Abstract
Purpose
We aimed to evaluate HIV-1 compartmentalization between the cerebrospinal fluid (CSF) and plasma and investigate as to which extent HIV-1 strains in CSF differ from those in blood and whether a correlation with either plasma viral load (pVL) or an altered blood–brain barrier (BBB) does exist.
Study design
We retrospectively evaluated paired CSF/blood samples collected from 86 HIV+ patients. HIV-RNA quantification, pol (PR/RT), and V3 sequencing were performed. HIV coreceptor tropism (CRT) was inferred (g2p, false-positive rate 10%, FPR). Data of standard CSF analysis were also reviewed; an altered CSF/plasma albumin ratio signified BBB damage. Neurological abnormalities (NA) were recorded.
Results
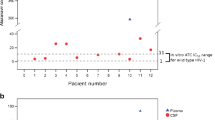
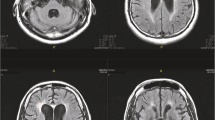
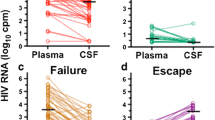
Overall, 32% of patients had a CSF/plasma HIV-RNA ratio > 1 (discordance); 3% of patients had detectable CSF HIV-RNA despite suppressed pVL (escape). Discordance was more frequent in ART-treated patients (p < 0.001) and in patients with NA (p = 0.016), but was independent of BBB damage (p = 0.65) and AIDS diagnosis (p = 0.96). Finally, CSF/plasma discordance was significantly more frequent (p < 0.0001) in patients with lower pVL values (< 10.000 copies/ml). Env divergence > 10% was found in 44% of sequences and was associated with ART (p = 0.008) and NA (p = 0.037). Overall, 24% of patients had a discordant CSF/blood CRT. A 100% nucleotide identity was observed in only 7.3% of pol sequences; notably, 10% of patients had resistance-associated mutations in CSF, but not in blood.
Conclusions
Our data confirm an independent replication and evolution of HIV within the CSF. A number of factors either hinder or contribute to the compartmentalization of HIV.
Similar content being viewed by others
References
Bednar MM, Sturdevant CB, Tompkins LA, et al. Compartmentalization, viral evolution, and viral latency of HIV in the CNS. Curr HIV/AIDS Rep. 2015;12:262–71. https://doi.org/10.1007/s11904-015-0265-9.
Aylin Yilmaz RW, Price. Magnus Gisslen. Antiretroviral drug treatment of CNS HIV-1 infection. J Antimicrob Chemother. 2012;67:299–311. https://doi.org/10.1093/jac/dkr492 (Epub 2011 Dec 8).
Eden A, Fuchs D, Hagberg L, et al. HIV-1 viral escape in cerebrospinal fluid of subjects on suppressive antiretroviral treatment. J Infect Dis 202:1819–1825. https://doi.org/10.1086/657342 (Epub 2010 Nov 4).
Rawson T, Muir D, Mackie NE, Garvey, et al. Factors associated with cerebrospinal fluid HIV RNA in HIV infected subjects undergoing lumbar puncture examination in a clinical setting. J Infect 65:239–245. https://doi.org/10.1016/j.jinf.2012.04.007. (Epub 2012 Apr 17).
Churchill M, Nath A. Where does HIV hide? A focus on the central nervous system. Curr Opin HIV Aids. 2013;8:165–9. https://doi.org/10.1097/COH.0b013e32835fc601.
Di Stefano M, Monno L, Fiore JR, et al. Neurological disorders during HIV-1 infection correlate with viral load in cerebrospinal fluid but not with virus phenotype. AIDS 1998;12:737–43. https://doi.org/10.1097/COH.0b013e32835fc601.
Pillai SK, Pond SL, Liu Y, et al. Genetic attributes of cerebrospinal fluid-derived HIV-1 env. Brain. 2006;129:1872–83. https://doi.org/10.1093/brain/awl136.
Hellmuth J, Valcour V, Spudich S. CNS reservoirs for HIV: implications for eradication. J Vir Erad. 2015;1:67–71.
Schnell G, Price RW, Swanstrom R, et al. Compartmentalization and clonal amplification of HIV-1 variants in the cerebrospinal fluid during primary infection. J Virol. 2010;84:2395–407. https://doi.org/10.1128/JVI.01863-09 (Epub 2009 Dec 16).
Canestri A, Lescure F, Jaureguiberry S, et al. Discordance between cerebral spinal fluid and plasma HIV replication in patients with neurological symptoms who are receiving suppressive antiretroviral therapy. Clin Infect Dis. 2010;50:773–8.
Soulié C, Tubiana R, Simon A, et al. Presence of HIV-1 R5 viruses in cerebrospinal fluid even in patients harboring R5 × 4/X4 viruses in plasma. J Acquir Immune Defic Syndr. 2009;51:60–4.
Soulié C, Fourati S, Lambert-Niclot S, et al. HIV genetic diversity between plasma and cerebrospinal fluid in patients with HIV encephalitis. AIDS. 2010;24:2412–4. https://doi.org/10.1016/S1473-3099(13)70269-X.
Soulie C, Grudé M, Descamps D, et al. Antiretroviral-treated HIV-1 patients can harbour resistant viruses in CSF despite an undetectable viral load in plasma. J Antimicrob Chemother. 2017;72:2351–2354. https://doi.org/10.1093/jac/dkx128.
Monno L, Punzi G, Scarabaggio T, et al. Mutational patterns of paired blood and rectal biopsies in HIVinfected patients on HAART. J Med Virol. 2003;70:1–9.
Monno L, Brindicci G, Saracino A, et al. V3 sequences and paired HIV isolates from 52 non-subtype B HIV type-1 infected patients. AIDS Res Hum Retroviruses. 2010;26:365–72. https://doi.org/10.1089/aid.2009.0224.
Vandekerckhove LP, Wensing AM, Kaiser R, et al. European guidelines on the clinical management of HIV-1 tropism testing. Lancet Infect Dis. 2011 May;11:394–407. https://doi.org/10.1016/S1473-3099(10)70319-4.
Fois AF, Brew BJ. The Potential of the CNS as a Reservoir for HIV-1 Infection: Implications for HIV eradication. Curr HIV/AIDS Rep. 2015;12:299–303. https://doi.org/10.1007/s11904-015-0257-9.
Peluso MJ, Ferretti F, Peterson J, et al. Cerebrospinal fluid HIV escape associated with progressive neurologic dysfunction in patients on antiretroviral therapy with well controlled plasma viral load. AIDS. 2012;26:1765–74. https://doi.org/10.1097/QAD.0b013e328355e6b2.
He J, Chen Y, Farzan M, et al. CCR3 and CCR5 are co-receptors for HIV-1 infection of microglia. Nature. 1997;385:645–9.
Fletcher CV, Staskus K, Wietgrefe SW, et al. Persistent HIV-1 replication is associated with lower antiretroviral drug concentrations in lymphatic tissues. Proc Natl Acad Sci USA. 2014;111:2307–12. https://doi.org/10.1073/pnas.1318249111. (Epub 2014 Jan 27).
Nightingale S, Geretti AM, Beloukas A, et al. Discordant CSF/plasma HIV-1 RNA in patients with unexplained low-level viraemia. J Neurovirol. 2016;22:852–60. https://doi.org/10.1007/s13365-016-0448-1.
Mukerji SS, Misra V, Lorenz D, et al. temporal patterns and drug resistance in CSF viral escape among ART-experienced HIV-1 infected adults. J Acquir Immune Defic Syndr (1999). 2017;75:246–55. https://doi.org/10.1097/QAI.0000000000001362. 2017 (.
Di Carlofelice M, Everit A, Muir D, et al. Cerebrospinal fluid HIV RNA in persons living with HIV. HIV Med. 2018. https://doi.org/10.1111/hiv.12594.
Kugathasan R, Collier DA, Haddow LJ, et al. Diffuse white matter signal abnormalities on magnetic resonance imaging are associated with human immunodeficiency virus type 1 Viral escape in the central nervous system among patients with neurological symptoms. Clin Infect Dis. 2017;64:1059–65. https://doi.org/10.1093/cid/cix035.
Dravid AN, Natrajan K, Kulkarni MM, et al. Discordant CSF/plasma HIV-1 RNA in individuals on virologically suppressive antiretroviral therapy in Western India. Medicine 2018;97:e9969. https://doi.org/10.1097/MD.0000000000009969.
Acknowledgements
The authors would like to thank all patients who participated in the study. The authors also wish to thank Mrs Paulene Butts for her assistance in manuscript preparation.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No authors have any conflict of interest to declare.
Ethical approval
The research did not require approval from the ethics committee according to the Italian law since it was performed as an observational retrospective study in the context of normal clinical routines.
Rights and permissions
About this article
Cite this article
Bavaro, D.F., Calamo, A., Lepore, L. et al. Cerebrospinal fluid compartmentalization of HIV-1 and correlation with plasma viral load and blood–brain barrier damage. Infection 47, 441–446 (2019). https://doi.org/10.1007/s15010-019-01268-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-019-01268-8