Summary
Melanoma is one of the most common cancers, and its incidence has continued to increase over the past few decades. Chemotherapy resistance and related defects in apoptotic signaling are critical for the high mortality of melanoma. Effective drugs are lacking because apoptosis regulation in this tumor type is not well understood. The folate pathway has been considered an interesting target for anticancer therapies, and approaches targeting this pathway have recently been extended to melanoma treatment. In this study, the intracellular apoptosis signaling pathways of two melanoma cells lines (SK-MEL-2 and SK-MEL-28) were investigated after treatment with a new experimental antifolate substance (MR36) that targets thymidylate synthase. In both melanoma cell lines, apoptosis induction was triggered by a p53-independent mechanism. MR36-induced apoptosis was associated with a loss of both mitochondrial membrane potential and caspase-3 activation. Induction of cell cycle arrest by MR36 was associated with changes in the expression of key cell cycle regulators, such as p21 and cyclin D1, and the hypophosphorylation of pRb. In addition, Fas signaling was also analyzed. These findings suggest that, unlike classical antifolates, MR36 exerted an inhibitory effect on both the enzymatic function and expression of thymidylate synthase, thereby inducing apoptosis through the activation of the extrinsic and intrinsic pathways in the melanoma cell lines. MR36 showed a different mechanism of action from the known antifolates (Nolatrexed and Pemetrexed) that resulted in higher anticancer activity. Therefore, MR36 should be included as a potential new therapeutic treatment in melanoma research.
Similar content being viewed by others
Introduction
Malignant melanoma has long been identified as one of the most important and inscrutable skin diseases, with increasing incidence and extremely poor prognosis at advanced stages [1]. Historically, dacarbazine has been employed as a standard treatment for melanoma, although it rarely leads to complete remission (5–10% of patients) [2]. In recent years, dacarbazine has been replaced by other chemotherapeutic agents, such as temozolomide (TMZ). Recently, targeted therapies have been developed based on molecular insights into tumor pathogenesis, but these have been relatively ineffective [3]. The lack of therapeutic response to the currently available treatments highlights the importance of improving our understanding of the complex molecular mechanism(s) that contribute to melanoma development [4]. Recent studies have shown that apoptosis is a common mechanism through which chemotherapeutic agents exert their cytotoxicity [5], and genes inducing apoptosis can mediate chemosensitivity [6]. Melanoma cells have low levels of spontaneous apoptosis in vivo compared with other tumor cell types, and they are relatively resistant to drug-induced apoptosis in vitro [7]. Apoptosis may be induced in some cancer cells through the deregulation of cell cycle control genes [8]. The majority of solid human tumors are genetically unstable and have defects in the cell cycle checkpoint control mechanism [9]. Such tumors frequently contain mutations that knock down G1 phase components of the cell cycle (e.g., p53 and retinoblastoma), which affects the ability of chemotherapeutic drugs to inhibit cell proliferation and induce apoptosis [10]. Mutation or deletion of p53 has been linked to more than 55% of all human cancers, including melanoma [11]. However, the role of p53 in melanoma remains controversial.
Thymidylate synthase (TS), a key enzyme in DNA synthesis, is an important chemotherapeutic target that catalyzes the reductive methylation of 2′-deoxyuridine 5′-monophosphate (dUMP) to 2′-deoxythymidine 5′-monophosphate (dTMP). dTMP is then converted to a triphosphate by DNA polymerase and is incorporated into DNA [12]. The reaction is assisted by N5,N10-methylenetetrahydrofolate (mTHF), a co-substrate for the catalyzed reaction, and is the only source of dTMP. TS inhibition leads to thymineless death, which is a complex mechanism that affects the replication process. The roles of TS expression in the prognosis and response to therapy of human tumors have been addressed in several recent studies that suggest an association between high levels of TS and decreased sensitivity to treatment. Many compounds with anticancer activity, such as raltitrexed and pemetrexed, have been designed to target the TS enzyme and the folate pathway in which TS is involved [13, 14]. However, these compounds need to be activated by the polyglutamylation pathway in which the enzyme folylpolyglutamyl synthetase (FPGS) adds more glutamyl groups to the one already present in the TS structure. The failure of this reaction induces the failure of drug activity. Drug resistance problem are induced by the downregulation of FPGS or enzyme mutations. To avoid this drug resistance mechanism, many compounds have been designed as candidate drugs that do not need to be activated by the polyglutamylation pathway. Among these compounds, nolatrexed (AG337) is a candidate in a clinical trial against colon cancer. AG337 has been well tolerated in initial phase I studies, and it has shown promising activity against head and neck, pancreatic, and hepatocellular cancers. A phase II trial of AG337 in patients with squamous cell cancer has shown complete responses in 2 patients and partial responses in 2 out of 22 patients, with an overall response rate of 18% [15]. AG337 has also been characterized by its apoptotic effect in colon cancer cell lines, but its efficacy in melanoma has not been demonstrated.
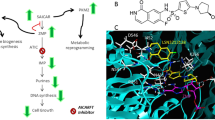
To improve therapeutic selectivity, a structure-based drug design approach has recently been used to synthesize new thymidylate synthase inhibitors (TSIs) that might be able to overcome the resistance problems. These TSIs have a structure that is markedly unrelated to the classical inhibitors and are able to form an enzyme-inhibitor complex that prevents cofactor binding. Compounds, including MR36 used in the present study (Fig. 1), have been designed specifically to avoid polyglutamylation and to enter the cell through membrane diffusion [16].
Chemical structure of the thymidylate synthase inhibitor MR36. MR36 was synthesized based on the X-ray structure of the binary complex of Lactobacillus casei TS with phenolphthalein (PTH). In particular, the 2,3-naphthalein and 1,8-naphthalein derivatives were modified by the introduction of substitutions on the naphthalene ring that influenced the biological activity profile and affinity fingerprint. Docking algorithms were used to generate the naphthalein derivatives
Recently, Giudice et al. demonstrated that MR36, a TSI with a naphthalein structure, has promising activity for melanoma treatment. They hypothesized that MR36 induces apoptosis through a caspase-mediated pathway without the classical involvement of p53/Bax signaling [17]. In the current study, we demonstrated that the inhibition of melanoma cell growth in vitro after MR36 treatment is associated with changes in the expression of key cell cycle regulators that induce an intrinsic pathway-dependent mechanism that is able to act synergistically with the Fas pathway.
Materials and methods
Cell cultures and treatments
The cell lines SK-MEL-2 (from metastatic tissue) and SK-MEL-28 (from a primary malignant melanoma) were obtained from the American Type Culture Collection (ATCC; Manassas, VA, USA) and cultured as previously described [17]. SK-MEL-2 and SK-MEL-28 cells were seeded in 60-mm cell culture dishes (5 × 105 SK-MEL-2 cells/dish and 3 × 105 SK-MEL-28 cells/dish; Costar, Cambridge, MA, USA) for the experiments, and MR36 was added to the cell cultures for 24 h at two different concentrations (20 and 40 μM). The stock solution of the MR36 (100 mM) was dissolved in DMSO at a final concentration not exceeding 0.4%. This concentration has previously been demonstrated not to be toxic in SK-MEL-2 and SK-MEL-28 cells (data not shown). Different concentrations of this compound were prepared in DMEM medium without fetal calf serum. 5-Fluorouracil (5-FU) (Sigma, St Louis, MO, USA) was used at 2.7 μM and 5.5 μM concentration.
Genomic DNA sequencing
DNA was extracted from cultured cells using a DNA extraction kit (Qiagen, Hilden, Germany) in accordance with the manufacturer’s instructions. Exons 5, 6, 7, and 8 of the p53 gene were amplified by PCR, and DNA sequencing was performed using the Big Dye Terminator v3.0 Cycle Sequencing Ready Reaction Kit (Applied Biosystems, Foster City, CA, USA). The sequence products were analyzed by a 3100 Avant Sequencer (Applied Biosystems).
TS assay
Cells to be used for the enzyme assays were harvested at the exponential growth phase and stored at −80°C for at least 6 months. Cell pellets were thawed by the addition of ice-cold assay buffer (200 mM Tris-HCl, pH 7.4; 20 mM 2-mercaptoethanol; 100 mM NaF; and 1% Triton X-100), sonicated and centrifuged at 14,000 g for 15 min at 4°C. The supernatant was used for the TS assay [18]. In brief, the supernatant was added to the assay buffer (without Triton X-100) with 650 μM mTHF. The reaction was started by adding [5-3H]dUMP (final concentration of 1 μM and specific activity of 5 mCi/mol), incubated for 60 min at 37°C, and stopped by adding 50 μl of ice-cold 35% trichloroacetic acid. Residual [5-3H]dUMP was removed with the addition of 10% neutral activated charcoal. After the charcoal was removed, the supernatant was assayed for tritium radioactivity by liquid scintillation counting in a Tri-Carb 2100 liquid scintillation analyzer (Packard, Toronto, ON, Canada). For each cell line, the linearity of [5-3H]dUMP conversion with respect to the amount of protein and time was established.
Reverse-transcription and quantitative PCR
Total cellular RNA from SK-MEL-2 and SK-MEL-28 cells was extracted using TRIzol reagent (Sigma) according to the manufacturer’s protocol. RNA concentration was determined in a spectrophotometer (UV-1601, Shimadzu, Duisburg, Germany), and the quality of total RNA was verified by electrophoresis on a 1% agarose gel. RT-PCR was performed using 1 μg total cellular RNA and 100 ng/μl random primers (Roche, Penzberg, Germany). Each sample was denatured at 70°C for 5 min and placed on ice for 5 min. The samples were mixed with 25 mM dNTPs, 20 U RNase inhibitors, 200 U MMLV reverse transcriptase and 5× reverse transcriptase buffer (all purchased from Promega, Madison, WI, USA), and the reaction was performed in a thermocycler (Biorad, Monaco, Germany). PCR was performed using 25 mM MgCl2, 5× buffer without MgCl2, 25 mM dNTPs (Promega), and 20 pmol/μl primers. The following specific primers were used: human TS forward, 5′AGTACCTGGGGCAGATCCAA3′ and human TS reverse, 5′TGGTCAACTCCCTGTCCTGA3′ (Invitrogen, Carlsbad, CA, USA); β-actin forward, 5′AAAGACCTGTACGCCAACACAGTG3′ and β-actin reverse, 5′GTCATACTCCTGCTTGCTGATCCA3′ (Sigma). PCR was performed in a thermocycler (Biorad). For the amplification of human TS, each sample was denatured at 94°C for 4 min and subjected to 30 amplification cycles (denaturation at 94°C for 1 min, annealing at 53°C for 1 min and elongation at 72°C for 1 min) followed by a final extension at 72°C for 1 min. For the amplification of ß-actin, the same program was used but with an annealing temperature of 60°C. The amplified products were run on a non-denaturing 1.5% agarose gel with ethidium bromide in TBE at 70 V. DNA molecular weight markers were obtained from Roche. Agarose gels were then scanned with a laser densitometer to measure the signals (Pharmacia LKB Ultroscan XL, Lab Extreme, Kent City, MI, USA).
Fas/CD95 blocking experiment
To determine the involvement of the Fas death receptor, SK-MEL-2 and SK-MEL-28 cells were incubated for 30 min at 37°C with 500 ng/ml anti-Fas mAb (clone ZB4, mouse IgG1, MBL International, Watertown, MA, USA) and 100 ng/ml anti-human Fas ligand (clone TNFSF6, R&D Systems, Minneapolis, MN, USA) before treatment with MR36. The cells were then suspended in fresh medium with MR36 for 24 h. These antibody concentrations had previously been optimized for blocking experiments (results not shown). Apoptosis was evaluated at the end of drug exposure by western blot analysis.
Western blot
For Western blot analysis, melanoma cell line proteins were extracted with RIPA buffer (50 mM Tris-HCl,150 mM NaCl, 1% Na deoxycolate, 1% Triton X-100, 0.1% SDS, 0.2% NaN3, PMSF, aprotinin and leupeptin). Equal amounts of each cell lysate were separated using SDS polyacrylamide gel electrophoresis (PAGE). The separated proteins were transferred onto a nitrocellulose membrane and blocked with 5% non-fat dry milk in Phosphate buffer saline (PBS, Lonza, Basel, Switzerland). The blots were incubated with the following primary antibodies: anti-pRb (clone LM95.1, Oncogene, Boston, MA, USA), anti-caspase-8 (clone 1–3, Oncogene), anti-caspase-3 (clone 5F6.H7, Cell Signaling Technology, Danvers, MA, USA), anti-thymidylate synthase (clone TS106, Zymed Laboratories Inc., San Francisco, CA, USA), anti-p21 (clone C-19, Santa Cruz Biotechnology, Santa Cruz, CA, USA), anti-PARP (clone C-2-10, Biomol GmbH, Hamburg, Germany) and anti-cyclin D1(clone DCS-6, Calbiochem, Darmstadt, Germany). Subsequently, the blots were incubated with horseradish peroxidase-conjugated goat anti-mouse IgG (BioRad) and goat anti-rabbit IgG (Dako, Glostrup, Denmark) at a 1:3000 dilution at room temperature. A β-actin antibody (Sigma) was included as a loading control. Immunoblotted bands were visualized by an ECL chemiluminescent system (Amersham, Glattbrugg, Switzerland) and quantified by densitometric analysis using MacBiophotonics ImageJ software for Windows (MacBiophotonics, Hamilton, Ontario, USA).
Statistical analysis
All values were expressed as the mean ± standard error of the mean (SEM). Differences between the controls (C) and the treated samples were determined by paired Student’s t-test. Values of P ≤ 0.05 were considered statistically significant.
Results
TS was expressed in both melanoma cell lines and was inhibited by treatment with MR36
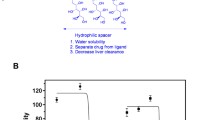
Because TS is an essential S phase enzyme required for DNA synthesis, we hypothesized that MR36 may inhibit TS and induce melanoma cell death. TS catalytic activity was measured by the TS assay. Enzyme levels are shown in Fig. 2. Under basal conditions, TS was expressed at high levels in both melanoma cell lines, which was consistent with results reported for other tumor cells. After treatment with even 5 μM MR36, TS activity in the SK-MEL-28 cell line was inhibited, indicating that SK-MEL-28 cells were more sensitive than SK-MEL-2 cells. The enzyme level decreased in SK-MEL-2 cells after MR36 treatment at a concentration of 20 μM.
Effects of MR36 on thymidylate synthase levels. Comparison of TS levels in SK-MEL-2 and SK-MEL-28 cell lines after MR36 treatment. Values are the means ± SE of at least three independent experiments. The TS assays were performed as described in “Methods.” TS activity was expressed as a percentage of the control
TS protein expression after MR36 treatment was not accompanied by alterations in mRNA expression in either melanoma cell line
TS mRNA expression levels were measured by PCR. TS mRNA was detected in both melanoma cell lines under basal conditions after treatment with MR36 (Fig. 3a, b). The results showed that exposure to MR36 was not accompanied by an increase in TS mRNA expression levels.
PCR and western blot analyses of thymidylate synthase expression and activity. The expression of TS was assessed by PCR (a, b) as described in “Methods.” The specific effect of TS on TS mRNA was evaluated using total cellular mRNA extracted from SK-MEL-2 and SK-MEL-28 cells after treatment with different concentrations of MR36. For quantitative measurements, agarose gels were scanned with a laser densitometer (LKB Ultroscan XL). TS protein levels were assessed by western blot analysis (c, d). All the experiments were performed with MR36 at concentrations of 20 and 40 μM. TS levels decreased in a dose-dependent manner, especially in the SK-MEL-28 cell line. Values are the means of at least three independent experiments. The relative expression levels of TS were determined by densitometric measurements. The controls were set to 100%. (e) Western blot analysis of thymidylate synthase in SK-MEL-2 and SK-MEL-28 cells after treatment with 5-FU and ternary complex formation. The band for TS was as expected at 36kD. Additional band in the second lane is indicated as T (ternary complex). Normal TS is indicated as N. β-actin antibody was included as a loading control
TS protein levels were then measured by western blot analysis. A decrease in TS protein expression was observed after treatment with MR36 (Fig. 3c, d). The decrease in TS protein expression was more evident in the SK-MEL-28 cell line. Moreover, the relative intensity of the bands quantified by densitometric analysis showed that the protein levels significantly decreased in both melanoma cell lines after treatment with MR36 at concentrations of 20 and 40 μM. Western blot analysis showed that MR36 works with a different mechanism in comparison to 5-FU: a ternary complex formed between TS, FdUMP, and mTHF (Fig. 3e), is not observed after MR36 treatment.
p53 is mutated in the SK-MEL-2 and SK-MEL-28 cell lines
To determine whether mutations in p53, a tumor suppressor gene, were present in the SK-MEL-2 and SK-MEL-28 cell lines, DNA sequencing was performed. The alterations in p53 were characterized using polymerase chain reaction single-strand conformational polymorphism analysis and sequencing. p53 exons 5 to 8 were analyzed in both melanoma cell lines.
Molecular analysis revealed that p53 had a G to A transition (codon 245 in exon 7) in SK-MEL-2 cells and a CTG to CGT transversion (codon 145 in exon 5) in SK-MEL-28 cells (data not shown).
p53-independent upregulation of p21 and the phosphorylation of pRb contributes to G1 cell cycle arrest after MR36 exposure
To explore the underlying mechanism of cell cycle arrest induced by MR36, we examined the expression of cell cycle-related proteins (cyclin D1, p21 and pRb) in total cell lysates by western blot analysis. The expression of p21 was upregulated and pRb was hypophosphorylated in both melanoma cell lines after MR36 treatment (Fig. 4a). Moreover, cyclin D1 protein expression was decreased following MR36 treatment, especially at a concentration of 40 μM, in SK-MEL-28 cells.
Protein levels of cyclin D1, p21, pRb and caspase-3 in the SK-MEL-2 and SK-MEL-28 cell lines after MR36 exposure (a). MR36 induced cell cycle arrest by the activation of cell cycle-related proteins (cyclin D1, p21 and pRb). MR36 treatment reduced the expression of full-length caspase-3 as demonstrated by western blot analysis. The cells were incubated with MR36 (20 and 40 μM) for 24 h in the absence of serum. β-actin was included as a loading control. Western blot analysis of caspase-8 and PARP protein levels in the SK-MEL-2 and SK-MEL-28 cell lines after treatment with MR36 and ZB4/FasL neutralization (b). ZB4 and anti-human FasL partially inhibited the extrinsic pathway, as indicated by decreased levels of full-length caspase-8 after MR36 treatment. In contrast, Fas neutralization did not involve the intrinsic pathway because PARP cleavage was still present. Fas was neutralized by pre-incubating the cells with ZB4 and anti-human FasL for 1 h. After pretreatment, MR36 was added for 24 h. The proteins were then extracted, and the induction of apoptosis was analyzed by western blot. β-actin was included as a loading control
Molecular mechanism of TSI-mediated apoptosis: cleavage of caspase-3 and involvement of both the extrinsic and intrinsic pathways
Based on previous results [17], we focused on the molecular mechanism of TSI-mediated apoptosis in melanoma cell lines. In particular, we analyzed caspase-3 activity by western blot analysis. The expression of full-length caspase-3 was reduced in both melanoma cell lines after treatment with 40 μM MR36 (Fig. 4a).
The involvement of the extrinsic and intrinsic pathways in MR36-mediated apoptosis was also evaluated. To determine the involvement of the Fas death receptor, a specific anti-Fas mAb (clone ZB4) and an anti-human Fas Ligand (FasL) were used. The cells were treated with 500 ng/ml anti-Fas mAb in the presence of anti-human FasL to prevent the binding of FasL to its receptor. After 1 h, the cells were exposed to MR36, and apoptosis was subsequently evaluated by western blot analysis. Figure 4b shows a clear reduction in full-length caspase-8 and PARP cleavage after MR36 treatment. The reduction in full-length caspase-8 cleavage was decreased in cells pretreated with anti-Fas mAb, indicating the involvement of the Fas death receptor. PARP cleavage was still present after anti-Fas mAb pretreatment, indicating that the intrinsic pathway was involved in the apoptosis program, even though Fas was neutralized. The results were the same in both melanoma cell lines, even though SK-MEL-28 cells were more sensitive to the antifolate treatment.
Discussion
Melanoma has a poor prognosis, and it is largely resistant to conventional treatments [2]. The present study focused on TS, a crucial enzyme for DNA synthesis that is inhibited by substrate analogs, such as 5-fluoro-2′-deoxyuridine 5′-monophosphate (FdUMP), or cofactor analogs, such as ZD1694, pemetrexed (Alimta) [19] and thymitaq/AG337 [20]. All these TSIs have been shown to act as anticancer drugs through different mechanisms that involve interacting with components of the TS pathway [21].
TSIs have also been tested for melanoma treatment and have shown limited effectiveness due to drug resistance. For example, methotrexate (MTX), the most frequently used antifolate, is an effective drug for several types of cancer, but it is not active against melanoma [22]. The specific basis for the resistance of melanoma cells to MTX is unclear, but it may be related to a reduction in the cellular uptake of this drug, an insufficient rate of MTX polyglutamylation and high intracellular levels of dihydrofolate reductase (DHFR) [23].
Previously, Benassi et al. [24] used a structure-based drug design approach to synthesize a new non-classical TSI (MR36) to overcome the resistance problems and to obtain a structure markedly unrelated to the classical inhibitors. This naphthalein derivative competes with folate to form an enzyme-inhibitor complex, which prevents the binding of the cofactor. MR36 has been tested in a primary in vitro anticancer screening by the National Cancer Institute (NCI, Bethesda, USA). The NCI results regarding SK-MEL-2 and SK-MEL-28 cells showed a growth inhibitory effect (GI50) at a concentration of 20 μM and a cytotoxic effect (LC50) at a concentration of 100 μM for both cell lines [24].
In the present study, we extended the biochemical characterization of MR36 and showed that it could compete with TS and inhibit its catalytic activity by approximately 20% in SK-MEL-2 cells and by 30–40% in SK-MEL-28 cells compared with control cells when used at concentrations of 20 and 40 μM (Fig. 2). Although the classical TSIs are active in a nanomolar range when polyglutamylated, and MR36-induced inhibition is insufficient in colon cancer cell lines, the results of the present study are interesting when considering that classical antifolates are not effective in melanoma cell lines. AG337 exerts stronger inhibitory activity than MR36 at the same concentrations, but AG337 is completely ineffective in melanoma cell lines [14, 25]. The present study supported the evidence that melanoma cell cultures are sensitive to treatment with MR36, unlike conventional TSIs, even if the inhibitory effect is moderate.
Chu et al. [26] demonstrated that intracellular TS levels are controlled by an autoregulatory mechanism in which binding of TS protein to its own mRNA inhibits translation, resulting in decreased intracellular levels of TS. Exposure to 5-FU increased the expression of TS levels without a corresponding increase in the levels of TS mRNA. A number of studies with cultured cell lines, tumor models, and clinical specimens have shown that TS expression increases after 5-FU exposure disrupts the TS mRNA-protein complex, thereby restoring mRNA translation [21, 27] and inducing enzyme levels by approximately 2- to 4-fold. These studies have provided the basis for the translational autoregulation model and explained the occurrence of resistance to compounds targeting TS, including the inhibitors 5-FU, raltitrexed, pemetrexed, and ZD9331. In the present study, TS protein levels decreased in both melanoma cell lines after treatment with MR36 (Fig. 3c, d), and this result was not accompanied by changes in mRNA levels. This indicates that MR36 preserved the autoregulatory feedback loop of TS by promoting its inhibitory effect (Fig. 3a, b). In addition, our analysis of TS protein levels revealed that MR36 used a different mechanism from the classical TSI mechanism. Moreover, FdUMP forms a ternary complex with TS and mTHF to inhibit dTMP synthesis. The presence of the ternary complex has been demonstrated by the presence of an additional band at approximately 38 kDa on western blots from different tumor cell lines (Fig. 3e). The absence of this band after treatment with MR36 suggested that this new TSI acts without the formation of a ternary complex (Fig. 3c, d).
TSIs can induce an imbalance in dNTPs, which results in DNA damage [28]. In normal cells, progression through the cell cycle is dependent on the coordinated actions of various proteins encoded by genes known as proto-oncogene and tumor suppressor genes. Mutations of these genes may result in neoplastic transformation and tumor formation. In human cancer studies [29], mutations leading to the loss of function of p53, a tumor suppressor gene, are found in approximately 50% of all tumors. Recent data have shown that several human myeloid leukemia cell lines (HL-60, THP-1, and U937), colon cancer cell lines and prostate cancer cell lines in which p53 is either not expressed or mutated undergo apoptosis when treated with TSIs that use a mechanism involving cell cycle arrest [30]. The SK-MEL-2 and SK-MEL-28 cell lines used in this study contained mutant forms of p53; DNA sequencing revealed that p53 in SK-MEL-2 cells had a G to A transition (codon 245 in exon 7) and that p53 in SK-MEL-28 cells had a CTG to CGT transversion (codon 145 in exon 5).
The in vitro experiments using melanoma cell lines in the present study demonstrated that MR36 treatment caused the activation of a molecular pathway that first leads to cell cycle arrest and then to apoptosis [31]. Western blot analysis demonstrated the upregulation of p21, the hypophosphorylation of pRb and the downregulation of cyclin D1 (Fig. 4a). These results suggested that MR36-induced apoptosis in melanoma cell lines involves G1 cell-cycle arrest. During the G1 phase, the D-type cyclins accumulate and form complexes with cyclin-dependent kinases that lead to pRb phosphorylation, which is an essential event for cell cycle progression. pRb proteins are pocket proteins that sequester E2F transcription factors, thereby preventing the activation of critical genes in cell proliferation. After pRb phosphorylation, E2F proteins are released, which promote the transcription of essential genes for the transition into S phase of the cell cycle. In addition, pRb-mediated cell cycle arrest is associated with p21 accumulation.
Apoptosis is a tightly regulated process, which involves changes in the expression of a distinct pattern of genes [32]. In particular, apoptosis acts through the extrinsic and intrinsic major molecular pathways. The proapoptotic effect of TSIs involve different mechanisms. In colon cancer cell lines, AG337 induces apoptosis with an intrinsic pathway-dependent mechanism [30]. Many studies have reported a defective or downregulated extrinsic death receptor signaling pathway in melanoma cells [33]. The present study demonstrated that MR36 induced apoptosis in SK-MEL-2 and SK-MEL-28 cell lines with both intrinsic- and extrinsic-pathway-dependent mechanisms (Fig. 5). Independent of p53 status, caspase-3 clearly mediated MR36-induced apoptosis. Furthermore, caspase-8 and PARP were activated via the Fas system. However, MR36-induced apoptosis may be activated by other death receptors or caspases, or it may even be mitochondria-dependent. These suggestions were confirmed by the observation that MR36-induced apoptosis was triggered even after treatment with anti-Fas mAb (clone ZB4) and anti-human FasL (Fig. 4b).
MR36 apoptotic pathway. MR36-induced apoptosis can be initiated through the following two main pathways: the death receptor (extrinsic) pathway (1) and the mitochondrial (intrinsic) pathway (7). The death receptor pathway is activated by the binding of FAS ligands (2) to their receptors, which stimulates receptor aggregation. This aggregation induces the recruitment of FADD (3) and procaspase-8 activation. Caspase-8 activation (4) leads to caspase-3 cleavage (11), which initiates multiple proapoptotic processes, including CAD stimulation (12) and DNA cleavage (13). At the same time, in the mitochondrial pathway, proapoptotic proteins form pores in the mitochondria. This process then releases apoptogenic factors, including cytochrome C (8), APAF1, and caspase-9, from the mitochondrial intermembrane space (9). These factors form the apoptosome (10), which stimulates apoptosis through caspase-3 cleavage (11), CAD stimulation (12) and DNA cleavage (13). Data from the present study suggest that MR36 regulates the levels of the known cell cycle regulator cyclin D and the cell cycle inhibitors p21 (5) and pRb (6), resulting in cell cycle arrest and apoptosis (13)
In conclusion, we focus on two results. First, MR36 is a new potential melanoma treatment that is able to inhibit TS protein expression. Second, the study suggests the possibility of a new TSI strategy that may be able to circumvent mechanisms of resistance. MR36-induced apoptosis in melanoma cell lines is mediated via caspases with a clear involvement of Fas signaling. The independence of the downstream apoptosis processes from the status of p53 is a crucial point that will allow the use of this drug not only in melanoma but in all types of cancer with p53 mutations.
MR36 exerts inhibitory effects on melanoma cell cycle progression. These results give more detailed insight into the process of TS inhibition and its downstream events, which in the future can contribute to the development of better treatment strategies for patients with melanoma.
References
Yang CS, Chung JY, Yang GY, Li C, Meng X, Lee MJ (2000) Mechanisms of inhibition of carcinogenesis by tea. Biofactors 13:73–79
Wolchok JD, Saenger YM (2007) Current topics in melanoma. Curr Opin Oncol 19:116–120
Lissitzky JC, Parriaux D, Ristorcelli E, Vérine A, Lombardo D, Verrando P (2009) Cyclic AMP signaling as a mediator of vasculogenic mimicry in aggressive human melanoma cells in vitro. Cancer Res 69:802–809
Zheng H, Gao L, Feng Y, Yuan L, Zhao H, Cornelius LA (2009) Down-regulation of Rap1GAP via promoter hypermethylation promotes melanoma cell proliferation, survival, and migration. Cancer Res 69:449–457
Guchelaar HJ, Vermes A, Vermes I, Haanen C (1997) Apoptosis: Molecular mechanism and implications for cancer chemotherapy. Pharm World Sci 19:119–125
Citro G, D’Agnano I, Leonetti C, Perini R, Bucci B, Zon G et al (1998) c-myc antisense oligodeoxynucleotides enhance the efficacy of cisplatin in melanoma chemotherapy in vitro and in nude mice. Cancer Res 58:283–289
Hersey P (2006) Apoptosis and melanoma: how new insightsare effecting the development of new therapies for melanoma. Curr Opin Oncol 18:189–196
Pucci B, Kasten M, Giordano A (2000) Cell cycle and apoptosis. Neoplasia 2:2291–2299
Chiu LC, Wong EY, Ooi VE (2004) Docosahexaenoic acid modulates different genes in cell cycle and apoptosis to control growth of human leukemia HL-60 cells. Int J Oncol 25:737–744
King RW, Jackson PK, Kirschner MW (1994) Mitosis in transition. Cell 79:563–571
Greenblatt MS, Bennett WP, Hollstein M, Harris CC (1994) Mutations in the p53 tumor suppressor gene: clues to cancer etiology and molecular pathogenesis. Cancer Res 54:4855–4878
Costi MP, Gelain A, Barlocco D, Ghelli S, Soragni F, Reniero F et al (2006) Antibacterial agent discovery using thymidylate synthase biolibrary screening. J Med Chem 49:5958–5968
Chattopadhyay S, Moran RG, Goldman ID (2007) Pemetrexed: biochemical and cellular pharmacology, mechanisms, and clinical applications. Mol Cancer Ther 6:404–417
Peters GJ, van Triest B, Backus HH, Kuiper CM, van der Wilt CL, Pinedo HM (2000) Molecular downstream events and induction of thymidylate synthase in mutant and wild-type p53 colon cancer cell lines after treatment with 5-fluorouracil and the thymidylate synthase inhibitor raltitrexed. Eur J Cancer 36:916–924
McGuire JJ, Canestrari JG, Nagel GS (1999) Characterization of the effect of AG337, a novel lipophilic thymidylate synthase inhibitor, on human head and neck and human leukemia cell lines. Int J Oncol 15:1245–1250
Costi MP, Tondi D, Rinaldi M, Barlocco D, Pecorari P, Soragni F et al (2002) Structure-based studies on species-specific inhibition of thymidylate synthase. Biochim Biophys Acta 1587:206–214
Giudice S, Benassi L, Bertazzoni G, Costi MP, Gelain A, Venturelli A et al (2007) New thymidylate synthase inhibitors induce apoptosis in melanoma cell lines. Toxicol In Vitro 21:240–248
van Triest B, Pinedo HM, van Hensbergen Y, Smid K, Telleman F, Schoenmakers PS et al (1999) Thymidylate synthase level as the main predictive parameter for sensitivity to 5-fluorouracil, but not for folate-based thymidylate synthase inhibitors, in 13 nonselected colon cancer cell lines. Clin Cancer Res 5:643–654
Shih C, Chen VJ, Gossett LS, Gates SB, MacKellar WC, Habeck LL et al (1997) LY231514, a pyrrolo[2,3-d]- pyrimidine-based antifolate that inhibits multiple folate-requiring enzymes. Cancer Res 57:1116–1123
Webber S, Bartlett CA, Boritzki TJ, Hillard JA, Howland EF, Johnston AL et al (1996) AG337, a novel lipophilic thymidylate synthase inhibitor: in vitro and in vivo pre-clinical studies. Cancer Chemother Pharmacol 37:509–517
Ghelli S, Rinaldi M, Barlocco D, Gelain A, Pecorari P, Tondi D et al (2003) ortho-Halogen naphthaleins as specific inhibitors of Lactobacillus casei thymidylate synthase. Conformational properties and biological activity. Bioorg Med Chem 11:951–963
Kufe DW, Wick MM, Abelson HT (1980) Natural resistance to methotrexate in human melanomas. J Invest Dermatol 75:357–359
Sánchez-del-Campo L, Montenegro MF, Cabezas-Herrera J, Rodríguez-López JN (2009) The critical role of alpha-folate receptor in the resistance of melanoma to methotrexate. Pigment Cell Melanoma Res 22:588–600
Benassi L, Magnoni C, Giudice S, Bertazzoni G, Costi MP, Rinaldi M et al (2006) Pharmacological and toxicological evaluation of a new series of thymidylate synthase inhibitors as anticancer agents. Anticancer Res 26:3499–3504
Fanciullino R, Giacometti S, Mercier C, Aubert C, Blanquicett C, Piccerelle P et al (2007) In vitro and in vivo reversal of resistance to 5-fluorouracil in colorectal cancer cells with a novel stealth double-liposomal formulation. Br J Cancer 97:919–926
Chu E, Allegra CJ (1996) The role of thymidylate synthase in cellular regulation. Adv Enzyme Regul 36:143–163
Keyomarsi K, Samet J, Molnar G, Pardee AB (1993) The thymidylate synthase inhibitor, ICI D1694, overcomes translational detainment of the enzyme. J Biol Chem 15:15142–15149
Curtin NJ, Harris AL, Aherne GW (1991) Mechanism of cell death following thymidylate synthase inhibition: 2′-deoxyuridine-5′-triphosphate accumulation, DNA damage, and growth inhibition following exposure to CB3717 and dipyridamole. Cancer Res 51:2346–2352
Brown CJ, Lain S, Verma CS, Fersht AR, Lane DP (2009) Awakening guardian angels: drugging the p53 pathway. Nat Rev Cancer 9:862–873
Backus HH, Wouters D, Ferreira CG, van Houten VM, BrakenhoV RH, Pinedo HM et al (2003) Thymidylate synthase inhibition triggers apoptosis via caspases-8 and −9 in both wild-type and mutant p53 colon cancer cell lines. Eur J Cancer 39:1310–1317
Coudray AM, Louvet C, Kornprobst M, Raymond E, André T, Tournigand C et al (2005) Increased anticancer activity of the thymidylate synthase inhibitor BGC9331 combined with the topoisomerase I inhibitor SN-38 in human colorectal and breast cancer cells: induction of apoptosis and ROCK cleavage through caspase-3-dependent and -independent mechanisms. Int J Oncol 27:553–561
Bowen AR, Hanks AN, Allen SM, Alexander A, Diedrich MJ, Grossman D (2003) Apoptosis regulators and responses in human melanocytic and keratinocytic cells. J Invest Dermatol 120:48–55
Ashkenazi A, Dixit VM (1998) Death receptors: signalling and modulation. Science 281:1305–1308
Acknowledgements
We thank Professor Marcella Rinaldi (Department of Pharmaceutical Sciences, University of Modena and Reggio Emilia) for supplying and synthesizing the Thymidylate synthase inhibitor and Doctor Gaetano Marverti (Department of Biochemistry, University of Modena and Reggio Emilia) for helping with biochemical facilities. This work has been supported by PRIN2006 grant number 2006030430_004 to Maria Paola Costi and AIRC grant IG 10474.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Giudice, S., Benassi, L., Bertazzoni, G. et al. Biological evaluation of MR36, a novel non-polyglutamatable thymidylate synthase inhibitor that blocks cell cycle progression in melanoma cell lines. Invest New Drugs 30, 1484–1492 (2012). https://doi.org/10.1007/s10637-011-9733-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-011-9733-2