Abstract
Background
There is increasing evidence for the role of inflammation in clinical outcome after subarachnoid hemorrhage (SAH). Specifically, the TNF-alfa(α) pathway seems to be relevant after SAH. Although the TNF-α main receptor, TNF-R1 is associated with aneurysm growth and rupture, its relation to prognosis is unknown.
We sought to compare TNF-R1 levels in peripheral venous blood and arterial blood closer to the ruptured aneurysm to study the association of TNF-R1 blood levels with poor prognosis (modified Rankin Scale > 2 at discharge, 3 and 6 months) and complications (hydrocephalus or delayed cerebral ischemia/DCI) following SAH.
Methods
We included consecutive SAH patients admitted in the first 72 h of symptoms. Blood samples were simultaneously collected from a peripheral vein and from the main parent artery of the aneurysm. Levels of TNF-R1 were measured using enzyme-linked immunosorbent assays.
Results
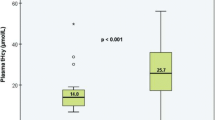
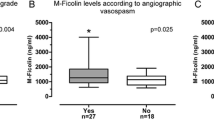
We analyzed 58 patients. Arterial and venous levels of TNF-R1 were correlated (R = 0.706, p < 0.001). In multivariate regression analysis, venous TNF-R1 was an independent predictor of poor outcome at 6 months after adjusting by age and sex [odds ratio (OR) 11.63; 95% CI 2.09–64.7, p = 0.005] and after adjusting by Glasgow Coma Scale and Fisher scales (OR 8.74; 95% CI 1.45–52.7, p = 0.018). There was no association of TNF-R1 with DCI. A cut-off for arterial TNF-R1 of 1523.7 pg/mL had 75% sensitivity/66% specificity for the prediction of hydrocephalus.
Conclusion
Levels of venous TNF-R1 are associated with poor outcome in SAH. A specific association was found between levels of arterial TNF-R1 and hydrocephalus. These results are consistent with the role of TNF-α pathway in SAH and need to be validated in larger cohorts.




Similar content being viewed by others
References
Hop JW, Rinkel GJE, Algra A, van Gijn J. Case-fatality rates and functional outcome after subarachnoid hemorrhage: a systematic review. Stroke. 1997;28(3):660–4.
Rosengart AJ, Schultheiss KE, Tolentino J, Macdonald RL. Prognostic factors for outcome in patients with aneurysmal subarachnoid hemorrhage. Stroke. 2007;38(8):2315–21.
Hijdra A, Van Gijn J, Nagelkerke NJD, Vermeulen M, Van Crevel H. Prediction of delayed cerebral ischemia, rebleeding, and outcome after aneurysmal subarachnoid hemorrhage. Stroke. 1988;19:1250–7.
Vergouwen MDI, Ilodigwe D, MacDonald RL. Cerebral infarction after subarachnoid hemorrhage contributes to poor outcome by vasospasm-dependent and -independent effects. Stroke. 2011;42(4):924–9.
Hong CM, Tosun C, Kurland DB, Gerzanich V. Biomarkers as outcome predictors in subarachnoid hemorrhage–a systematic review. Biomarkers. 2014;19(2):95–108.
Jordan JD, Nyquist P. Biomarkers and Vasospasm after aneurysmal subarachnoid hemorrhage. Neurosurg Clin N Am. 2010;21(2):381–91.
Chou SH-Y, Feske SK, Simmons SL, et al. Elevated peripheral neutrophils and matrix metalloproteinase 9 as biomarkers of functional outcome following subarachnoid hemorrhage. Transl Stroke Res. 2011;2(4):600–7.
McGirt MJ, Lynch JR, Blessing R, Warner DS, Friedman AH, Laskowitz DT. Serum von Willebrand factor, matrix metalloproteinase-9, and vascular endothelial growth factor levels predict the onset of cerebral vasospasm after aneurysmal subarachnoid hemorrhage. Neurosurgery. 2002;51(5):1125–8.
Seifert V, Loffler BM, Zimmermann M, Roux S, Stolke D. Endothelin concentrations in patients with aneurysmal subarachnoid hemorrhage. Correlation with cerebral vasospasm, delayed ischemic neurological deficits, and volume of hematoma. J Neurosurg. 1995;82(1):55–62.
Schebesch K-M, Brawanski A, Bele S, et al. Neuropeptide Y—an early biomarker for cerebral vasospasm after aneurysmal subarachnoid hemorrhage. Neurol Res. 2013;35(10):1038–43.
Wang J, Wang J-F, Hu X-M. Caspase-3 in serum predicts outcome after aneurysmal subarachnoid hemorrhage. Clin Chim Acta. 2016;460:196–202.
Frijns CJM, Rinkel GJE, Castigliego D, Van Gijn J, Sixma JJ, Fijnheer R. Endothelial cell activation after subarachnoid hemorrhage. Neurosurgery. 2002;50(6):1223–30.
Mathiesen T, Edner G, Ulfarsson E, Andersson B. Cerebrospinal fluid interleukin-1 receptor antagonist and tumor necrosis factor-alpha following subarachnoid hemorrhage. J Neurosurg. 1997;87(2):215–20.
Chou SH, Feske SK, Atherton J, et al. Early elevation of serum TNFα is associated with poor outcome in subarachnoid hemorrhage. J Investig Med. 2012;60(7):1054–8.
Young AMH, Karri SK, You W, Ogilvy CS. Specific TNF-alpha inhibition in cerebral aneurysm formation and subarachnoid hemorrhage. Curr Drug Saf. 2012;7(3):190–6.
Rogy MA, Coyle SM, Oldenburg HS, et al. Persistently elevated soluble tumor necrosis factor receptor and interleukin-1 receptor antagonist levels in critically ill patients. J Am Coll Surg. 1994;178(2):132–8.
Frontera JA, Claassen J, Schmidt JM, et al. Prediction of symptomatic vasospasm after subarachnoid hemorrhage: the modified fisher scale. Neurosurgery. 2006;59(1):21–7.
Hijdra A, Brouwers PJ, Vermeulen M, van Gijn J. Grading the amount of blood on computed tomograms after subarachnoid hemorrhage. Stroke. 1990;21(8):1156–61.
van Gijn J, Hijdra A, Wijdicks EF, Vermeulen M, van Crevel H. Acute hydrocephalus after aneurysmal subarachnoid hemorrhage. J Neurosurg. 1985;63(3):355–62.
Frontera JA, Fernandez A, Schmidt JM, et al. Defining vasospasm after subarachnoid hemorrhage: What is the most clinically relevant definition? Stroke. 2009;40(6):1963–8.
Vergouwen MDI, Vermeulen M, Muizelaar JP, et al. Definition of delayed cerebral ischemia after aneurysmal subarachnoid hemorrhage as an outcome event in clinical trials and observational studies proposal of a multidisciplinary research group. Stroke. 2010;41:2391–5.
Janssen PM, Visser NA, Dorhout Mees SM, Klijn CJM, Algra A, Rinkel GJE. Comparison of telephone and face-to-face assessment of the modified Rankin Scale. Cerebrovasc Dis. 2010;29(2):137–9.
Aoki T, Fukuda M, Nishimura M, Nozaki K, Narumiya S. Critical role of TNF-alpha-TNFR1 signaling in intracranial aneurysm formation. Acta Neuropathol Commun. 2014;2(1):34.
Gruber A, Rössler K, Graninger W, Donner A, Illievich MU, Czech T. Ventricular cerebrospinal fluid and serum concentrations of sTNFR-I, IL-1ra, and IL-6 after aneurysmal subarachnoid hemorrhage. J Neurosurg Anesthesiol. 2000;12(4):297–306.
Sedger LM, McDermott MF. TNF and TNF-receptors: from mediators of cell death and inflammation to therapeutic giants—past, present and future. Cytokine Growth Factor Rev. 2014;25(4):453–72.
Lotocki G, Alonso OF, Dietrich WD, Keane RW. Tumor necrosis factor receptor 1 and its signaling intermediates are recruited to lipid rafts in the traumatized brain. J Neurosci. 2004;24(49):11010–6.
Lucke-Wold BP, Logsdon AF, Manoranjan B, et al. Aneurysmal subarachnoid hemorrhage and neuroinflammation: a comprehensive review. Int J Mol Sci. 2016;17(4):1–17.
Sehba FA, Pluta RM, Zhang JH. Metamorphosis of subarachnoid hemorrhage research: from delayed vasospasm to early brain injury. Mol Neurobiol. 2011;43(1):27–40.
Pantoni L, Sarti C, Inzitari D. Cytokines and cell adhesion molecules in cerebral ischemia: experimental bases and therapeutic perspectives. Arterioscler Thromb Vasc Biol. 1998;18(4):503–13.
McKeating EG, Andrews PJ, Signorini DF, Mascia L. Transcranial cytokine gradients in patients requiring intensive care after acute brain injury. Br J Anaesth. 1997;78(5):520–3.
Hirashima Y, Nakamura S, Endo S, Kuwayama N, Naruse Y, Takaku A. Elevation of platelet activating factor, inflammatory cytokines, and coagulation factors in the internal jugular vein of patients with subarachnoid hemorrhage. Neurochem Res. 1997;22(10):1249–55.
Tuttolomondo A, Pecoraro R, Pinto A. Studies of selective TNF inhibitors in the treatment of brain injury from stroke and trauma: a review of the evidence to date. Drug Des Dev Ther. 2014;8:2221–39.
Acknowledgments
We thank the Clinical Pathology Laboratory of Hospital São José, CHLC, for careful preparation of the blood samples.
Funding
Dr Fragata was supported by Sociedade Portuguesa de AVC/Tecnifar. Dr Bustamante is supported by a Juan Rodes research contract (JR16/00008) from Instituto de Salud Carlos III.
Author information
Authors and Affiliations
Contributions
IF, AB, PC, JM contributed to project design; IF, AB, AP, PF, APN contributed to data collection; AB, IF performed data analysis; IF, AB, JM, PC contributed to Writing. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
Institutional review board approval was obtained for this study. Informed consent obtained from patient or legal representative.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
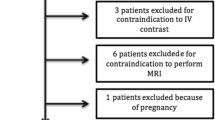
Figure 1
Flowchart depicting patients enrolled, included, and excluded in the study (TIFF 80095 kb)
Rights and permissions
About this article
Cite this article
Fragata, I., Bustamante, A., Penalba, A. et al. Venous and arterial TNF-R1 predicts outcome and complications in acute subarachnoid hemorrhage. Neurocrit Care 31, 107–115 (2019). https://doi.org/10.1007/s12028-019-00669-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-019-00669-9