Abstract
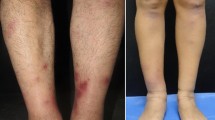
Erythema nodosum (EN) is the most common form of panniculitis. It is characterized by erythematous, raised, tender nodules that usually occur bilaterally on the extensor surfaces of the lower extremities. EN is associated with many underlying conditions including infection, sarcoidosis, malignancy, and pregnancy. Its underlying etiology, however, is unknown in up to half of cases. Pregnancy is thought to create an optimal background for EN to develop, although the exact mechanisms are unclear. Immune complexes may play a role in the pathogenesis of EN during pregnancy, or EN may be a hypersensitivity reaction to either estrogens or progesterone. EN is a self-limiting process, and non-pharmacologic means such as bed rest and elastic web bandages may be sufficient to control the symptoms. Potassium iodide, systemic and intralesional corticosteroids, non-steroidal anti-inflammatory drugs, salicylates, tumor necrosis factor-α inhibitors, hydroxychloroquine, colchicine, and dapsone are other treatment options available, but some of these drugs are contraindicated in pregnancy while others are considered safe. Before prescribing one of these treatments to a pregnant patient, the patient’s obstetrician should be consulted, and a careful risk-benefit analysis should be performed.



Similar content being viewed by others
References
Mana J, Marcoval J. Erythema nodosum. Clin Dermatol. 2007;25(3):288–94.
Brodell RT, Mehrabi D. Underlying causes of erythema nodosum: lesions may provide clue to systemic disease. Postgrad Med. 2000;108(6):147–9.
Hannuksela M. Erythema nodosum. Clin Dermatol. 1986;4(4):88–95.
Bartelsmeyer JA, Petrie RH. Erythema nodosum, estrogens, and pregnancy. Clin Obstet Gynecol. 1990;33(4):777–81.
Fitzpatrick TB, Klaus W. Fitzpatrick’s dermatology in general medicine. New York: McGraw-Hill Medical; 2008.
Requena L, Yus ES. Erythema nodosum. Semin Cutan Med Surg. 2007;26(2):114–25.
Psychos DN, Voulgari PV, Skopouli FN, et al. Erythema nodosum: the underlying conditions. Clin Rheumatol. 2000;19(3):212–6.
Garcia-Porrua C, Gonzalez-Gay MA, Vazquez-Caruncho M, et al. Erythema nodosum: etiologic and predictive factors in a defined population [Erratum appears in Arthritis Rheum 2000;43(5):1061]. Arthritis Rheum. 2000;43(3):584–92.
Cribier B, Caille A, Heid E, et al. Erythema nodosum and associated diseases: a study of 129 cases. Int J Dermatol. 1998;37(9):667–72.
Puavilai S, Sakuntabhai A, Sriprachaya-Anunt S, et al. Etiology of erythema nodosum. J Med Assoc Thail. 1995;78(2):72–5.
Requena L, Yus ES. Panniculitis: part I. Mostly septal panniculitis. J Am Acad Dermatol. 2001;45(2):163–83 (quiz 84–6).
Miescher G. Histologic diagnosis of erythema nodosum. Dermatologica. 1950;101(4–5):255–6.
LeBoit PE. From Sweet to Miescher and back again. Am J Dermatopathol. 2006;28(4):381–3.
Bombardieri S, Munno OD, Di Punzio C, et al. Erythema nodosum associated with pregnancy and oral contraceptives. BMJ. 1977;1(6075):1509–10.
Jelinek JE. Oral contraceptives and the skin. Am Fam Phys. 1971;4(5):68–74.
Gelfand M. Oral contraceptives and erythema nodosum: report of a case. Cent Afr J Med. 1982;28(8):199–201.
Baker H. Adverse cutaneous reaction to oral contraceptives. Br J Dermatol. 1969;81(12):946–9.
Merk H, Ruzicka T. Oral contraceptives as a cause of erythema nodosum. Arch Dermatol. 1981;117(8):454.
Baden HP, Holcomb FD. Erythema nodosum from oral contraceptives. Arch Dermatol. 1968;98(6):634–5.
Papagrigoraki A, Gisondi P, Rosina P, et al. Erythema nodosum: etiological factors and relapses in a retrospective cohort study. Eur J Dermatol. 2010;20(6):773–7.
Jeon HC, Choi M, Paik SH, et al. A case of assisted reproductive therapy-induced erythema nodosum. Ann Dermatol. 2011;23(3):362–4.
Yang SG, Han KH, Cho KH, et al. Development of erythema nodosum in the course of oestrogen replacement therapy. Br J Dermatol. 1997;137(2):319–20.
Jhaveri K, Halperin P, Shin SJ, et al. Erythema nodosum secondary to aromatase inhibitor use in breast cancer patients: case reports and review of the literature. Breast Cancer Res Treat. 2007;106(3):315–8.
Jones JV, Cumming RH, Asplin CM. Evidence for circulating immune complexes in erythema nodosum and early sarcoidosis. Ann N Y Acad Sci. 1976;278:212–9.
Marzi M, Vigano A, Trabattoni D, et al. Characterization of type 1 and type 2 cytokine production profile in physiologic and pathologic human pregnancy. Clin Exp Immunol. 1996;106(1):127–33.
Piccinni MP, Giudizi MG, Biagiotti R, et al. Progesterone favors the development of human T helper cells producing Th2-type cytokines and promotes both IL-4 production and membrane CD30 expression in established Th1 cell clones. J Immunol. 1995;155(1):128–33.
Grimaldi CM, Cleary J, Dagtas AS, et al. Estrogen alters thresholds for B cell apoptosis and activation. J Clin Investig. 2002;109(12):1625–33.
Grimaldi CM, Michael DJ, Diamond B. Cutting edge: expansion and activation of a population of autoreactive marginal zone B cells in a model of estrogen-induced lupus. J Immunol. 2001;167(4):1886–90.
Medina KL, Strasser A, Kincade PW. Estrogen influences the differentiation, proliferation, and survival of early B-lineage precursors. Blood. 2000;95(6):2059–67.
Clemens LE, Siiteri PK, Stites DP. Mechanism of immunosuppression of progesterone on maternal lymphocyte activation during pregnancy. J Immunol. 1979;122(5):1978–85.
Munroe JS. Progesteroids as immunosuppressive agents. J Reticuloendothel Soc. 1971;9(4):361–75.
Mori T, Kobayashi H, Nishimoto H, et al. Inhibitory effect of progesterone and 20 alpha-hydroxypregn-4-en-3-one on the phytohemagglutinin-induced transformation of human lymphocytes. Am J Obstet Gynecol. 1977;127(2):151–7.
Akdis AC, Kilicturgay K, Helvaci S, et al. Immunological evaluation of erythema nodosum in tularaemia. Br J Dermatol. 1993;129(3):275–9.
Ryan T. Cutaneous vasculitis. In: Champion R, Burton J, Burns D, et al., editors. Textbook of dermatology. Oxford: Blackwell; 1998. p. 2155–225.
Wetherill JH. Recurrent erythema nodosum of pregnancy. BMJ. 1971;3(5773):535.
Daw E. Recurrent erythema nodosum of pregnancy. BMJ. 1971;2(5752):44.
Schulz EJ, Whiting DA. Treatment of erythema nodosum and nodular vasculitis with potassium iodide. Br J Dermatol. 1976;94(1):75–8.
Horio T, Imamura S, Danno K, et al. Potassium iodide in the treatment of erythema nodosum and nodular vasculitis. Arch Dermatol. 1981;117(1):29–31.
Marshall JK, Irvine EJ. Successful therapy of refractory erythema nodosum associated with Crohn’s disease using potassium iodide. Can J Gastroenterol. 1997;11(6):501–2.
Cohen S, Benacerraf B, McCluskey RT, et al. Effect of anticoagulants on delayed hypersensitivity reactions. J Immunol. 1967;98(2):351–8.
Honma K, Saga K, Onodera H, et al. Potassium iodide inhibits neutrophil chemotaxis. Acta Dermato-Venereol. 1990;70(3):247–9.
Briggs GGFRK, Yaffe SJ. Drugs in pregnancy and lactation: a reference guide to fetal and neonatal risk. 9th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2011.
Katzung BG, Masters SB, Trevor AJ, et al. Basic and clinical pharmacology. New York: McGraw-Hill Medical; 2012.
Golding D. Treating erythema nodosum. BMJ. 1969;4(5682):560–1.
Ubogy Z, Persellin RH. Suppression of erythema nodosum by indomethacin. Acta Dermato-Venereol. 1982;62(3):265–6.
Mert A, Ozaras R, Tabak F, et al. Erythema nodosum: an experience of 10 years. Scand J Infect Dis. 2004;36(6–7):424–7.
Marpeau L, Bouillie J, Barrat J, et al. Obstetrical advantages and perinatal risks of indomethacin: a report of 818 cases. Fetal Diagn Ther. 1994;9(2):110–5.
Rasanen J, Jouppila P. Fetal cardiac function and ductus arteriosus during indomethacin and sulindac therapy for threatened preterm labor: a randomized study. Am J Obstet Gynecol. 1995;173(1):20–5.
Cunningham FG, Williams JW. Williams obstetrics. New York: McGraw-Hill Medical; 2010.
Imboden JB, Hellmann DB, Stone J. Current diagnosis and treatment in rheumatology. New York: London: McGraw-Hill Medical, 2006.
Buckshee K, Chadha S. Post tonsillitic erythema nodosum in pregnancy. Int J Gynaecol Obstet. 1996;55(3):293–4.
Langer R, Bukovsky I, Lipshitz I, et al. Erythema nodosum associated with pregnancy: case reports. Eur J Obstet Gynecol Reprod Biol. 1979;9(6):399–401.
Goodman LS, Brunton LL, Chabner B, et al. Goodman and Gilman’s the pharmacological basis of therapeutics. New York: McGraw-Hill Medical; 2011.
Mat C, Yurdakul S, Uysal S, et al. A double-blind trial of depot corticosteroids in Behcet’s syndrome. Rheumatology. 2006;45(3):348–52.
Salvatore MA, Lynch PJ. Erythema nodosum, estrogens, and pregnancy. Arch Dermatol. 1980;116(5):557–8.
Coaccioli S, Donati L, Di Cato L, et al. Onset of erythema nodosum during pregnancy: a case report. Clin Exp Obstet Gynecol. 1998;25(1–2):40–1.
Labunski S, Posern G, Ludwig S, et al. Tumour necrosis factor-alpha promoter polymorphism in erythema nodosum. Acta Dermato-Venereol. 2001;81(1):18–21.
Boyd AS. Etanercept treatment of erythema nodosum. Skinmed. 2007;6(4):197–9.
Kugathasan S, Miranda A, Nocton J, et al. Dermatologic manifestations of Crohn disease in children: response to infliximab. J Pediatr Gastroenterol Nutr. 2003;37(2):150–4.
Clayton TH, Walker BP, Stables GI. Treatment of chronic erythema nodosum with infliximab. Clin Exp Dermatol. 2006;31(6):823–4.
Neblett TR, Burnham TK, Kay N. Chloroquine: its mechanism of action upon immune phenomena. Arch Dermatol. 1965;92(6):720–5.
Fox RI. Mechanism of action of hydroxychloroquine as an antirheumatic drug. Semin Arthritis Rheum. 1993;23(2 Suppl 1):82–91.
Alloway JA, Franks LK. Hydroxychloroquine in the treatment of chronic erythema nodosum. Br J Dermatol. 1995;132(4):661–2.
McGready R, Cho T, Keo NK, et al. Artemisinin antimalarials in pregnancy: a prospective treatment study of 539 episodes of multidrug-resistant Plasmodium falciparum. Clin Infect Dis. 2001;33(12):2009–16.
McGready R, Thwai KL, Cho T, et al. The effects of quinine and chloroquine antimalarial treatments in the first trimester of pregnancy. Trans R Soc Trop Med Hyg. 2002;96(2):180–4.
Goodman LS, Brunton LL, Chabner B, et al. Goodman and Gilman’s pharmacological basis of therapeutics. New York: McGraw-Hill; 2011.
Wallace SL. Erythema nodosum treatment with colchicine. JAMA. 1967;202(11):1056.
Yurdakul S, Mat C, Tuzun Y, et al. A double-blind trial of colchicine in Behcet’s syndrome. Arthritis Rheum. 2001;44(11):2686–92.
Brownlie A. Ichthyol and its uses in some skin diseases. The Lancet. 1900;156(4030):1491–2.
Acknowledgments
No sources of funding were received to prepare this article. The authors have no conflicts of interest that are directly relevant to the content of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Acosta, K.A., Haver, M.C. & Kelly, B. Etiology and Therapeutic Management of Erythema Nodosum During Pregnancy: An Update. Am J Clin Dermatol 14, 215–222 (2013). https://doi.org/10.1007/s40257-013-0024-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-013-0024-x