Abstract
Purpose
The gender differences in patients with obstructive sleep apnea (OSA) are not fully understood so far, as previous studies had conflicting results. No reports have addressed the differences in OSA between Chinese men and women. Therefore, the purpose of this study was to investigate the clinical and polysomnographic differences between Chinese men and women with OSA.
Methods
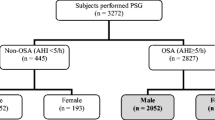
This case-paired control retrospective study included 580 consecutive Chinese patients (290 males and 290 females) newly diagnosed as OSA by overnight polysomnography from the Sleep Disorders Center of Tangdu Hospital affiliated to the Fourth Military Medical University of China. Demographic, clinical, and polysomnographic data of men and women with OSA were compared. Order logistic regression analysis was used to determine the risk factors for OSA severity.
Results
Male and female patients had similar age (57.3 ± 9.2 vs. 58.2 ± 8.9, p > 0.05) and body mass index (BMI) (25.4 ± 3.4 vs. 25.5 ± 3.9, p > 0.05). Women more commonly presented with insomnia (70.3% vs. 40.3%, p < 0.001), poor sleep quality (58.3% vs. 40.7%, p < 0.001), and headache on awakening (23.1% vs. 13.8%, p < 0.01) than men, while men more frequently reported habitual snoring (69.0% vs. 52.1%, p < 0.001) compared with women. The apnea–hypopnea index (AHI) during total sleep time and non-rapid eye movement sleep was higher in men compared with women (25.8 ± 20.4 vs. 19.3 ± 16.8; 22.0 ± 18.2 vs. 15.1 ± 15.4; p < 0.001, respectively), whereas AHI during rapid eye movement sleep was higher in women than in men (4.2 ± 3.6 vs. 3.7 ± 4.3, p < 0.01). Compared with men, women had lower sleep efficiency (75.4 ± 15.7 vs. 78.1 ± 15.5, p < 0.05), longer REM latency (128.9 ± 88.6 vs. 107.7 ± 72.4, p < 0.01), and greater wakefulness after sleep onset (WASO) (98.3 ± 70.2 vs. 88.0 ± 70.3, p < 0.05). No significant differences in the lowest oxygen desaturation and oxygen desaturation index (ODI) were observed between men and women (80.4 ± 10.8 vs. 80.8 ± 9.0; 17.0 ± 20.9 vs. 13.1 ± 16.5; p > 0.05, respectively). In addition, ordinal logistic regression analysis identified neck circumference as an independent risk factor for OSA severity in male patients (OR, 1.161; 95% CI, 1.020–1.325; p < 0.05) and in female patients (OR, 1.163; 95% CI, 1.013–1.338; p < 0.05).
Conclusions
Overall, female patients had less severe OSA when compared with male patients. The female patients more commonly reported “atypical” OSA symptoms, while male patients more frequently reported “typical” OSA symptoms. In clinical practices, physicians dealing with OSA need to take the gender disparity into consideration for more precise diagnosis and treatment, as women may be atypically symptomatic at a less severe OSA.


Similar content being viewed by others
References
Hnin K, Mukherjee S, Antic NA, Catcheside P, Chai-Coetzer CL, McEvoy D, Vakulin A (2018) The impact of ethnicity on the prevalence and severity of obstructive sleep apnea. Sleep Med Rev 41:78–86
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Bixler EO, Vgontzas AN, Lin HM, Ten Have T, Rein J, Vela-Bueno A et al (2001) Prevalence of sleep-disordered breathing in women: effects of gender. Am J Respir Crit Care Med 163:608–613
Kapsimalis F, Kryger MH (2002) Gender and obstructive sleep apnea syndrome, part 1: clinical features. Sleep 25:412–419
Hoffstein V, Szalai JP (1993) Predictive value of clinical features in diagnosing obstructive sleep apnea. Sleep 16:118–122
Vagiakis E, Kapsimalis F, Lagogianni I, Perraki H, Minaritzoglou A, Alexandropoulou K, Roussos C, Kryger M (2006) Gender differences on polysomnographic findings in Greek subjects with obstructive sleep apnea syndrome. Sleep Med 7:424–430
Mohsenin V (2001) Gender differences in the expression of sleep-disordered breathing: role of upper airway dimensions. Chest 120:1442–1447
Walker RP, Durazo-Arvizu R, Wachter B, Gopalsami C (2001) Preoperative differences between male and female patients with sleep apnea. Laryngoscope 111:1501–1505
Leech JA, Onal E, Dulberg C, Lopata MA (1988) A comparison of men and women with occlusive sleep apnea syndrome. Chest 94:983–988
O'Connor C, Thornley KS, Hanly PJ (2000) Gender differences in the polysomnographic features of obstructive sleep apnea. Am J Respir Crit Care Med 161:1465–1472
Ware JC, McBrayer RH, Scott JA (2000) Influence of sex and age on duration and frequency of sleep apnea events. Sleep 23:165–170
Bozkurt MK, Oy A, Aydin D, Bilen SH, Ertürk IO, Saydam L et al (2008) Gender differences in polysomnographic findings in Turkish patients with obstructive sleep apnea syndrome. Eur Arch Otorhinolaryngol 265:821–824
Alotair H, Bahammam A (2008) Gender differences in Saudi patients with obstructive sleep apnea. Sleep Breath 12:323–329
Yamakoshi S, Kasai T, Tomita Y, Takaya H, Kasagi S, Kawabata M, Narui K, Setoguchi Y (2016) Comparison of clinical features and polysomnographic findings between men and women with sleep apnea. J Thorac Dis 8:145–151
Leong WB, Arora T, Jenkinson D, Thomas A, Punamiya V, Banerjee D, Taheri S (2013) The prevalence and severity of obstructive sleep apnea in severe obesity: the impact of ethnicity. J Clin Sleep Med 9:853–858
Sutherland K, Lee RW, Cistulli PA (2012) Obesity and craniofacial structure as risk factors for obstructive sleep apnoea: impact of ethnicity. Respirology 17:213–222
Lee RW, Vasudavan S, Hui DS, Prvan T, Petocz P, Darendeliler MA et al (2010) Differences in craniofacial structures and obesity in Caucasian and Chinese patients with obstructive sleep apnea. Sleep 33:1075–1080
Miao J, Li H, Lin H, Su C, Liu Y, Lei G, Yang T, Li Z (2007) Severe sleep-disordered breathing in a patient with Brown-Vialetto-Van Laere syndrome: polysomnographic findings. J Neurol Sci 263:214–217
Su C, Miao J, Liu Y, Liu R, Lei G, Zhang W, Yang T, Li Z (2009) Multiple forms of rhythmic movements in an adolescent boy with rhythmic movement disorder. Clin Neurol Neurosurg 111:896–899
Liu Y, Su C, Liu R, Lei G, Zhang W, Yang T (2011) NREM-AHI greater than REM-AHI versus REM-AHI greater than NREM-AHI in patients with obstructive sleep apnea: clinical and polysomnographic features. Sleep Breath 15:463–470
Berry RB, Brooks R, Gamaldo CE, Harding SM, Marcus CL et al (2012) For the American Academy of Sleep Medicine. The AASM manual for the scoring of sleep and associated events: rules, terminology, and technical specifications. Version 2.0. American Academy of Sleep Medicine, Darien
Xu M, Yang Y, Zhang J (2013) Levels of neuroglobin in serum and neurocognitive impairments in Chinese patients with obstructive sleep apnea. Sleep Breath 17:573–582
Yu Q, Yin G, Zhang P, Song Z, Chen Y, Zhang D, Hu W (2014) Distinct associations between hypertension and obstructive sleep apnea in male and female patients. PLoS One 9:e113076
Stelmach-Mardas M, Mardas M, Iqbal K, Kostrzewska M, Piorunek T (2017) Dietary and cardio-metabolic risk factors in patients with obstructive sleep apnea: cross-sectional study. Peer J 5:e3259
Dancey DR, Hanly PJ, Soong C, Lee B, Shepard J Jr, Hoffstein V (2003) Gender differences in sleep apnea: the role of neck circumference. Chest 123:1544–1550
Quintana-Gallego E, Carmona-Bernal C, Capote F, Sánchez-Armengol A, Botebol-Benhamou G, Polo-Padillo J, Castillo-Gómez J (2004) Gender differences in obstructive sleep apnea syndrome: a clinical study of 1166 patients. Respir Med 98:984–989
Lin CM, Davidson TM, Ancoli-Israel S (2008) Gender differences in obstructive sleep apnea and treatment implications. Sleep Med Rev 12:481–496
Heinzer R, Marti-Soler H, Marques-Vidal P, Tobback N, Andries D, Waeber G, Preisig M, Vollenweider P, Haba-Rubio J (2018) Impact of sex and menopausal status on the prevalence, clinical presentation, and comorbidities of sleep-disordered breathing. Sleep Med 51:29–36
Smith R, Ronald J, Delaive K, Walld R, Manfreda J, Kryger MH (2002) What are obstructive sleep apnea patients being treated for prior to this diagnosis? Chest 121:164–172
Guilleminault C, Quera-Salva MA, Partinen M, Jamieson A (1988) Women and the obstructive sleep apnea syndrome. Chest 93:104–109
Dancey DR, Hanly PJ, Soong C, Lee B, Hoffstein V (2001) Impact of menopause on the prevalence and severity of sleep apnea. Chest 120:151–155
Young T, Finn L, Austin D, Peterson A (2003) Menopausal status and sleep-disordered breathing in the Wisconsin Sleep Cohort Study. Am J Respir Crit Care Med 167:1181–1185
Strohl KP, Redline S (1996) Recognition of obstructive sleep apnea. Am J Respir Crit Care Med 154:279–289
Vgontzas AN, Tan TL, Bixler EO, Martin LF, Shubert D, Kales A (1994) Sleep apnea and sleep disruption in obese patients. Arch Intern Med 154:1705–1711
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28:309–314
Ambrogetti A, Olson LG, Saunders NA (1991) Differences in the symptoms of men and women with obstructive sleep apnoea. Aust NZ J Med 21:863–866
Pillar G, Lavie P (1998) Psychiatric symptoms in sleep apnea syndrome: effects of gender and respiratory disturbance index. Chest 114:697–703
Ohayon M (1996) Epidemiological study on insomnia in the general population. Sleep 19:S7–S15
Acknowledgments
We thank Dr. Wangzhong Li (Department of Nasopharyngeal Carcinoma, Sun Yat-Sen University Cancer Center, China) for his supports with statistical analyses.
Funding
This study was funded in part by the National Natural Science Foundation of China (No. 81471111).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, Z., Cheng, J., Yang, W. et al. Gender differences in clinical manifestations and polysomnographic findings in Chinese patients with obstructive sleep apnea. Sleep Breath 24, 1019–1026 (2020). https://doi.org/10.1007/s11325-019-01943-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01943-y