Abstract
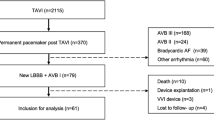
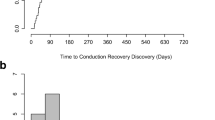
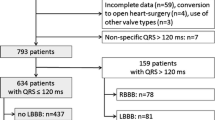
Data on the accurate onset date and serial changes of the complete atrioventricular block (CAVB) after transcatheter aortic valve implantation (TAVI) are limited. This study aimed to assess the incidence, timing, and potential recovery of CAVB following TAVI. Total 696 patients who underwent TAVI were enrolled. Acute CAVB was evaluated within 24 h; delayed CAVB was evaluated 24 h after TAVI. Recovered CAVB was defined as ventricular pacing < 1% during the follow-up or transit block without the need for permanent pacemaker implantation (PMI). The other patients with CAVB were categorized as continued CAVB. Clinical differences between the recovered and continued CAVB groups were evaluated, and the predictive factors of continued CAVB were assessed. The incidence rates of CAVB, acute CAVB, and delayed CAVB were 6.9% (48/696), 4.6% (32/696), and 2.3% (16/696), respectively. Overall, 47.9% (23/48) of patients had recovered CAVB, which was more prevalent in the acute CAVB group than in the delayed CAVB group [59.4% (19/32) vs. 25.0% (4/16), p = 0.025]. CAVB recovery occurred within 24 h (61.0%, 14/23) and after 24 h (39.0%, 9/23). Before CAVB recovery, 21.7% (5/23) of patients had already undergone PMI. A pre-existing complete right bundle branch block (CRBBB) was the only independent predictive factor of continued CAVB (odds ratio 4.51, 95% confidence interval 1.03–19.6, p = 0.045). In conclusion, a pre-existing CRBBB and the timing and prolonged duration of CAVB may be used in risk stratification to determine the appropriateness of early discharge, optimal PMI date, and PMI indication.



Similar content being viewed by others
References
Smith CR, Leon MB, Mack MJ, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Williams M, Dewey T, Kapadia S, Babaliaros V, Thourani VH, Corso P, Pichard AD, Bavaria JE, Herrmann HC, Akin JJ, Anderson WN, Wang D, Pocock SJ, PARTNER Trial Investigators. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med. 2011;364:2187–98.
Adams DH, Popma JJ, Reardon MJ, Yakubov SJ, Coselli JS, Deeb GM, Gleason TG, Buchbinder M, Hermiller J Jr, Kleiman NS, Chetcuti S, Heiser J, Merhi W, Zorn G, Tadros P, Robinson N, Petrossian G, Hughes GC, Harrison JK, Conte J, Maini B, Mumtaz M, Chenoweth S, Oh JK, US CoreValve Clinical Investigators. Transcatheter aortic-valve replacement with a self-expanding prosthesis. N Engl J Med. 2014;370:1790–8.
Buellesfeld L, Stortecky S, Heg D, Hausen S, Mueller R, Wenaweser P, Pilgrim T, Gloekler S, Khattab AA, Huber C, Carrel T, Eberle B, Meier B, Boekstegers P, Jüni P, Gerckens U, Grube E, Windecker S. Impact of permanent pacemaker implantation on clinical outcome among patients undergoing transcatheter aortic valve implantation. J Am Coll Cardiol. 2012;60:493–501.
Ledwoch J, Franke J, Gerckens U, Kuck KH, Linke A, Nickenig G, Krülls-Münch J, Vöhringer M, Hambrecht R, Erbel R, Richardt G, Horack M, Zahn R, Senges J, Sievert H, German Transcatheter Aortic Valve Interventions Registry Investigators. Incidence and predictors of permanent pacemaker implantation following transcatheter aortic valve implantation: analysis from the German transcatheter aortic valve interventions registry. Catheter Cardiovasc Interv. 2013;82:569–77.
Gensas CS, Caixeta A, Siqueira D, Carvalho LA, Sarmento-Leite R, Mangione JA, Lemos PA, Colafranceschi AS, Caramori P, Ferreira MC, Abizaid A, Brito FS Jr, Brazilian Registry in Transcatheter Aortic Valve Implantation Investigators. Predictors of permanent pacemaker requirement after transcatheter aortic valve implantation: insights from a Brazilian registry. Int J Cardiol. 2014;175:248–52.
Nazif TM, Dizon JM, Hahn RT, Xu K, Babaliaros V, Douglas PS, El-Chami MF, Herrmann HC, Mack M, Makkar RR, Miller DC, Pichard A, Tuzcu EM, Szeto WY, Webb JG, Moses JW, Smith CR, Williams MR, Leon MB, Kodali SK, PARTNER Publications Office. Predictors and clinical outcomes of permanent pacemaker implantation after transcatheter aortic valve replacement: the PARTNER (Placement of AoRtic TraNscathetER Valves) trial and registry. JACC Cardiovasc Interv. 2015;8:60–9.
Ramazzina C, Knecht S, Jeger R, Kaiser C, Schaer B, Osswald S, Sticherling C, Kühne M. Pacemaker implantation and need for ventricular pacing during follow-up after transcatheter aortic valve implantation. Pacing Clin Electrophysiol. 2014;37:1592–601.
Boerlage-Van Dijk K, Kooiman KM, Yong ZY, Wiegerinck EM, Damman P, Bouma BJ, Tijssen JG, Piek JJ, Knops RE, Baan J Jr. Predictors and permanency of cardiac conduction disorders and necessity of pacing after transcatheter aortic valve implantation. Pacing Clin Electrophysiol. 2014;37:1520–9.
Barbanti M, Capranzano P, Ohno Y, Attizzani GF, Gulino S, Immè S, Cannata S, Aruta P, Bottari V, Patanè M, Tamburino C, Di Stefano D, Deste W, Giannazzo D, Gargiulo G, Caruso G, Sgroi C, Todaro D, di Simone E, Capodanno D, Tamburino C. Early discharge after transfemoral transcatheter aortic valve implantation. Heart. 2015;101:1485–90.
Durand E, Eltchaninoff H, Canville A, Bouhzam N, Godin M, Tron C, Rodriguez C, Litzler PY, Bauer F, Cribier A. Feasibility and safety of early discharge after transfemoral transcatheter aortic valve implantation with the Edwards SAPIEN-XT prosthesis. Am J Cardiol. 2015;115:1116–22.
Surawicz B, Childers R, Deal BJ, Gettes LS, Bailey JJ, Gorgels A, Hancock EW, Josephson M, Kligfield P, Kors JA, Macfarlane P, Mason JW, Mirvis DM, Okin P, Pahlm O, Rautaharju PM, van Herpen G, Wagner GS, Wellens H, American Heart Association Electrocardiography, and Arrhythmias Committee, Council on Clinical Cardiology; American College of Cardiology Foundation; Heart Rhythm Society. AHA/ACCF/HRS recommendations for the standardization and interpretation of the electrocardiogram: part III: intraventricular conduction disturbances: a scientific statement from the American Heart Association Electrocardiography and Arrhythmias Committee, Council on Clinical Cardiology; the American College of Cardiology Foundation; and the Heart Rhythm Society. Endorsed by the International Society for Computerized Electrocardiology. J Am Coll Cardiol. 2009;53:976–81.
Inohara T, Hayashida K, Watanabe Y, Yamamoto M, Takagi K, Yashima F, Arai T, Shimizu H, Chevalier B, Lefèvre T, Fukuda K, Morice MC. Streamlining the learning process for TAVI: insight from a comparative analysis of the OCEAN-TAVI and the massy registries. Catheter Cardiovasc Interv. 2016;87:963–70.
Kappetein AP, Head SJ, Genereux P, Piazza N, van Mieghem NM, Blackstone EH, et al. Updated standardized endpoint definitions for transcatheter aortic valve implantation: the Valve Academic Research Consortium-2 consensus document. J Thorac Cardiovasc Surg. 2013;145:6–23.
Brignole M, Auricchio A, Baron-Esquivias G, Bordachar P, Boriani G, Breithardt OA, Cleland J, Deharo JC, Delgado V, Elliott PM, Gorenek B, Israel CW, Leclercq C, Linde C, Mont L, Padeletti L, Sutton R, Vardas PE, ESC Committee for Practice Guidelines (CPG), Zamorano JL, Achenbach S, Baumgartner H, Bax JJ, Bueno H, Dean V, Deaton C, Erol C, Fagard R, Ferrari R, Hasdai D, Hoes AW, Kirchhof P, Knuuti J, Kolh P, Lancellotti P, Linhart A, Nihoyannopoulos P, Piepoli MF, Ponikowski P, Sirnes PA, Tamargo JL, Tendera M, Torbicki A, Wijns W, Windecker S, Reviewers D, Kirchhof P, Blomstrom-Lundqvist C, Badano LP, Aliyev F, Bänsch D, Baumgartner H, Bsata W, Buser P, Charron P, Daubert JC, Dobreanu D, Faerestrand S, Hasdai D, Hoes AW, Le Heuzey JY, Mavrakis H, McDonagh T, Merino JL, Nawar MM, Nielsen JC, Pieske B, Poposka L, Ruschitzka F, Tendera M, Van Gelder IC, Wilson CM. ESC guidelines on cardiac pacing and cardiac resynchronization therapy: the task force on cardiac pacing and resynchronization therapy of the European Society of Cardiology (ESC). Developed in collaboration with the European Heart Rhythm Association (EHRA). European Society of Cardiology (ESC); European Heart Rhythm Association (EHRA). Europace. 2013;2013(15):1070–118.
Urena M, Webb JG, Cheema A, Serra V, Toggweiler S, Barbanti M, Cheung A, Ye J, Dumont E, DeLarochellière R, Doyle D, Al Lawati HA, Peterson M, Chisholm R, Igual A, Ribeiro HB, Nombela-Franco L, Philippon F, Garcia del Blanco B, Rodés-Cabau J. Impact of new-onset persistent left bundle branch block on late clinical outcomes in patients undergoing transcatheter aortic valve implantation with a balloon-expandable valve. JACC Cardiovasc Interv. 2014;7:128–36.
Nombela-Franco L, del Trigo M, Morrison-Polo G, Veiga G, Jimenez-Quevedo P, Abdul-Jawad Altisent O, Campelo-Parada F, Biagioni C, Puri R, DeLarochellière R, Dumont E, Doyle D, Paradis JM, Quirós A, Almeria C, Gonzalo N, Nuñez-Gil I, Salinas P, Mohammadi S, Escaned J, Fernández-Ortiz A, Macaya C, Rodés-Cabau J. Incidence, causes, and predictors of early (≤30 Days) and late unplanned hospital readmissions after transcatheter aortic valve replacement. JACC Cardiovasc Interv. 2015;8:1748–57.
Hannan EL, Samadashvili Z, Jordan D, Sundt TM 3rd, Stamato NJ, Lahey SJ, Gold JP, Wechsler A, Ashraf MH, Ruiz C, Wilson S, Smith CR. Thirty-day readmissions after transcatheter aortic valve implantation versus surgical aortic valve replacement in patients with severe aortic stenosis in New York state. Circ Cardiovasc Interv. 2015;8:e002744.
De Torres-Alba F, Kaleschke G, Diller GP, Vormbrock J, Orwat S, Radke R, Reinke F, Fischer D, Reinecke H, Baumgartner H. Changes in the pacemaker rate after transition from Edwards SAPIEN XT to SAPIEN 3 transcatheter aortic valve implantation: the critical role of valve implantation height. JACC Cardiovasc Interv. 2016;9:805–13.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kagase, A., Yamamoto, M., Shimura, T. et al. Evaluation of the incidence, timing, and potential recovery rates of complete atrioventricular block after transcatheter aortic valve implantation: a Japanese multicenter registry study. Cardiovasc Interv and Ther 36, 246–255 (2021). https://doi.org/10.1007/s12928-020-00670-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12928-020-00670-6