Abstract
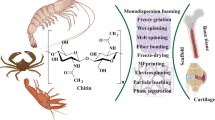
Successful tissue engineering with the aid of a polymer scaffold offers the possibility to produce a larger construct and to mould the shape after the defect. We investigated the use of cryogelation to form protein-based scaffolds through different types of formation mechanisms; enzymatic crosslinking, chemical crosslinking, and non-covalent interactions. Casein was found to best suited for enzymatic crosslinking, gelatin for chemical crosslinking, and ovalbumin for non-covalent interactions. Fibroblasts and myoblasts were used to evaluate the cryogels for tissue engineering purposes. The stability of the cryogels over time in culture differed depending on formation mechanism. Casein cryogels showed best potential to be used in skeletal tissue engineering, whereas gelatin cryogels would be more suitable for compliable soft tissues even though it also seemed to support a myogenic phenotype. Ovalbumin cryogels would be better suited for elastic tissues with faster regeneration properties due to its faster degradation time. Overall, the cryogelation technique offers a fast, cheap and reproducible way of creating porous scaffolds from proteins without the use of toxic compounds.






Similar content being viewed by others
References
Shimizu K, Fujita H, Nagamori E. Alignment of skeletal muscle myoblasts and myotubes using linear micropatterned surfaces ground with abrasives. Biotechnol Bioeng. 2009;103(3):631–8.
Yan W, et al. Tissue engineering of skeletal muscle. Tissue Eng. 2007;13(11):2781–90.
Bian W, Bursac N. Engineered skeletal muscle tissue networks with controllable architecture. Biomaterials. 2009;30(7):1401–13.
Liao H, Zhou GQ. Development and progress of engineering of skeletal muscle tissue. Tissue Eng B Rev. 2009;15(3):319–31.
Okano T, Matsuda T. Hybrid muscular tissues: preparation of skeletal muscle cell-incorporated collagen gels. Cell Transplant. 1997;6(2):109–18.
Gilmore KJ, et al. Skeletal muscle cell proliferation and differentiation on polypyrrole substrates doped with extracellular matrix components. Biomaterials. 2009;30(29):5292–304.
Gomes ME, Malafaya PB and Reis RL. In: Hollander AP and Hatton PV, editors. Methodologies for processing biodegradable and natural origin scaffolds for bone and cartilage tissue-engineering applications, in biopolymer methods in tissue engineering. Totowa: Humana Press Inc; 2004. p. 65–77.
Lv S, et al. Designed biomaterials to mimic the mechanical properties of muscles. Nature. 2010;465(7294):69–73.
Langer R, Tirrell DA. Designing materials for biology and medicine. Nature. 2004;428(6982):487–92.
Brandl F, Sommer F, Goepferich A. Rational design of hydrogels for tissue engineering: impact of physical factors on cell behavior. Biomaterials. 2007;28(2):134–46.
Levy-Mishali M, Zoldan J, Levenberg S. Effect of scaffold stiffness on myoblast differentiation. Tissue Eng Part A. 2009;15(4):935–44.
Bölgen N, et al. Three-dimensional ingrowth of bone cells within biodegradable cryogel scaffolds in bioreactors at different regimes. Tissue Eng Part A. 2008;14(10):1743–50.
Dainiak MB, et al. Gelatin-fibrinogen cryogel dermal matrices for wound repair: preparation, optimisation and in vitro study. Biomaterials. 2010;31(1):67–76.
Singh D, Nayak V, Kumar A. Proliferation of myoblast skeletal cells on three-dimensional supermacroporous cryogels. Int J Biol Sci. 2010;6(4):371–81.
Singh D, et al. Proliferation of chondrocytes on a 3-d modelled macroporous poly(hydroxyethyl methacrylate)-gelatin cryogel. J Biomater Sci Polym Ed. 2011;22(13):1733–51.
Srivastava A, Kumar A. Thermoresponsive poly(N-vinylcaprolactam) cryogels: synthesis and its biophysical evaluation for tissue engineering applications. J Mater Sci Mater Med. 2010;21(11):2937–45.
Lozinsky VI. Cryogels on the basis of natural and synthetic polymers: preparation, properties and application. Russ Chem Rev. 2002;71(6):559–85.
Lozinsky VI, et al. Polymeric cryogels as promising materials of biotechnological interest. Trends Biotechnol. 2003;21(10):445–51.
Bölgen N, et al. Cryogelation for preparation of novel biodegradable tissue-engineering scaffolds. J Biomater Sci Polym Ed. 2007;18(9):1165–79.
Myllarinen P, Buchert J, Autio K. Effect of transglutaminase on rheological properties and microstructure of chemically acidified sodium caseinate gels. Int Dairy J. 2007;17(7):800–7.
Nonaka M, et al. Sodium caseinate and skim milk gels formed by incubation with microbial transglutaminase. J Food Sci. 1992;57:1214–41.
Jurga M, et al. The performance of laminin-containing cryogel scaffolds in neural tissue regeneration. Biomaterials. 2011;32(13):3423–34.
Gawlik K, et al. Laminin alpha 1 chain reduces muscular dystrophy in laminin alpha 2 chain deficient mice. Hum Mol Genet. 2004;13(16):1775–84.
Hager M, et al. Laminin {alpha}1 chain corrects male infertility caused by absence of laminin {alpha}2 chain. Am J Pathol. 2005;167(3):823–33.
Mayer U. Integrins: Redundant or important players in skeletal muscle? J Biol Chem. 2003;278(17):14587–90.
Wolfe J, Bryant G, Koster KL. What is ‘unfreezable water’, how unfreezable is it and how much is there? Cryoletters. 2002;23:157–66.
Konstantinova NR, Lozinsky VI. Cryotropic gelation of ovalbumin solutions. Food Hydrocoll. 1997;11(2):113–23.
Kirsebom H, et al. Modulating the porosity of cryogels by influencing the nonfrozen liquid phase through the addition of inert solutes. Langmuir. 2010;26(20):16129–33.
Kathuria N, et al. Synthesis and characterization of elastic and macroporous chitosan–gelatin cryogels for tissue engineering. Acta Biomater. 2009;5(1):406–18.
O’Brien FJ, et al. The effect of pore size on cell adhesion in collagen-GAG scaffolds. Biomaterials. 2005;26(4):433–41.
Salem AK, et al. Interactions of 3T3 fibroblasts and endothelial cells with defined pore features. J Biomed Mater Res. 2002;61(2):212–7.
Laminins DM. Cell Tissue Res. 2010;339(1):259–68.
Schuler F, Sorokin LM. Expression of laminin isoforms in mouse myogenic cells in vitro and in vivo. J Cell Sci. 1995;108:3795–805.
González-Ramírez R, et al. Nuclear and nuclear envelope localization of dystrophin Dp71 and dystrophin-associated proteins (DAPs) in the C2C12 muscle cells: dAPs nuclear localization is modulated during myogenesis. J Cell Biochem. 2008;105(3):735–45.
Yokoyama K, Nio N, Kikuchi Y. Properties and applications of microbial transglutaminase. Appl Microbiol Biotechnol. 2004;64(4):447–54.
Stein PE, et al. Crystal structure of ovalbumin as a model for the reactive centre of serpins. Nature. 1990;347(6288):99–102.
Ren K, et al. Manipulation of the adhesive behaviour of skeletal muscle cells on soft and stiff polyelectrolyte multilayers. Acta Biomater. 2010;6(11):4238–48.
Acknowledgments
The authors thank R. Wallén for help with sample preparation and assistance at the scanning electron microscope. Ajinomoto, T. Sasaki and U. Mayer for gifts of reagents. This study was financially supported by the Swedish Research Council (VR).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Elowsson, L., Kirsebom, H., Carmignac, V. et al. Porous protein-based scaffolds prepared through freezing as potential scaffolds for tissue engineering. J Mater Sci: Mater Med 23, 2489–2498 (2012). https://doi.org/10.1007/s10856-012-4713-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10856-012-4713-4