Abstract
Background
Sleep is increasingly recognized as a potential risk for overweight and obesity. Observational studies have shown links between short sleep duration with weight gain. However, the findings from longitudinal studies in adults are conflicting. This review aimed to examine the effectiveness of experimental sleep restriction on adult body weight.
Method
A systematic search was undertaken in MEDLINE, EMBASE, PsycINFO, and CENTRAL (Cochrane center register of controlled trials) to identify experimental studies examining the effectiveness of sleep restriction on body weight, and search period was from January 2005 to June 2018. Meta-analysis was applied by using the random model.
Results
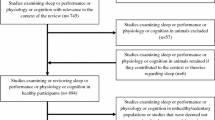
A total of 275 adults from six experimental studies were included. The pooled standard mean difference in body weight and body fat was 0.44 (95% CI − 0.13 to 1.02) (Z = 1.51, p > 0.05) and 0.35 kg (95% CI − 0.19 to 0.88) (Z = 1.27, p > 0.05), respectively. The experimental sleep restriction did not result in significant differences in adult body weight or body fat. Subgroup analysis showed that there were differences in weight gain between genders and races.
Conclusion
The finding from this review cannot support the hypothesis from observational studies that short sleep leads to weight gain.






Similar content being viewed by others
References
Grandner MA, Hale L, Moore M, Patel NP (2010) Mortality associated with short sleep duration: the evidence, the possible mechanisms, and the future. Sleep Med Rev 14:191–203
Altevogt BM, Colten, HR (Eds.) (2006) Sleep disorders and sleep deprivation: an unmet public health problem. National Academies Press
Wu Y, Zhai L, Zhang D (2014) Sleep duration and obesity among adults: a meta-analysis of prospective studies. Sleep Med 15(12):1456–1462
Matricciani L, Olds T, Petkov J (2012) In search of lost sleep: secular trends in the sleep time of school-aged children and adolescents. Sleep Med Rev 16(3):203–211
Taheri S (2006) The link between short sleep duration and obesity: we should recommend more sleep to prevent obesity. Arch Dis Child 91(11):881–884
Singh M, Drake CL, Roehrs T, Hudgel DW, Roth T (2005) The association between obesity and short sleep duration: a population-based study. J Clin Sleep Med 1(4):357–363
Chaput JP, Leblanc C, Pérusse L, Després JP, Bouchard C, Tremblay A (2009) Risk factors for adult overweight and obesity in the Quebec Family Study: have we been barking up the wrong tree? Obesity (Silver Spring) 17:1964–1970
Chaput JP, Tremblay A (2012) Insufficient sleep as a contributor to weight gain: an update. Curr Obes Rep 1(4):245–256
Koren D, Levitt Katz LE, Brar PC, Gallagher PR, Berkowitz RI, Brooks LJ (2011) Sleep architecture and glucose and insulin homeostasis in obese adolescents. Diabetes Care 34(11):2442–2447
Spiegel K, Tasali E, Leproult R, Van Cauter E (2009) Effects of poor and short sleep on glucose metabolism and obesity risk. Nat Rev Endocrinol 5(5):253–261
Taheri S, Lin L, Austin D, Young T, Mignot E (2004) Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Med 1(3):e62
Chen X, Beydoun MA, Wang Y (2008) Is sleep duration associated with childhood obesity? A systematic review and meta-analysis. Obesity 16(2):265–274
Cappuccio FP, Taggart FM, Kandala N, Currie A, Peile E, Stranges S, Miller MA (2008) Meta-analysis of short sleep duration and obesity in children and adults. Sleep 31(5):619–626
Patel SR, Malhotra A, White DP, Gottlieb DJ, Hu FB (2006) Association between reduced sleep and weight gain in women. Am J Epidemiol 164(10):947–954
Watanabe M, Kikuchi H, Tanaka K, Takahashi M (2010) Association of short sleep duration with weight gain and obesity at 1-year follow-up: a large-scale prospective study. Sleep 33(2):161–167
Fatima Y, Doi S, Mamun A (2015) Longitudinal impact of sleep on overweight and obesity in children and adolescents: a systematic review and bias-adjusted meta-analysis. Obes Rev 16(2):137–149
Thind H, Davies SL, Lewis T, Pekmezi D, Evans R, Baskin ML (2015) Does short sleep lead to obesity among children and adolescents? Current understanding and implications. Am J Lifestyle Med 9(6):428–437
Magee L, Hale L (2012) Longitudinal associations between sleep duration and subsequent weight gain: a systematic review. Sleep Med Rev 16(3):231–241
Yoong SL, Chai LK, Williams CM, Wiggers J, Finch M, Wolfenden L (2016) Systematic review and meta-analysis of interventions targeting sleep and their impact on child body mass index, diet, and physical activity. Obesity 24(5):1140–1147
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151:264–269
Mariela H (2012) RefWorks usage patterns: exploring the first four semesters of use by faculty, graduate students, and undergraduates. Internet Ref Serv Q 17(2):45–64
Higgins JP, Green S (Eds.) (2008) Cochrane handbook for systematic reviews of interventions
RevMan R (2014) The nordic cochrane centre, the cochrane collaboration
Borenstein M, Hedges LV, Higgins JP, Rothstein HR (2015) Biostat: comprehensive meta-analysis (version 3)[software]. Englewood: Biostat
Calvin AD, Covassin N, Kremers WK et al (2014) Experimental sleep restriction causes endothelial dysfunction in healthy humans. J Am Heart Assoc 3(6):e001143
Spaeth AM, Dinges DF, Goel N (2013) Effects of experimental sleep restriction on weight gain, caloric intake, and meal timing in healthy adults. Sleep 36(7):981–990
Wang X, Sparks JR, Bowyer KP, Youngstedt SD (2018) Influence of sleep restriction on weight loss outcomes associated with caloric restriction. Sleep 41(5):027
Nedeltcheva AV, Kilkus JM, Imperial J, Kasza K, Schoeller DA, Penev PD (2009) Sleep curtailment is accompanied by increased intake of calories from snacks. Am J Clin Nutr 89:126–133
Nedeltcheva AV, Kilkus JM, Imperial J, Schoeller DA, Penev PD (2010) Insufficient sleep undermines dietary efforts to reduce adiposity. Ann Intern Med 153(7):435–441
O’Keeffe M, Roberts AL, Kelleman M, RoyChoudhury A, St-Onge MP (2013) No effects of short-term sleep restriction, in a controlled feeding setting, on lipid profiles in normal-weight adults. Sleep 22:717–720
Hall KD, Heymsfield SB, Kemnitz JW, Klein S, Schoeller DA, Speakman JR (2012) Energy balance and its components: implications for body weight regulation. Am J Clin Nutr 95(4):989–994
Capers PL, Fobian AD, Kaiser KA, Borah R, Allison DB (2015) A systematic review and meta-analysis of randomized controlled trials of the impact of sleep duration on adiposity and components of energy balance. Obes Rev 16(9):771–782
Robertson MD, Russell-Jones D, Umpleby AM, Dijk DJ (2013) Effects of three weeks of mild sleep restriction implemented in the home environment on multiple metabolic and endocrine markers in healthy young men. Metabolism 62:204–211
Nielsen LS, Danielsen KV, Sorensen TI (2011) Short sleep duration as a possible cause of obesity: critical analysis of the epidemiological evidence. Obes Rev 12:78–92
Tan X, Alén M, Wang K, Tenhunen J, Wiklund P, Partinen M, Cheng S (2016) Effect of six-month diet intervention on sleep among overweight and obese men with chronic insomnia symptoms: a randomized controlled trial. Nutrients 8(11):751
Weinert W (2007) The circadian rhythm of core temperature: effects of physical activity and aging. Physiol Behav 90(2):246–256
McCambridge J, Witton J, Elbourne DR (2014) Systematic review of the Hawthorne effect: new concepts are needed to study research participation effects. J Clin Epidemiol 67(3):267–277
Cizza G, Piaggi P, Rother KI, Csako G, Sleep Extension Study Group (2014) Hawthorne effect with transient behavioral and biochemical changes in a randomized controlled sleep extension trial of chronically short-sleeping obese adults: implications for the design and interpretation of clinical studies. PLoS One 9(8):e104176
Spaeth AM, Dinges DF, Goel N (2014) Sex and race differences in caloric intake during sleep restriction in healthy adults. Am J Clin Nutr 100(2):559–566
Hu X, Lin S, Zhong W, Lin X (2013) Analysis of influencing factors of adult overweight and obesity in 5 national disease monitoring sites in Fujian province. Chin J Dis Control 17(01):20–23
Guansheng M, Dechun L, Ailing L, Yanping L, Chaohui C, Xiaoqi H (2007) Relationship between physical activity level and overweight and obesity in Chinese adult occupational population. Chinese Journal of Nutrition (5):426–430
Van Cauter E, Leproult R, Plat L (2000) Age-related changes in slow wave sleep and REM sleep and relationship with growth hormone and cortisol levels in healthy men. Jama 284(7):861–868
Ohayon MM, Carskadon MA, Guilleminault C, Vitiello MV (2004) Meta-analysis of quantitative sleep parameters from childhood to old age in healthy individuals: developing normative sleep values across the human lifespan. Sleep 27(7):1255–1273
Dijk DJ, Duffy JF (1999) Circadian regulation of human sleep and age-related changes in its timing, consolidation and EEG characteristics. Ann Med 31(2):130–140
Funding
The work was supported by the grant from the Ministry of Education’s Humanities and Social Sciences Research Project (No. 18YJA630015).
Author information
Authors and Affiliations
Contributions
All reviewers entered every step to ensure the security and completeness of the data, if there was a disagreement, discussing together or assessing by the third reviewer to resolve.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Date sharing statement
No additional data are available.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix 1: search strategy used in the Ovid MEDLINE January 2005–June 2018
-
1.
adult$.tw (969812)
-
2.
female$.tw (723552)
-
3.
male$.tw (893686)
-
4.
m?n.tw (1261299)
-
5.
wom?n.tw (923021)
-
6.
or/ 1–5 (3660745)
-
7.
sleep$.tw (138539)
-
8.
(sleep adj3 duration$).tw (6304)
-
9.
(sleep$ adj3 tim$).tw (10550)
-
10.
(bedtime or bed tim$ or time in bed).tw (4974)
-
11.
(sleep$ adj3 hour$).tw (3771)
-
12.
night rest.tw (53)
-
13.
or/7–12 (141267)
-
14.
randomi?ed.tw (471727)
-
15.
non randomi?ed.tw (8828)
-
16.
clinical trial.tw (101372)
-
17.
randomi?ed controlled trial.pt (467664)
-
18.
controlled clinical trial.pt (92598)
-
19.
experiment$ study.tw (1523737)
-
20.
(pre-post or prepost or pre post).tw (6905)
-
21.
(posttest or post test).tw (14669)
-
22.
(pretest or pretest).tw (13928)
-
23.
before after.tw (3683)
-
24.
(qua?i-randomi?ed or qua?irandomi?ed).tw (3589)
-
25.
quasiexperimental study.tw (125)
-
26.
or/14–25 (2281151)
-
27.
weight (914152)
-
28.
exp weight loss/ (37322)
-
29.
(weight loss$ or weight-loss$).tw (66114)
-
30.
(weight adj3 reduc$).tw (27861)
-
31.
exp BMI/ (101940)
-
32.
exp body mass index/ (11048)
-
33.
or/ 27–32 (978486)
-
34.
apn?ea.ti (20146)
-
35.
sleep apn?ea.ti (17399)
-
36.
study protocol.ti (5120)
-
37.
(sleep$ adj1 disorder$).ti (5190)
-
38.
OSA.ti (614)
-
39.
or/34–38 (28061)
-
40.
6 AND 13 AND 26 AND 33 NOT 39 (337)
Appendix 2: data extraction form
Administration details | ||||
|---|---|---|---|---|
Study ID (last name of the first author and publication date) | ||||
Title of the article | ||||
Country | ||||
Language | ||||
Study details | ||||
Aim of the study | ||||
Study design | ||||
Setting of the study | ||||
Duration of the study | ||||
Methods | ||||
Randomization | ||||
Allocation | ||||
Blinding | ||||
Notes | ||||
Participants characteristics | ||||
Patient baseline characteristics | Total | Intervention group | Control (no supplement) | Difference between the groups |
Number randomized | ||||
Number analyzed | ||||
Age | ||||
Gender (M/F), n (%) | ||||
Weight measure | ||||
BMI level | ||||
Interventions/comparators | ||||
Intervention type | ||||
Intervention description | ||||
Who delivered the intervention | ||||
Who else also involved the intervention? | ||||
Control description | ||||
Follow-up | ||||
Duration of the intervention | ||||
Numbers of participants dropped out of the study (%) | Original number | Final number | Reasons | |
Time of follow-up | ||||
Numbers of participants dropped out during follow-up (%) | Original number | Final number | Reasons | |
Outcome measure and assessment | ||||
Outcome measure method | Details: | |||
Outcome evaluation method | Self-report or observed measure | Details | ||
Outcome effect Mean change difference with 95% CI | Intervention group | Control group | ||
Analyzed participants number (total) | Mean change (95% CI) | Analyzed participants number (total) | Mean change (95% CI) | |
Comments: | ||||
Rights and permissions
About this article
Cite this article
Yu, H., Lu, J., Jia, P. et al. Experimental sleep restriction effect on adult body weight: a meta-analysis. Sleep Breath 23, 1341–1350 (2019). https://doi.org/10.1007/s11325-019-01828-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01828-0