Abstract
Purpose of Review
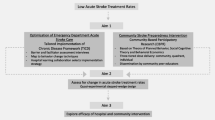
Acute stroke treatments reduce the risk of post-stroke disability. These treatments, tissue plasminogen activator (tPA) and intra-arterial treatment, are highly time-dependent; thus, one of the main barriers to treatment is pre-hospital delay. Stroke preparedness is defined as the ability to recognize stroke symptoms and the intent to activate emergency medical services (EMS). This review describes types of acute stroke treatment and preparedness interventions, including recent mass media interventions to increase acute stroke treatment rates, and adult and youth community interventions to increase stroke preparedness.
Recent Findings
The mass media campaigns show mixed results regarding acute stroke treatment rates, possibly attributed to the various media platforms utilized and resources available. The adult and youth community interventions reveal an overall increase in stroke symptom recognition and behavioral intent to call EMS. However, most of these community interventions were not grounded in health behavior theory, and they were tested in single group, pre-post test study designs that assessed behavioral rather than clinical outcomes. The delivery of stroke preparedness information by youth to adults, for example via home assignments, is a promising and innovative approach to stroke preparedness.
Summary
Mass media and community interventions show promise to increase stroke preparedness and acute stroke treatment rates. The development of health behavior theory-based interventions that are tested via scientifically rigorous study designs are needed to prioritize which interventions should be disseminated to culturally and socially similar communities.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Wilkinson PR, Wolfe CDA, Warburton FG, et al. A long-term follow-up of stroke patients. Stroke. 1997;28(3):507–12.
Kelly-Hayes M, Beiser A, Kase CS, Scaramucci A, D’Agostino RB, Wolf PA. The influence of gender and age on disability following ischemic stroke: the Framingham study. J Stroke Cerebrovasc Dis. 2003;12(3):119–26.
Hacke W, Donnan G, Fieschi C, et al. Association of outcome with early stroke treatment: pooled analysis of ATLANTIS, ECASS, and NINDS rt-PA stroke trials. Lancet. 2004;363(9411):768–74.
Powers WJ, Derdeyn CP, Biller J, et al. American Heart Association/American Stroke Association Focused update of the 2013 Guidelines for the Early Management of Patients with Acute Ischemic Stroke Regarding Endovascular Treatment a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2015. 2015;46(10):3020–35.
• Skolarus LE, Meurer WJ, Shanmugasundaram K, Adelman EE, Scott PA, Burke JF. Marked regional variation in acute stroke treatment among Medicare beneficiaries. Stroke. 2015;46(7):1890–6. A retrospective cross-sectional study of regional differences in thrombolysis rates among Medicare fee-for-service beneficiaries demonstrating substantial regional variation in thrombolysis treatment rates. These results suggest considerable opportunities to improve thromboytic treatment rates.
Kunisawa S, Morishima T, Ukawa N, et al. Association of geographical factors with administration of tissue plasminogen activator for acute ischemic stroke. J Am Heart Assoc. 2013;2(5):e000336.
Evenson KR, Foraker RE, Morris DL, Rosamond WD. A comprehensive review of prehospital and in-hospital delay times in acute stroke care. Int J stroke : Off J Int Stroke Soc. 2009;4(3):187–99.
Kleindorfer D, Kissela B, Schneider A, et al. Eligibility for recombinant tissue plasminogen activator in acute ischemic stroke: a population-based study. Stroke. 2004;35(2):e27–9.
Rosamond WD, Gorton RA, Hinn AR, Hohenhaus SM, Morris DL. Rapid response to stroke symptoms: the Delay in Accessing Stroke Healthcare (DASH) study. Acad Emerg Med. 1998;5(1):45–51.
Saver JL. Time is brain—quantified. Stroke. 2006;37(1):263–6.
Schroeder EB, Rosamond WD, Morris DL, Evenson KR, Hinn AR. Determinants of use of emergency medical services in a population with stroke symptoms: the Second Delay in Accessing Stroke Healthcare (DASH II) Study. Stroke. 2000;31(11):2591–6.
Williams LS, Bruno A, Rouch D, Marriott DJ. Stroke patients’ knowledge of stroke. Influence on time to presentation. Stroke. 1997;28(5):912–5.
Menon SC, Pandey DK, Morgenstern LB. Critical factors determining access to acute stroke care. Neurology. 1998;51(2):427–32.
Centers for Disease C. Prevention: Prehospital and hospital delays after stroke onset—United States, 2005-2006. MMWR Morb Mortal Wkly Rep. 2007;56(19):474–8.
Wester P, Radberg J, Lundgren B, Peltonen M. Factors associated with delayed admission to hospital and in-hospital delays in acute stroke and TIA: a prospective, multicenter study. Seek-Medical-Attention-in-Time Study Group. Stroke. 1999;30(1):40–8.
Glanz K, Bishop DB. The role of behavioral science theory in development and implementation of public health interventions. Annu Rev Public Health. 2010;31:399–418.
Wein TH, Staub L, Felberg R, et al. Activation of emergency medical services for acute stroke in a nonurban population: the T.L.L. Temple Foundation Stroke Project. Stroke. 2000;31(8):1925–8.
Kothari RU, Pancioli A, Liu T, Brott T, Broderick J. Cincinnati prehospital stroke scale: reproducibility and validity. Ann Emerg Med. 1999;33(4):373–8.
Mellon L, Hickey A, Doyle F, Dolan E, Williams D. Can a media campaign change health service use in a population with stroke symptoms? Examination of the first Irish stroke awareness campaign. Emerg Med J 2013.
Nishijima H, Kon T, Ueno T, et al. Effect of educational television commercial on pre-hospital delay in patients with ischemic stroke. Neurol Sci. 2016;37(1):105–9.
• Flynn D, Ford GA, Rodgers H, Price C, Steen N, Thomson RG. A time series evaluation of the FAST national stroke awareness campaign in England. 2014. Interrupted time series analysis of the UK FAST campaign demonstrating an increase in emergency department (ED) stroke presentations and acute stroke treatment rates over time.
Bray JE, Straney L, Barger B, Finn J. Effect of public awareness campaigns on calls to ambulance across Australia. Stroke. 2015;46(5):1377–80.
Dombrowski SU, Mackintosh JE, Sniehotta FF, et al. The impact of the UK ‘Act FAST’ stroke awareness campaign: content analysis of patients, witness and primary care clinicians’ perceptions. BMC Public Health. 2013;13(1):915.
Trobbiani K, Freeman K, Arango M, Lalor E, Jenkinson D, Thrift AG. Comparison of stroke warning sign campaigns in Australia, England, and Canada. Int J Stroke. 2013;8(A100):28–31.
Wakefield MA, Loken B, Hornik RC. Use of mass media campaigns to change health behaviour. The Lancet. 2010;376(9748):1261–71.
Ajzen I. The theory of planned behavior. Organ Behav Hum Decis Process. 1991;50(2):179–211.
Gardois P, Booth A, Goyder E, Ryan T. Health promotion interventions for increasing stroke awareness in ethnic minorities: a systematic review of the literature. BMC public health. 2014;14(1):409.
Yang L, Zhao Q, Zhu X, et al. Effect of a comprehensive health education program on pre-hospital delay intentions in high-risk stroke population and caregivers. Qual Life Res. 2017:1–8.
Kilkenny MF, Purvis T, Werner M, Reyneke M, Czerenkowski J, Cadilhac DA. Improving stroke knowledge through a ‘volunteer-led’ community education program in Australia. Prev Med. 2016;86:1–5.
Skolarus LE, Zimmerman MA, Bailey S, et al. Stroke ready intervention: community engagement to decrease prehospital delay. J Am Heart Assoc. 2016;5(5):e003331.
Ravenell J, Leighton-Herrmann E, Abel-Bey A, et al. Tailored approaches to stroke health education (TASHE): study protocol for a randomized controlled trial. Trials. 2015;16(1):176.
Williams O, Leighton-Herrmann E, DeSorbo A, et al. Effect of two 12-minute culturally targeted films on intent to call 911 for stroke. Neurology. 2016;86(21):1992–5.
FACTANK: A record 60.6 million Americans live in multigenerational households [http://www.pewresearch.org/fact-tank/2016/08/11/a-record-60-6-million-americans-live-in-multigenerational-households/]
Williams O, DeSorbo A, Noble J, Gerin W. Child-mediated stroke communication. Stroke. 2012;43(1):163–9.
Shigehatake Y, Yokota C, Amano T, et al. Stroke education using an animated cartoon and a manga for junior high school students. J Stroke Cerebrovasc Dis. 2014;23(6):1623–7.
Amano T, Yokota C, Sakamoto Y, et al. Stroke education program of act FAST for junior high school students and their parents. J Stroke Cerebrovasc Dis. 2014;23(5):1040–5.
Sakamoto Y, Yokota C, Miyashita F, et al. Effects of stroke education using an animated cartoon and a manga on elementary school children. J Stroke Cerebrovasc Dis. 2014;23(7):1877–81.
Marto JP, Borbinha C, Filipe R, Calado S, Viana-Baptista M. Impact of stroke education on middle school students and their parents: a cluster randomized trial. Int J Stroke. 2017;12(4):401–11.
Sharkey S, Denke L, Herbert MA. Using puppets to teach schoolchildren to detect stroke and call 911. J Sch Nurs. 2016;32(4):228–33.
Williams O, Noble JM. Hip-Hop’ Stroke. Stroke. 2008;39(10):2809–16.
Williams O, Hecht MF, DeSorbo AL, Huq S, Noble JM. Effect of a novel video game on stroke knowledge of 9- to 10-year-old, low-income children. Stroke. 2014;45(3):889–92.
Williams O, Leighton-Herrmann E, DeSorbo A, et al: Hip hop stroke: study protocol for a randomized controlled trial to address stroke literacy. J Clin Trials 2015, 5(5).
Matsuzono K, Yokota C, Takekawa H, et al. Effects of stroke education of junior high school students on stroke knowledge of their parents. Stroke. 2015;46(2):572–4.
Williams LS, Bruno A, Rouch D, Marriott DJ, MAS DJ. Stroke patients’ knowledge of stroke: influence on time to presentation. Stroke. 1997;28(5):912–5.
Fussman C, Rafferty AP, Lyon-Callo S, Morgenstern LB, Reeves MJ. Lack of association between stroke symptom knowledge and intent to call 911. Stroke. 2010;41(7):1501–7.
Dombrowski SU, Sniehotta FF, Mackintosh J, et al. Witness response at acute onset of stroke: a qualitative theory-guided study. PloS one. 2012;7(7):e39852.
Skolarus LE, Murphy JB. Zimmerman MA, et al: individual and community determinants of calling 911 for stroke among African Americans in an urban community. Circ: Cardiovasc Qual Outcome. 2013;6(3):278–83.
Nemeth LS, Jenkins C, Jauch EC, et al. A community-engaged assessment of barriers and facilitators to rapid stroke treatment. Res Nurs Health. 2016;39(6):438–48.
Mellon L. Stroke warning campaigns: delivering better patient outcomes? A systematic review. Patient related outcome measures. 2015;6:61.
Morgenstern LB, Staub L, Chan W, et al. Improving delivery of acute stroke therapy. Stroke. 2002;33(1):160–6.
•• Rasura M, Baldereschi M, Di Carlo A, et al. Effectiveness of public stroke educational interventions: a review. Eur J Neurol. 2014;21(1):11–20. Narrative synthesis of public education interventions which suggests the importance of community interventions and e-health.
Beal CC, Flanders SA, Bader SG. Can children reduce delayed hospital arrival for ischemic stroke?: A systematic review of school-based stroke education. J Neurosci Nurs. 2016;48(3):E2–E13.
•• Mellon L, Doyle F, Rohde D, Williams D, Hickey A. Stroke warning campaigns: delivering better patient outcomes? A systematic review. Patient related outcome measures 2015, 6:61. A systematic review of stroke waning campaigns that demonstrated the positive effects of most studies. However, there were methodological limitations.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Kathleen M. Kelly, Kathryn T. Holt, Gina M. Neshewat, and Lesli E. Skolarus declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Cardiovascular Disease and Stroke
Rights and permissions
About this article
Cite this article
Kelly, K.M., Holt, K.T., Neshewat, G.M. et al. Community Interventions to Increase Stroke Preparedness and Acute Stroke Treatment Rates. Curr Atheroscler Rep 19, 64 (2017). https://doi.org/10.1007/s11883-017-0695-5
Published:
DOI: https://doi.org/10.1007/s11883-017-0695-5