Abstract
Background
Preclinical left ventricular diastolic dysfunction (LVDD) is a high-risk state for heart failure. Kidney dysfunction is a known risk factor for heart failure, but its association with asymptomatic LVDD is not well-known.
Methods
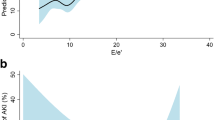
A hospital-based retrospective cohort study was conducted on patients who underwent echocardiogram between 2006 and 2016 to assess the association between baseline kidney function and LVDD on echocardiogram. E/e′ ratio was defined as the ratio of peak velocity of early diastolic left ventricular inflow (E) to mitral annular velocity (e′). The primary outcome was time to development of LVDD, which was defined as E/e′ ratio > 14. The changes in the E/e′ ratio and other echocardiographic parameters were assessed using a mixed effects model.
Results
Among 1167 patients, the mean age was 61 years, and the mean baseline E/e′ ratio and ejection fraction were 9.6 and 69%, respectively. During a median follow-up of 3.2 years, 231 (19.8%) people developed LVDD. According to eGFR (mL/min/1.73 m2), the risk for LVDD based on hazard ratio [95% confidence interval (95% CI)] was 1.20 (0.82, 1.75) for 60 to < 90, 1.42 (0.87, 2.31) for 45 to < 60, and 2.57 (1.61, 4.09) for < 45 (P trend < 0.001). The adjusted risks (95% CI) for annual change in E/e′ ratio was 0.09 (0.03, 0.14) overall and 0.28 (0.11, 0.45) in the lowest eGFR group; the trend in changes in annual E/e′ ratio by baseline eGFR was significant (P trend = 0.01).
Conclusions
Relatively low kidney function was related with the risks for LVDD. Long-term cohort studies are warranted to confirm the association between LVDD and symptomatic heart failure in patients with kidney dysfunction.
Graphic abstract


Similar content being viewed by others
Availability of data and material (data transparency)
The datasets used and/ or analyzed in the current study are available from the corresponding author with the permission of the ethics committee upon reasonable request.
References
Lund LH, Savarese G (2017) Global public health burden of heart failure. Card Fail Rev. https://doi.org/10.15420/cfr.2016:25:2
Bansal N, Zelnick L, Bhat Z, Dobre M, He J, Lash J, Jaar B, Mehta R, Raj D, Rincon-Choles H, Saunders M, Schrauben S, Weir M, Wright J, Go AS, Investigators CS (2019) Burden and outcomes of heart failure hospitalizations in adults with chronic kidney disease. J Am Coll Cardiol 73(21):2691–2700. https://doi.org/10.1016/j.jacc.2019.02.071
Damman K, Valente MA, Voors AA, O’Connor CM, van Veldhuisen DJ, Hillege HL (2014) Renal impairment, worsening renal function, and outcome in patients with heart failure: an updated meta-analysis. Eur Heart J 35(7):455–469. https://doi.org/10.1093/eurheartj/eht386
Writing Committee M, Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Drazner MH, Fonarow GC, Geraci SA, Horwich T, Januzzi JL, Johnson MR, Kasper EK, Levy WC, Masoudi FA, McBride PE, McMurray JJ, Mitchell JE, Peterson PN, Riegel B, Sam F, Stevenson LW, Tang WH, Tsai EJ, Wilkoff BL, American College of Cardiology Foundation/American Heart Association Task Force on Practice G (2013) 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation 128(16):e240–e327. https://doi.org/10.1161/CIR.0b013e31829e8776
Ziaeian B, Fonarow GC (2016) Epidemiology and aetiology of heart failure. Nat Rev Cardiol 13(6):368–378. https://doi.org/10.1038/nrcardio.2016.25
Wan SH, Vogel MW, Chen HH (2014) Pre-clinical diastolic dysfunction. J Am Coll Cardiol 63(5):407–416. https://doi.org/10.1016/j.jacc.2013.10.063
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3, Dokainish H, Edvardsen T, Flachskampf FA, Gillebert TC, Klein AL, Lancellotti P, Marino P, Oh JK, Popescu BA, Waggoner AD (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 29(4):277–314. https://doi.org/10.1016/j.echo.2016.01.011
McAlister FA, Ezekowitz J, Tonelli M, Armstrong PW (2004) Renal insufficiency and heart failure: prognostic and therapeutic implications from a prospective cohort study. Circulation 109(8):1004–1009. https://doi.org/10.1161/01.CIR.0000116764.53225.A9
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, Yamagata K, Tomino Y, Yokoyama H, Hishida A, Collaborators developing the Japanese equation for estimated GFR (2009) Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 53(6):982–992. https://doi.org/10.1053/j.ajkd.2008.12.034
Powell BD, Redfield MM, Bybee KA, Freeman WK, Rihal CS (2006) Association of obesity with left ventricular remodeling and diastolic dysfunction in patients without coronary artery disease. Am J Cardiol 98(1):116–120. https://doi.org/10.1016/j.amjcard.2006.01.063
Solomon SD, Janardhanan R, Verma A, Bourgoun M, Daley WL, Purkayastha D, Lacourcière Y, Hippler SE, Fields H, Naqvi TZ, Mulvagh SL, Arnold JMO, Thomas JD, Zile MR, Aurigemma GP (2007) Effect of angiotensin receptor blockade and antihypertensive drugs on diastolic function in patients with hypertension and diastolic dysfunction: a randomised trial. Lancet 369(9579):2079–2087. https://doi.org/10.1016/s0140-6736(07)60980-5
Liu JE, Robbins DC, Palmieri V, Bella JN, Roman MJ, Fabsitz R, Howard BV, Welty TK, Lee ET, Devereux RB (2003) Association of albuminuria with systolic and diastolic left ventricular dysfunction in type 2 diabetes. J Am Coll Cardiol 41(11):2022–2028. https://doi.org/10.1016/s0735-1097(03)00403-0
Elesber AA, Redfield MM, Rihal CS, Prasad A, Lavi S, Lennon R, Mathew V, Lerman LO, Lerman A (2007) Coronary endothelial dysfunction and hyperlipidemia are independently associated with diastolic dysfunction in humans. Am Heart J 153(6):1081–1087. https://doi.org/10.1016/j.ahj.2007.03.007
Poirier P, Bogaty P, Garneau C, Marois L, Dumesnil JG (2001) Diastolic dysfunction in normotensive men with well-controlled type 2 diabetes: importance of maneuvers in echocardiographic screening for preclinical diabetic cardiomyopathy. Diabetes Care 24(1):5–10. https://doi.org/10.2337/diacare.24.1.5
Ahmed A, Rich MW, Sanders PW, Perry GJ, Bakris GL, Zile MR, Love TE, Aban IB, Shlipak MG (2007) Chronic kidney disease associated mortality in diastolic versus systolic heart failure: a propensity matched study. Am J Cardiol 99(3):393–398. https://doi.org/10.1016/j.amjcard.2006.08.042
Dries DL, Exner DV, Domanski MJ, Greenberg B, Stevenson LW (2000) The prognostic implications of renal insufficiency in asymptomatic and symptomatic patients with left ventricular systolic dysfunction. J Am Coll Cardiol 35(3):681–689. https://doi.org/10.1016/s0735-1097(99)00608-7
Dini FL, Demmer RT, Simioniuc A, Morrone D, Donati F, Guarini G, Orsini E, Caravelli P, Marzilli M, Colombo PC (2012) Right ventricular dysfunction is associated with chronic kidney disease and predicts survival in patients with chronic systolic heart failure. Eur J Heart Fail 14(3):287–294. https://doi.org/10.1093/eurjhf/hfr176
Mohammed SF, Hussain I, AbouEzzeddine OF, Takahama H, Kwon SH, Forfia P, Roger VL, Redfield MM (2014) Right ventricular function in heart failure with preserved ejection fraction: a community-based study. Circulation 130(25):2310–2320. https://doi.org/10.1161/CIRCULATIONAHA.113.008461
Caballero L, Kou S, Dulgheru R, Gonjilashvili N, Athanassopoulos GD, Barone D, Baroni M, Cardim N, Gomez de Diego JJ, Oliva MJ, Hagendorff A, Hristova K, Lopez T, Magne J, Martinez C, de la Morena G, Popescu BA, Penicka M, Ozyigit T, Rodrigo Carbonero JD, Salustri A, Van De Veire N, Von Bardeleben RS, Vinereanu D, Voigt JU, Zamorano JL, Bernard A, Donal E, Lang RM, Badano LP, Lancellotti P (2015) Echocardiographic reference ranges for normal cardiac Doppler data: results from the NORRE Study. Eur Heart J Cardiovasc Imaging 16(9):1031–1041. https://doi.org/10.1093/ehjci/jev083
Diez J, Gonzalez A, Lopez B, Querejeta R (2005) Mechanisms of disease: pathologic structural remodeling is more than adaptive hypertrophy in hypertensive heart disease. Nat Clin Pract Cardiovasc Med 2(4):209–216. https://doi.org/10.1038/ncpcardio0158
Simonetti OP, Kim RJ, Fieno DS, Hillenbrand HB, Wu E, Bundy JM, Finn JP, Judd RM (2001) An improved MR imaging technique for the visualization of myocardial infarction. Radiology 218(1):215–223. https://doi.org/10.1148/radiology.218.1.r01ja50215
Mark PB, Johnston N, Groenning BA, Foster JE, Blyth KG, Martin TN, Steedman T, Dargie HJ, Jardine AG (2006) Redefinition of uremic cardiomyopathy by contrast-enhanced cardiac magnetic resonance imaging. Kidney Int 69(10):1839–1845. https://doi.org/10.1038/sj.ki.5000249
Edwards NC, Moody WE, Yuan M, Hayer MK, Ferro CJ, Townend JN, Steeds RP (2015) Diffuse interstitial fibrosis and myocardial dysfunction in early chronic kidney disease. Am J Cardiol 115(9):1311–1317. https://doi.org/10.1016/j.amjcard.2015.02.015
Toyama T, Neuen BL, Jun M, Ohkuma T, Neal B, Jardine MJ, Heerspink HL, Wong MG, Ninomiya T, Wada T, Perkovic V (2019) Effect of SGLT2 inhibitors on cardiovascular, renal and safety outcomes in patients with type 2 diabetes mellitus and chronic kidney disease: a systematic review and meta-analysis. Diabetes Obes Metab 21(5):1237–1250. https://doi.org/10.1111/dom.13648
Acknowledgements
We deeply appreciate all the study participants and hospital staff for their participation and cooperation.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
TW and TT conceived the study. YM acquired the data. YM and TT performed the analyses and drafted the manuscript. All authors contributed to the interpretation of the results and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
None.
Ethics approval
The study protocol was approved by the ethics committee of Kanazawa University (approval number 907). The study was carried out in accordance with the principles of the Declaration of Helsinki.
Consent to participate
The study was announced on the hospital’s website. All participants were given the opportunity to opt out of the study by sending an opt-out document to the hospital if they wished. All analyses were performed using deidentified data.
Consent for publication (include appropriate statements)
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Miyajima, Y., Toyama, T., Mori, M. et al. Relationships between kidney dysfunction and left ventricular diastolic dysfunction: a hospital-based retrospective study. J Nephrol 34, 773–780 (2021). https://doi.org/10.1007/s40620-020-00940-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-020-00940-9