content analysis, an elaborate and rigorous research technique that involves groups of analysts working independently and together over extended group sessions.
Findings
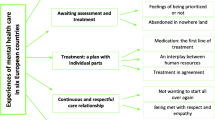
Three main themes emerged across respondent groups: “medication and treatment options”, “objectification and marginalisation of patient” and “integrity of service delivery”. Within these, patients embraced the opportunity to write about their illness at length, whilst carers’ and parents’ main concerns were about how patients were dealing with their illnesses, the services they were getting and the side effects of treatments. Carers and patients’ parents perceived themselves to be the ‘go-between’, carrying messages between patients and professionals, in order to enable services to function. Mental health service providers and professionals considered uncertainties surrounding medication and treatment from an ‘evidence-base’ perspective, concentrating on medication choices and the adoption of new approaches to care rather than patient need and expectation. Patients wanted to know what alternatives were available to the drug regimes they were on and felt their opinions were rarely listened to. As a consequence patients felt marginalised by the health systems there to support them and by society as a whole.
Conclusions
Narrative content analysis can help distil large amounts of free text data and enable their successful interpretation. Listening to patients’ voices should become an integral part of routine service evaluation and may help bring patient expectation more in line with service organisation and delivery towards an optimal delivery of care.


Similar content being viewed by others
References
Lloyd K, Rose Fenton (2006) Identifying uncertainties about the effects of treatments for schizophrenia. J Ment Health 15:1–15
Rose D (2003) Collaborative research between users and professionals: peaks and pitfalls. Psychiatr Bull 27:404–406
Philpot M, Collins C, Trivedi P, Treloar A, Gallagher S, Rose D (2004) Eliciting users’ views of ECT in two mental health trusts with a user-designed questionnaire. J Ment Health 13(4):403–414
Wessley S (2007) A defense of the randomised controlled trial in mental health. BioSocieties 2:115–127
Priebe S, Slade M (2001) Evidence in Mental Health Care. Routledge, London
Leichsenring F (2004) Randomised controlled versus naturalistic studies: a new research agenda. Bull Menninger Clin 68(2):137–151
Slade M, Priebe S (2001) Are randomised controlled trials the only gold that glitters? (Editorial). The Br J Psychiatry 179:286–287
van Manen M (1990) Researching lived experience: human science for an action sensitive pedagogy. State University of New York Press, Albany
van Manen M (1997) From meaning to method. Qual Health Res 7(3):345–369
Brown C, Lloyd KR (2001) Qualitative research methods in psychiatric research. Adv Psychiatr Treat 7:350–356
Naylor CD (1995) Grey zones of clinical practice: identifying some limits to evidence-based medicine. Lancet 345(8953):840–842
Green J, Britten N (1998) Qualitative research and evidence-based medicine. BMJ 316(7139):1230–1232
Rapport F (ed) (2004) New qualitative methodologies in health and social care research. Routledge, London
Rapport F, Wainwright P, Elwyn G (2005) Of the edgelands’: broadening the scope of qualitative methodology. Med Humanit 31(1):37–43
Walsh SH (2004) The clinician’s perspective on electronic health records and how they can affect patient care. BMJ 328:1184–1187
Murray M (2003) Narrative psychology. In: Smith JA (ed) Qualitative psychology. Sage Publications, London
Mishler E (2004) Storylines: craftartists’ narratives of identity. Harvard University Press, Harvard
Bruner JS (2002) Making stories: law, literature, life. Harvard University Press, London
Jones EE (1986) Interpreting interpersonal behavior: the effects of expectancies. Science 234:41–46
Snyder M, Stukas AA Jr (1999) Interpersonal processes: the interplay of cognitive, motivational, and behavioral activities in social interaction. Annu Rev Psychol 50:273–303
Savage-Rumbaugh S, Murphy J, Sevcik RA, Brakke KE, Williams SL, Rumbaugh D (1993) Language comprehension in Ape and Child. Monogr Soc Res Child Dev 58(233):3–4
Frank A (1995) The wounded storyteller: body, illness, and ethics. University Press, Chicago
Hurwitz B, Greenhalgh T, Skultans V (eds) (2004) Narrative research in health and illness. BMJ Books, Oxford
Elwyn G, Gwyn R (1999) Stories we hear and stories we tell: analysing talk in clinical practice. BMJ 318:186–188
Picker Institute (2008) UK PCT Patient Survey 2008 Hillingdon Primary Care Trust. Executive summary. http://www.pickereurope.org; http://www.picker-results.org
Campbell JL, Ramsay J, Green J (2001) Age, gender, socioeconomic, and ethnic differences in patients’ assessments of primary health care. Qual Health Care 10:90–95
Thornicroft G, Leese M, Tansella M, Howard L, Toulmin H, Herran A, Schene A (2002) Gender differences in living with schizophrenia. A cross-sectional, European, multi-site study. Schizophr Res 57:191–200
Gibson PG, Talbot PI, Toneguzzi RC (2005) Consultations for Asthma: will greater patient involvement deliver better health? Thorax 60:177–178
Chalmers I (2004) Well informed uncertainties about the effects of treatments. Br Med J 328:475–476
Wancat J, Freidl M, Krautgartner M, Friedrich F, Matschnig T, Unger A, Gossler R, Fruhwald S (2008) Gender aspects of parents’ needs of schizophrenia patients. Soc Psychiatry Psychiatr Epidemiol 43(12):968–974
Coffey A, Atkinson P (1996) Making sense of qualitative data. Sage, Thousand Oaks
Rashidian A, Eccles MP, Russell I (2008) Falling on stony ground? A qualitative study of implementation of clinical guidelines’ prescribing recommendations in primary care. Health Policy 85:148–161
Hollway W, Jefferson T (2000) The practice of cooperative inquiry: research “with” rather than “on” people. In: Reason P, Bradbury H (eds) Handbook of action research: participative inquiry and practice. Sage, London
Schwandt TA (1997) Qualitative inquiry: a dictionary of terms. Sage Publications, Thousand Oaks
Gotell E, Brown S, Ekman SL (2008) The influence of caregiver singing and background music on vocally expressed emotions and moods in dementia care: a qualitative analysis. Int J Nurs Stud 46(4):422–430
Schmoll BJ (1993) Qualitative research. In: Bork CE (ed) Research in physical therapy. J B Lippincott, Philadelphia, pp 83–124
Robson C (2002) Real world research. Blackwell, Oxford
Denzin NK, Lincoln YS (eds) (2002) Handbook of qualitative research, 2nd edn. Sage Publications Inc., Thousand Oaks
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rapport, F.L., Jerzembek, G.S., Doel, M.A. et al. Narrating uncertainties about treatment of mental health conditions. Soc Psychiat Epidemiol 45, 371–379 (2010). https://doi.org/10.1007/s00127-009-0072-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-009-0072-y