Abstract
Purpose of Review
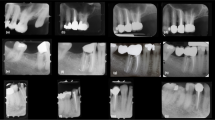
This article reviews recent evidence and provides a general overview on the clinical performance of resin composite restorations. Four electronic databases were searched for articles that investigated factors associated with the long-term performance and failure of resin composites placed in anterior and posterior teeth. Signs that could be observed in aging restorations were also addressed.
Recent Findings
Resin composite restorations fail due to the same reasons that lead to restoration of teeth, namely: caries, esthetics, fractures, and wear. Variables influencing failure rates include tooth-related factors (e.g., loss of dental tissue, quality of remaining structure, tooth position, endodontic treatment) and patient-related risk factors (e.g., caries, parafunctional habits, sex, age, socioeconomic variables). State of the art restorative techniques and materials have limited influence on the durability of resin composite restorations. Dentists and their clinical decisions also play a significant role in longevity, including their approach to aging restorations that are in service. Aging restorations may show surface and marginal staining, loss of anatomical shape and translucency, wear, chipping, fractures, and other minor defects that do not need intervention.
Summary
The clinical service of resin composite restorations is a challenging aspect of their longevity, but posterior and anterior composites can achieve long-lasting clinical durability. Patients’ risks appear to be the most predominant factors affecting longevity. In general, the longevity of restorations would be longer if dentists were to use a more conservative approach when dealing with aging restorations in service.



Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Worthington HV, Khangura S, Seal K, Mierzwinski-Urban M, Veitz-Keenan A, Sahrmann P, et al. Direct composite resin fillings versus amalgam fillings for permanent posterior teeth. Cochrane Database Syst Rev. 2021;8:CD005620. https://doi.org/10.1002/14651858.CD005620.pub3.
Da Rosa Rodolpho PA, Donassollo TA, Cenci MS, Loguércio AD, Moraes RR, Bronkhorst EM, et al. 22-Year clinical evaluation of the performance of two posterior composites with different filler characteristics. Dent Mater. 2011;27:955–63. https://doi.org/10.1016/j.dental.2011.06.001.
Pallesen U, van Dijken J. A randomized controlled 27 years follow up of three resin composites in class II restorations. J Dent. 2015;43:1547–58. https://doi.org/10.1016/j.jdent.2015.09.003.
Pallesen U, van Dijken J. A randomized controlled 30 years follow up of three conventional resin composites in class II restorations. Dent Mater. 2015;31:1232–44. https://doi.org/10.1016/j.dental.2015.08.146.
Laske M, Opdam NJ, Bronkhorst EM, Braspenning JC, Huysmans MC. Longevity of direct restorations in Dutch dental practices. Descriptive study out of a practice based research network. J Dent. 2016;46:12–7. https://doi.org/10.1016/j.jdent.2016.01.002.
•• Collares K, Opdam NJ, Laske M, Bronkhorst EM, Demarco FF, Correa MB, et al. Longevity of anterior composite restorations in a general dental practice-based network. J Dent Res. 2017;96:1092–9. https://doi.org/10.1177/0022034517717681. This study shows a large variation in failure rates of anterior resin composite restorations placed by different operators.
Montag R, Dietz W, Nietzsche S, Lang T, Weich K, Sigusch BW, et al. Clinical and micromorphologic 29-year results of posterior composite restorations. J Dent Res. 2018;97:1431–7. https://doi.org/10.1177/0022034518788798.
Baldissera RA, Corrêa MB, Schuch HS, Collares K, Nascimento GG, Jardim PS, et al. Are there universal restorative composites for anterior and posterior teeth? J Dent. 2013;41:1027–35. https://doi.org/10.1016/j.jdent.2013.08.016.
Burke FJ, Lucarotti PS. The ultimate guide to restoration longevity in England and Wales. Part 4: resin composite restorations: time to next intervention and to extraction of the restored tooth. Br Dent J. 2018;224:945–6. https://doi.org/10.1038/sj.bdj.2018.443.
•• Burke FJ, Lucarotti PS. The ultimate guide to restoration longevity in England and Wales. Part 10: key findings from a ten million restoration dataset. Br Dent J. 2018;225:1011–8. https://doi.org/10.1038/sj.bdj.2018.1029. This study analyzed a large dataset of restorations and reported that the patient treatment history is one of the main factors affecting longevity.
•• Laske M, Opdam NJ, Bronkhorst EM, Braspenning JCC, Huysmans MC. Risk factors for dental restoration survival: a practice-based study. J Dent Res. 2019;98:414–22. https://doi.org/10.1177/0022034519827566. This study observed that a wide range of patient-related variables was related to a high risk for reintervention in resin composite restorations, including patient age, general health, periodontal status, caries risk, and risk for parafunctional habits.
• Demarco FF, Corrêa MB, Cenci MS, Moraes RR, Opdam NJ. Longevity of posterior composite restorations: not only a matter of materials. Dent Mater. 2012;28:87–101. https://doi.org/10.1016/j.dental.2011.09.003. This classic review article explored several factors other than material-related variables that may affect the clinical performance of posterior resin composite restorations.
Laske M, Opdam NJ, Bronkhorst EM, Braspenning JC, Huysmans MC. Ten-year survival of class ii restorations placed by general practitioners. JDR Clin Trans Res. 2016;1:292–9. https://doi.org/10.1177/2380084416663192.
Montagner AF, Sande FHV, Müller C, Cenci MS, Susin AH. Survival, reasons for failure and clinical characteristics of anterior/posterior composites: 8-year findings. Braz Dent J. 2018;29:547–54. https://doi.org/10.1590/0103-6440201802192.
Fan J, Xu Y, Si L, Li X, Fu B, Hannig M. Long-term clinical performance of composite resin or ceramic inlays, onlays, and overlays: a systematic review and meta-analysis. Oper Dent. 2021;46:25–44. https://doi.org/10.2341/19-107-LIT.
Kang SH, Kim BS, Kim Y. Cracked teeth: Distribution, characteristics, and survival after root canal treatment. J Endod. 2016;42:557–62. https://doi.org/10.1016/j.joen.2016.01.014.
Nuamwisudhi P, Jearanaiphaisarn T. Oral functional behaviors and tooth factors associated with cracked teeth in asymptomatic patients. J Endod. 2021;47:1383–90. https://doi.org/10.1016/j.joen.2021.05.012.
Kuper NK, Opdam NJ, Bronkhorst EM, Huysmans MC. The influence of approximal restoration extension on the development of secondary caries. J Dent. 2012;40:241–7. https://doi.org/10.1016/j.jdent.2011.12.014.
Van Meerbeek B, Yoshihara K, Van Landuyt K, Yoshida Y, Peumans M. From Buonocore’s pioneering acid-etch technique to self-adhering restoratives. A status perspective of rapidly advancing dental adhesive technology. J Adhes Dent. 2020;22:7–34. https://doi.org/10.3290/j.jad.a43994.
Linnemann T, Kramer EJ, Schwendicke F, Wolf TG, Meyer-Lueckel H, Wierichs RJ. Longevity and risk factors of post restorations after up to 15 years: a practice-based study. J Endod. 2021;47:577–84. https://doi.org/10.1016/j.joen.2020.10.009.
Ning K, Bronkhorst E, Bremers A, Bronkhorst H, van der Meer W, Yang F, et al. Wear behavior of a microhybrid composite vs. a nanocomposite in the treatment of severe tooth wear patients: a 5-year clinical study. Dent Mater. 2021;37:1819–27. https://doi.org/10.1016/j.dental.2021.09.011.
Lempel E, Lovász BV, Bihari E, Krajczár K, Jeges S, Tóth Á, et al. Long-term clinical evaluation of direct resin composite restorations in vital vs. endodontically treated posterior teeth — retrospective study up to 13 years. Dent Mater. 2019;35:1308–18. https://doi.org/10.1016/j.dental.2019.06.002.
Pontoriero DI, Grandini S, Spagnuolo G, Discepoli N, Benedicenti S, Maccagnola V, et al. Clinical outcomes of endodontic treatments and restorations with and without posts up to 18 years. J Clin Med. 2021;10:908. https://doi.org/10.3390/jcm10050908.
Girotto LP, Dotto L, Pereira GK, Bacchi A, Sarkis-Onofre R. Restorative preferences and choices of dentists and students for restoring endodontically treated teeth: a systematic review of survey studies. J Prosthet Dent. 2021;126:489.e5. https://doi.org/10.1016/j.prosdent.2020.07.005.
Naumann M, Schmitter M, Frankenberger R, Krastl G. “Ferrule comes first. Post is second!” Fake news and alternative facts? A systematic review. J Endod. 2018;44:212–9. https://doi.org/10.1016/j.joen.2017.09.020.
Wierichs RJ, Kramer EJ, Wolf TG, Naumann M, Meyer-Lueckel H. Longevity of composite build-ups without posts—10-year results of a practice-based study. Clin Oral Investig. 2019;23:1435–42. https://doi.org/10.1007/s00784-018-2565-0.
Schwendicke F, Kramer EJ, Krois J, Meyer-Lueckel H, Wierichs RJ. Long-term costs of post-restorations: 7-year practice-based results from Germany. Clin Oral Investig. 2021;25:2175–81. https://doi.org/10.1007/s00784-020-03529-5.
van de Sande FH, Opdam NJ, Rodolpho PA, Correa MB, Demarco FF, Cenci MS. Patient risk factors’ influence on survival of posterior composites. J Dent Res. 2013;92:78S-83S. https://doi.org/10.1177/0022034513484337.
Demarco FF, Collares K, Correa MB, Cenci MS, Moraes RR, Opdam NJ. Should my composite restorations last forever? Why are they failing? Braz Oral Res. 2017;31:e56. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0056.
Collares K, Opdam NJ, Peres KG, Peres MA, Horta BL, Demarco FF, et al. Higher experience of caries and lower income trajectory influence the quality of restorations: a multilevel analysis in a birth cohort. J Dent. 2018;68:79–84. https://doi.org/10.1016/j.jdent.2017.11.009.
• Wierichs RJ, Kramer EJ, Meyer-Lueckel H. Risk factors for failure of direct restorations in general dental practices. J Dent Res. 2020;99:1039–46. https://doi.org/10.1177/0022034520924390. This long-term, multicenter study showed that restorations submitted to more frequent check-ups per year showed higher failure rates than those with fewer check-ups.
Wong C, Blum IR, Louca C, Sparrius M, Wanyonyi K. A retrospective clinical study on the survival of posterior composite restorations in a primary care dental outreach setting over 11 years. J Dent. 2021;106:103586. https://doi.org/10.1016/j.jdent.2021.103586.
Skupien JA, Opdam NJ, Winnen R, Bronkhorst EM, Kreulen CM, Pereira-Cenci T, et al. Survival of restored endodontically treated teeth in relation to periodontal status. Braz Dent J. 2016;27:37–40. https://doi.org/10.1590/0103-6440201600495.
Jukka L, Hannu V, Ellinoora R, Laura J, Ritva N, Vuokko A. The survival time of restorations is shortened in patients with dry mouth. J Dent. 2021;113:103794. https://doi.org/10.1016/j.jdent.2021.103794.
Mehta SB, Bronkhorst EM, Lima VP, Crins L, Bronkhorst H, Opdam NJ, et al. The effect of pre-treatment levels of tooth wear and the applied increase in the vertical dimension of occlusion (VDO) on the survival of direct resin composite restorations. J Dent. 2021;111:103712. https://doi.org/10.1016/j.jdent.2021.103712.
Palmier NR, Madrid Troconis CC, Normando AG, Guerra EN, Araújo AL, Arboleda LP, et al. Impact of head and neck radiotherapy on the longevity of dental adhesive restorations: a systematic review and meta-analysis. J Prosthet Dent. 2021. https://doi.org/10.1016/j.prosdent.2021.02.002.
Nedeljkovic I, De Munck J, Ungureanu AA, Slomka V, Bartic C, Vananroye A, et al. Biofilm-induced changes to the composite surface. J Dent. 2017;63:36–43. https://doi.org/10.1016/j.jdent.2017.05.015.
Nedeljkovic I, Teughels W, De Munck J, Van Meerbeek B, Van Landuyt KL. Is secondary caries with composites a material-based problem? Dent Mater. 2015;31:e247–77. https://doi.org/10.1016/j.dental.2015.09.001.
Moro BL, Freitas RD, Pontes LR, Passaro AL, Lenzi TL, Tedesco TK, et al. Influence of different clinical criteria on the decision to replace restorations in primary teeth. J Dent. 2020;101:103421. https://doi.org/10.1016/j.jdent.2020.103421.
Freitas BN, Pintado-Palomino K, de Almeida CV, Cruvinel PB, Souza-Gabriel AE, Corona SA, et al. Clinical decision-making in anterior resin composite restorations: a multicenter evaluation. J Dent. 2021;113:103757. https://doi.org/10.1016/j.jdent.2021.103757.
Espíndola-Castro LF, Guimarães RP, Souza FB, Monteiro GQ, Menezes Filho PF, Fernandes LO, et al. A 14-year follow-up of resin composite occlusal restorations: split mouth randomised clinical trial and wear evaluation by optical coherence tomography. J Clin Diagnostic Res. 2019;13:ZC10-15. https://doi.org/10.7860/jcdr/2019/37436.12436.
Gurgan S, Koc Vural U, Kutuk ZB, Cakir FY. Does a new formula have an input in the clinical success of posterior composite restorations? A chat study. Clin Oral Investig. 2021;25:1715–27. https://doi.org/10.1007/s00784-020-03472-5.
Tardem C, Albuquerque EG, Lopes LS, Marins SS, Calazans FS, Poubel LA, et al. Clinical time and postoperative sensitivity after use of bulk-fill (syringe and capsule) vs. incremental filling composites: a randomized clinical trial. Braz Oral Res. 2019;33:e089. https://doi.org/10.1590/1807-3107bor-2019.vol33.0089.
Yazici AR, Kutuk ZB, Ergin E, Karahan S, Antonson SA. Six-year clinical evaluation of bulk-fill and nanofill resin composite restorations. Clin Oral Investig. 2021. https://doi.org/10.1007/s00784-021-04015-2.
Schwendicke F, Göstemeyer G, Blunck U, Paris S, Hsu LY, Tu YK. Directly placed restorative materials: review and network meta-analysis. J Dent Res. 2016;95:613–22. https://doi.org/10.1177/0022034516631285.
Dreweck FD, Burey A, de Oliveira DM, Loguercio AD, Reis A. Adhesive strategies in cervical lesions: systematic review and a network meta-analysis of randomized controlled trials. Clin Oral Investig. 2021;25:2495–510. https://doi.org/10.1007/s00784-021-03844-5.
Heintze SD, Ilie N, Hickel R, Reis A, Loguercio A, Rousson V. Laboratory mechanical parameters of composite resins and their relation to fractures and wear in clinical trials-a systematic review. Dent Mater. 2017;33:e101–14. https://doi.org/10.1016/j.dental.2016.11.013.
Opdam NJ, Collares K, Hickel R, Bayne SC, Loomans BA, Cenci MS, et al. Clinical studies in restorative dentistry: new directions and new demands. Dent Mater. 2018;34:1–12. https://doi.org/10.1016/j.dental.2017.08.187.
Crins LA, Opdam NJ, Kreulen CM, Bronkhorst EM, Sterenborg BA, Huysmans MC, et al. Randomized controlled trial on the performance of direct and indirect composite restorations in patients with severe tooth wear. Dent Mater. 2021;37:1645–54. https://doi.org/10.1016/j.dental.2021.08.018.
Heintze SD, Rousson V. Clinical effectiveness of direct class II restorations - a meta-analysis. J Adhes Dent. 2012;14:407–31. https://doi.org/10.3290/j.jad.a28390.
Miao C, Yang X, Wong MC, Zou J, Zhou X, Li C, Wang Y. Rubber dam isolation for restorative treatment in dental patients. Cochrane Database Syst Rev. 2021;5:CD009858. https://doi.org/10.1002/14651858.CD009858.pub3.
da Rosa WL, Lima VP, Moraes RR, Piva E, da Silva AF. Is a calcium hydroxide liner necessary in the treatment of deep caries lesions? A systematic review and meta-analysis. Int Endod J. 2019;52:588–603. https://doi.org/10.1111/iej.13034.
Blum IR, Wilson NH. An end to linings under posterior composites? J Am Dent Assoc. 2018;149:209–13. https://doi.org/10.1016/j.adaj.2017.09.053.
Vetromilla BM, Opdam NJ, Leida FL, Sarkis-Onofre R, Demarco FF, van der Loo MP, et al. Treatment options for large posterior restorations: a systematic review and network meta-analysis. J Am Dent Assoc. 2020;151:614-24.e18. https://doi.org/10.1016/j.adaj.2020.05.006.
Estay J, Martin J, Vildósola P, Villablanca C, Mjör I, de Oliveira Jr OB, et al. Sealing of restorations with marginal defects does not affect their longevity. Am J Dent. 2018;31:107–12.
Fernández E, Vildósola P, Bersezio C, Gordan VV, Mjör IA, Oliveira OB, et al. Does refurbishing composites lead to short-term effects or long-lasting improvement? Am J Dent. 2015;28:203–8.
Frese C, Wohlrab T, Soliman S, Hahn B, Büsch C, Babai A, et al. A multicenter trial on the long-term performance of direct composite buildups in the anterior dentition - survival and quality outcome. J Adhes Dent. 2020;22:573–80. https://doi.org/10.3290/j.jad.a45514.
Estay J, Martín J, Viera V, Valdivieso J, Bersezio C, Vildosola P, et al. 12 Years of repair of amalgam and composite resins: a clinical study. Oper Dent. 2018;43:12–21. https://doi.org/10.2341/16-313-C.
van de Sande FH, Moraes RR, Elias RV, Montagner AF, Rodolpho PA, Demarco FF, et al. Is composite repair suitable for anterior restorations? A long-term practice-based clinical study. Clin Oral Investig. 2019;23:2795–803. https://doi.org/10.1007/s00784-018-2722-5.
Casagrande L, Laske M, Bronkhorst EM, Huysmans MC, Opdam NJ. Repair may increase survival of direct posterior restorations – a practice based study. J Dent. 2017;64:30–6. https://doi.org/10.1016/j.jdent.2017.06.002.
Pontes LR, Lara JS, Novaes TF, Freitas JG, Gimenez T, Moro BL, et al. Negligible therapeutic impact, false-positives, overdiagnosis and lead-time are the reasons why radiographs bring more harm than benefits in the caries diagnosis of preschool children. BMC Oral Health. 2021;21:168. https://doi.org/10.1186/s12903-021-01528-w.
Funding
This study was partially financed by Coordenação de Aperfeiçoamento de Pessoal de Nível Superior — (CAPES), Brazil (Finance Code 001).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Dental Restorative Materials
Rights and permissions
About this article
Cite this article
Moraes, R.R., Cenci, M.S., Moura, J.R. et al. Clinical performance of resin composite restorations. Curr Oral Health Rep 9, 22–31 (2022). https://doi.org/10.1007/s40496-022-00308-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40496-022-00308-x