Abstract
Purpose
The study compared the mechanical behavior of bioresorbable polymeric stents with various designs during deployment, and investigated their fatigue performance under pulsatile blood pressure loading.
Methods
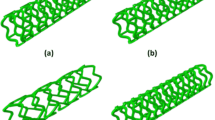
Finite element simulations have been carried out to compare the mechanical performance of four bioresorbable polymeric stents, i.e., Absorb, Elixir, Igaki-Tamai and RevaMedical, during deployment in diseased artery. Tri-folded balloon was modelled to expand the crimped stent onto the three-layered arterial wall with plaque. Cyclic diastolic-systolic pressure loading was applied to both stent and arterial wall to study fatigue behavior.
Results
Stents with larger U-bend and longer axial strut demonstrate more flexibility but suffer from severe dogboning and recoiling effects. Stress concentrations in the stent, as well as in the plaque and artery, are higher for stents designed with increased rigidity such as those with smaller U-bends and shorter axial struts. Simulations of fatigue deformation for Elixir stent demonstrate that the U-bends, with high stress concentrations, have a potential risk of fatigue failure under pulsatile systolic-diastolic blood pressure as opposed to the counter metallic stents which are normally free of fatigue failure.
Conclusion
The structural behaviour of bioresorbable polymeric stent is strongly affected by its design, in terms of expansion, dogboning, recoiling and stress distribution during the deployment process.

















Similar content being viewed by others
References
Ang, H. Y., H. Bulluck, P. Wong, S. S. Venkatraman, Y. Huang, and N. Foin. Bioresorbable stents: current and upcoming bioresorbable technologies. Int. J. Cardiol. 228:931–939, 2016.
Averett, R. D. Experimental aspects and mechanical modeling paradigms for the prediction of degradation and failure in nanocomposite materials subjected to fatigue loading conditions. Dissertations & Thesis-Gradworks, 2008.
Azaouzi, M., A. Makradi, and S. Belouettar. Fatigue life prediction of cardiovascular stent using finite element method. Comput. Methods Biomech. Biomed. Eng. 15(1):93–95, 2012.
Bandar, A. M., M. Rosaire, and Y. Stephen. Coronary stents fracture: an engineering approach (review). Mater. Sci. Appl. 4(10):606–621, 2013.
Bedoya, J., C. A. Meyer, L. H. Timmins, M. R. Moreno, and J. E. Moore. Effects of stent design parameters on normal artery wall mechanics. J. Biomech. Eng. 128(5):757–765, 2006.
Bobel, A. C., and P. E. Mchugh. Computational analysis of the utilisation of the shape memory effect and balloon expansion in fully polymeric stent deployment. Cardiovasc. Eng. Technol. 9(1):1–13, 2017.
Bobel, A. C., S. Petisco, J. R. Sarasua, W. Wang, and P. E. Mchugh. Computational bench testing to evaluate the short-term mechanical performance of a polymeric stent. Cardiovasc. Eng. Technol. 6(4):519–532, 2015.
Debusschere, N., P. Segers, P. Dubruel, B. Verhegghe, and M. De Beule. A finite element strategy to investigate the free expansion behaviour of a biodegradable polymeric stent. J. Biomech. 48(10):2012–2018, 2015.
Dordoni, E., L. Petrini, W. Wu, F. Migliavacca, G. Dubini, and G. Pennati. Computational modeling to predict fatigue behavior of NiTi stents: what do we need? J. Funct. Biomater. 6(2):299–317, 2015.
Dreher, M. L., S. Nagaraja, and B. Batchelor. Effects of fatigue on the chemical and mechanical degradation of model stent sub-units. J. Mech. Behav. Biomed. Mater. 59:139–145, 2016.
Gajjar, C. R., and M. W. King. Degradation process. In: Resorbable Fiber-Forming Polymers for Biotextile Applications. Springer Briefs in Materials, Berlin: Springer, 2014, pp. 7–10.
Gao, R. TCT-310 four-year clinical outcomes from randomized comparison of everolimus-eluting bioresorbable vascular scaffolds versus everolimus-eluting metallic stents in patients with coronary artery disease from ABSORB China Trial. J. Am. Coll. Cardiol. 72(13):B128, 2018.
Gao, R., Y. Yang, Y. Han, Y. Huo, J. Chen, B. Yu, X. Su, L. Li, H. C. Kuo, S. W. Ying, W. F. Cheong, Y. L. Zhang, X. L. Su, B. Xu, J. J. Popma, and G. W. Stone. Bioresorbable vascular scaffolds versus metallic stents in patients with coronary artery disease: absorb China trial. J. Am. Coll. Cardiol. 66(21):2298–2309, 2015.
Gasser, T. C., R. W. Ogden, and G. A. Holzapfel. Hyperelastic modelling of arterial layers with distributed collagen fibre orientations. J. R. Soc. Interface 3(6):15–35, 2006.
Gee, M. W., C. H. Förster, and W. A. Wall. A computational strategy for prestressing patient specific biomechanical problems under finite deformation. Int. J. Numer. Methods Biomed. Eng. 26:52–72, 2010.
Holzapfel, G. A., T. C. Gasser, and R. W. Ogden. A new constitutive framework for arterial wall mechanics and a comparative study of material models. J. Elasticity 61:1–48, 2000.
Holzapfel, G. A., and R. W. Ogden. On the tension–compression switch in soft fibrous solids. Eur. J. Mech. A 49(49):561–569, 2015.
Holzapfel, G. A., G. Sommer, C. T. Gasser, and P. Regitnig. Determination of layer-specific mechanical properties of human coronary arteries with nonatherosclerotic intimal thickening and related constitutive modeling. Am. J. Physiol. Heart Circ. Physiol. 289(5):H2048–H2058, 2005.
Kereiakes, D., S. Ellis, and G. Stone. TCT-61 Clinical outcomes following complete bioresorption of the Absorb everolimus-eluting bioresorbable scaffold: four-year results from the ABSORB III trial. J. Am. Coll. Cardiol. 72(13):B27, 2018.
Kimura, T., K. Kozuma, K. Tanabe, S. Nakamura, M. Yamane, T. Muramatsu, S. Saito, J. Yajima, N. Hagiwara, K. Mitsudo, J. J. Popma, P. W. Serruys, S. H. Ying, S. Cao, P. Staehr, W. F. Cheong, H. Kusano, and G. W. Stone. A randomized trial evaluating everolimus-eluting absorb bioresorbable scaffolds vs. everolimus-eluting metallic stents in patients with coronary artery disease: absorb Japan. Eur. Heart J. 36(47):3332–3342, 2015.
Lee, S. H., J. S. Park, D. G. Shin, Y. J. Kim, G. R. Hong, W. Kim, and B. S. Shim. Frequency of stent fracture as a cause of coronary restenosis after sirolimus-eluting stent implantation. Am. J. Cardiol. 100(4):627–630, 2007.
Li, J., Q. Luo, Z. Xie, Y. Li, and Y. Zeng. Fatigue life analysis and experimental verification of coronary stent. Heart Vessels 25(4):333–337, 2010.
Li, K. W., R. W. Ogden, and G. A. Holzapfel. Computational method for excluding fibers under compression in modeling soft fibrous solids. Eur. J. Mech. A 57:178–193, 2016.
Li, K. W., R. W. Ogden, and G. A. Holzapfel. A discrete fibre dispersion method for excluding fibres under compression in the modelling of fibrous tissues. J. R. Soc. Interface 15(138):20170766, 2018.
Loree, H. M., A. J. Grodzinsky, S. Y. Park, L. J. Gibson, and R. T. Lee. Static circumferential tangential modulus of human atherosclerotic tissue. J. Biomech. 27(2):195–204, 1994.
Migliavacca, F., L. Petrini, V. Montanari, I. Quagliana, F. Auricchio, and G. Dubini. A predictive study of the mechanical behaviour of coronary stents by computer modelling. Med. Eng. Phys. 27(1):13–18, 2005.
Nakazawa, G., A. V. Finn, M. Vorpahl, E. Ladich, R. Kutys, I. Balazs, F. D. Kolodgie, and R. Virmani. Incidence and predictors of drug-eluting stent fracture in human coronary artery: a pathologic analysis. J. Am. Coll. Cardiol. 54(21):1924–1931, 2009.
Ogden, R. W. Large deformation isotropic elasticity-on the correlation of theory and experiment for incompressible rubberlike solids. Proc. R. Soc. Lond. A 326(1567):565–584, 1972.
Osswald, T. A. Understanding Polymer Processing: Processes and Governing Equations. Munich: Carl Hanser Verlag, 2015.
Pauck, R. G., and B. D. Reddy. Computational analysis of the radial mechanical performance of PLLA coronary artery stents. Med. Eng. Phys. 37(1):7–12, 2015.
Pierce, D. M., T. E. Fastl, B. Rodriguez-Vila, P. Verbrugghe, I. Fourneau, G. Maleux, P. Herijgers, J. Enrique, and G. A. Holzapfel. A method for incorporating three-dimensional residual stretches/stresses into patient-specific finite element simulations of arteries. J. Mech. Behav. Biomed. Mater. 47:147–164, 2015.
Schiavone, A., C. Abunassar, S. Hossainy, and L. G. Zhao. Computational analysis of mechanical stress–strain interaction of a bioresorbable scaffold with blood vessel. J. Biomech. 49(13):2677–2683, 2016.
Schiavone, A., T. Qiu, and L. G. Zhao. Crimping and deployment of metallic and polymeric stents-finite element modelling. Vessel Plus 1(1):12–21, 2017.
Schiavone, A., and L. G. Zhao. A computational study of stent performance by considering vessel anisotropy and residual stresses. Mater. Sci. Eng. C 62:307–316, 2016.
Schiavone, A., L. G. Zhao, and A. A. Abdel-Wahab. Effects of material, coating, design and plaque composition on stent deployment inside a stenotic artery—finite element simulation. Mater. Sci. Eng. C 42:479–488, 2014.
Shaikh, F., R. Maddikunta, M. Djelmami-Hani, J. Solis, S. Allaqaband, and T. Bajwa. Stent fracture, an incidental finding or a significant marker of clinical in-stent restenosis? Catheter. Cardiovasc. Interv. 71(5):614–618, 2008.
Testa, L., A. Latib, R. A. Montone, A. Colombo, and F. Bedogni. Coronary bioresorbable vascular scaffold use in the treatment of coronary artery disease. Circ. Cardiovasc. Interv. 9(7):e3978, 2016.
Timmins, L. H., C. A. Meyer, M. R. Moreno, and J. E. Moore, Jr. Mechanical modeling of stents deployed in tapered arteries. Ann. Biomed. Eng. 36(12):2042–2050, 2008.
Vasava, P., P. Jalali, M. Dabagh, and P. J. Kolari. Finite element modelling of pulsatile blood flow in idealized model of human aortic arch: study of hypotension and hypertension. Comput. Math. Methods Med. 20(1):861837, 2012.
Weisbecker, H., D. M. Pierce, and G. A. Holzapfel. A generalized prestressing algorithm for finite element simulations of preloaded geometries with application to the aorta. Int. J. Numer. Methods Biomed. Eng. 30:857–872, 2014.
Xu, B., Y. Yang, Y. Han, Y. Huo, L. Wang, X. Qi, J. Li, Y. Chen, H. Kuo, S. Ying, W. Cheong, Y. Zhang, X. Su, J. Popma, R. Gao, and G. W. Stone. Comparison of everolimus-eluting bioresorbable vascular scaffolds and metallic stents: three-year clinical outcomes from the ABSORB China randomised trial. Eurointervention. 14(5):554–561, 2018.
Yamaji, K., Y. Ueki, G. Souteyrand, J. Daemen, J. Wiebe, H. Nef, T. Adriaenssens, J. P. Loh, B. Lattuca, J. J. Wykrzykowska, J. Gomez-Lara, L. Timmers, P. Motreff, P. Hoppmann, M. Abdel-Wahab, R. A. Byrne, F. Meincke, N. Boeder, B. Honton, C. J. O’Sullivan, A. Ielasi, N. Delarche, G. Christ, J. K. T. Lee, M. Lee, N. Amabile, A. Karagiannis, S. Windecker, and L. Räber. Mechanisms of very late bioresorbable scaffold thrombosis: the INVEST Registry. J. Am. Coll. Cardiol. 70(19):2330–2344, 2017.
Yamaji, K., Y. Ueki, G. Souteyrand, J. Daemen, J. Wiebe, H. Nef, T. Adriaenssens, J. P. Loh, B. Lattuca, J. J. Wykrzykowska, J. Josep, L. Timmers, P. Motreff, P. Hoppmann, M. Abdel-Wahab, R. A. Byrne, F. Meincke, N. Boeder, B. Honton, C. J. O’Sullivan, A. Ielasi, N. Delarche, G. Christ, J. K. T. Lee, M. Lee, N. Amabile, A. Karagiannis, S. Windecker, and L. Räber. Mechanisms of very late bioresorbable scaffold thrombosis—the INVEST registry. J. Am. Coll. Cardiol. 70:2331–2344, 2017.
Acknowledgments
LGZ acknowledge the support from the British Heart Foundation (Grant Number: FS/15/21/31424; Title: Towards controlling the mechanical performance of polymeric bioresorbable vascular scaffold during biodegradation) and the Royal Society of UK (Grant Number: IE160066; Title: Evaluating the Performance of Additively Manufactured Endovascular Scaffolds).
Conflict of interest
Authors T. Y. Qiu, L. G. Zhao and M. Song declare that they have no conflicts of interest to this work.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human participants or animals performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Dr. Ajit P. Yoganathan and Dr. Hwa Liang Leo oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Qiu, T.Y., Zhao, L.G. & Song, M. A Computational Study of Mechanical Performance of Bioresorbable Polymeric Stents with Design Variations. Cardiovasc Eng Tech 10, 46–60 (2019). https://doi.org/10.1007/s13239-018-00397-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-018-00397-9