Abstract
Clarification of the molecular mechanisms of insulin secretion is crucial for understanding the pathogenesis and pathophysiology of diabetes and for development of novel therapeutic strategies for the disease. Insulin secretion is regulated by various intracellular signals generated by nutrients and hormonal and neural inputs. In addition, a variety of glucose-lowering drugs including sulfonylureas, glinide-derivatives, and incretin-related drugs such as dipeptidyl peptidase IV (DPP-4) inhibitors and glucagon-like peptide 1 (GLP-1) receptor agonists are used for glycaemic control by targeting beta cell signalling for improved insulin secretion. There has been a remarkable increase in our understanding of the basis of beta cell signalling over the past two decades following the application of molecular biology, gene technology, electrophysiology and bioimaging to beta cell research. This review discusses cell signalling in insulin secretion, focusing on the molecular targets of ATP, cAMP and sulfonylurea, an essential metabolic signal in glucose-induced insulin secretion (GIIS), a critical signal in the potentiation of GIIS, and the commonly used glucose-lowering drug, respectively.
Similar content being viewed by others
Introduction
The blood glucose level is tightly controlled by insulin secretion from pancreatic beta cells and insulin action in target tissues such as liver, muscle and adipose tissue. Pancreatic beta cells secrete an appropriate amount of insulin in a process that is precisely regulated temporally to maintain glucose homeostasis. Insulin secretion is regulated by various factors, including nutrients and hormonal and neural inputs to the beta cells, among which glucose is the most important physiological regulator. Beta cell dysfunction impairs normal regulation of insulin secretion and leads to diabetes or hypoglycaemia. The mechanisms of insulin secretion have been studied extensively both in vivo and in vitro in the 50 years since the establishment of the radioimmunoassay for insulin [1]. Our understanding of the mechanisms of insulin secretion was deepened but remained incomplete. By the early 1980s, the major intracellular signals in pancreatic beta cells for insulin secretion had been identified by pharmacological, physiological and biochemical methods. These include Ca2+, ATP, cAMP and phospholipid-derived molecules such as diacylglycerol (DAG) and inositol 1,4,5-trisphosphate (IP3) [2–4].
Glucose-induced insulin secretion (GIIS) is the principal mechanism of insulin secretion (Fig. 1a). Early studies proposed two models of beta cell glucoreceptor signalling in GIIS: the regulatory-site model [5] and the substrate-site model [6, 7], although most studies supported the latter model [8]. Following the discovery of the ATP-sensitive K+ (KATP) channel in cardiomyocytes by electrophysiology [9], the KATP channel and the glucose-regulated K+ channel were also found in pancreatic beta cells [10–12]. As the KATP channel couples glucose metabolism to electrical activity of the beta cell [13], the discovery of the channel supported the notion that glucose metabolism is essential for GIIS. Accumulating evidence indicates that glucose induces insulin secretion by two different pathways: the triggering pathway (KATP channel-dependent pathway) and the metabolic amplifying pathway (KATP channel-independent pathway), the former of which is essential for GIIS [14]. According to the current consensus on the triggering pathway of GIIS, glucose transported into the beta cell through glucose transporters is rapidly metabolised to yield an increase in the ATP concentration (ATP/ADP ratio), which causes closure of KATP channels and depolarisation of the cell membrane. Membrane depolarisation opens the voltage-dependent Ca2+ channels, allowing Ca2+ influx. The resultant rise in intracellular Ca2+ concentration ([Ca2+]i) in the beta cell leads to fusion of insulin granules to the plasma membrane in a soluble N-ethylmaleimide-sensitive factor attachment protein receptor (SNARE)-dependent process. In contrast to this well-established triggering pathway, the metabolic amplifying pathway is more complex and its mechanism less well understood. It has been suggested that metabolic signals generated by glucose, such as ATP, act on steps in the secretory process distal to the [Ca2+]i rise [15–17]. However, this pathway does not influence insulin secretion if [Ca2+]i is not increased; the metabolic amplifying pathway does not function if the triggering pathway is not operational. In addition to metabolic signals generated by glucose, intracellular signals such as cAMP, DAG and IP3, evoked by hormonal and neuronal inputs, are important for normal regulation of insulin secretion (neurohormonal amplifying pathway) [14]. Lipid metabolism is also important for regulating as well as modulating insulin secretion [18]. The molecular bases for stimulus-secretion coupling in GIIS and its potentiation were largely unknown until the early 1990s. By utilising molecular biology, gene technology and bioimaging, many regulators and targets of intracellular signals in insulin secretion have been identified, greatly enhancing our understanding of GIIS. This review discusses the targets of ATP, cAMP and the glucose-lowering drug sulfonylurea and their roles in GIIS, based on our recent studies.
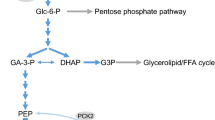
a Glucose-induced insulin secretion and its potentiation. Glucose is transported thorough the glucose transporter into the pancreatic beta cell. Metabolism of glucose increases ATP production (ATP/ADP ratio), closing the KATP channels, depolarising beta cell membrane (ΔΨ), opening the voltage-dependent Ca2+ channels (VDCCs) and allowing Ca2+ influx, thereby triggering insulin secretion (formerly called the KATP channel-dependent pathway, presently called the triggering pathway). In addition to the triggering pathway, metabolic signals generated by glucose metabolism amplify insulin secretion (formerly called the KATP channel-independent pathway, presently called the metabolic amplifying pathway). Insulin secretion is also amplified by hormones and neurotransmitters that generate intracellular signals such as cAMP, DAG, and IP3 (neurohormonal amplifying pathways). PLCβ, phospholipase C-β; AC, adenylyl cyclase; ACh, acetylcholine. b Modes of insulin granule exocytosis. There are three modes of insulin granule exocytosis based on the dynamics of the granules. ‘Old face’: predocked granules that are fused to the plasma membrane by stimulation. ‘Restless newcomer’: granules that are newly recruited by stimulation and immediately fused to the plasma membrane. ‘Resting newcomer’: granules that are newly recruited by stimulation, docked and fused to the plasma membrane by stimulation. Modified from [27] with permission. Copyright 2007 National Academy of Sciences, U.S.A. c Models of glucose-induced insulin secretion. In the existing model of GIIS, the first phase of insulin secretion results from an RRP comprising predocked insulin granules (old face); the second phase secretion results from an RP comprising granules located farther away (resting newcomer), granules that are newly recruited upon stimulation, docked, and fused to the plasma membrane. In the new model, both phases are caused by restless newcomer granules that are recruited upon stimulation and immediately fused to the plasma membrane without docking. Modified with permission of the American Society for Clinical Investigation, from [31]; permission conveyed through Copyright Clearance Center, Inc.
Dynamics of insulin secretion
Insulin secretion is a highly dynamic process. Glucose induces insulin secretion in a biphasic pattern: there is an initial component (first phase) that develops rapidly but lasts only a few minutes, and this is followed by a progressively increasing or sustained component (second phase) [14, 19, 20]. Loss of first phase secretion and reduced second phase secretion are characteristic features of type 2 diabetes. It is known that there is a decrease in the first phase of GIIS in the early stage of type 2 diabetes and in impaired glucose tolerance [21].
By analogy with the exocytosis of neurotransmitters in neurons [22], insulin granule exocytosis is thought to involve several steps, including recruitment, docking, priming and fusion [23]. It has been suggested that secretory vesicles in pancreatic beta cells exist in functionally distinct pools and that the sequential release of these pools underlies the separable components in the dynamics of exocytosis [20]. Pancreatic beta cells contain at least two pools of insulin secretory granules that differ in release competence: a reserve pool (RP) accounting for the vast majority of granules, and a readily releasable pool (RRP) accounting for the remaining <5%. A current hypothesis maintains that the first phase of GIIS is caused by release of RRP granules and that the second phase of GIIS represents a subsequent supply of new granules mobilised from the RP [14, 20, 24].
Investigation of insulin granule dynamics has recently been refined by use of the total internal reflection fluorescence microscopy (TIRFM) system [25–28]. TIRF is a technology that provides a means of selectively exciting fluorophores in an aqueous or cellular environment very near a solid surface (within 100 nm) without exciting fluorescence from regions further from the surface [29]. This unique feature of TIRFM analysis has has led to its application in various different areas of biochemistry and cell biology. A previous TIRFM study reported that insulin granule exocytosis occurs in two modes [26]. In one mode (mode 1), fusion events are caused by granules that are predocked to the plasma membrane (referred to as ‘previously docked granules’ in [26] and ‘old face’ in [27]). In the other mode, fusion events are caused by granules that are newly recruited to the plasma membrane (‘newcomer’). Detailed analyses of insulin granule dynamics induced by various stimuli using primary cultured pancreatic beta cells show that ‘newcomer’ can be classified into two modes: one mode (mode 2), in which granules are newly recruited and immediately fused to the plasma membrane without docking (a docking state that can barely be detected by TIRFM) (‘restless newcomer’), and another mode (mode 3) in which granules are newly recruited, docked and then fused to the plasma membrane (‘resting newcomer’) [27] (Fig. 1b). The three modes of insulin granule exocytosis have been confirmed by other studies [28, 30]. Unlike the original model of GIIS, in which the first phase results from the RRP comprising predocked granules and the second phase from RP, a new model in which both phases of GIIS are caused by ‘restless newcomer’ has been proposed (Fig. 1c) [31].
In contrast, most K+-induced insulin granule exocytosis that occurs immediately and transiently after stimulation represents the release of predocked granules (‘old face’) [27, 32]. The dynamics of insulin granule exocytosis vary according to whether stimulation is due to K+ or glucose. As K+ stimulation elicits only Ca2+ influx and glucose stimulation generates various metabolic signals such as ATP in addition to Ca2+ influx in pancreatic beta cells, this difference in intracellular signal may underlie the distinct modes of exocytosis.
Various proteins associated with insulin granule exocytosis have been identified [23, 33], among which Rab-interacting molecule 2 (Rim2, Rim2α) was identified as a molecule interacting with exchange protein activated by cAMP (Epac) 2A (cAMP-GEFII) [34]. In addition to Epac2A, Rim2α interacts with various exocytosis-related molecules, at least in vitro, including Rab3 [34], Munc13-1 [35], Rab8 [36], ELKS [37, 38], Piccolo [39], and synaptotagmin 1 [40]. Although synaptotagmin 1 is produced in insulinoma cells, the synaptotagmin genes expressed in primary mouse beta cells are those encoding synaptotagmin 7 [41] and 9 [42]. Rim2α null (Rim2α −/−) mice exhibit a marked impairment in glucose tolerance [43]. Analysis by TIRFM shows that both K+-induced insulin granule exocytosis and glucose-induced insulin granule exocytosis, especially the first phase, are severely impaired in pancreatic beta cells of Rim2α null mice [43]. Rim2α has been found to determine the docking and priming states depending on interaction with Rab3 or Munc13-1, respectively.
The exocyst is an octameric protein complex that ensures spatial docking or tethering of exocytotic vesicles to fusion sites of the plasma membrane [44]. Eight subunits of the exocyst complex are expressed in both pancreatic islets and MIN6 cells. Exocyst complex component 3-like (Exoc3l), an isoform of Sec6, the core subunit of the exocyst complex, was identified by in silico screening [45]. Exoc3l forms tertiary complexes consisting of Sec5, Sec8 and Sec10, all of which are binding partners of Sec6. Exoc3l is suggested to be involved in the regulated exocytosis of insulin granules through formation of the exocyst complex.
cAMP-increasing ligands potentiate both the first phase and second phase of GIIS [4]. However, the potentiating effect of cAMP occurs only at glucose concentrations above a certain threshold [46]. cAMP also affects various steps of insulin secretion. In normal pancreatic islets, the in vitro concentration dependence of GIIS displays a sigmoidal curve [47], in which a glucose concentration exceeding 6 mmol/l is required to trigger insulin secretion. In addition, it has been reported that glucagon-like peptide 1 (GLP-1) renders glucose-insensitive beta cells glucose-competent, probably by modulating KATP channel activity [48]. These findings suggest a mechanism by which cAMP might induce beta cell glucose responsiveness. Using a pancreatic perfusion system, we recently found that pretreatment with GLP-1 or glucose-dependent insulinotropic polypeptide (GIP) improved glucose responsiveness to some extent in Kir6.2 null (Kir6.2 −/−) mice, in which almost no insulin secretion in response to glucose is detected [49], but the effect of GLP-1 was stronger. The dynamics of GIIS is usually assessed by the insulin secretory response to a large and prompt change in glucose concentration, e.g. from 2.8 to 16.7 mmol/l in 1 min, using perfusion of the pancreas and perifusion of pancreatic islets. However, such a drastic change in glucose concentration is unlikely to occur in the physiological state. As regards the perfusion of the pancreases of wild-type mice, when the glucose concentration was increased in a stepwise manner (1.4 mmol/l every 5 min) from 2.8 to 12.5 mmol/l in the absence of cAMP-increasing agents (8-bromo-cAMP or GLP-1), no insulin secretion was evoked (Fig. 2a) [50]. Interestingly, the presence of these agents resulted in a dramatic induction of GIIS (Fig. 2a, b). Similar results also were found in Kir6.2 null mice. This GIIS was almost completely abolished by treatment with niflumic acid, indicating that cAMP signalling also evokes glucose responsiveness by activating niflumic acid-sensitive channels (Fig. 2c). Niflumic acid is often used to block Cl− channels but it also acts on other channels, including transient receptor potential (TRP) channels. Since removal of Na+ did not abolish the membrane depolarisation caused by glucose and cAMP [50], Na+ influx through TRP channels is unlikely to be a contributor to initial membrane depolarisation; Ca2+-activated Cl− channels are the more likely candidate for the niflumic acid-sensitive channels responsible for depolarisation caused by glucose and cAMP. These findings indicate that cAMP signalling is important not only for potentiation of GIIS but also for induction of glucose responsiveness in insulin secretion.
a Insulin secretion in response to small and stepwise increases (increment of 1.4 mmol/l per 5 min) in glucose concentration in the absence (white circles) and presence (white triangles) of 1 mmol/l 8-bromo-cAMP. b Insulin secretion in response to small and stepwise increases in glucose concentration in the absence of 10 nmol/l GLP-1. c Effect of niflumic (100 μmol/l) acid on insulin secretion in response to small and stepwise increases in glucose concentration in the presence of 1 mmol/l 8-bromo-cAMP. Reproduced from [50] with permission of Springer Science+Business Media
The role of cAMP signalling in insulin granule exocytosis has also been investigated by TIRFM. The cAMP analogue 8-bromo-cAMP alone did not cause either significant docking or fusion events of insulin granules. However, 8-bromo-cAMP clearly enhanced the frequency of glucose-induced fusion events in both the first phase and the second phase. 8-bromo-cAMP promoted fusion events by increasing only ‘restless newcomer’. Comparison of the fusion sites induced by glucose stimulation and those induced by 8-bromo-cAMP stimulation showed that new fusion sites appeared upon 8-bromo-cAMP stimulation, suggesting that cAMP signaling also participates in the spatial regulation of insulin granule exocytosis [27].
The KATP channel as a target of ATP and sulfonylurea
The KATP channel links cellular metabolic status to the electrical activity of pancreatic beta cells [10–12] and is a key molecule in the regulation of GIIS. The beta cell KATP channel was also suggested to be the target for sulfonylurea [51], a widely used drug in the treatment of type 2 diabetes. However, whether the target (receptor) for sulfonylurea was the KATP channel itself or a molecule associated closely with the KATP channel was not known. In 1995, a receptor (SUR1) for sulfonylurea was cloned by Aguilar-Bryan and colleagues [52] (Fig. 3a). SUR1 was found to be a member of the ATP-binding cassette (ABC) transporter family [52]. However, expression of SUR1 alone in Xenopus oocytes did not generate K+ currents, demonstrating that SUR1 is not itself the KATP channel. At almost the same time that SUR1 was cloned, we identified a novel member of the inwardly rectifying K+ channel family, designated BIR (now known as Kir6.2), by homology screening of the insulin-secreting cell line MIN6 cDNA library using uKATP-1 (now Kir6.1) as a probe (Fig. 3a) [53]. Like SUR1, expression of Kir6.2 alone in mammalian cells did not produce K+ channel activity. We therefore explored the possibility that Kir6.2 generates K+ channel activity by coupling with SUR1. Coexpression of Kir6.2 and SUR1 in mammalian cells generated ATP-sensitive and sulfonylurea-sensitive K+ currents with electrophysiological and pharmacological properties similar to those of beta cell KATP channels [53], demonstrating that the beta cell KATP channel is composed of Kir6.2, a pore-forming subunit, and SUR1, a regulatory subunit (Fig. 3a). Reconstitution of the beta cell KATP channel currents from Kir6.2 and SUR1 was also reported using a Xenopus oocyte expression system by Ashcroft and her colleagues [54]. The beta cell KATP channel functions as a hetero-octameric complex comprising a tetramer of the Kir6.2 subunit and a tetramer of the SUR1 subunit (Fig. 3b). SUR2 (SUR2A and SUR2B) was subsequently cloned. It is now known that differing combinations of Kir6.2 or Kir6.1 and SUR1, SUR2A or SUR2B constitute different KATP channels with distinct nucleotide sensitivities and pharmacological properties in various cell types [55, 56], where they function as metabolic sensors [57, 58]. A two-site (A site and B site) model for the interaction of SUs and glinides with SUR has been proposed [59, 60]. The A site is located on the eighth cytosolic loop (between transmembrane segments [TM] 15 and 16), which is specific for SUR1, and the B site is located on the third cytosolic loop (between TM 5 and 6), which is very similar in all SURs. Based on this model, SUs and glinides can be divided into three groups. The first group (which includes tolbutamide, gliclazide and nateglinide) binds specifically to the A site of SUR1; the second group (which includes glibenclamide, known as glyburide in the USA and Canada, and glimepiride) binds to the B sites of both SUR1 and SUR2A as well as to the A site of SUR1; the third group (which includes meglitinide and repaglinide) binds to the B site of SUR1 and SUR2A.
a Kir6.2 and SUR1. Kir6.2, which belongs to the inwardly rectifying K+ channel family, is the pore-forming subunit. SUR1, which belongs to the ATP-binding cassette transporter family, is the regulatory subunit. b Subunit structure of the beta cell KATP channel. A beta cell KATP channel is composed of Kir6.2 and SUR1 with 4 to 4 stoichiometry. c Insulin secretion from perifused pancreatic islets of Kir6.2 null mice (black circles) and wild-type mice (white circles). NBF, nucleotide binding fold; TMD, transmembrane domain. Reproduced from [62] with permission. Copyright 1998 National Academy of Sciences, USA
Studies of various KATP genetically engineered mice [61–64] clearly show the essential role of the KATP channel for GIIS and sulfonylurea-induced insulin secretion (Fig. 3c). Under certain conditions in Kir6.2 null mice [63, 65], GIIS was detected to some extent, indicating that the metabolic amplifying pathway contributes at least in part to GIIS. However, during stimulation with glucose alone, the metabolic amplifying pathway is ineffective as long as the triggering pathway is inoperative. The triggering and metabolic amplifying pathways in GIIS have recently been reviewed in detail [14]. Mutations of the beta cell KATP channels cause neonatal diabetes or persistent hyperinsulinaemic hypoglycaemia of infancy (PHHI), depending on gain-of function (activating) mutation or loss-of-function mutation, respectively. The pathophysiology of PHHI and neonatal diabetes owing to mutations of Kir6.2 and SUR1 have been discussed in detail in recent review articles [66–68].
The ventromedial hypothalamus (VMH) has been shown to possess the highest density of glucose-responsive (GR) neurons, which play a critical role in glucose homeostasis and are involved in glucagon secretion during hypoglycaemia [69]. The VMH KATP channel has been found to consist of Kir6.2 and SUR1 [70], which is identical to the beta cell KATP channel. Recovery from systemic hypoglycaemia induced by insulin injection was severely impaired in Kir6.2 null mice due to a marked reduction in glucagon secretion in vivo in these mice. Glucagon secretion in response to low glucose concentrations in isolated pancreatic islets from Kir6.2 null mice to that islets from wild-type mice, indicating a normal response of glucagon secretion from alpha cells [71]. Administration of 2-deoxyglucose (2DG) into the intracerebroventricle, which is known to induce neuroglucopenia in the hypothalamus and to stimulate glucagon secretion through activation of autonomic neurons, produced an increase in glucagon secretion in normal mice but not in Kir6.2 null mice. Thus, the KATP channels in the VMH function as glucose sensors for glucagon secretion during hypoglycemia. Beta-cell and VMH KATP channels act in concert as peripheral and central glucose sensors in the maintenance of glucose homeostasis.
It was suggested that some sulfonylureas enhance glucose uptake in skeletal muscles [72, 73]. The glucose-lowering effect by insulin injection at a relatively low dose is significantly increased in Kir6.2 null mice compared with that in normal mice, suggesting that insulin sensitivity is enhanced in Kir6.2 null mice [62]. In fact, glucose uptake in some skeletal muscles is increased in Kir6.2 null mice [74]. The involvement of the KATP channels in glucose uptake in skeletal muscles also is indicated by a study of SUR2 null (SUR2 −/−) mice [75]. Thus, closure of the KATP channels in skeletal muscles can enhance glucose transport. KATP channels in pancreatic beta cells, hypothalamus and skeletal muscle are critically involved in the maintenance of glucose homeostasis [76].
Epac2A (cAMP-GEFII) as a target of cAMP
Since the discovery of cAMP as an intracellular second messenger, it has been shown to mediate a variety of cellular responses. Various hormones and neurotransmitters, including GLP-1 [77–79], GIP [77, 79], vasoactive intestinal polypeptide (VIP) [80] and pituitary adenylate cyclase-activating polypeptide (PACAP) [80], potentiate insulin secretion by promoting cAMP generation in pancreatic beta cells. Eight adenylyl cyclase isoforms (types I–VIII) are expressed in pancreatic islets and beta cell lines [81, 82]. In fact, MDL12330A, an adenylyl cyclase inhibitor, completely blocks both GLP-1- and GIP-induced cAMP production in islets and also markedly reduces both GLP-1- and GIP-potentiated insulin secretions [83].
Until recently, the action of cAMP in insulin secretion was thought to primarily be mediated by protein kinase A (PKA), which phosphorylates various proteins associated with the secretory process [84]. Kir6.2, the pore-forming subunit of KATP channels, and the α-subunit of the voltage-dependent Ca2+ channel can be phosphorylated by PKA on stimulation in beta cell lines [85, 86]. GLUT2 can also be phosphorylated by GLP-1 in purified beta bcells [87]. Although phosphorylation of these proteins influences their activities [85–87], a direct effect of phosphorylation on insulin secretion has not been established. We recently found that in MIN6 cells, Rip11, an effector of the small G-protein Rab11, participates in the potentiation of exocytosis by cAMP plus glucose stimulation but not in that of glucose stimulation alone [88]. In addition, Rip11 was found to be phosphorylated by PKA in MIN6 cells. These findings indicate that Rip11, as a substrate of PKA, is involved in the regulation of insulin secretion potentiated by cAMP in pancreatic beta cells.
It is now known that cAMP also potentiates GIIS by a PKA-independent mechanism [84] (Fig. 4a). This mechanism is mediated by the cAMP-binding protein Epac2 (also referred to as cAMP-GEFII; Fig. 4b). Two Epacs, Epac1 (cAMP-GEFI) and Epac2, have been identified [89–91]. Both Epac proteins possess guanine nucleotide exchange factor (GEF) activity towards the small G-proteins Rap1 and Rap2 in a cAMP-dependent manner [89–91]. It has become apparent that Epac proteins are cAMP sensors that regulate several cellular processes independently of PKA. Epac1 mRNA is ubiquitously expressed, while Epac2 mRNA is mainly expressed in neurons, neuroendocrine cells and endocrine cells [34, 89, 90]. Epac1 and Epac2 are each encoded by two genes. Structurally, both Epac proteins have common features: an amino-terminal regulatory region harbouring cAMP-binding domains and a Dishevelled, Egl-10, and Pleckstrin (DEP) domain and a carboxyl-terminal catalytic region harboring an Ras exchange motif (REM) domain, an Ras-association (RA) domain, and a CDC25-homology domain for GEF activity. However, Epac1 possesses one cAMP-binding domain, while Epac2 possesses two cAMP-binding domains. X-ray crystallographic analysis of the inactive and active forms of Epac2 reveal that in the absence of cAMP, the regulatory region covers the catalytic region and autoinhibits GEF activity by hindering the binding of Rap proteins to the CDC25-homology domain [92]. Binding of cAMP to Epac causes a conformational change, thereby eliciting GEF activity toward Rap proteins [92]. Recently, a novel splicing variant was found in mouse adrenal glands [93]. This splicing variant, which lacks the amino-terminal cAMP-binding domain of Epac2, is designated Epac2B (adrenal type), while the original Epac2 is now called Epac2A (brain/beta cell type). A previously identified splicing variant, also lacking the amino-terminal cAMP-binding domain, which is specifically expressed in liver [94], is referred to as Epac2C (liver type). Conformational change of Epac1 induced by its binding to cAMP induces the translocation of Epac1 to the plasma membrane via the DEP domain [95]. Epac2A is localised to the plasma membrane through the interaction of the RA domain with activated Ras proteins [96, 97]. The amino-terminal cAMP-binding domain A of Epac2A also mediates its localisation to the plasma membrane [93]. Localisation of Epac2A to the plasma membrane is independent of its binding to cAMP.
a PKA-dependent and PKA-independent pathways of cAMP-potentiated insulin secretion. AC, adenylyl cyclase. b Functional domains of Epac2A (cAMP-GEFII). DEP, Dishevelled, Egl-10, and Pleckstrin; RA, Ras-association; REM, Ras exchange motif. c Proposed mechanism of potentiation of GIIS by cAMP signalling. Reproduced with permission of the American Society for Clinical Investigation, from [31]; permission conveyed through Copyright Clearance Center, Inc.
Studies of Epac2A null (Epac2a −/−) mice and Rap1 knockdown in clonal mouse beta cells indicate that Epac2A/Rap1 signalling is required for first phase potentiation of glucose-induced insulin granule exocytosis by cAMP [27]. It has been proposed that activation of Epac2A/Rap1 signalling increases the size of the RRP and/or recruitment of insulin granules from the RRP, while PKA signalling increases the size of the RP and/or recruitment of insulin granules from the RP (Fig. 4c) [31]. Rim2α has been found to be essential for Epac2A-mediated potentiation of GIIS by cAMP [43, 83]. Epac2A has also been shown to be involved in mobilisation of Ca2+ from intracellular Ca2+ stores in pancreatic beta cells [98]. The effect of Epac2A on Ca2+ mobilisation has been shown to be mediated by ryanodine receptors and IP3 receptors by studying ryanodine receptor null mice and phospholipase Cε null mice, respectively [98].
cAMP signals are known to be compartmentalised in different regions of cardiac myocytes [99]. Such cAMP compartmentalisation is thought to underlie the distinct biological responses mediated by the different cAMP-increasing ligands. By analogy with the effects of cAMP in cardiac myocytes, cAMP compartmentalisation has also been proposed in pancreatic beta cells [84].
Epac2A as a target of sulfonylurea
Sulfonylureas stimulate insulin secretion by closing KATP channels through binding to SUR1, as mentioned above. Although sulfonylureas were also suggested to act intracellularly to stimulate insulin granule exocytosis [100–102], the direct target was not identified.
To screen for agents and ligands that activate Epac2A, Epac2A fluorescence resonance energy transfer (FRET) sensor, in which the full-length Epac2A was fused amino-terminally to enhanced cyan fluorescent protein (ECFP) and carboxyl-terminally to enhanced yellow fluorescent protein (EYFP; termed C-Epac2A-Y) was established (Fig. 5a) [103]. FRET is the radiationless transfer of energy from an initially excited donor to an acceptor [104]. It is dependent on the proper spectral overlap of the donor and acceptor, their distance from each other and the relative orientation of the chromophore’s transition dipoles. In the case of green fluorescent proteins (GFPs), including ECFP and EYFP, the distance between a donor and an acceptor must be within 5 nm for FRET to be detectable [105]. Epac2A is a closed form in the inactive state, so that ECFP and EYFP are located very close to each other, which causes FRET. Upon binding of cAMP, Epac2A changes its conformation, so that ECFP and EYFP separate away. As a result, FRET does not occur (active state). Utilising the Epac2A FRET sensor, the activation status of Epac2A can be monitored. In the course of screening for agents that activate Epac2A, we found that tolbutamide and glibenclamide, both of which are glucose-lowering sulfonylurea drugs, significantly decreased the FRET response in C-Epac2A-Y transfected cells [103] (Fig. 5b, c). The effect on FRET was confirmed using other sulfonylureas, including chlorpropamide, acetohexamide, and glipizide, all of which significantly decreased the FRET response to different degrees and with varying kinetics. However, gliclazide, another sulfonylurea, did not change FRET. Glinide derivatives, which stimulate insulin secretion by closure of KATP channels by acting directly on SUR1, had no effect on the FRET response. Direct binding of sulfonylurea to Epac2A was confirmed by specific binding of radiolabelled glibenclamide to Epac2A expressed in COS-1 cells. In addition, the sulfonylureas that decreased FRET all activated Rap1 in MIN6 cells, whereas gliclazide did not. These results indicate that Epac2A is a target of sulfonylurea. Moreover, tolbutamide-induced insulin secretion and glibenclamide-induced insulin secretion from isolated pancreatic islets were significantly reduced in Epac2A null mice compared with wild-type mice. However, there was no significant difference in insulin secretion in response to gliclazide. Furthermore, the insulin response to oral administration of tolbutamide alone or to concomitant administration of glucose and tolbutamide in Epac2A null mice was significantly reduced compared with that in wild-type mice, and the glucose-lowering effect of tolbutamide in Epac2A null mice was significantly less than that in wild-type mice. Although closure of the KATP channels is essential for sulfonylureas to stimulate insulin secretion, activation of Epac2A/Rap1 signalling is required for sulfonylureas to exert their full effects with regard to insulin secretion (except for gliclazide). Considering the role of Epac2A/Rap1 signalling in insulin granule exocytosis [27], sulfonylureas may increase the size of the RRP of insulin granules near the plasma membrane (Fig. 5d) [106]. Since Epac2A is also the target of incretin/cAMP signalling, Epac2A is critical for the actions of both sulfonylureas and incretin-related glucose-lowering drugs such as DPP-4 inhibitors and GLP-1 receptor agonists. It is possible that sulfonylurea and cAMP signalling interact with each other through Epac2A, in which case the effects of sulfonylurea on Epac2A might be influenced by cellular cAMP concentrations and vice versa.
a Epac2A FRET sensor. A FRET sensor was constructed in which the full-length Epac2A was sandwiched between ECFP at the N-terminus and EYFP at the C-terminus. FRET occurs in the inactive state (closed form). Upon cAMP binding, Epac2A changes its conformation and becomes the open form. As a result, FRET does not occur. DEP, Dishevelled, Egl-10, and Pleckstrin; RA, Ras-association; REM, Ras exchange motif. b, c Activation of Epac2A by sulfonylureas. Tolbutamide (b) and glibenclamide (c) decrease Epac2A FRET, indicating that they activate Epac2A. The EYFP/ECFP ratio (R) was normalised to R 0 to describe FRET efficiency changes (FRET change = R/R 0), where R 0 is the EYFP/ECFP ratio at time 0. Reproduced from [103] with permission. d Mechanisms of sulfonylurea action in insulin secretion. Closure of KATP channels is required for sulfonylureas to stimulate insulin secretion; activation of Epac2A/Rap1 signalling is required for sulfonylureas to exert their full effect on insulin secretion. ΔΨ, depolarising beta cell membrane, VDDC, voltage-dependent Ca2+ channel. Modified from [106] with permission
Conclusions
GIIS is the principal mechanism of insulin secretion. Potentiation of GIIS by cAMP-increasing ligands such as incretin is also critical for normal regulation of insulin secretion. Sulfonylurea, a glucose-lowering drug widely used for treatment of diabetes, stimulates insulin secretion. Utilising molecular biology and gene technology, it has been shown that the KATP channel is the target of both ATP, an essential signal for GIIS, and sulfonylurea, and that Epac2A is the target of both cAMP, a critical signal for potentiation of GIIS, and sulfonylurea. It is now known that ATP, cAMP, and sulfonylurea interact with one another to facilitate stimulus–secretion coupling in insulin release (Fig. 6). In 1970, Prof. Albert Renold published the article ‘Insulin biosynthesis and secretion – a still unsettled topic’ in The New England Journal of Medicine [107]. Although our understanding of insulin secretion has increased remarkably since that time, the title of the paper remains true.
Abbreviations
- [Ca2+]i :
-
Intracellular calcium concentration
- DAG:
-
Diacylglycerol
- DPP-4:
-
Dipeptidyl peptidase IV
- ECFP:
-
Enhanced cyan fluorescent protein
- Epac:
-
Exchange protein activated by cAMP
- Exoc3l:
-
Exocyst complex component 3-like
- EYFP:
-
Enhanced yellow fluorescent protein
- FRET:
-
Fluorescence resonance energy transfer
- GEF:
-
Guanine nucleotide exchange factor
- GFP:
-
Green fluorescent protein
- GIIS:
-
Glucose-induced insulin secretion
- GIP:
-
Glucose-dependent insulinotropic polypeptide
- GLP-1:
-
Glucagon-like peptide 1
- GR:
-
Glucose-responsive
- IP3 :
-
Inositol 1,4,5-trisphosphate
- KATP channel:
-
ATP-sensitive K+ channel
- PHHI:
-
Persistent hyperinsulinaemic hypoglycaemia of infancy
- PKA:
-
Protein kinase A
- RP:
-
Reserve pool
- RRP:
-
Readily releasable pool
- SUR:
-
Sulfonylurea receptor
- TIRFM:
-
Total internal reflection fluorescence microscopy
- TM:
-
Transmembrane
- TRP:
-
Transient receptor potential
- VMH:
-
Ventromedial hypothalamus
References
Berson SA, Yalow RS (1959) Quantitative aspects of the reaction between insulin and insulin-binding antibody. J Clin Invest 38:1996–2016
Wollheim CB, Sharp GW (1981) Regulation of insulin release by calcium. Physiol Rev 61:914–973
Malaisse WJ, Malaisse-Lagae F (1984) The role of cyclic AMP in insulin release. Experientia 40:1068–1074
Prentki M, Matschinsky FM (1987) Ca2+, cAMP, and phospholipid-derived messengers in coupling mechanisms of insulin secretion. Physiol Rev 67:1185–1248
Davis B, Lazarus NR (1976) An in vitro system for studying insulin release caused by secretory granules–plasma membrane interaction: definition of the system. J Physiol 256:709–729
Grodsky GM, Batts AA, Bennett LL, Vcella C, McWilliams NB, Smith DF (1963) Effects of carbohydrates on secretion of insulin from isolated rat pancreas. Am J Physiol 205:638–644
Coore HG, Randle PJ (1964) Regulation of insulin secretion studied with pieces of rabbit pancreas incubated in vitro. Biochem J 93:66–78
Hedeskov CJ (1980) Mechanism of glucose-induced insulin secretion. Physiol Rev 60:442–509
Noma A (1983) ATP-regulated K+ channels in cardiac muscle. Nature 305:147–148
Cook DL, Hales CN (1984) Intracellular ATP directly blocks K+ channels in pancreatic B-cells. Nature 311:271–273
Ashcroft FM, Harrison DE, Ashcroft SJ (1984) Glucose induces closure of single potassium channels in isolated rat pancreatic β-cells. Nature 312:446–448
Rorsman P, Trube G (1985) Glucose dependent K+-channels in pancreatic β-cells are regulated by intracellular ATP. Pflugers Arch 405:305–309
Ashcroft FM, Rorsman P (1989) Electrophysiology of the pancreatic β-cell. Prog Biophys Mol Biol 54:87–143
Henquin JC (2009) Regulation of insulin secretion: a matter of phase control and amplitude modulation. Diabetologia 52:739–751
Detimary P, Gilon P, Nenquin M, Henquin JC (1994) Two sites of glucose control of insulin release with distinct dependence on the energy state in pancreatic B cells. Biochem J 297:455–461
Eliasson L, Renstrom E, Ding WG, Proks P, Rorsman P (1997) Rapid ATP-dependent priming of secretory granules precedes Ca2+-induced exocytosis in mouse pancreatic B cells. J Physiol 503:399–412
Takahashi N, Kadowaki T, Yazaki Y, Ellis-Davies GC, Miyashita Y, Kasai H (1999) Post-priming actions of ATP on Ca2+-dependent exocytosis in pancreatic β cells. Proc Natl Acad Sci USA 96:760–765
Nolan CJ, Madiraju MS, Delghingaro-Augusto V, Peyot ML, Prentki M (2006) Fatty acid signaling in the β-cell and insulin secretion. Diabetes 55(Suppl 2):S16–S23
Curry DL, Bennett LL, Grodsky GM (1968) Dynamics of insulin secretion by the perfused rat pancreas. Endocrinology 83:572–584
Rorsman P, Renstrom E (2003) Insulin granule dynamics in pancreatic β cells. Diabetologia 46:1029–1045
Porte D Jr (1991) Banting lecture 1990. β-cells in type II diabetes mellitus. Diabetes 40:166–180
Südhof TC, Rizo J (2011) Synaptic vesicle exocytosis. Cold Spring Harb Perspect Biol 3:a005637
Eliasson L, Abdulkader F, Braun M, Galvanovskis J, Hoppa MB, Rorsman P (2008) Novel aspects of the molecular mechanisms controlling insulin secretion. J Physiol 586:3313–3324
Straub SG, Shanmugam G, Sharp GW (2004) Stimulation of insulin release by glucose is associated with an increase in the number of docked granules in the β-cells of rat pancreatic islets. Diabetes 53:3179–3183
Tsuboi T, Zhao C, Terakawa S, Rutter GA (2000) Simultaneous evanescent wave imaging of insulin vesicle membrane and cargo during a single exocytotic event. Curr Biol 10:1307–1310
Ohara-Imaizumi M, Nakamichi Y, Tanaka T, Ishida H, Nagamatsu S (2002) Imaging exocytosis of single insulin secretory granules with evanescent wave microscopy: distinct behavior of granule motion in biphasic insulin release. J Biol Chem 277:3805–3808
Shibasaki T, Takahashi H, Miki T et al (2007) Essential role of Epac2/Rap1 signaling in regulation of insulin granule dynamics by cAMP. Proc Natl Acad Sci USA 104:19333–19338
Kasai K, Fujita T, Gomi H, Izumi T (2008) Docking is not a prerequisite but a temporal constraint for fusion of secretory granules. Traffic 9:1191–1203
Axelrod D (1981) Cell–substrate contacts illuminated by total internal reflection fluorescence. J Cell Biol 89:141–145
Takahashi N, Hatakeyama H, Okado H, Noguchi J, Ohno M, Kasai H (2010) SNARE conformational changes that prepare vesicles for exocytosis. Cell Metab 12:19–29
Seino S, Shibasaki T, Minami K (2011) Dynamics of insulin secretion and the clinical implications for obesity and diabetes. J Clin Invest 121:2118–2125
Seino S, Takahashi H, Fujimoto W, Shibasaki T (2009) Roles of cAMP signalling in insulin granule exocytosis. Diabetes Obes Metab 11(Suppl 4):180–188
Wang Z, Thurmond DC (2009) Mechanisms of biphasic insulin-granule exocytosis—roles of the cytoskeleton, small GTPases and SNARE proteins. J Cell Sci 122:893–903
Ozaki N, Shibasaki T, Kashima Y et al (2000) cAMP-GEFII is a direct target of cAMP in regulated exocytosis. Nat Cell Biol 2:805–811
Dulubova I, Lou X, Lu J et al (2005) A Munc13/RIM/Rab3 tripartite complex: from priming to plasticity? EMBO J 24:2839–2850
Fukuda M (2003) Distinct Rab binding specificity of Rim1, Rim2, rabphilin, and Noc2. Identification of a critical determinant of Rab3A/Rab27A recognition by Rim2. J Biol Chem 278:15373–15380
Ohara-Imaizumi M, Ohtsuka T, Matsushima S et al (2005) ELKS, a protein structurally related to the active zone-associated protein CAST, is expressed in pancreatic β cells and functions in insulin exocytosis: interaction of ELKS with exocytotic machinery analyzed by total internal reflection fluorescence microscopy. Mol Biol Cell 16:3289–3300
Inoue E, Deguchi-Tawarada M, Takao-Rikitsu E et al (2006) ELKS, a protein structurally related to the active zone protein CAST, is involved in Ca2+-dependent exocytosis from PC12 cells. Genes Cells 11:659–672
Fujimoto K, Shibasaki T, Yokoi N et al (2002) Piccolo, a Ca2+ sensor in pancreatic β-cells. Involvement of cAMP-GEFII⋅Rim2⋅Piccolo complex in cAMP-dependent exocytosis. J Biol Chem 277:50497–50502
Shibasaki T, Sunaga Y, Fujimoto K, Kashima Y, Seino S (2004) Interaction of ATP sensor, cAMP sensor, Ca2+ sensor, and voltage-dependent Ca2+ channel in insulin granule exocytosis. J Biol Chem 279:7956–7961
Gustavsson N, Lao Y, Maximov A et al (2008) Impaired insulin secretion and glucose intolerance in synaptotagmin-7 null mutant mice. Proc Natl Acad Sci USA 105:3992–3997
Iezzi M, Kouri G, Fukuda M, Wollheim CB (2004) Synaptotagmin V and IX isoforms control Ca2+-dependent insulin exocytosis. J Cell Sci 117:3119–3127
Yasuda T, Shibasaki T, Minami K et al (2010) Rim2α determines docking and priming states in insulin granule exocytosis. Cell Metab 12:117–129
He B, Guo W (2009) The exocyst complex in polarized exocytosis. Curr Opin Cell Biol 21:537–542
Saito T, Shibasaki T, Seino S (2008) Involvement of Exoc3l, a protein structurally related to the exocyst subunit Sec6, in insulin secretion. Biomed Res 29:85–91
Weir GC, Mojsov S, Hendrick GK, Habener JF (1989) Glucagonlike peptide I (7–37) actions on endocrine pancreas. Diabetes 38:338–342
Gembal M, Detimary P, Gilon P, Gao ZY, Henquin JC (1993) Mechanisms by which glucose can control insulin release independently from its action on adenosine triphosphate-sensitive K+ channels in mouse B cells. J Clin Invest 91:871–880
Holz GG 4th, Kuhtreiber WM, Habener JF (1993) Pancreatic β-cells are rendered glucose-competent by the insulinotropic hormone glucagon-like peptide-1(7–37). Nature 361:362–365
Miki T, Minami K, Shinozaki H et al (2005) Distinct effects of glucose-dependent insulinotropic polypeptide and glucagon-like peptide-1 on insulin secretion and gut motility. Diabetes 54:1056–1063
Fujimoto W, Miki T, Ogura T et al (2009) Niflumic acid-sensitive ion channels play an important role in the induction of glucose-stimulated insulin secretion by cyclic AMP in mice. Diabetologia 52:863–872
Sturgess NC, Ashford ML, Cook DL, Hales CN (1985) The sulphonylurea receptor may be an ATP-sensitive potassium channel. Lancet 2:474–475
Aguilar-Bryan L, Nichols CG, Wechsler SW et al (1995) Cloning of the β cell high-affinity sulfonylurea receptor: a regulator of insulin secretion. Science 268:423–426
Inagaki N, Gonoi T, Clement JP 4th et al (1995) Reconstitution of I KATP: an inward rectifier subunit plus the sulfonylurea receptor. Science 270:1166–1170
Sakura H, Ammala C, Smith PA, Gribble FM, Ashcroft FM (1995) Cloning and functional expression of the cDNA encoding a novel ATP-sensitive potassium channel subunit expressed in pancreatic β-cells, brain, heart and skeletal muscle. FEBS Letters 377:338–344
Aguilar-Bryan L, Bryan J (1999) Molecular biology of adenosine triphosphate-sensitive potassium channels. Endocrine reviews 20:101–135
Seino S (1999) ATP-sensitive potassium channels: a model of heteromultimeric potassium channel/receptor assemblies. Annu Rev Physiol 61:337–362
Seino S, Miki T (2003) Physiological and pathophysiological roles of ATP-sensitive K+ channels. Prog Biophys Mol Biol 81:133–176
Gribble FM, Reimann F (2003) Sulphonylurea action revisited: the post-cloning era. Diabetologia 46:875–891
Winkler M, Stephan D, Bieger S, Kuhner P, Wolff F, Quast U (2007) Testing the bipartite model of the sulfonylurea receptor binding site: binding of A-, B-, and A + B-site ligands. J Pharmacol Exp Ther 322:701–708
Proks P, Ashcroft FM (2009) Modeling KATP channel gating and its regulation. Prog Biophys Mol Biol 99:7–19
Miki T, Tashiro F, Iwanaga T et al (1997) Abnormalities of pancreatic islets by targeted expression of a dominant-negative KATP channel. Proc Natl Acad Sci USA 94:11969–11973
Miki T, Nagashima K, Tashiro F et al (1998) Defective insulin secretion and enhanced insulin action in KATP channel-deficient mice. Proc Natl Acad Sci USA 95:10402–10406
Seghers V, Nakazaki M, DeMayo F, Aguilar-Bryan L, Bryan J (2000) Sur1 knockout mice. A model for KATP channel-independent regulation of insulin secretion. J Biol Chem 275:9270–9277
Shiota C, Larsson O, Shelton KD et al (2002) Sulfonylurea receptor type 1 knock-out mice have intact feeding-stimulated insulin secretion despite marked impairment in their response to glucose. J Biol Chem 277:37176–37183
Ravier MA, Nenquin M, Miki T, Seino S, Henquin JC (2009) Glucose controls cytosolic Ca2+ and insulin secretion in mouse islets lacking adenosine triphosphate-sensitive K+ channels owing to a knockout of the pore-forming subunit Kir6.2. Endocrinology 150:33–45
Gloyn AL, Pearson ER, Antcliff JF et al (2004) Activating mutations in the gene encoding the ATP-sensitive potassium-channel subunit Kir6.2 and permanent neonatal diabetes. N Engl J Med 350:1838–1849
Remedi MS, Nichols CG (2009) Hyperinsulinism and diabetes: genetic dissection of β cell metabolism–excitation coupling in mice. Cell Metab 10:442–453
Ashcroft FM (2010) New uses for old drugs: neonatal diabetes and sulphonylureas. Cell Metab 11:179–181
Borg WP, During MJ, Sherwin RS, Borg MA, Brines ML, Shulman GI (1994) Ventromedial hypothalamic lesions in rats suppress counterregulatory responses to hypoglycemia. J Clin Invest 93:1677–1682
Miki T, Liss B, Minami K et al (2001) ATP-sensitive K+ channels in the hypothalamus are essential for the maintenance of glucose homeostasis. Nat Neurosci 4:507–512
MacDonald PE, de Marinis YZ, Ramracheya R et al (2007) A KATP channel-dependent pathway within α cells regulates glucagon release from both rodent and human islets of Langerhans. PLoS Biol 5:e143
Wang PH, Moller D, Flier JS, Nayak RC, Smith RJ (1989) Coordinate regulation of glucose transporter function, number, and gene expression by insulin and sulfonylureas in L6 rat skeletal muscle cells. J Clin Invest 84:62–67
Pulido N, Casla A, Suarez A, Casanova B, Arrieta FJ, Rovira A (1996) Sulphonylurea stimulates glucose uptake in rats through an ATP-sensitive K+ channel dependent mechanism. Diabetologia 39:22–27
Minami K, Morita M, Saraya A et al (2003) ATP-sensitive K+ channel-mediated glucose uptake is independent of IRS-1/phosphatidylinositol 3-kinase signaling. Am J Physiol Endocrinol Metab 285:E1289–E1296
Chutkow WA, Samuel V, Hansen PA et al (2001) Disruption of Sur2-containing KATP channels enhances insulin-stimulated glucose uptake in skeletal muscle. Proc Natl Acad Sci USA 98:11760–11764
Minami K, Miki T, Kadowaki T, Seino S (2004) Roles of ATP-sensitive K+ channels as metabolic sensors: studies of Kir6.x null mice. Diabetes 53(Suppl 3):S176–S180
Drucker DJ (2006) The biology of incretin hormones. Cell Metab 3:153–165
Holst JJ (2007) The physiology of glucagon-like peptide 1. Physiol Rev 87:1409–1439
Nauck MA (2009) Unraveling the science of incretin biology. Am J Med 122:S3–S10
Winzell MS, Ahren B (2007) Role of VIP and PACAP in islet function. Peptides 28:1805–1813
Delmeire D, Flamez D, Hinke SA, Cali JJ, Pipeleers D, Schuit F (2003) Type VIII adenylyl cyclase in rat β cells: coincidence signal detector/generator for glucose and GLP-1. Diabetologia 46:1383–1393
Guenifi A, Portela-Gomes GM, Grimelius L, Efendic S, Abdel-Halim SM (2000) Adenylyl cyclase isoform expression in non-diabetic and diabetic Goto–Kakizaki (GK) rat pancreas. Evidence for distinct overexpression of type-8 adenylyl cyclase in diabetic GK rat islets. Histochem Cell Biol 113:81–89
Kashima Y, Miki T, Shibasaki T et al (2001) Critical role of cAMP–GEFII–Rim2 complex in incretin-potentiated insulin secretion. J Biol Chem 276:46046–46053
Seino S, Shibasaki T (2005) PKA-dependent and PKA-independent pathways for cAMP-regulated exocytosis. Physiol Rev 85:1303–1342
Leiser M, Fleischer N (1996) cAMP-dependent phosphorylation of the cardiac-type α1 subunit of the voltage-dependent Ca2+ channel in a murine pancreatic β-cell line. Diabetes 45:1412–1418
Safayhi H, Haase H, Kramer U et al (1997) L-type calcium channels in insulin-secreting cells: biochemical characterization and phosphorylation in RINm5F cells. Mol Endocrinol 11:619–629
Thorens B, Deriaz N, Bosco D et al (1996) Protein kinase A-dependent phosphorylation of GLUT2 in pancreatic β cells. J Biol Chem 271:8075–8081
Sugawara K, Shibasaki T, Mizoguchi A, Saito T, Seino S (2009) Rab11 and its effector Rip11 participate in regulation of insulin granule exocytosis. Genes Cells 14:445–456
de Rooij J, Zwartkruis FJ, Verheijen MH et al (1998) Epac is a Rap1 guanine-nucleotide-exchange factor directly activated by cyclic AMP. Nature 396:474–477
Kawasaki H, Springett GM, Mochizuki N et al (1998) A family of cAMP-binding proteins that directly activate Rap1. Science 282:2275–2279
de Rooij J, Rehmann H, van Triest M, Cool RH, Wittinghofer A, Bos JL (2000) Mechanism of regulation of the Epac family of cAMP-dependent RapGEFs. J Biol Chem 275:20829–20836
Gloerich M, Bos JL (2010) Epac: defining a new mechanism for cAMP action. Annu Rev Pharmacol Toxicol 50:355–375
Niimura M, Miki T, Shibasaki T, Fujimoto W, Iwanaga T, Seino S (2009) Critical role of the N-terminal cyclic AMP-binding domain of Epac2 in its subcellular localization and function. J Cell Physiol 219:652–658
Ueno H, Shibasaki T, Iwanaga T et al (2001) Characterization of the gene EPAC2: structure, chromosomal localization, tissue expression, and identification of the liver-specific isoform. Genomics 78:91–98
Ponsioen B, Gloerich M, Ritsma L, Rehmann H, Bos JL, Jalink K (2009) Direct spatial control of Epac1 by cyclic AMP. Mol Cell Biol 29:2521–2531
Li Y, Asuri S, Rebhun JF, Castro AF, Paranavitana NC, Quilliam LA (2006) The RAP1 guanine nucleotide exchange factor Epac2 couples cyclic AMP and Ras signals at the plasma membrane. J Biol Chem 281:2506–2514
Liu C, Takahashi M, Li Y et al (2008) Ras is required for the cyclic AMP-dependent activation of Rap1 via Epac2. Mol Cell Biol 28:7109–7125
Leech CA, Dzhura I, Chepurny OG et al (2011) Molecular physiology of glucagon-like peptide-1 insulin secretagogue action in pancreatic β cells. Prog Biophys Mol Biol 107:236–247
Vandecasteele G, Rochais F, Abi-Gerges A, Fischmeister R (2006) Functional localization of cAMP signalling in cardiac myocytes. Biochem Soc Trans 34:484–488
Ozanne SE, Guest PC, Hutton JC, Hales CN (1995) Intracellular localization and molecular heterogeneity of the sulphonylurea receptor in insulin-secreting cells. Diabetologia 38:277–282
Eliasson L, Renstrom E, Ammala C et al (1996) PKC-dependent stimulation of exocytosis by sulfonylureas in pancreatic β cells. Science 271:813–815
Eliasson L, Ma X, Renstrom E et al (2003) SUR1 regulates PKA-independent cAMP-induced granule priming in mouse pancreatic B cells. J Gen Physiol 121:181–197
Zhang CL, Katoh M, Shibasaki T et al (2009) The cAMP sensor Epac2 is a direct target of antidiabetic sulfonylurea drugs. Science 325:607–610
Lakowicz JR (1999) Energy transfer. In: Lakowicz JR (ed) Principles of fluorescence spectroscopy. Kluwer Academic, New York, pp 368–391
Miyawaki A, Tsien RY (2000) Monitoring protein conformations and interactions by fluorescence resonance energy transfer between mutants of green fluorescent protein. Methods Enzymol 327:472–500
Seino S, Zhang CL, Shibasaki T (2010) Sulfonylurea action re-revisited. J Diabetes Invest 1:37–39
Renold AE (1970) Insulin biosynthesis and secretion—a still unsettled topic. N Engl J Med 282:173–182
Acknowledgements
This review was presented in partial form as the Albert Renold Prize Lecture at the European Association for the Study of Diabetes (EASD) 2010, Stockholm, Sweden. I thank present and former colleagues in our laboratory and our collaborators for their involvement in the studies in this review. I am especially grateful to T. Shibasaki, N. Yokoi, and K Minami for critical reading of the manuscript along with their helpful suggestions and G. H. Honkawa for her assistance in preparing the manuscript. The studies of our laboratory were supported by a CREST grant from the Japan Science and Technology Agency and Grant-in-Aid for Scientific Research.
Contribution statement
The author was responsible for the conception, design and drafting of the manuscript, and approved the final version for publication.
Author information
Authors and Affiliations
Corresponding author
Additional information
This review was invited based on the Albert Renold Prize Lecture at the EASD, September 2010.
Rights and permissions
About this article
Cite this article
Seino, S. Cell signalling in insulin secretion: the molecular targets of ATP, cAMP and sulfonylurea. Diabetologia 55, 2096–2108 (2012). https://doi.org/10.1007/s00125-012-2562-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-012-2562-9