Abstract
Background
The effects of statins in patients with non-valvular atrial fibrillation (NVAF) taking oral anticoagulants (OACs) are not well-studied. This study was a historical multicenter registry of patients with NVAF taking OACs in Japan.
Methods
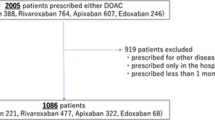
We excluded those patients with mechanical heart valves or a history of pulmonary or deep vein thrombosis. Overall, 7826 patients were registered on 26 February 2013 and followed until 25 February 2017. We compared those with versus without statin treatment (statin vs. no-statin groups) for the primary outcome of major bleeding and secondary outcomes of all-cause mortality, ischemic events, hemorrhagic stroke, and ischemic stroke.
Results
Statins were administered in 2599 (33%) patients. The statin group was more likely to have paroxysmal AF (37% vs. 33%; p = 0.0003), hypertension (84% vs. 76%; p < 0.0001), diabetes mellitus (41% vs. 27%; p < 0.0001), and dyslipidemia (91% vs. 30%; p < 0.0001) than the no-statin group. The cumulative incidence of major bleeding was 6.9% and 8.1% (p = 0.06). The adjusted hazard ratio [HR] (95% confidence interval [CI]) of the statin group for major bleeding was 0.77 (0.63–0.94) compared with the no-statin group. The adjusted HR (95% CI) for all-cause mortality, ischemic events, hemorrhagic stroke, and ischemic stroke were 0.58 (0.47–0.71), 0.77 (0.59–0.999), 0.85 (0.48–1.50), and 0.79 (0.60–1.05), respectively.
Conclusions
Statins significantly reduced the risk of major bleeding, all-cause mortality, and ischemic events in patients with NVAF taking OACs. Their additive benefits should be considered in routine practice and thus be further researched.








Similar content being viewed by others
References
Amarenco P, Bogousslavsky J, Callahan A 3rd, Goldstein LB, Hennerici M, Rudolph AE, et al. High-dose atorvastatin after stroke or transient ischemic attack. N Engl J Med. 2006;355(6):549–59.
Chou R, Dana T, Blazina I, Daeges M, Jeanne TL. Statins for prevention of cardiovascular disease in adults: evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2016;316(19):2008–24.
Ridker PM, Lonn E, Paynter NP, Glynn R, Yusuf S. Primary Prevention with statin therapy in the elderly: new meta-analyses from the contemporary JUPITER and HOPE-3 Randomized Trials. Circulation. 2017;135(20):1979–81.
Di Napoli P, Taccardi AA, Oliver M, De Caterina R. Statins and stroke: evidence for cholesterol-independent effects. Eur Heart J. 2002;23(24):1908–21.
Toyota T, Morimoto T, Yamashita Y, Shiomi H, Kato T, Makiyama T, et al. More-versus less-intensive lipid-lowering therapy. Circ Cardiovasc Qual Outcomes. 2019;12(8): e005460.
Go AS, Hylek EM, Phillips KA, Chang Y, Henault LE, Selby JV, et al. Prevalence of diagnosed atrial fibrillation in adults: national implications for rhythm management and stroke prevention: the AnTicoagulation and Risk Factors in Atrial Fibrillation (ATRIA) Study. JAMA. 2001;285(18):2370–5.
Steffel J, Verhamme P, Potpara TS, Albaladejo P, Antz M, Desteghe L, et al. The 2018 European Heart Rhythm Association Practical Guide on the use of non-vitamin K antagonist oral anticoagulants in patients with atrial fibrillation. Eur Heart J. 2018;39(16):1330–93.
Morimoto T, Uchida K, Sakakibara F, Kinjo N, Ueda S. Effect of concomitant antiplatelet therapy on ischemic and hemorrhagic events in patients taking oral anticoagulants for nonvalvular atrial fibrillation in daily clinical practice. Pharmacoepidemiol Drug Saf. 2021;30(10):1321–31.
Gage BF, Waterman AD, Shannon W, Boechler M, Rich MW, Radford MJ. Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA. 2001;285(22):2864–70.
Pisters R, Lane DA, Nieuwlaat R, de Vos CB, Crijns HJ, Lip GY. A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro Heart Survey. Chest. 2010;138(5):1093–100.
Schulman S, Kearon C. Definition of major bleeding in clinical investigations of antihemostatic medicinal products in non-surgical patients. J Thromb Haemost. 2005;3(4):692–4.
Sacco RL, Kasner SE, Broderick JP, Caplan LR, Connors JJ, Culebras A, et al. An updated definition of stroke for the 21st century: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2013;44(7):2064–89.
Hicks KA, Tcheng JE, Bozkurt B, Chaitman BR, Cutlip DE, Farb A, et al. 2014 ACC/AHA key data elements and definitions for cardiovascular endpoint events in clinical trials: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Data Standards (Writing Committee to Develop Cardiovascular Endpoints Data Standards). J Am Coll Cardiol. 2015;66(4):403–69.
Butzer JF, Cancilla PA, Cornell SH. Computerized axial tomography of intracerebral hematoma. A clinical and neuropathological study. Arch Neurol. 1976;33(3):206–14.
Noguchi K, Ogawa T, Seto H, Inugami A, Hadeishi H, Fujita H, et al. Subacute and chronic subarachnoid hemorrhage: diagnosis with fluid-attenuated inversion-recovery MR imaging. Radiology. 1997;203(1):257–62.
Kumagai N, Nusser JA, Inoue H, Okumura K, Yamashita T, Kubo T, et al. Effect of addition of a statin to warfarin on thromboembolic events in japanese patients with nonvalvular atrial fibrillation and diabetes mellitus. Am J Cardiol. 2017;120(2):230–5.
Violi F, Calvieri C, Ferro D, Pignatelli P. Statins as antithrombotic drugs. Circulation. 2013;127(2):251–7.
Undas A, Brummel-Ziedins KE, Mann KG. Anticoagulant effects of statins and their clinical implications. Thromb Haemost. 2014;111(3):392–400.
Liu X, Guo CY, Ma XJ, Wu CF, Zhang Y, Sun MY, et al. Anti-inflammatory effects of tanshinone IIA on atherosclerostic vessels of ovariectomized ApoE mice are mediated by estrogen receptor activation and through the ERK signaling pathway. Cell Physiol Biochem. 2015;35(5):1744–55.
Huang B, Zhou ZY, Li S, Huang XH, Tang JY, Hoi MPM, et al. Tanshinone I prevents atorvastatin-induced cerebral hemorrhage in zebrafish and stabilizes endothelial cell-cell adhesion by inhibiting VE-cadherin internalization and actin-myosin contractility. Pharmacol Res. 2018;128:389–98.
Wu HH, Chang SH, Lee TH, Tu HT, Liu CH, Chang TY. Concurrent use of statins decreases major bleeding and intracerebral hemorrhage in non-valvular atrial fibrillation patients taking direct oral anticoagulants: a nationwide cohort study. Front Cardiovasc Med. 2022;9: 969259.
Ho BL, Lin YJ, Lin SF, Chou PS, Chen CF, Lin RT, et al. Statins and the risk of bleeding in patients taking dabigatran. Acta Neurol Scand. 2019;139(5):455–61.
Chang SH, Chou IJ, Yeh YH, Chiou MJ, Wen MS, Kuo CT, et al. Association between use of non-vitamin K oral anticoagulants with and without concurrent medications and risk of major bleeding in nonvalvular atrial fibrillation. JAMA. 2017;318(13):1250–9.
Yoshimura S, Sakai N, Uchida K, Yamagami H, Ezura M, Okada Y, et al. Endovascular therapy in ischemic stroke with acute large-vessel occlusion: recovery by endovascular salvage for cerebral ultra-acute embolism Japan Registry 2. J Am Heart Assoc. 2018;7(9):e008796.
Uchida K, Yoshimura S, Imamura H, Ohara N, Sakai N, Tanaka K, et al. Effect of statin administration after onset of acute ischemic stroke with large vessel occlusion: insights from RESCUE-Japan Registry 2. J Am Heart Assoc. 2020;9(23): e017472.
Katsanos AH, Shoamanesh A. Does the magnitude of lipid lowering with statin therapy indicate higher intracranial bleeding risk? Brain. 2022;145(8):2624–5.
Acknowledgments
The authors are indebted to the data managers of the Institute for Clinical Effectiveness (Ms. Makiko Ohtorii, Ms. Ai Sunagawa, Ms. Kaori Yamamoto, Ms. Sachiko Kitamura, Ms. Hirono Saito, and Ms. Saeko Nagano) for managing the data and performing the statistical analyses.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was supported in part by Bristol-Myers Squibb and JSPS KAKENHI (JP21H03176). The funders did not participate in any part of the study from conception to article preparation.
Conflicts of Interest
Kazutaka Uchida reports lecturer’s fees from Daiichi Sankyo. Shinichiro Ueda reports receiving research grants from Bristol-Myers Squibb, Chugai, Kowa, MSD, Pfizer, and Takeda; lecturer’s fee from Boehringer Ingelheim, MSD, and Taiho; and manuscript fees from Kowa. He has also served on an advisory board for Otsuka. Takeshi Morimoto reports lecturer’s fees from AstraZeneca, Bristol-Myers Squibb, Daiichi Sankyo, Japan Lifeline, Kowa, Toray, and Tsumura; manuscript fees from Bristol-Myers Squibb and Kowa; and advisory board fees from Novartis and Teijin. Norito Kinjo, Fumihiro Sakakibara, Mari Nezu, and Hideki Arai have no disclosures to report.
Availability of Data and Material
The data supporting this study’s findings are available from the corresponding author upon reasonable request.
Ethics Approval
The Institutional Review Boards of all 71 participating sites approved the study protocol in accordance with the Ethical Guidelines for Medical and Health Research Involving Human Subjects in Japan Declaration of Helsinki.
Consent
The Institutional Review Boards approved the opt-out method in place of written informed consent.
Author Contributions
TM and SU: Study conception and design; data acquisition and management. KU, TM, FS and NK: Statistical analyses. All authors: Interpretation of the data. KU and TM: Drafting of the manuscript. FS, NK, MN, HA, and SU: Critical revision of the manuscript. All authors: Final approval of the manuscript.
Consent to participate
Written informed consent from each participant was substituted by opt-out method under the approval from the institutional review boards.
Consent for publication
Consent for publication from study participants was not obtained because the opt-out method was used.
Code availability
The code supporting the study findings are available from the corresponding author upon reasonable request.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Uchida, K., Ueda, S., Sakakibara, F. et al. Statins Reduce Bleeding Risk in Patients Taking Oral Anticoagulants for Nonvalvular Atrial Fibrillation: A Retrospective Registry Study. Am J Cardiovasc Drugs 23, 89–99 (2023). https://doi.org/10.1007/s40256-022-00555-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40256-022-00555-4