Abstract
Background and Aims
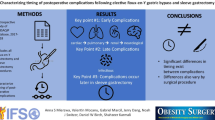
Clostridium difficile infection (CDI) is major health care concern with reports linking it to obesity. Our aim was to investigate the little known impact of the two most common bariatric surgeries, Roux-en-Y gastric bypass (RYGB) and vertical sleeve gastrectomy (VSG), on risk of CDI admissions.
Methods
This is a retrospective cohort study using the 2013 Nationwide Readmission Database. We examined inpatient CDI rates within 120 days after RYGB (n = 40,059) and VSG (n = 45,394). In a time to event analysis we also evaluated inpatient CDI rates up to 11 months post-surgery. We chose morbidly obese patients that underwent non-emergent ventral hernia repair (VHR) as additional surgical controls (n = 9673).
Result
CDI rates were higher after RYGB than VSG in the first 30 days (odds ratio [OR] = 2.10; 95% confidence interval [CI], 1.05–4.20) with a similar but nonsignificant trend within 31–120 days. CDI rates were also higher after RYGB compared to VHR controls within 31–120 days after surgery (OR = 3.22, 95%CI: 1.31, 7.88, p = 0.01). In a time to event analysis with up to 11 months follow up, RYGB led to higher CDI compared to VSG (hazard ratio [HR] = 1.87; 95% CI, 1.12–3.13) with a trend towards higher CDI compared to VHR (HR = 1.95; 95% CI, 0.94–4.06). Similar CDI rates occurred after VSG vs VHR.
Conclusions
RYGB may increase the risk of CDI hospitalization when compared to VSG and VHR controls. This data suggest VSG may be a better bariatric choice when post-surgical CDI risk is a concern.

Similar content being viewed by others
Abbreviations
- AHA:
-
Americans Heart Association
- AHRQ:
-
Agency for Healthcare Research and Quality
- CDI:
-
Clostridium Difficile infection
- CI:
-
Confidence Interval
- HCUP:
-
Healthcare Cost and Utilization Project
- HR:
-
Hazard ratio
- ICD-9-CM:
-
International Classification of Diseases, Ninth Revision, Clinical Modification
- LOS:
-
Length of hospital stay
- NRD:
-
Nationwide Readmission Database
- OR:
-
Odds ratio
- PPI:
-
Proton pump inhibitors
- RYGB:
-
Roux-en-Y Gastric Bypass
- SID:
-
State Inpatient Databases
- VHR:
-
Ventral Hernia Repair
- VSG:
-
Vertical Sleeve Gastrectomy
References
To KB, Napolitan LM. Clostridium difficile infection: update on diagnosis, epidemiology, and treatment strategies. Surg Infect. 2014;15(5):490–502. https://doi.org/10.1089/sur.2013.186.
Tattevin P, Buffet-Bataillon S, Donnio PY, et al. Clostridium difficile infections: do we know the real dimensions of the problem? Int J Antimicrob Agents. 2013;42(Suppl):S36–40. https://doi.org/10.1016/j.ijantimicag.2013.04.009.
Lo Vecchio A, Zacur GM. Clostridium difficile infection: an update on epidemiology, risk factors, and therapeutic options. Curr Opin Gastroenterol. 2012;28(1):1–9. https://doi.org/10.1097/MOG.0b013e32834bc9a9.
Bloomfield LE, Riley TV. Epidemiology and risk factors for community-associated clostridium difficile infection: a narrative review. Infect Dis Ther. 2016;5(3):231–51. https://doi.org/10.1007/s40121-016-0117-y.
Rodríguez-Pardo D et al. Epidemiology of clostridium difficile Infection and risk factors for unfavorable clinical outcomes: results of a hospital-based study in Barcelona, Spain. J Clin Microbiol. 2013;51(5):1465–73. https://doi.org/10.1128/JCM.03352-12.
Deshpande A, Pasupuleti V, Thota P, et al. Community-associated clostridium difficile infection and antibiotics: a meta-analysis. J Antimicrob Chemother. 2013;68(9):1951–61. https://doi.org/10.1093/jac/dkt129.
Olsen MA, Young-Xu Y, Stwalley D, et al. The burden of clostridium difficile infection: estimates of the incidence of CDI from U.S. administrative databases. BMC Infect Dis. 2016;16(1):177. https://doi.org/10.1186/s12879-016-1501-7.
Punni E, Pula JL, Asslo F, et al. Is obesity a risk factor for Clostridium difficile infection? Obes Res Clin Pract. 2015;9(1):50–4. https://doi.org/10.1016/j.orcp.2013.12.007.
Madan R, Petri Jr WA. Role of obesity and adipose tissue-derived cytokine leptin during Clostridium difficile infection. Anaerobe. 2015;34:182–6. https://doi.org/10.1016/j.anaerobe.2014.12.009.
Tsai F, Coyle WJ. The microbiome and obesity: is obesity linked to our gut flora? Curr Gastroenterol Rep. 2009;11(4):307–13. https://doi.org/10.1007/s11894-009-0045-z.
Leung J, Burke B, Ford D, et al. Possible association between obesity and Clostridium difficile infection. Emerg Infect Dis. 2013;19(11):1791–8. https://doi.org/10.3201/eid1911.130618.
Bishara J, Farah R, Mograbi J, et al. Obesity as a risk factor for Clostridium Difficile infection. Clin Infect Dis. 2013;57(4):489–93. https://doi.org/10.1093/cid/cit280.
Nathanson BH, Higgins TL, McGee WT. The dangers of extreme body mass index values in patients with Clostridium difficile. Infection. 2017;45(6):787–93. https://doi.org/10.1007/s15010-017-1036-x.
Mulki R et al. Body mass index greater than 35 is associated with severe Clostridium Difficile infection. Aliment Pharmacol Ther. 2016;
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36. https://doi.org/10.1007/s11695-012-0864-0.
ASMBS estimates of bariatric surgeries. Accessed on 02/06/2017.
Puzziferri N, Roshek III TB, Mayo HG, et al. Long-term follow-up after bariatric surgery: a systematic review. JAMA. 2014;312(9):934–42. https://doi.org/10.1001/jama.2014.10706.
Vendrell J, Broch M, Vilarrasa N, et al. Resistin, adiponectin, ghrelin, leptin, and proinflammatory cytokines: relationships in obesity. Obes Res. 2004;12(6):962–71. https://doi.org/10.1038/oby.2004.118.
Laimer M, Ebenbichler CF, Kaser S, et al. Markers of chronic inflammation and obesity: a prospective study on the reversibility of this association in middle-aged women undergoing weight loss by surgical intervention. Int J Obes Relat Metab Disord. 2002;26(5):659–62. https://doi.org/10.1038/sj.ijo.0801970.
Tremaroli V, Karlsson F, Werling M, et al. Roux-en-Y gastric bypass and vertical banded gastroplasty induce long-term changes on the human gut microbiome contributing to fat mass regulation. Cell Metab. 2015;22(2):228–38. https://doi.org/10.1016/j.cmet.2015.07.009.
Anhe FF et al. The gut microbiota as a mediator of metabolic benefits after bariatric surgery. Can J Diabetes. 2017;41(4):439–47. https://doi.org/10.1016/j.jcjd.2017.02.002.
Ryan KK, Tremaroli V, Clemmensen C, et al. FXR is a molecular target for the effects of vertical sleeve gastrectomy. Nature. 2014;509(7499):183–8. https://doi.org/10.1038/nature13135.
Dubberke ER, Butler AM, Nyazee HA, et al. The impact of ICD-9-CM code rank order on the estimated prevalence of Clostridium difficile infections. Clin Infect Dis. 2011;53(1):20–5. https://doi.org/10.1093/cid/cir246.
Dubberke ER et al. ICD-9 codes and surveillance for Clostridium difficile-associated disease. Emerg Infect Dis. 2006;12(10):1576–9. https://doi.org/10.3201/eid1210.060016.
Ali M, Ananthakrishnan AN, Ahmad S, et al. Clostridium difficile infection in hospitalized liver transplant patients: a nationwide analysis. Liver Transpl. 2012;18(8):972–8. https://doi.org/10.1002/lt.23449.
Bajaj JS, Ananthakrishnan AN, Hafeezullah M, et al. Clostridium difficile is associated with poor outcomes in patients with cirrhosis: a national and tertiary center perspective. Am J Gastroenterol. 2010;105(1):106–13. https://doi.org/10.1038/ajg.2009.615.
Kassam Z, Cribb Fabersunne C, Smith MB, et al. Clostridium difficile associated risk of death score (CARDS): a novel severity score to predict mortality among hospitalised patients with C. difficile infection. Aliment Pharmacol Ther. 2016;43(6):725–33. https://doi.org/10.1111/apt.13546.
Mamic P, Heidenreich PA, Hedlin H, et al. Hospitalized patients with heart failure and common bacterial infections: a nationwide analysis of concomitant Clostridium difficile infection rates and in-hospital mortality. J Card Fail. 2016;22(11):891–900. https://doi.org/10.1016/j.cardfail.2016.06.005.
Flagg A, Koch CG, Schiltz N, et al. Analysis of Clostridium difficile infections after cardiac surgery: epidemiologic and economic implications from national data. J Thorac Cardiovasc Surg. 2014;148(5):2404–9. https://doi.org/10.1016/j.jtcvs.2014.04.017.
McDonald LC, Coignard B, Dubberke E, et al. Recommendations for surveillance of Clostridium difficile-associated disease. Infect Control Hosp Epidemiol. 2007;28(2):140–5. https://doi.org/10.1086/511798.
Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360(14):1418–28. https://doi.org/10.1056/NEJMsa0803563.
Southern WN, Rahmani R, Aroniadis O, et al. Post-surgical Clostridium difficile-associated diarrhea. Surgery. 2010;148(1):24–30. https://doi.org/10.1016/j.surg.2009.11.021.
Abdelsattar Z et al. The postoperative burden of hospital acquired clostridium difficile infection. Infect Control Hosp Epidemiol. 2015;36(1):40–6. https://doi.org/10.1017/ice.2014.8.
Renvall S, Niinikoski J, Aho AJ. Wound infections in abdominal surgery. A prospective study on 696 operations. Acta Chir Scand. 1980;146(1):25–30.
Brim RL, Miller FG. The potential benefit of the placebo effect in sham-controlled trials: implications for risk-benefit assessments and informed consent. J Med Ethics. 2013;39(11):703–7. https://doi.org/10.1136/medethics-2012-101045.
Swank DJ, Swank-Bordewijk SCG, Hop WCJ, et al. Laparoscopic adhesiolysis in patients with chronic abdominal pain: a blinded randomised controlled multi-centre trial. Lancet. 2003;361(9365):1247–51. https://doi.org/10.1016/S0140-6736(03)12979-0.
Roughead EE et al. Proton pump inhibitors and risk of Clostridium difficile infection: a multi-country study using sequence symmetry analysis. Expert Opin Drug Saf. 2016:1–7.
Young MT, Phelan MJ, Nguyen NT. A decade analysis of trends and outcomes of male vs female patients who underwent bariatric surgery. J Am Coll Surg. 2016;222(3):226–31. https://doi.org/10.1016/j.jamcollsurg.2015.11.033.
Simon KL, Frelich MJ, Gould JC, et al. Inpatient outcomes after elective versus non-elective ventral hernia repair. J Surg Res. 2015;198(2):305–10. https://doi.org/10.1016/j.jss.2015.03.073.
Pournaras DJ, Osborne A, Hawkins SC, et al. Remission of type 2 diabetes after gastric bypass and banding: mechanisms and 2 year outcomes. Ann Surg. 2010;252(6):966–71. https://doi.org/10.1097/SLA.0b013e3181efc49a.
Courcoulas AP, Christian NJ, Belle SH, et al. Weight change and health outcomes at 3 years after bariatric surgery among individuals with severe obesity. JAMA. 2013;310(22):2416–25. https://doi.org/10.1001/jama.2013.280928.
Maciejewski ML, Arterburn DE, van Scoyoc L, et al. Bariatric surgery and long-term durability of weight loss. JAMA Surg. 2016;151(11):1046–55. https://doi.org/10.1001/jamasurg.2016.2317.
Ward EK, Schuster DP, Stowers KH, et al. The effect of PPI use on human gut microbiota and weight loss in patients undergoing laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2014;24(9):1567–71. https://doi.org/10.1007/s11695-014-1275-1.
Sillakivi T, Suumann J, Kirsimägi U, et al. Plasma levels of gastric biomarkers in patients after bariatric surgery: biomarkers after bariatric surgery. Hepato-Gastroenterology. 2013;60(128):2129–32.
Morinigo R et al. Glucagon-like peptide-1, peptide YY, hunger, and satiety after gastric bypass surgery in morbidly obese subjects. J Clin Endocrinol Metab. 2006;91(5):1735–40. https://doi.org/10.1210/jc.2005-0904.
Smith CD, Herkes SB, Behrns KE, et al. Gastric acid secretion and vitamin B12 absorption after vertical Roux-en-Y gastric bypass for morbid obesity. Ann Surg. 1993;218(1):91–6. https://doi.org/10.1097/00000658-199307000-00014.
Author information
Authors and Affiliations
Contributions
Dr. Hussan was involved in conception, design, interpretation of data and the drafting and critical revision of the manuscript. Mr. Kyle Porter was involved in study design, performed the acquisition and the statistical analysis of the data and provided critical revision of the manuscript. The above authors had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Dr. Ugbarugba collected the institutional data and was involved in design, interpretation of data and critical revision of the manuscript. Drs. Bailey, Needleman, Noria, O’Donnell and Clinton were involved in design, interpretation of data and critical revision of the manuscript. All gave final approval of the submitted manuscript and take responsibility for the integrity of the work.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Statement of Informed Consent
NRD database is comprised of de-identified patient information and does not meet the criteria for human subject and as such did not need institutional Review Board (IRB) approval nor require any form of consenting process prior to analysis of the data. Our supplemental tertiary center analysis was a de-identified retrospective chart review that contained no identifiable information and required no informed consent. Thus, no identifying information is available in the article and no informed consent was obtained.
Statement of Human and Animal Right
For this type of study formal consent is not required.
Additional information
AWARD:
This research was presented as an oral at the American College of Gastroenterology (ACG) 2016 National Meeting and awarded the 2016 ACG Obesity Award for Best Scientific Paper.
Grant Support:
No financial support was utilized in the creation of this project.
Electronic supplementary material
ESM 1
(DOCX 96 kb)
Rights and permissions
About this article
Cite this article
Hussan, H., Ugbarugba, E., Bailey, M.T. et al. The Impact of Bariatric Surgery on Short Term Risk of Clostridium Difficile Admissions. OBES SURG 28, 2006–2013 (2018). https://doi.org/10.1007/s11695-018-3131-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3131-1