Abstract
In some patients with chronic myeloproliferative neoplasms, myelofibrosis (MF) develops as natural evolution of the disease. The aim of this study was to analyze predictive factors that may cause MF in polycythemia vera (PV) and essential thrombocythemia (ET) patients. This retrospective study was conducted on PV and ET patients who attended our hospital between 2008 and 2019. The development of MF during follow-up was recorded, and comparisons were made of the patients who developed MF and those who did not develop MF. Evaluation was made of 126 ET and 105 PV patients. During follow-up period, MF had developed 5.7% of PV and 7.1% of ET patients. It was determined that JAK-2 mutant allele burden, lymphocyte count, vitaminB12 levels, and grade of bone marrow fibrosis at diagnosis had statistically significant impact on the development of MF in all patients. In the logistic-regression analysis, it was found that initial hemoglobin, hematocrit, neutrophil-to-lymphocyte ratio, and monocyte count for PV patients; vitaminB12, the presence of splenomegaly; and BM fibrosis at diagnosis for ET patients have statistically significant effect on MF development. The results of the current study demonstrated that some parameters especially vitamin B12 levels can be used as predictive markers for the development of MF.
Similar content being viewed by others
Introduction
Both polycythemia vera (PV) and essential thrombocythemia (ET) are BCR-ABL negative myeloproliferative neoplasms (MPNs) and the main underlying mechanism of these disorders is clonal hematopoiesis and overproduction of one or more myeloid lineages in the bone marrow (BM) [1]. Diagnosis of these diseases are made according to World Health Organization (WHO) criteria [2].
Myelofibrosis (MF) is a clonal MPN that is characterized by development of reticulin or collagen fibrosis in the BM stroma [3]. MF, may develop de novo (primary myelofibrosis [PMF]), or may occur during the clinical course of PV or ET [4]. Post-polycythemia vera MF (PPV-MF) and post-essential thrombocythemia MF (PET-MF) are diagnosed according to consensus criteria established by the International Working Group for MPN Research and Treatment (IWG-MRT) (Table 1) [5].
Transformation to MF usually occurs 7–20 years after diagnosis in ET and PV patients [6,7,8]. The cumulative incidence of developing MF at 15 years has been reported to be 12–21% for PV and 9–10% for ET [8]. When MF develops during the course of PV or ET, the survival of the patients is shortened in addition to a deterioration in quality of life due to increased constitutional symptoms. The most common symptoms are fatigue, night sweats, fever, weight loss, and bone pain [9]. Patients with PPV or PET-MF may show significantly different disease characteristics compared to patients with PMF in terms of clinical presentation or prognosis [10].
Predictive factors that may cause MF in the course of PV and ET have been investigated in many studies. The aim of this study was to examine our PV and ET patients who were followed in our center and compare them with the literature.
Patients and methods
This study was conducted on PV and ET patients who attended the Hematology Department of Diskapi Yildirim Beyazit Training and Research Hospital between 2008 and 2019. A total of 231 patients were retrospectively analyzed. The diagnosis of MPN was made according to the 2008 WHO criteria [11]. High-risk and low-risk categories were evaluated in PV and ET patients according to age and previous thrombosis history [12].
A record was made for all patients of the date of diagnosis, demographic and clinical characteristics, physical examination findings, treatment management, and follow-up period. Status of JAK2 V617F, CALR ve MPL mutations, which genetic analysis from peripheral blood had performed by using PCR, were recorded. The percentage of mutant JAK-2 allele burden of the patients was categorized as 0–29%, 30–59%, and 60–100% to reveal the relationship more clearly. Hematological parameters were examined at the time of diagnosis, including hemoglobin (Hb) level, hematocrit (Hct) level, white blood cell count (WBC), neutrophil count, lymphocyte count, monocyte count, platelet count, platelet distribution width, mean platelet volume (MPV), lactate dehydrogenase (LDH), ferritin, and B12 vitamin levels. The presence of BM fibrosis at diagnosis was recorded. European classification was used for grading fibrosis at the time of diagnosis (grade 2–3: diffuse, often coarse fiber network with no evidence of collagenization (negative trichrome stain) or diffuse, coarse fiber network with areas of collagenization (positive trichrome stain)).
Patients who developed MF during the follow-up period were recorded. The diagnosis of PPV-MF and PET-MF was made according to the IWG-MRT group criteria [5]. In all patients who developed MF, grade 2 or grade 3 reticulin or collagen fibrosis was demonstrated by bone marrow biopsy. These patients (PostMPN-MF) were compared with patients who did not develop MF (Non-MF). This comparison was made by including all patients, as well as PV and ET separately.
Statistical analysis
Data obtained in the study were analyzed statistically using the SPSS Statistics 20 software (IBM, Armonk, NY, USA). Descriptive data were given as percentages. The Independent Samples t-test (t-table value) was used to compare two independent groups with normal distribution of the measurement values, and the Mann–Whitney U-test (Z-table value) was applied to data not showing normal distribution. χ2-cross tables were used to examine the relationships between qualitative variables. Only the variables with statistical significance in the univariate analysis were included in the multivariate Cox regression model. Two-sided p values < 0.05 were considered statistically significant. Survival was estimated from Kaplan–Meier curves. Comparisons between the patient groups were made using the log-rank test.
Ethical approval and informed consent
All procedures performed in this study were conducted in accordance with the ethical standards of the institutional and/or national research committee and the 1964 Declaration of Helsinki and its subsequent amendments or comparable ethical standards.
Results
Overall patients
A total of 231 MPN patients, comprising 126 ET and 105 PV, were included in the study. The distribution of demographic and disease characteristics of the patient subgroups is given in Table 2. MF developed in 15 (6.4%) patients after a mean follow-up period of 226 (95% CI: 199.0–253.0) months.
Patients developing MF and patients without MF were compared. A statistically significant difference was found in terms of lymphocyte count according to MF status (Z = − 2.610; p = 0.009). The lymphocyte count at the time of diagnosis (initial PV or ET diagnosis) of patients with MF was significantly lower than that of non-MF patients (1.5 × 109/L [1.1–2.2] vs 2.0 × 109/L [0.6–7.1]; p = 0.009). LDH values at the time of diagnosis of patients with MF were significantly higher than those of non-MF patients (291.0 U/L [222.0–504.0] vs 253.5 U/L [140.0–625.0]; p = 0.026). The vitamin B12 levels of patients with MF were statistically significantly higher than those of non-MF patients (438.0 pg/mL [138.0–881.0] vs 281.5 pg/mL [79.0–1298.0]; p = 0.017). A statistically significant relationship was detected between development of MF and the presence of BM reticuline fibrosis at the time of diagnosis PV or ET (p < 0.05). It was determined that non-MF patients predominantly had no reticuline fibrosis in BM at diagnosis, while approximately half of the MF patients had BM fibrosis at the time of diagnosis PV or ET (≥ grade 1). The comparisons of all the parameters according to MF development status of all the patients are given in Table 3.
The mutational status of the patients was analyzed. JAK-2 V617F gene mutation was detected in 80% of both non-MF patients and post-PV/ET MF patients. The presence of the JAK-2 mutation was not significant in terms of development of MF. The JAK-2 mutant allele burden was determined to be a significant variable in terms of the development of myelofibrosis. When the post-PV/ET MF patients were examined, it was determined that 75% of these patients had JAK-2 allele burden ≥ 60%. Of the patients who did not develop MF, 86% had JAK-2 allele burden of ≤ 29%.
CALR and MPL mutation analysis could be applied to a total of 22 patients. CALR mutation was observed in 7 patients in the non-MF group, and no CALR mutation was detected in the post-MF group. MPL mutation was detected negative in both groups.
In the logistic regression analysis, using the backward method, based on the MF status in all patients, all the parameters were included in the model. In addition to the JAK-2 mutant allele burden, lymphocyte count, vitamin B12 levels, and grade of BM fibrosis at diagnosis were determined to have a statistically significant impact on the development of MF (p < 0.05); lymphocyte count OR = 0.232 [95% CI: 0.062–0.8191; p = 0.023], vitamin B12 value OR = 1.003 [95% CI: 1.000–1.007; p = 0.025], and grade of bone marrow fibrosis OR = 8.428 [95% CI: 2.021–35.144; p = 0.003]. The logistic regression analysis results of all the patients are given in Table 4.
The mean OS could not be calculated and there was no significant difference in terms of survival according to MF status as a result of the Log Rank (Mantel-Cox) test (p > 0.05).
Patients with polycythemia vera
MF developed in 6 (5.7%) of 105 PV patients during the mean follow-up period of 263 months (95% CI: 257–268). The PPV-MF and non-MF patients were compared.
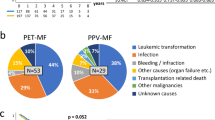
The hemoglobin and hematocrit values of the PPV-MF patients were significantly lower than those of the non-MF patients (15.9 gr/dl [15.6–17.9] vs 17.5 gr/dl [15.0–23.0]; p = 0.018 and 50.7 [48.6–56.0] vs 54.0 [47.3–68.6]; p = 0.048, respectively). The monocyte count of the PPV-MF patients was significantly lower than that of the non-MF patients (0.4 × 109/L [0.2–0.6] vs 0.6 × 109/L [0.1–3.5]; p = 0.029). The NLR values of the PPV-MF group were significantly higher than those of the non-MF patients (7.9 [3.7–14.7] vs 4.0 [1.1–27.1]; p = 0.037). A statistically significant relationship was found between development of MF and BM fibrosis (≥ grade 1) at initial diagnosis (p < 0.05). When calculated according to the patients who were applied with BM biopsy during PV diagnosis, it was determined that 4% of non-MF patients and 33.3% of PPV-MF patients had BM reticuline fibrosis at diagnosis of PV. Comparisons of all the parameters according to MF development in patients with PV are shown in Table 5.
A statistically significant relationship was detected between the MF status and the JAK-2 mutant allele burden in PV patients (p < 0.05). Of the non-MF patients, 40 (41.6%) had 0–29% JAK-2 mutant allele burden, and 5 patients (100.0%) with PPV-MF had 60–100% JAK-2 mutant allele burden. In the logistic regression analysis, the JAK-2 mutant allele burden was not found to be a significant variable in terms of MF development in patients with PV.
In the logistic regression analysis, using the backward method based on MF status in patients with PV, the Hb, Hct, NLR, and monocyte values were found to be statistically significant (p < 0.05) and OR was found to be 0.520 for Hb, 0.525 for Hct value, 1.412 for NLR, and 0.001 for monocyte count. The logistic regression analysis for PV patients is shown in Table 4.
No significant difference was deterrmined in terms of survival according to MF status (p > 0.05) and treatment status (p > 0.05) as a result of the Log Rank (Mantel-Cox) test.
Patients with essential thrombocythemia
MF developed in 9 (7.1%) of 126 ET patients during the mean follow-up period of 161 months (95% CI: 143–178). The PET-MF and non-MF patients were compared.
The lymphocyte count of the PET-MF patients was statistically significantly lower than that of non-MF patients (1.5 × 109/L [1.2–2.0] vs 2.0 × 109/L [0.7–7.1]; p = 0.033). The initial ferritin levels of those with PET-MF were significantly higher than those of the non-MF patients (71.0 ng/mL [28.6–399.0] vs 37.0 ng/mL [2.0–454.0]; p = 0.043). The vitamin B12 levels of the PET-MF patients were significantly higher than those of the non-MF patients (505.0 pg/mL [202.0–881.0] vs 289.0 pg/mL [79.0–1298.0]; p = 0.019). A statistically significant relationship was detected between MF status and the presence of splenomegaly and BM fibrosis (≥ grade 1) at ET diagnosis (p < 0.05). Splenomegaly at the time of ET diagnosis was determined in 38 (24.8%) non-MF patients and 6 (66.7%) PET-MF patients. In the analysis applied according to the patients who underwent BM biopsy during ET diagnosis, it was found that 13.7% of non-MF patients and 44.4% of PET-MF patients had BM fibrosis at ET diagnosis. Comparisons of all the parameters according to MF development in patients with ET are given in Table 6.
A statistically significant relationship was detected between the MF status and the JAK-2 mutant allele burden in ET patients (p < 0.05). JAK-2 mutant allele burden at 0–29% was determined in 44 (62.8%) non-MF patients, and at 60–100% in 8 (66.0%) PPV-MF patients. In the logistic regression analysis, JAK-2 mutant allele burden was determined to be a significant variable in terms of the development of myelofibrosis. Patients with JAK-2 mutant allele burden of ≥ 60 were 29,333 times more likely to develop myelofibrosis than patients with JAK-2 mutant allele burden of ≤ 29.
In the logistic regression analysis, using the backward method based on MF status in patients with ET, all parameters were included in the model and vitamin B12, the presence of splenomegaly and BM fibrosis at diagnosis were found to be statistically significant (p < 0.05 and OR: 1.004; 7.800; 7.590, respectively). The logistic regression analysis for ET patients is given in Table 4.
No significant difference was determined in terms of survival according to MF status (p > 0.05) and treatment status (p > 0.05) as a result of the Log Rank (Mantel-Cox) test.
Discussion
MF is characterized by fibrosis in bone marrow stroma and extramedullary hematopoiesis. Splenomegaly and cytopenias, especially transfusion related anemia and constitutional symptoms, are usually seen [13]. Fibrotic transformation may occur in the clinical course of PV and ET, which are relatively benign diseases, known as post-PV MF and post-ET MF [3].
In a study from the Mayo Clinic, fibrotic transformation rates were found to be 12.5% in PV and 10.3% in ET [14]. In another study, MF evolution was seen to occur in PV at the rate of 12–21% and in ET rate at 9–10% [8]. The frequency of development of MF is higher in PV patients than in ET patients and this complication occurs later during the course of the disease [15, 16]. The percentage of myelofibrosis development in the current study was 7.1% in ET patients and 5.7% in PV patients, which were lower rates than reported in previous studies. This may have been due to some missing data because of the retrospective design of the current study and insufficient follow-up times. Again, in contrast to previous literature, fibrotic transformation was more common in the current study patients with ET.
Hyperactivation of the JAK-STAT pathway, which causes abnormal myeloproliferation and excessive release of proinflammatory cytokines, is mainly responsible for MF pathogenesis. Most patients with MF have JAK2 (Janus kinase 2, located on chromosome 9p24) (60% of cases); CALR (calreticulin, located on chromosome 19p13.2) (20% of cases); and MPL (myeloproliferative leukemia virus oncogene, located on chromosome 1p34) (10% of cases) mutations [17, 18].
Passamonti et al.[19] showed that high JAK2 mutant allele burden was associated with post PV MF, while in another study [6], the presence of JAK2 mutation was found to be associated with a lower risk of fibrotic transformation in ET patients. JAK-2 gene mutation was detected in 80% of both non-MF patients and PET and PPV-MF patients. The JAK-2 mutation status was observed to have no effect on the development of myelofibrosis in the current study. It was also observed that patients with JAK-2 mutant allele burden of ≥ 60 were 22,897 times more likely to develop myelofibrosis than patients with JAK-2 mutant allele burden of ≤ 29. In other words, the increase in JAK-2 mutant allele burden was found to be a risk factor for the development of myelofibrosis.
ET patients with CALR mutations were found to have higher incidence of myelofibrosis, compared with JAK2-mutated patients. In the ET patients with type 1 CALR mutation, the development of myelofibrosis was observed more frequently than in patients with type 2 mutation. MPL mutations have also been associated with an increased risk of fibrotic transformation in ET [20]. In the current study, CALR mutation positivity was not determined in any of the patients with post-PV MF or post-ET MF. Although CALR mutation analysis could not be performed on all patients, it can be suggested from these data that CALR mutation positivity is not related to MF development.
Many previous studies have investigated the factors that may be associated with MF transformation.
In PV, although multiple factors have been determined to affect the development of fibrotic transformation, elevated leukocyte count (> 15 × 109/l) is the most frequently reported factor [19]. It has been shown in other studies that leukocytosis (15 × 109/l), grade of bone marrow reticuline fibrosis, long disease duration, or JAK-2 mutation allele burden (> 50%) may cause MF in PV patients [19, 21, 22]. In the current study, low hemoglobin and hemotocrit levels, low monocyte count, and increased neutrophil lymphocyte ratio (NLR) at the time of diagnosis were found to be associated with fibrotic transformation in PV patients. NLR is the proportion of absolute neutrophil count to lymphocyte count, and this is known to be well correlated with systemic inflamation and disease activity in chronic inflammatory disorders or malignancy [23, 24]. It has been reported that patients with a higher fibrosis grade in the bone marrow had a higher NLR [25]. The reason for the relationship between increased NLR and myelofibrosis in the current study may have been chronic inflammation that causes the release of fibrogenic cytokines such as transforming growth factor B1 in PV [26] or myeloproliferation itself. There are no studies showing the relationship between monocyte level or hemoglobin/hematocrite values of PV patients at initial diagnosis and the development of MF. Moreover, most diseases with inflammation are associated with monocytosis rather than monocytopenia [27]. In the current study, it was observed that MF was seen more frequently in patients with both low monocyte count and low hemoglobin/hematocrite values when they were initially diagnosed with PV. However, the reason for this relationship is not fully understood.
Studies have shown that advanced age at diagnosis and the presence of anemia are related to the development of MF in ET patients [28]. In the current study, elevated vitamin B12 levels, the presence of splenomegaly, and bone marrow fibrosis at the time of ET diagnosis were observed to increase the risk of myelofibrosis. In patients with MPN, increased cell turnover may cause vitamin B12 and folate deficiency. However, in most hematological disorders vitamin B-12 levels are higher because vitamin B-12 levels do not show the actual vitamin status but methylmalonic acid (MMA) or HoloTranscobalamine (HoloTC) are more sensitive [29]. To the best of our knowledge, there is no information in literature showing the relationship between vitamin B12 level and myelofibrosis in PV and ET patients. In the current study, it was found that MF developed more frequently in both ET and total MPN patients with elevated vitamin B12 levels at the time of initial diagnosis. In our opinion, the elevation of vitamin B12 may be related to the inflammation status at the time of diagnosis, and may be related to the elevation of the acute phase reactant, transcobalamin.
The role of inflammation in the development of myelofibrosis is well known. Chronic inflammation increases genomic instability and clonal evolution to myelofibrosis [30]. According to this idea, elevated vitamin B12 level (due to the increase in transcobalamin level), which may give a clue about the severity of inflammation when patients are diagnosed with PV and ET, may be associated with the development of MF in the future.
Splenomegaly often occurs when MF develops in PV or ET patients. In these patients, splenomegaly is generally not observed during the initial diagnosis of PV or ET.
In the current study, myelofibrosis was more likely to develop in ET patients who had splenomegaly when initially diagnosed with ET.
Reticuline or collagen fibrosis in the bone marrow has been reported in 11% of PV patients and in even fewer ET patients at diagnosis [31]. In the current study, the presence of reticuline fibrosis at initial ET diagnosis was found to be associated with PET-MF. The same results were achieved in the overall patient group. When logistic regresion analysis was performed according to the patients who underwent BM biopsy during ET diagnosis, it was found that 13.7% of non-MF patients and 44.4% of PET-MF patients had BM fibrosis at diagnosis. In the overall patient group, 9.3% of non-MF patients and 40% of post-PV/ET MF patients had BM fibrosis at diagnosis. Consequently, bone marrow fibrosis at the time of diagnosis can be considered a predictive value in terms of MF development, especially in ET patients.
Bone marrow biopsy is very important to demonstrate fibrosis and its grade. It is also necessary for diagnose pre-PMF and overt primary MF [1]. For the diagnosis of MF, grade 2 or 3 reticulin or collagen fibrosis should be demonstrated in the bone marrow [32]. Prefibrotic PMF, which is considered to be the early stage of PMF, and ET are clinically very similar. Performing a bone marrow biopsy in the diagnosis of PV and ET is also essential to eliminate the confusion between the diagnoses of pre-fibrotic PMF and ET, because the differential diagnosis of these two diseases is mainly based on the morphological findings of the bone marrow biopsy and the grade of fibrosis [33, 34]. Bone marrow biopsy findings of prefibrotic MF and ET also show changes other than collagen or reticulin fibrosis. While large and mature-appearing megakaryocytes are observed in ET; immature megakaryocytes with hyperchromatic and irregularly folded nuclei is seen in prefibrotic MF [35].
This study’s result also demonstrated that bone marrow biopsy is very important in MPNs not only for the diagnostic approach, but because it shows that the grade of fibrosis in the bone marrow poses a risk in the development of myelofibrosis and affects the course of the disease. ET and PV patients with at least grade 1 (differential diagnosis with prefibrotic MF and not meeting prefibrotic MF criteria) fibrosis in the bone marrow at the time of diagnosis should be followed more closely and carefully monitored in terms of the risk of overt myelofibrosis development.
The clinical significance of reticuline fibrosis at diagnosis has not been studied with prospective methods so it has not been well documented in the literature. Furthermore, the prognostic significance of bone marrow fibrosis at the initial MPN diagnosis is not clear. In a previous study, it was determined that an increase in bone marrow fibrosis from baseline by 1 grade was associated with increased risks of fibrotic transformation, although it was not associated with shorter survival [36]. In this context, the use of JAK2 inhibitors can be promising for patients at risk of developing myelofibrosis.
In the current study, a relationship was also determined between low lymphocyte count at the time of diagnosis and the development of fibrosis when the PV and ET patients were evaluated in total. It is known that a decreased lymphocyte count may be a characteristic feature of MF but there is not enough information about the predictive significance of lymphocyte count for fibrotic transformation [37].
The development of myelofibrosis impairs the quality of life as well as shortening survival. Hernandez-Boluda et al. found that advanced age (> 65 years), anemia (Hb < 10 gr/dl), and increased blast percentage in peripheral blood, hydroxyurea treatment at the time of fibrotic transformation to be factors that shorten OS in post PV and ET MF patients [38]. In a retrospective study of 1099 patients by Masarova et al., anemia (Hb < 10 gr/dl), and constitutional symptoms were determined to be associated with shorter OS for PPV-MF, and anemia (Hb < 10 gr/dl), trombocytopenia (Plt < 100.000 × 106/L), constitutional symptoms, and peripheral blasts ≥ 1% for PET-MF [39]. Due to the low number of patients in the current study who developed MF and the relatively short follow-up period, OS could not be calculated and thus it was not possible to make comparisons with other studies in this respect.
Although allogeneic hematopoietic stem cell transplantation is the only curative treatment for postMPN-MF, palliative treatment options are usually preferred. The treatment of PPV and PET-MF patients is focused on reducing splenomegaly-related and constitutional symptoms. The JAK1/2 inhibitor, ruxolitinib, has been used successfully in this context [40]. The Controlled Myelofibrosis Study with oral JAK inhibitor treatment (COMFORT-I/II) registrative trials also showed that ruxolitinib had a positive effect on survival [41]. However, in the current study, taking palliative therapy had no effect on survival.
In the current study, in the treatment of the non-MF group, 4 (1.9%) patients had been using anagralide, 166 patients had been using HU (76.9%), and 46 (21.2%) patients had no indication for treatment. In the post-PV/ET MF group, 1 (6.7%) patient had been using anagralide, 11 (73.3%) patients had been using HU, and 3 (20%) patients had no indication for treatment. No statistically significant relationship was determined between treatment status and MF status (p > 0.05).
There were some limitations to this study, primarily that it was a retrospective study from a single center. Second, some data may have been lost due to the long disease course. The total follow-up period should be longer for diseases such as ET and PV, which have survival rates close to those of the normal population. Furthermore, since detailed genetic studies have only just begun to be studied, genetic mutation analysis could not be performed for all patients. There is a need for further, larger prospective studies to definite inferences and strengthen the current study results.
In conclusion the results of the current study demonstrated that independently of initial BM fibrosis, the presence of splenomegaly and elevated vitamin B12 levels can predict the development of PET-MF, whereas elevated NLR and lower monocyte, Hb, and Hct can predict the development of PPV-MF. Patients with those initial predictive factors should be monitored more carefully.
References
Tefferi A, Thiele J, Orazi A, Kvasnicka HM, Barbui T, Hanson CA et al (2007) Proposals and rationale for revision of the World Health Organization diagnostic criteria for polycythemia vera, essential thrombocythemia, and primary myelofibrosis: recommendations from an ad hoc international expert panel. Blood J Am Soc Hematol 110(4):1092–1097
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM et al (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127(20):2391–2405
Cervantes F, Pereira A (2012) Prognostication in primary myelofibrosis. Curr Hematol Malig Rep 7(1):43–49. https://doi.org/10.1007/s11899-011-0102-1
Tefferi A (2003) The forgotten myeloproliferative disorder: myeloid metaplasia. Oncologist 8(3):225–231
Barosi G, Mesa RA, Thiele J, Cervantes F, Campbell PJ, Verstovsek S et al (2008) Proposed criteria for the diagnosis of post-polycythemia vera and post-essential thrombocythemia myelofibrosis: a consensus statement from the International Working Group for Myelofibrosis Research and Treatment. Leukemia 22(2):437–438. https://doi.org/10.1038/sj.leu.2404914
Passamonti F, Rumi E, Arcaini L, Boveri E, Elena C, Pietra D et al (2008) Prognostic factors for thrombosis, myelofibrosis, and leukemia in essential thrombocythemia: a study of 605 patients. Haematologica 93(11):1645–1651. https://doi.org/10.3324/haematol.13346
Passamonti F, Rumi E, Pungolino E, Malabarba L, Bertazzoni P, Valentini M et al (2004) Life expectancy and prognostic factors for survival in patients with polycythemia vera and essential thrombocythemia. Am J Med 117(10):755–761. https://doi.org/10.1016/j.amjmed.2004.06.032
Tefferi A, Guglielmelli P, Larson DR, Finke C, Wassie EA, Pieri L et al (2014) Long-term survival and blast transformation in molecularly annotated essential thrombocythemia, polycythemia vera, and myelofibrosis. Blood 124(16):2507–2513. https://doi.org/10.1182/blood-2014-05-579136 (quiz 615)
Mesa RA, Niblack J, Wadleigh M, Verstovsek S, Camoriano J, Barnes S et al (2007) The burden of fatigue and quality of life in myeloproliferative disorders (MPDs): an international internet-based survey of 1179 MPD patients. Cancer 109(1):68–76. https://doi.org/10.1002/cncr.22365
Boiocchi L, Mathew S, Gianelli U, Iurlo A, Radice T, Barouk-Fox S, et al. Morphologic and cytogenetic differences between post-polycythemic myelofibrosis and primary myelofibrosis in fibrotic stage. Modern Pathology: an official journal of the United States and Canadian Academy of Pathology, Inc. 2013;26(12):1577–85. https://doi.org/10.1038/modpathol.2013.109.
Tefferi A, Thiele J, Vardiman JW (2009) The 2008 World Health Organization classification system for myeloproliferative neoplasms: order out of chaos. Cancer 115(17):3842–3847. https://doi.org/10.1002/cncr.24440
Barbui T, Barosi G, Birgegard G, Cervantes F, Finazzi G, Griesshammer M et al (2011) Philadelphia-negative classical myeloproliferative neoplasms: critical concepts and management recommendations from European LeukemiaNet. J Clin Oncol 29(6):761
Barosi G (1999) Myelofibrosis with myeloid metaplasia: diagnostic definition and prognostic classification for clinical studies and treatment guidelines. J Clin Oncol: Official J Am Soc Clin Oncol 17(9):2954–2970. https://doi.org/10.1200/jco.1999.17.9.2954
Wolanskyj AP, Schwager SM, McClure RF, Larson DR, Tefferi A (2006) Essential thrombocythemia beyond the first decade: life expectancy, long-term complication rates, and prognostic factors. Mayo Clin Proc 81(2):159–166. https://doi.org/10.4065/81.2.159
Cervantes F, Alvarez-Larrán A, Talarn C, Gómez M, Montserrat E (2002) Myelofibrosis with myeloid metaplasia following essential thrombocythaemia: actuarial probability, presenting characteristics and evolution in a series of 195 patients. Br J Haematol 118(3):786–790. https://doi.org/10.1046/j.1365-2141.2002.03688.x
Passamonti F, Rumi E, Caramella M, Elena C, Arcaini L, Boveri E et al (2008) A dynamic prognostic model to predict survival in post-polycythemia vera myelofibrosis. Blood 111(7):3383–3387. https://doi.org/10.1182/blood-2007-11-121434
Klampfl T, Gisslinger H, Harutyunyan AS, Nivarthi H, Rumi E, Milosevic JD et al (2013) Somatic mutations of calreticulin in myeloproliferative neoplasms. N Engl J Med 369(25):2379–2390. https://doi.org/10.1056/NEJMoa1311347
Nangalia J, Massie CE, Baxter EJ, Nice FL, Gundem G, Wedge DC et al (2013) Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N Engl J Med 369(25):2391–2405. https://doi.org/10.1056/NEJMoa1312542
Passamonti F, Rumi E, Pietra D, Elena C, Boveri E, Arcaini L et al (2010) A prospective study of 338 patients with polycythemia vera: the impact of JAK2 (V617F) allele burden and leukocytosis on fibrotic or leukemic disease transformation and vascular complications. Leukemia 24(9):1574–1579. https://doi.org/10.1038/leu.2010.148
Spivak JL (2017) Myeloproliferative neoplasms. N Engl J Med 376(22):2168–2181. https://doi.org/10.1056/NEJMra1406186
Barbui T, Thiele J, Passamonti F, Rumi E, Boveri E, Randi ML et al (2012) Initial bone marrow reticulin fibrosis in polycythemia vera exerts an impact on clinical outcome. Blood 119(10):2239–2241. https://doi.org/10.1182/blood-2011-11-393819
Marchioli R, Finazzi G, Landolfi R, Kutti J, Gisslinger H, Patrono C et al (2005) Vascular and neoplastic risk in a large cohort of patients with polycythemia vera. J Clin Oncol: Official J Am Soc Clin Oncol 23(10):2224–2232. https://doi.org/10.1200/jco.2005.07.062
Mercan R, Bitik B, Tufan A, Bozbulut UB, Atas N, Ozturk MA et al (2016) The association between neutrophil/lymphocyte ratio and disease activity in rheumatoid arthritis and ankylosing spondylitis. J Clin Lab Anal 30(5):597–601. https://doi.org/10.1002/jcla.21908
Proctor MJ, McMillan DC, Morrison DS, Fletcher CD, Horgan PG, Clarke SJ (2012) A derived neutrophil to lymphocyte ratio predicts survival in patients with cancer. Br J Cancer 107(4):695–699. https://doi.org/10.1038/bjc.2012.292
Romano A, Palandri F, Masarova L, Bonifacio M, Polverelli N, Elli EM et al (2018) Prognostic role of neutrophil to lymphocyte ratio (NLR) in myelofibrosis patients treated with ruxolitinib: a multi-center experience. Blood 132(Supplenent 1):4303. https://doi.org/10.1182/blood-2018-99-116418
Kisseleva T, Brenner DA (2008) Mechanisms of fibrogenesis. Exp Biol Med 233(2):109–122
Wong KL, Yeap WH, Tai JJ, Ong SM, Dang TM, Wong SC (2012) The three human monocyte subsets: implications for health and disease. Immunol Res 53(1–3):41–57. https://doi.org/10.1007/s12026-012-8297-3
Barbui T, Thiele J, Passamonti F, Rumi E, Boveri E, Ruggeri M et al (2011) Survival and disease progression in essential thrombocythemia are significantly influenced by accurate morphologic diagnosis: an international study. J Clin Oncol: Official J Am Soc Clin Oncol 29(23):3179–3184. https://doi.org/10.1200/jco.2010.34.5298
Vener C, Novembrino C, Catena FB, Fracchiolla NS, Gianelli U, Savi F et al (2010) Oxidative stress is increased in primary and post-polycythemia vera myelofibrosis. Exp Hematol 38(11):1058–1065. https://doi.org/10.1016/j.exphem.2010.07.005
Gaman AM, Moisa C, Diaconu CC, Gaman MA (2019) Crosstalk between oxidative stress, chronic inflammation and disease progression in essential thrombocythemia. Rev Chim 70(10):3486–3489
Ellis JT, Peterson P, Geller SA, Rappaport H (1986) Studies of the bone marrow in polycythemia vera and the evolution of myelofibrosis and second hematologic malignancies. Semin Hematol 23(2):144–155
Cervantes F, Dupriez B, Pereira A, Passamonti F, Reilly JT, Morra E et al (2009) New prognostic scoring system for primary myelofibrosis based on a study of the International Working Group for Myelofibrosis Research and Treatment. Blood 113(13):2895–2901. https://doi.org/10.1182/blood-2008-07-170449
Georgii A, Buhr T, Buesche G, Kreft A, Choritz H (1996) Classification and staging of Ph-negative myeloproliferative disorders by histopathology from bone marrow biopsies. Leuk Lymphoma 22(sup1):15–29
Guglielmelli P, Pacilli A, Rotunno G, Rumi E, Rosti V, Delaini F et al (2017) Presentation and outcome of patients with 2016 WHO diagnosis of prefibrotic and overt primary myelofibrosis. Blood J Am Soc Hematol 129(24):3227–3236
Tefferi A (2013) Primary myelofibrosis: 2013 update on diagnosis, risk-stratification, and management. Am J Hematol 88(2):141–150
Campbell PJ, Bareford D, Erber WN, Wilkins BS, Wright P, Buck G et al (2009) Reticulin accumulation in essential thrombocythemia: prognostic significance and relationship to therapy. J Clin Oncol: Official J Am Soc Clin Oncol 27(18):2991–2999. https://doi.org/10.1200/jco.2008.20.3174
Cervantes F, Hernandez-Boluda JC, Villamor N, Serra A, Montserrat E (2000) Assessment of peripheral blood lymphocyte subsets in idiopathic myelofibrosis. Eur J Haematol 65(2):104–108. https://doi.org/10.1034/j.1600-0609.2000.90262.x
Hernandez-Boluda JC, Pereira A, Gomez M, Boque C, Ferrer-Marin F, Raya JM et al (2014) The International Prognostic Scoring System does not accurately discriminate different risk categories in patients with post-essential thrombocythemia and post-polycythemia vera myelofibrosis. Haematologica 99(4):e55–e57. https://doi.org/10.3324/haematol.2013.101733
Masarova L, Bose P, Daver N, Pemmaraju N, Newberry KJ, Manshouri T et al (2017) Patients with post-essential thrombocythemia and post-polycythemia vera differ from patients with primary myelofibrosis. Leuk Res 59:110–116. https://doi.org/10.1016/j.leukres.2017.06.001
Harrison CN, Vannucchi AM, Kiladjian JJ, Al-Ali HK, Gisslinger H, Knoops L et al (2016) Long-term findings from COMFORT-II, a phase 3 study of ruxolitinib vs best available therapy for myelofibrosis. Leukemia 30(8):1701–1707. https://doi.org/10.1038/leu.2016.148
Cervantes F, Pereira A (2017) Does ruxolitinib prolong the survival of patients with myelofibrosis? Blood 129(7):832–837. https://doi.org/10.1182/blood-2016-11-731604
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The abstract of this study was presented as a poster at the 7. Aegean Hematology Oncology Symposium-AHOS 2020.
Rights and permissions
About this article
Cite this article
Tığlıoğlu, P., Albayrak, M., Yıldız, A. et al. Analysis of factors associated with the development of myelofibrosis in polycythemia vera and essential thrombocythemia patients: a single-center experience. J Hematopathol 15, 83–93 (2022). https://doi.org/10.1007/s12308-022-00488-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12308-022-00488-6