Abstract
Background
We performed this study to analyze changing survival patterns regarding recurrent breast cancer in Korea during the last 16 years (1993–2008). We also sought to determine factors possibly influencing outcomes and changes over time in the duration of survival after recurrence.
Methods
We retrospectively analyzed 9671 patients with breast cancer treated between January 1993 and December 2008, comparing the periods 1993–2002 and 2003–2008.We retrospectively reviewed the collected database including the age at diagnosis, clinical manifestations, pathology report, surgical methods, types of adjuvant treatment modalities, type of recurrence, and follow-up period.
Results
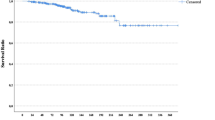
There were 1944 cases (20.1%) of recurrence. Median age at the first recurrence was 49.5 years (range 21.8–92.9). Median follow-up was 28.8 months (range 0–228.0) from the time of relapse. Median survival time was 35.0 months. Survival after recurrence (SAR) significantly improved in 2003–2008 compared to that in 1993–2002. Median survival time increased from 27.6 months in the period I to 42.3 months in period II (p = 0.001). Independent prognostic factors after the first recurrence by multivariate analysis were age at diagnosis, tumor size, nodal status, tumor grade, subtype, anti-hormonal therapy, time at diagnosis, and disease-free interval.
Conclusions
Outcomes of breast cancer have been improving recently, and survival time after the first recurrence of breast cancer has steadily increased in recent decades. We confirmed that advances in treatments have contributed to this improvement in survival after the first recurrence.



Similar content being viewed by others
References
Haffty BG, Fischer D, Beinfield M, McKhann C. Prognosis following local recurrence in the conservatively treated breast cancer patient. Int J Radiat Oncol Biol Phys. 1991;21:293–8.
Ravdin PM, Siminoff LA, Davis GJ, Mercer MB, Hewlett J, Gerson N, et al. Computer program to assist in making decisions about adjuvant therapy for women with early breast cancer. J Clin Oncol. 2001;19:980–91.
Michaelson JS, Chen LL, Bush D, Fong A, Smith B, Younger J. Improved web-based calculators for predicting breast carcinoma outcomes. Breast Cancer Res Treat. 2011;128:827–35. https://doi.org/10.1007/s10549-011-1366-9.
Tsuji W, Teramukai S, Ueno M, Toi M, Inamoto T. Prognostic factors for survival after first recurrence in breast cancer: a retrospective analysis of 252 recurrent cases at a single institution. Breast Cancer. 2014;21:86–95. https://doi.org/10.1007/s12282-012-0358-x.
Giordano SH, Buzdar AU, Smith TL, Kau SW, Yang Y, Hortobagyi GN. Is breast cancer survival improving? Cancer. 2004;100:44–52.
Chapman JA, Trudeau ME, Pritchard KI, Sawka CA, Mobbs BG, Hanna WM, et al. A comparison of all-subset Cox and accelerated failure time models with Cox step-wise regression for node-positive breast cancer. Breast Cancer Res Treat. 1992;22:263–72.
McCready DR, Chapman JA, Hanna WM, Kahn HJ, Murray D, Fish EB, et al. Factors affecting distant disease-free survival for primary invasive breast cancer: use of a log-normal survival model. Ann Surg Oncol. 2000;7:416–26.
Koenders PG, Beex LV, Kloppenborg PW, Smals AG, Benraad TJ. Human breast cancer: survival from first metastasis. Breast Cancer Study Group. Breast Cancer Res Treat. 1992;21:173–80.
Weichselbaum RR, Hellman S. Oligometastases revisited. Nat Rev Clin Oncol. 2011;8:378–82.
Thelen A, Benckert C, Jonas S, Lopez-Hanninen E, Sehouli J, Neumann U, et al. Liver resection for metastases from breast cancer. J Surg Oncol. 2008;97:25–9. https://doi.org/10.1002/jso.20911.
Clark GM, Sledge GW Jr, Osborne CK, McGuire WL. Survival from first recurrence: relative importance of prognostic factors in 1,015 breast cancer patients. J Clin Oncol. 1987;5:55–61. https://doi.org/10.1200/jco.1987.5.1.55.
Vogel CL, Azevedo S, Hilsenbeck S, East DR, Ayub J. Survival after first recurrence of breast cancer. The Miami experience. Cancer. 1992;70:129–35.
Korean Breast Cancer Society. Nationwide Korean breast cancer data of 2004 using breast cancer registration program. J Breast Cancer. 2006;9:151–61. https://doi.org/10.4048/jbc.2006.9.2.151.
Jung YS, Na KY, Kim KS, Ahn SH, Lee SJ, Lee SJ, et al. Nation-wide Korean breast cancer data from 2008 using the breast cancer registration program. J Breast Cancer. 2011;14:229–36. https://doi.org/10.4048/jbc.2011.14.3.229.
Korean Breast Cancer Society. Nationwide Korean breast cancer data of 2002. J Korean Breast Cancer Soc. 2004;7:72–83.
Ahn SH. Clinical characteristics of breast cancer patients in Korea in 2000. Arch Surg. 2004;139:27–30. discussion 1.
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90. https://doi.org/10.3322/caac.20107.
Early Breast Cancer Trialists’ Collaborative Group. Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomised trials. Lancet. 2005;365:1687–1717. https://doi.org/10.1016/S0140-6736(05)66544-0.
Valagussa P, Bonadonna G, Veronesi U. Patterns of relapse and survival following radical mastectomy. Analysis of 716 consecutive patients. Cancer. 1978;41:1170–8.
Yamashita H, Iwase H, Toyama T, Takahashi S, Sugiura H, Yoshimoto N, et al. Estrogen receptor-positive breast cancer in Japanese women: trends in incidence, characteristics, and prognosis. Ann Oncol. 2011;22:1318–25. https://doi.org/10.1093/annonc/mdq596.
You JM, Kim YG, Moon HG, Nam SJ, Lee JW, Lim W, et al. Survival improvement in Korean breast cancer patients due to increases in early-stage cancers and hormone receptor positive/HER2 negative subtypes: a nationwide registry-based study. J Breast Cancer. 2015;18:8–15. https://doi.org/10.4048/jbc.2015.18.1.8.
Powles TJ, Coombes RC, Smith IE, Jones JM, Ford HT, Gazet JC. Failure of chemotherapy to prolong survival in a group of patients with metastatic breast cancer. Lancet. 1980;1:580–2.
Bonadonna G, Valagussa P, Rossi A, Tancini G, Brambilla C, Zambetti M, et al. Ten-year experience with CMF-based adjuvant chemotherapy in resectable breast cancer. Breast Cancer Res Treat. 1985;5:95–115.
Gentilini O, Botteri E, Veronesi P, Sangalli C, Del Castillo A, Ballardini B, et al. Repeating conservative surgery after ipsilateral breast tumor reappearance: criteria for selecting the best candidates. Ann Surg Oncol. 2012;19:3771–6. https://doi.org/10.1245/s10434-012-2404-5.
Botteri E, Rotmensz N, Sangalli C, Toesca A, Peradze N, De Oliveira Filho HR, et al. Unavoidable mastectomy for ipsilateral breast tumour recurrence after conservative surgery: patient outcome. Ann Oncol. 2009;20:1008–12. https://doi.org/10.1093/annonc/mdn732.
Davies C, Godwin J, Gray R, Clarke M, Cutter D, Darby S, et al. Relevance of breast cancer hormone receptors and other factors to the efficacy of adjuvant tamoxifen: patient-level meta-analysis of randomised trials. Lancet. 2011;378:771–84. https://doi.org/10.1016/s0140-6736(11)60993-8.
Peto R, Davies C, Godwin J, Gray R, Pan HC, Clarke M, et al. Comparisons between different polychemotherapy regimens for early breast cancer: meta-analyses of long-term outcome among 100,000 women in 123 randomised trials. Lancet. 2012;379:432–44. https://doi.org/10.1016/s0140-6736(11)61625-5.
Aebi S, Gelber S, Anderson SJ, Lang I, Robidoux A, Martin M, et al. Chemotherapy for isolated locoregional recurrence of breast cancer (CALOR): a randomised trial. Lancet Oncol. 2014;15:156–63. https://doi.org/10.1016/s1470-2045(13)70589-8.
Bhoo-Pathy N, Verkooijen HM, Tan EY, Miao H, Taib NA, Brand JS, et al. Trends in presentation, management and survival of patients with de novo metastatic breast cancer in a Southeast Asian setting. Sci Rep. 2015;5:16252. https://doi.org/10.1038/srep16252.
Di Meglio A, Freedman RA, Lin NU, Barry WT, Metzger-Filho O, Keating NL, et al. Time trends in incidence rates and survival of newly diagnosed stage IV breast cancer by tumor histology: a population-based analysis. Breast Cancer Res Treat. 2016;157:587–96. https://doi.org/10.1007/s10549-016-3845-5.
Inoue K, Ogawa M, Horikoshi N, Aiba K, Mukaiyama T, Mizunuma N, et al. Evaluation of prognostic factors for 233 patients with recurrent advanced breast cancer. Jpn J Clin Oncol. 1991;21:334–9.
Paterson AH, Zuck VP, Szafran O, Lees AW, Hanson J. Influence and significance of certain prognostic factors on survival in breast cancer. Eur J Cancer Clin Oncol. 1982;18:937–43.
Chang J, Clark GM, Allred DC, Mohsin S, Chamness G, Elledge RM. Survival of patients with metastatic breast carcinoma: importance of prognostic markers of the primary tumor. Cancer. 2003;97:545–53. https://doi.org/10.1002/cncr.11083.
Howell A, Barnes DM, Harland RN, Redford J, Bramwell VH, Wilkinson MJ, et al. Steroid-hormone receptors and survival after first relapse in breast cancer. Lancet. 1984;1:588–91.
Pater JL, Mores D, Loeb M. Survival after recurrence of breast cancer. Can Med Assoc J. 1981;124:1591–5.
Insa A, Lluch A, Prosper F, Marugan I, Martinez-Agullo A, Garcia-Conde J. Prognostic factors predicting survival from first recurrence in patients with metastatic breast cancer: analysis of 439 patients. Breast Cancer Res Treat. 1999;56:67–78.
Acknowledgements
This study was supported by a grant (2012-510, 2013-510) from Asan Institute for Life Sciences, Asan Medical Center, Seoul, Korea. The authors thank all clinical surgeons for collecting data. SB Lee and SH Ahn substantially contributed to the conception and design of the study, and to the analysis and interpretation of the data; SB Lee drafted the paper, and all authors revised the paper for intellectual content and approved the final version of the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors do not have any conflicts of interests to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Lee, S.B., Sohn, G., Kim, J. et al. Survival analysis according to period and analysis of the factors influencing changes in survival in patients with recurrent breast cancer: a large-scale, single-center study. Breast Cancer 25, 639–649 (2018). https://doi.org/10.1007/s12282-018-0869-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-018-0869-1