Abstract
Background
The safety and feasibility of hepatectomy for hepatocellular carcinoma (HCC) in the elderly population have not been defined to date.
Methods
A single-center, retrospective cohort study was conducted with 104 patients who underwent hepatectomy for HCC from 2005 to 2010. The patients were divided into two groups, the elderly group (age, ≥75 years; n = 22) and the nonelderly group (age, <75 years; n = 82), for comparison of short- and long-term outcomes.
Results
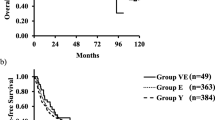
More patients were categorized as preoperative Eastern Cooperative Oncology Group (ECOG) performance status 1 in the elderly group (32 %) than in the nonelderly group (6 %) (P = 0.003). Complications with a Clavien–Dindo classification of grade 3a or higher were more frequently observed in the elderly group (41 %) than in the nonelderly group (17 %) (P = 0.006). Multivariate logistic regression showed ECOG performance status 1 as the only independent predictor of complications classified as Clavien–Dindo grade 3a or higher. The in-hospital mortality rates were similar between the two groups (P = 0.20). During a median follow-up period of 47 months, the unadjusted 5-year recurrence-free survival rates were similar in the elderly (25 %) and nonelderly (33 %) groups (P = 0.80). Multiple tumors and high alpha-fetoprotein levels emerged as independent negative indicators of recurrence-free survival using multivariate Cox analyses. The adjusted risk for recurrence was not elevated in the elderly group (hazard ratio [HR], 0.92; 95 % confidence interval [CI] 0.50–1.68; P = 0.78).
Conclusions
Despite the more frequent occurrence of complications with a Clavien–Dindo grade of 3a or higher among the elderly patients undergoing hepatectomy for HCC, their mortality and recurrence rates were comparable with those of the nonelderly patients. Therefore, age alone is not a determinant of surgical candidacy for HCC.

Similar content being viewed by others
References
El-Serag HB. Hepatocellular carcinoma. N Engl J Med. 2011;365:1118–27.
Tsujita E, Utsunomiya T, Ohta M, et al. Outcome of repeat hepatectomy in patients with hepatocellular carcinoma aged 75 years and older. Surgery. 2010;147:696–703.
Nanashima A, Abo T, Nonaka T, et al. Prognosis of patients with hepatocellular carcinoma after hepatic resection: are elderly patients suitable for surgery? J Surg Oncol. 2011;104:284–91.
Menon KV, Al-Mukhtar A, Aldouri A, Prasad RK, Lodge PA, Toogood GJ. Outcomes after major hepatectomy in elderly patients. J Am Coll Surg. 2006;203:677–83.
Reddy SK, Barbas AS, Turley RS, et al. Major liver resection in elderly patients: a multi-institutional analysis. J Am Coll Surg. 2011;212:787–95.
Melloul E, Halkic N, Raptis DA, Tempia A, Demartines N. Right hepatectomy in patients over 70 years of age: an analysis of liver function and outcome. World J Surg. 2012;36:2161–70.
de la Fuente SG1, Bennett KM, Scarborough JE. Functional status determines postoperative outcomes in elderly patients undergoing hepatic resections. J Surg Oncol. 2013;107:865–70.
Portolani N1, Baiocchi GL, Coniglio A, Tiberio GA, Prestini K, Gheza F, Benetti A, et al. Limited liver resection: a good indication for the treatment of hepatocellular carcinoma in elderly patients. Jpn J Clin Oncol. 2011;41:1358–65.
Huang J, Li BK, Chen GH, Li JQ, Zhang YQ, Li GH, Yuan YF. Long-term outcomes and prognostic factors of elderly patients with hepatocellular carcinoma undergoing hepatectomy. J Gastrointest Surg. 2009;13:1627–35.
Yamada S, Shimada M, Miyake H, et al. Outcome of hepatectomy in super-elderly patients with hepatocellular carcinoma. Hepatol Res. 2012;42:454–8.
Tsujita E, Utsunomiya T, Yamashita Y, et al. Outcome of hepatectomy in hepatocellular carcinoma patients aged 80 years and older. Hepatogastroenterology. 2012;59:1553–5.
Makuuchi M, Kosuge T, Takayama T, Yamazaki S, Kakazu T, Miyagawa S, Kawasaki S. Surgery for small liver cancers. Semin Surg Oncol. 1993;9:298–304.
Clavien PA, Barkun J, DeOliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–96.
The French METAVIR Cooperative Study Group. Intraovserver and interobserver variations in liver biopsy interpretation in patients with chronic hepatitis C. Hepatology. 1994;20:15–20.
Robinson TN, Eiseman B, Wallace JI, et al. Redefining geriatric preoperative assessment using frailty, disability, and comorbidity. Ann Surg. 2009;250:449–55.
Makary MA, Segev DL, Pronovost PJ, et al. Frailty as a predictor of surgical outcomes in older patients. J Am Coll Surg. 2010;210:901–8.
Chow WB, Rosenthal RA, Merkow RP, et al. Optimal preoperative assessment of the geriatric surgical patient: a best practices guideline from the American College of Surgeons National Surgical Quality Improvement Program and the American Geriatrics Society. J Am Coll Surg. 2012; 215:453–66.
Hamaker ME, Jonker JM, de Rooij SE, Vos AG, Smorenburg CH, van Munster BC. Frailty screening methods for predicting outcome of a comprehensive geriatric assessment in elderly patients with cancer: a systematic review. Lancet Oncol. 2012;13:e437–44.
Revenig LM, Canter DJ, Taylor MD, et al. Too frail for surgery? Initial results of a large multidisciplinary prospective study examining preoperative variables predictive of poor surgical outcomes. J Am Coll Surg. 2013;217:665–70.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39:412–23.
Shimada H, Makizako H, Doi T, et al. Combined prevalence of frailty and mild cognitive impairment in a population of elderly Japanese people. J Am Med Dir Assoc. 2013;14:518–24.
Dale W, Hemmerich J, Kamm A, et al. Geriatric assessment improves prediction of surgical outcomes in older adults undergoing pancreaticoduodenectomy: a prospective cohort study. Ann Surg. 2014;259:960–5.
Dagher I, Belli G, Fantini C, et al. Laparoscopic hepatectomy for hepatocellular carcinoma: a European experience. J Am Coll Surg. 2010;211:16–23.
Han HS, Yoon YS, Cho JY, Hwang DW. Laparoscopic liver resection for hepatocellular carcinoma: Korean experiences. Liver Cancer. 2013;2:25–30.
Cheung TT, Poon RT, Yuen WK, et al. Long-term survival analysis of pure laparoscopic versus open hepatectomy for hepatocellular carcinoma in patients with cirrhosis: a single-center experience. Ann Surg. 2013;257:506–11.
Kanazawa A, Tsukamoto T, Shimizu S, et al. Impact of laparoscopic liver resection for hepatocellular carcinoma with F4-liver cirrhosis. Surg Endosc. 2013;27:2592–7.
Memeo R, de’Angelis N, Compagnon P, et al. Laparoscopic vs open liver resection for hepatocellular carcinoma of cirrhotic liver: a case-control study. World J Surg. 2014;38:2919–26.
Conflict of interest
There are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Kishida, N., Hibi, T., Itano, O. et al. Validation of Hepatectomy for Elderly Patients with Hepatocellular Carcinoma. Ann Surg Oncol 22, 3094–3101 (2015). https://doi.org/10.1245/s10434-014-4350-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4350-x