Abstract
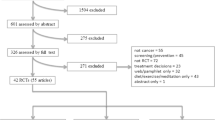
This study aims to describe the acceptability and feasibility of an educational and training experiential intervention (ETEI) we developed to enhance muscle invasive bladder cancer (MIBC) patients with treatment decision-making and post-operative self-care. Twenty-five patients were randomized to a control group (N = 8) or ETEI group (N = 17). ETEI group participated in a nurse-led session on MIBC education. The control group received diet and nutrition education. Study questionnaires were completed at baseline and at 1-month post-intervention. Our results showed acceptable recruitment (58%) and retention rates (68%). The ETEI group reported increased knowledge (82% vs. 50%), improved decisional support (64% vs. 50%), improved communication (73% vs. 50%), and increased confidence in treatment decisions (73% vs. 50%) compared to the control group. Patients in the control group reported improved diet (50% v. 27%) as well as maintaining a healthy lifestyle (67% vs. 45%) compared to the ETEI group. Patients in the ETEI group reported a significant decrease in cancer worries and increases in self-efficacy beliefs over time compared to the control group. The ETEI was feasible, acceptable, and showed a potential for inducing desired changes in cancer worries and efficacy beliefs.
Similar content being viewed by others
References
National Cancer Institute (n.d.). S39.Schwarzer R, Jerusalem M. Generalized Self-Efficacy scale. In J. Weinman, S. Wright, & M. Johnston, Measures in health psychology: A user’s portfolio. Causal and control beliefs. Windor: NFER:NELSON. 1995, 35-37.EER Stat Fact Sheets: bladder cancer. http://seer.cancer.gov/statfacts/html/urinb.html. Accessed July 2018
Bosetti C, Bertuccio P, Chatenoud L, Negri E, La Vecchia C, Levi F (2011) Trends in mortality from urologic cancers in Europe, 1970–2008. Eur Urol 60:1–15
Edwards BK, Ward E, Kohler BA, Eheman C, Zauber AG, Anderson RN, Jemal A, Schymura MJ, Lansdorp-Vogelaar I, Seeff LC, van Ballegooijen M, Goede SL, Ries LAG (2010) Annual report to the nation on the status of cancer, 1975-2006, featuring colorectal cancer trends and impact of interventions (risk factors, screening, and treatment) to reduce future rates. Cancer. 116:544–573
Ferlay J, Randi G, Bosetti C, Levi F, Negri E, Boyle P et al (2008) Declining mortality from bladder cancer in Europe. BJU Int 101:11–19
Thun MJ, Linet MS, Cerhan JR, Haiman C, Schottenfeld D (2006) Cancer epidemiology and prevention, fourth edition. Oxford University Press. https://doi.org/10.1093/oso/9780190238667.001.0001
Burger M, Catto JW, Dalbagni G, Grossman HB, Herr H, Karakiewicz P et al (2013) Epidemiology and risk factors of urothelial bladder cancer. Eur Urol 63:234–241
Babjuk M, Oosterlinck W, Sylvester R, Kaasinen E, Böhle A, Palou-Redorta J, Rouprêt M (2011) EAU guidelines on non–muscle-invasive urothelial carcinoma of the bladder, the 2011 update. Eur Urol 59:997–1008
Stenzl A, Cowan NC, De Santis M, Kuczyk MA, Merseburger AS, Ribal MJ et al (2011) Treatment of muscle-invasive and metastatic bladder cancer: update of the EAU guidelines. Eur Urol 59:1009–1018
Clark PE (2002) Urinary diversion after radical cystectomy. Curr Treat Options in Oncol 3:389–402
Hardt J, Filipas D, Hohenfellner R, Egle UT (2000) Quality of life in patients with bladder carcinoma after cystectomy: first results of a prospective study. Qual Life Res 9:1–12
Krupski T, Theodorescu D (2001) Orthotopic neobladder following cystectomy: indications, management, and outcomes. Journal of Wound Ostomy & Continence Nursing 28:37–46
Stein JP, Lieskovsky G, Cote R, Groshen S, Feng A-C, Boyd S, Skinner E, Bochner B, Thangathurai D, Mikhail M, Raghavan D, Skinner DG (2001) Radical cystectomy in the treatment of invasive bladder cancer: long-term results in 1,054 patients. J Clin Oncol 19:666–675
Studer U, Danuser H, Hochreiter W, Springer J, Turner W, Zingg E (1996) Summary of 10 years’ experience with an ileal low-pressure bladder substitute combined with an afferent tubular isoperistaltic segment. World J Urol 14:29–39
Grossman HB, Natale RB, Tangen CM, Speights V, Vogelzang NJ, Trump DL et al (2003) Neoadjuvant chemotherapy plus cystectomy compared with cystectomy alone for locally advanced bladder cancer. N Engl J Med 349:859–866
Konety BR, Allareddy V, Herr H (2006) Complications after radical cystectomy: analysis of population-based data. Urology. 68:58–64
Kim SP, Boorjian SA, Shah ND, Karnes RJ, Weight CJ, Moriarty JP, Tollefson MK, Shippee ND, Frank I (2012) Contemporary trends of in-hospital complications and mortality for radical cystectomy. BJU Int 110:1163–1168
Turner WH, Studer UE (1997) Cystectomy and urinary diversion. Semin Surg Oncol 13(5):350–358
Mohamed NE, Herrera PC, Hudson S, Revenson TA, Lee CT, Quale DZ et al (2014) Muscle invasive bladder cancer: examining survivor burden and unmet needs. J Urol 191:48–53
Miller SM, Diefenbach MA (1998) C-SHIP: a cognitive-social health information processing approach to cancer. In: Krantz D (ed) Perspectives in behavioral medicine. Lawrence Erlbaum, NJ, pp 219–244
Mohamed NE, Pisipati S, Cassara M, Goodman S, Lee CT, Knauer CJ, Mehrazin R, Sfakianos JP, Given B, Quale DZ, Hall S (2017) Patients’ evaluation of an educational and training experiential intervention (ETEI) to enhance treatment decision and self-care following the diagnosis of muscle invasive bladder cancer. JOJ Urology & Nephrology 4(2):555638
Okada Y, Oishi K, Shichiri Y, Kakehi Y, Hamaguchi A, Tomoyoshi T, Yoshida O (1997) Quality of life survey of urinary diversion patients: comparison of continent urinary diversion versus ileal conduit. Int J Urol 4(1):26–31
Asgari M, Safarinejad M, Shakhssalim N, Soleimani M, Shahabi A, Amini E (2013) Sexual function after non-nerve-sparing radical cystoprostatectomy: a comparison between ileal conduit urinary diversion and orthotopic ileal neobladder substitution. International braz j urol 39:474–483
Mohamed NE, Chaoprang Herrera P, Hall S, Diefenbach MA (2013) An educational intervention for patients with invasive bladder cancer. Society of Behavioral Medicine, San Francisco
Rammant E, Bultijnck R, Sundahl N, Ost P, Pauwels NS, Deforche B, Pieters R, Decaestecker K, Fonteyne V (2017) Rehabilitation interventions to improve patient-reported outcomes and physical fitness in survivors of muscle invasive bladder cancer: a systematic review protocol. BMJ Open 7(5):e016054
D’errico GM, Galassi JP, Schanberg R, Ware WB (2000) Development and validation of the Cancer Worries Inventory. J Psychosoc Oncol 17(3–4):119–137. https://doi.org/10.1300/J077v17n03_07
Légaré F1, Ratté S, Stacey D, Kryworuchko J, Gravel K, Graham ID, Turcotte S (2010) Interventions for improving the adoption of shared decision making by healthcare professionals. Cochrane Database Syst Rev (5):12, CD006732
Shariat SF, Sfakianos JP, Droller MJ, Karakiewicz PI, Meryn S, Bochner BH (2010) The effect of age and gender on bladder cancer: a critical review of the literature. BJU Int 105:300–308
Change Foundation (2005) Consumers and Canadian health care trending analysis 2004. The Change Foundation in partnership with IBM Business Consulting 2005:27
Berry DL, Nayak M, Halpenny B, Harrington S, Loughlin KR, Chang P, Rosenberg JE, Kibel AS (2015) Treatment decision making in patients with bladder cancer. Bladder Cancer 1(2):151–158
Wright JL, Porter MP (2007) Quality-of-life assessment in patients with bladder cancer. Nat Clin Pract Urol 4(3):147–154
Leon AC, Davis LL, Kraemer HC (2011) The role and interpretation of pilot studies in clinical research. J Psychiatr Res 45(5):626–629
Leventhal H, Diefenbach MA, Leventhal EA (1992) Illness cognition: using common sense to understand treatment adherence and affect cognition interactions. Cogn Ther Res 16:143–163
Ottawa Health Research Institute (n.d.) Ottawa decision support framework: update, gaps and research priorities. http://decisionaid.ohri.ca/odsf.html. Accessed August 2018
Mohamed NE, Pisipati S, Lee CT, Goltz HH, Latini DM, Gilbert FS et al (2016) Unmet informational and supportive care needs of patients following cystectomy for bladder cancer based on age, sex, and treatment choices. Urologic Oncology 34(12):7–14
Bloch A, Cassileth BR, Holmes MD, Thomson CA (2004) Eating well, staying well during and after cancer. American Cancer Society, Atlanta
Nutrition in cancer care—patient version. https://www.cancer.gov/about-cancer/treatment/side-effects/appetite-loss/nutrition-pdq. Accessed March 2019
Rock CL, Doyle C, Demark-Wahnefried W et al (2012) Nutrition and physical activity guidelines for cancer survivors. CA Cancer J Clin 62(4):242–274
O’Connor AM (1995) Validation of a Decisional Conflict Scale. Med Decis Mak 15(1):25–30
Cella DF, Tulsky DS, Gray G, Sarafian B, Linn E, Bonomi A, Silberman M, Yellen SB, Winicour P, Brannon J (1993) The functional assessment of cancer-therapy scale—development and validation of the general measure. J Clin Oncol 11:570–579
Schwarzer R, Jerusalem M (1995) Generalized self-efficacy scale. In: J Weinman, S Wright, M Johnston (eds) Measures in health psychology: A user’s portfolio. Causal and control beliefs. Windor: NFER:NELSON. 35–37
Radloff LS (1977) The CES-D Scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1(3):385–401
Osborn RL, Demoncada AC, Feuerstein M (2006) Psychosocial interventions for depression, anxiety, and quality of life in cancer survivors: meta-analyses. Int J Psych Med 36:13–34
Hart SL, Hoyt MA, Diefenbach M, Anderson DR, Kilbourn KM, Craft LL, Steel JL, Cuijpers P, Mohr DC, Berendsen M, Spring B, Stanton AL (2012) Meta-analysis of efficacy of interventions for elevated depressive symptoms in adults diagnosed with cancer. J Natl Cancer Inst 104(13):990–1004
US Preventive Services Task Force (2008) Screening for prostate cancer: US preventive services task force recommendation statement. Ann Intern Med 149:185–191
Sheridan SL, Griffith JM, Behrend L, Gizlice Z, Cai J, Pignone MP (2010) Effect of adding a values clarification exercise to a decision aid on heart disease prevention: a randomized trial. Med Decis Mak 30(4):E28–E39. https://doi.org/10.1177/0272989X10369008
Fitch MI, Miller D, Sharir S, McAndrew A (2010) Radical cystectomy for bladder cancer: a qualitative study of patient experiences and implications for practice. Can Oncol Nurs J 20(4):177–187
Perlis N, Krahn M, Alibhai S, Finelli A, Ritvo P, Bremner KE, Kulkarni G (2014 Oct) Conceptualizing global health-related quality of life in bladder cancer. Qual Life Res 23(8):2153–2167
Acknowledgements
We would like to thank Mr. Holden Kata for his help in the editing of this manuscript. We would also like to show our gratitude to the participants in this study and the BCAN Survivorship Working Group in providing input on the original version of the intervention materials.
Funding
This study is supported by mentored research scholar grants from the American Cancer Society (121193-MRSG-11-103-01-CPPB) and the National Cancer Institute (1R03CA165768-01A1).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by the Mount Sinai Health System (MSHS) Research Ethics Service. All study protocols (i.e., both qualitative and quantitative study methods) were reviewed and approved by the Institutional Review Board at the Icahn School of Medicine at Mount Sinai.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mohamed, N., Leung, T.M., Shah, Q.N. et al. Involving Patients in the Development and Evaluation of an Educational and Training Experiential Intervention (ETEI) to Improve Muscle Invasive Bladder Cancer Treatment Decision-making and Post-operative Self-care: a Mixed Methods Approach. J Canc Educ 35, 808–818 (2020). https://doi.org/10.1007/s13187-019-01534-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-019-01534-1