Abstract
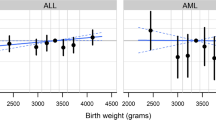
Infectious etiologies have been hypothesized for acute leukemias because of their high incidence in early childhood, but have seldom been examined for acute myeloid leukemia (AML). We conducted the first large cohort study to examine perinatal factors including season of birth, a proxy for perinatal infectious exposures, and risk of AML in childhood through young adulthood. A national cohort of 3,569,333 persons without Down syndrome who were born in Sweden in 1973–2008 were followed up for AML incidence through 2010 (maximum age 38 years). There were 315 AML cases in 69.7 million person-years of follow-up. We found a sinusoidal pattern in AML risk by season of birth (P < 0.001), with peak risk among persons born in winter. Relative to persons born in summer (June–August), incidence rate ratios for AML were 1.72 (95 % CI 1.25–2.38; P = 0.001) for winter (December–February), 1.37 (95 % CI 0.99–1.90; P = 0.06) for spring (March–May), and 1.27 (95 % CI 0.90–1.80; P = 0.17) for fall (September–November). Other risk factors for AML included high fetal growth, high gestational age at birth, and low maternal education level. These findings did not vary by sex or age at diagnosis. Sex, birth order, parental age, and parental country of birth were not associated with AML. In this large cohort study, birth in winter was associated with increased risk of AML in childhood through young adulthood, possibly related to immunologic effects of early infectious exposures compared with summer birth. These findings warrant further investigation of the role of seasonally varying perinatal exposures in the etiology of AML.

Similar content being viewed by others
Abbreviations
- ALL:
-
Acute lymphoblastic leukemia
- AML:
-
Acute myeloid leukemia
- CI:
-
Confidence interval
- DOB:
-
Date of birth
- ICD:
-
International classification of diseases
- IRR:
-
Incidence rate ratio
- SD:
-
Standard deviation
References
Linabery AM, Ross JA. Trends in childhood cancer incidence in the U.S. (1992–2004). Cancer. 2008;112(2):416–32. doi:10.1002/cncr.23169.
Eden T. Aetiology of childhood leukaemia. Cancer Treat Rev. 2010;36(4):286–97. doi:10.1016/j.ctrv.2010.02.004.
Kaatsch P. Epidemiology of childhood cancer. Cancer Treat Rev. 2010;36(4):277–85. doi:10.1016/j.ctrv.2010.02.003.
Deschler B, Lubbert M. Acute myeloid leukemia: epidemiology and etiology. Cancer. 2006;107(9):2099–107. doi:10.1002/cncr.22233.
Doll R, Wakeford R. Risk of childhood cancer from fetal irradiation. Br J Radiol. 1997;70:130–9. doi:10.1259/bjr.70.830.9135438.
Bruwier A, Chantrain CF. Hematological disorders and leukemia in children with down syndrome. Eur J Pediatr. 2012;171(9):1301–7. doi:10.1007/s00431-011-1624-1.
Cnattingius S, Zack M, Ekbom A, Gunnarskog J, Linet M, Adami HO. Prenatal and neonatal risk factors for childhood myeloid leukemia. Cancer Epidemiol Biomarkers Prev Publ Am Assoc Cancer Res Cosponsored Am Soc Prev Oncol. 1995;4(5):441–5.
Pui CH. Childhood leukemias. New Engl J Med. 1995;332(24):1618–30. doi:10.1056/NEJM199506153322407.
McNally RJ, Eden TO. An infectious aetiology for childhood acute leukaemia: a review of the evidence. Br J Haematol. 2004;127(3):243–63. doi:10.1111/j.1365-2141.2004.05166.x.
Greaves M. Childhood leukaemia. BMJ. 2002;324(7332):283–7.
Basta NO, James PW, Craft AW, McNally RJ. Season of birth and diagnosis for childhood cancer in Northern England, 1968-2005. Paediatr Perinat Epidemiol. 2010;24(3):309–18. doi:10.1111/j.1365-3016.2010.01112.x.
Feltbower RG, Pearce MS, Dickinson HO, Parker L, McKinney PA. Seasonality of birth for cancer in Northern England, UK. Paediatric Perinatal Epidemiol. 2001;15(4):338–45.
Sorensen HT, Pedersen L, Olsen J, Rothman K. Seasonal variation in month of birth and diagnosis of early childhood acute lymphoblastic leukemia. JAMA J Am Med Assoc. 2001;285(2):168–9.
Yaniv I, Lewy H, Avrahami G, Jeison M, Stark B, Laron Z. Possible link between month of birth and childhood leukemia supports the hypothesis of an infectious etiology. Israel Med Assoc J IMAJ. 2010;12(12):776.
Nyari TA, Kajtar P, Bartyik K, Thurzo L, McNally R, Parker L. Seasonal variation of childhood acute lymphoblastic leukaemia is different between girls and boys. Pathol Oncol Res POR. 2008;14(4):423–8. doi:10.1007/s12253-008-9017-0.
Kajtar P, Fazekasne KM, Mehes K. Month of birth in childhood acute lymphoblastic leukemia. Orv Hetil. 2003;144(38):1869–71.
Meltzer AA, Annegers JF, Spitz MR. Month-of-birth and incidence of acute lymphoblastic leukemia in children. Leukemia Lymphoma. 1996;23(1–2):85–92. doi:10.3109/10428199609054805.
Higgins CD, Dos Santos-Silva I, Stiller CA, Swerdlow AJ. Season of birth and diagnosis of children with leukaemia: an analysis of over 15 000 UK cases occurring from 1953–95. Br J Cancer. 2001;84(3):406–12. doi:10.1054/bjoc.2000.1575.
Marsal K, Persson PH, Larsen T, Lilja H, Selbing A, Sultan B. Intrauterine growth curves based on ultrasonically estimated foetal weights. Acta Paediatr. 1996;85(7):843–8.
Steliarova-Foucher E, Stiller C, Lacour B, Kaatsch P. International classification of childhood cancer, third edition. Cancer. 2005;103(7):1457–67. doi:10.1002/cncr.20910.
Crump C, Sundquist K, Sundquist J, Winkleby MA. Gestational age at birth and mortality in young adulthood. JAMA J Am Med Assoc. 2011;306(11):1233–40.
Zou G. A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159(7):702–6.
Efird JT, Nielsen SS. A method to model season of birth as a surrogate environmental risk factor for disease. Int J Env Res Public Health. 2008;5(1):49–53.
StataCorp. Stata statistical software: release 13. College Station, TX: StataCorp LP; 2013.
van Laar M, Kinsey SE, Picton SV, Feltbower RG. First description of seasonality of birth and diagnosis amongst teenagers and young adults with cancer aged 15–24 years in England, 1996–2005. BMC Cancer. 2013;13:365. doi:10.1186/1471-2407-13-365.
Naumburg E, Bellocco R, Cnattingius S, Jonzon A, Ekbom A. Perinatal exposure to infection and risk of childhood leukemia. Med Pediatr Oncol. 2002;38(6):391–7. doi:10.1002/mpo.10084.
Crump C, Sundquist J, Sieh W, Winkleby MA, Sundquist K. Season of birth and risk of Hodgkin and non-Hodgkin lymphoma. Int J Cancer. 2014;. doi:10.1002/ijc.28909.
Savitz DA, Andrews KW. Review of epidemiologic evidence on benzene and lymphatic and hematopoietic cancers. Am J Ind Med. 1997;31(3):287–95.
Pui CH, Ribeiro RC, Hancock ML, et al. Acute myeloid leukemia in children treated with epipodophyllotoxins for acute lymphoblastic leukemia. New Engl J Med. 1991;325(24):1682–7. doi:10.1056/NEJM199112123252402.
Ben-David Y, Bernstein A. Friend virus-induced erythroleukemia and the multistage nature of cancer. Cell. 1991;66(5):831–4.
Kerr JR, Barah F, Cunniffe VS, et al. Association of acute parvovirus B19 infection with new onset of acute lymphoblastic and myeloblastic leukaemia. J Clin Pathol. 2003;56(11):873–5.
Caughey RW, Michels KB. Birth weight and childhood leukemia: a meta-analysis and review of the current evidence. Int J Cancer. 2009;124(11):2658–70. doi:10.1002/ijc.24225.
O’Neill KA, Murphy MF, Bunch KJ, et al. Infant birthweight and risk of childhood cancer: international population-based case control studies of 40 000 cases. Int J Epidemiol. 2015;44(1):153–68. doi:10.1093/ije/dyu265.
Crump C, Sundquist K, Sieh W, Winkleby MA, Sundquist J. Perinatal and family risk factors for Hodgkin lymphoma in childhood through young adulthood. Am J Epidemiol. 2012;176(12):1147–58. doi:10.1093/aje/kws212.
Crump C, Sundquist K, Sieh W, Winkleby MA, Sundquist J. Perinatal and family risk factors for non-Hodgkin lymphoma in early life: a Swedish national cohort study. J Natl Cancer Inst. 2012;104(12):923–30. doi:10.1093/jnci/djs225.
Hjalgrim LL, Westergaard T, Rostgaard K, et al. Birth weight as a risk factor for childhood leukemia: a meta-analysis of 18 epidemiologic studies. Am J Epidemiol. 2003;158(8):724–35.
Pollak MN, Schernhammer ES, Hankinson SE. Insulin-like growth factors and neoplasia. Nat Rev Cancer. 2004;4(7):505–18. doi:10.1038/nrc1387nrc1387.
Tower RL, Spector LG. The epidemiology of childhood leukemia with a focus on birth weight and diet. Crit Rev Clin Lab Sci. 2007;44(3):203–42. doi:10.1080/10408360601147536.
McLaughlin CC, Baptiste MS, Schymura MJ, Nasca PC, Zdeb MS. Birth weight, maternal weight and childhood leukaemia. Br J Cancer. 2006;94(11):1738–44. doi:10.1038/sj.bjc.6603173.
Hjalgrim LL, Rostgaard K, Hjalgrim H, et al. Birth weight and risk for childhood leukemia in Denmark, Sweden, Norway, and Iceland. J Natl Cancer Inst. 2004;96(20):1549–56. doi:10.1093/jnci/djh287.
Johnson KJ, Soler JT, Puumala SE, Ross JA, Spector LG. Parental and infant characteristics and childhood leukemia in Minnesota. BMC Pediatr. 2008;8:7. doi:10.1186/1471-2431-8-7.
Reynolds P, Von Behren J, Elkin EP. Birth characteristics and leukemia in young children. Am J Epidemiol. 2002;155(7):603–13.
Ma X, Metayer C, Does MB, Buffler PA. Maternal pregnancy loss, birth characteristics, and childhood leukemia (United States). Cancer Causes Control CCC. 2005;16(9):1075–83. doi:10.1007/s10552-005-0356-9.
Rudant J, Orsi L, Monnereau A, et al. Childhood hodgkin’s lymphoma, non-Hodgkin’s lymphoma and factors related to the immune system: the escale study (SFCE). Int J Cancer. 2010;. doi:10.1002/ijc.25862.
Johnson KJ, Carozza SE, Chow EJ, et al. Parental age and risk of childhood cancer: a pooled analysis. Epidemiology. 2009;20(4):475–83. doi:10.1097/EDE.0b013e3181a5a332.
Zack M, Adami HO, Ericson A. Maternal and perinatal risk factors for childhood leukemia. Cancer Res. 1991;51(14):3696–701.
Shu XO, Gao YT, Brinton LA, et al. A population-based case-control study of childhood leukemia in Shanghai. Cancer. 1988;62(3):635–44.
Westergaard T, Andersen PK, Pedersen JB, et al. Birth characteristics, sibling patterns, and acute leukemia risk in childhood: a population-based cohort study. J Natl Cancer Inst. 1997;89(13):939–47.
Centre for Epidemiology. The swedish medical birth registry–a summary of content and quality. Stockholm: The National Board of Health and Welfare; 2003.
Centre for Epidemiology. Cancer incidence in Sweden 2011. Stockholm: The National Board of Health and Welfare; 2011.
Acknowledgments
This work was supported by the National Cancer Institute at the National Institutes of Health [grant number R03 CA171017]; the Swedish Research Council; and ALF project grant, Region Skåne/Lund University, Sweden. The funding agencies had no role in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, or approval of the manuscript. There were no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Crump, C., Sundquist, J., Sieh, W. et al. Perinatal risk factors for acute myeloid leukemia. Eur J Epidemiol 30, 1277–1285 (2015). https://doi.org/10.1007/s10654-015-0063-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-015-0063-0