Abstract
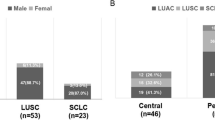
Hypermethylation of the promoter region of tumor suppressor genes is associated with carcinogenesis in lung cancer (LC). Endobronchial ultrasound with needle aspiration (EBUS-NA) is a semi-invasive method for obtaining cell blocks from lymph nodes, which can be used for epigenetic analyses. To establish the relationship between methylation status of p16, DAPK, RASSF1a, APC and CDH13 genes in lymph nodes sampled by EBUS-NA, tumor staging and prognosis. Methylation status of DAPK, p16, RASSF1a, APC and CDH13 genes was assessed in EBUS-NA cell blocks from LC patients and related to stage and survival. Eighty-five consecutive patients [mean age 67 (SD 8)] were included. Methylation of ≥1 gene was found in 43 malignant nodes (67 %). A higher prevalence of RASSF1a methylation was observed in small cell lung cancer patients [9/10 (90 %) vs. 15/53 (28 %); p < 0.001 χ2 test]. Methylation of APC and/or p16 was related to advanced staging in non-small cell lung cancer (NSCLC) [15/29 (52 %) vs. 6/24 (25 %), p = 0.048, χ2 test]. Patients with NSCLC showing methylation of APC and/or p16 had also lower 6-month survival (p = 0.019, log rank test), which persisted after adjustment for age and subtyping (HR = 6, 95 % CI [1.8–19.5], p = 0.003, Cox regression). Epigenetic analyses are feasible in EBUS-NA cell blocks and may identify methylation patterns associated with worse prognosis. Methylation of p16 and APC genes in NSCLC patients was associated with advanced staging and lower 6-month survival.

Similar content being viewed by others
References
Globocan (2012) Home. http://globocan.iarc.fr/Default.aspx. Accessed 10 Jul 2014
Siegel R, Naishadham D, Jemal A (2013) Cancer statistics, 2013. CA Cancer J Clin 63:11–30. doi:10.3322/caac.21166
Youlden DR, Cramb SM, Baade PD (2008) The international epidemiology of lung cancer: geographical distribution and secular trends. J Thorac Oncol 3:819–831. doi:10.1097/JTO.0b013e31818020eb
Kratz JR, Jablons DM (2009) Genomic prognostic models in early-stage lung cancer. Clin Lung Cancer 10:151–157. doi:10.3816/CLC.2009.n.021
Langevin SM, Kratzke RA, Kelsey KT (2014) Epigenetics of lung cancer. Transl Res J Lab Clin Med. doi:10.1016/j.trsl.2014.03.001
Darwiche K, Zarogoulidis P, Baehner K et al (2013) Assessment of SHOX2 methylation in EBUS-TBNA specimen improves accuracy in lung cancer staging. Ann Oncol 24:2866–2870. doi:10.1093/annonc/mdt365
Belinsky SA, Liechty KC, Gentry FD et al (2006) Promoter hypermethylation of multiple genes in sputum precedes lung cancer incidence in a high-risk cohort. Cancer Res 66:3338–3344. doi:10.1158/0008-5472.CAN-05-3408
Belinsky SA (2005) Silencing of genes by promoter hypermethylation: key event in rodent and human lung cancer. Carcinogenesis 26:1481–1487. doi:10.1093/carcin/bgi020
Belinsky SA, Nikula KJ, Palmisano WA et al (1998) Aberrant methylation of p16(INK4a) is an early event in lung cancer and a potential biomarker for early diagnosis. Proc Natl Acad Sci USA 95:11891–11896
Licchesi JDF, Westra WH, Hooker CM, Herman JG (2008) Promoter hypermethylation of hallmark cancer genes in atypical adenomatous hyperplasia of the lung. Clin Cancer Res 14:2570–2578. doi:10.1158/1078-0432.CCR-07-2033
Belinsky SA (2015) Unmasking the lung cancer epigenome. Annu Rev Physiol 77:453–474. doi:10.1146/annurev-physiol-021014-072018
Lin Q, Geng J, Ma K et al (2009) RASSF1A, APC, ESR1, ABCB1 and HOXC9, but not p16INK4A, DAPK1, PTEN and MT1G genes were frequently methylated in the stage I non-small cell lung cancer in China. J Cancer Res Clin Oncol 135:1675–1684. doi:10.1007/s00432-009-0614-4
Dammann R, Li C, Yoon JH et al (2000) Epigenetic inactivation of a RAS association domain family protein from the lung tumour suppressor locus 3p21.3. Nat Genet 25:315–319. doi:10.1038/77083
Licchesi JDF, Westra WH, Hooker CM et al (2008) Epigenetic alteration of Wnt pathway antagonists in progressive glandular neoplasia of the lung. Carcinogenesis 29:895–904. doi:10.1093/carcin/bgn017
Fukui T, Kondo M, Ito G et al (2005) Transcriptional silencing of secreted frizzled related protein 1 (SFRP 1) by promoter hypermethylation in non-small-cell lung cancer. Oncogene 24:6323–6327. doi:10.1038/sj.onc.1208777
Mazieres J, He B, You L et al (2004) Wnt inhibitory factor-1 is silenced by promoter hypermethylation in human lung cancer. Cancer Res 64:4717–4720. doi:10.1158/0008-5472.CAN-04-1389
Kim DH, Nelson HH, Wiencke JK et al (2001) Promoter methylation of DAP-kinase: association with advanced stage in non-small cell lung cancer. Oncogene 20:1765–1770. doi:10.1038/sj.onc.1204302
Tang X, Khuri FR, Lee JJ et al (2000) Hypermethylation of the death-associated protein (DAP) kinase promoter and aggressiveness in stage I non-small-cell lung cancer. J Natl Cancer Inst 92:1511–1516
Toyooka S, Toyooka KO, Miyajima K et al (2003) Epigenetic down-regulation of death-associated protein kinase in lung cancers. Clin Cancer Res 9:3034–3041
Raveh T, Droguett G, Horwitz MS et al (2001) DAP kinase activates a p19ARF/p53-mediated apoptotic checkpoint to suppress oncogenic transformation. Nat Cell Biol 3:1–7. doi:10.1038/35050500
Brock MV, Hooker CM, Ota-Machida E et al (2008) DNA methylation markers and early recurrence in stage I lung cancer. N Engl J Med 358:1118–1128. doi:10.1056/NEJMoa0706550
Agathanggelou A, Honorio S, Macartney DP et al (2001) Methylation associated inactivation of RASSF1A from region 3p21.3 in lung, breast and ovarian tumours. Oncogene 20:1509–1518. doi:10.1038/sj.onc.1204175
Honorio S, Agathanggelou A, Schuermann M et al (2003) Detection of RASSF1A aberrant promoter hypermethylation in sputum from chronic smokers and ductal carcinoma in situ from breast cancer patients. Oncogene 22:147–150. doi:10.1038/sj.onc.1206057
Belinsky SA, Nikula KJ, Palmisano WA et al (1998) Aberrant methylation of p16(INK4a) is an early event in lung cancer and a potential biomarker for early diagnosis. Proc Natl Acad Sci USA 95:11891–11896
Benlloch S, Galbis-Caravajal JM, Alenda C et al (2009) Expression of molecular markers in mediastinal nodes from resected stage I non-small-cell lung cancer (NSCLC): prognostic impact and potential role as markers of occult micrometastases. Ann Oncol 20:91–97. doi:10.1093/annonc/mdn538
Adams K, Shah PL, Edmonds L, Lim E (2009) Test performance of endobronchial ultrasound and transbronchial needle aspiration biopsy for mediastinal staging in patients with lung cancer: systematic review and meta-analysis. Thorax 64:757–762. doi:10.1136/thx.2008.109868
Varela-Lema L, Fernández-Villar A, Ruano-Ravina A (2009) Effectiveness and safety of endobronchial ultrasound-transbronchial needle aspiration: a systematic review. Eur Respir J 33:1156–1164. doi:10.1183/09031936.00097908
Sanz-Santos J, Serra M, Gallego M et al (2014) Determinants of false-negative results in non-small-cell lung cancer staging by endobronchial ultrasound-guided needle aspiration. Eur J Cardio-Thorac Surg. doi:10.1093/ejcts/ezu253
Nakajima T, Yasufuku K, Suzuki M et al (2007) Assessment of epidermal growth factor receptor mutation by endobronchial ultrasound-guided transbronchial needle aspiration. Chest 132:597–602. doi:10.1378/chest.07-0095
Garcia-Olivé I, Monsó E, Andreo F et al (2010) Endobronchial ultrasound-guided transbronchial needle aspiration for identifying EGFR mutations. Eur Respir J 35:391–395. doi:10.1183/09031936.00028109
Sanz-Santos J, Andreo F, Sánchez D et al (2010) Usefulness of a lung cancer rapid diagnosis specialist clinic. Contribution of ultrasound bronchoscopy. Arch Bronconeumol 46:640–645. doi:10.1016/j.arbres.2010.07.005
De Leyn P, Lardinois D, Van Schil PE et al (2007) ESTS guidelines for preoperative lymph node staging for non-small cell lung cancer. Eur J Cardio-Thorac Surg 32:1–8. doi:10.1016/j.ejcts.2007.01.075
Cerfolio RJ, Bryant AS (2007) Ratio of the maximum standardized uptake value on FDG-PET of the mediastinal (N2) lymph nodes to the primary tumor may be a universal predictor of nodal malignancy in patients with nonsmall-cell lung cancer. Ann Thorac Surg 83:1826–1829. doi:10.1016/j.athoracsur.2006.12.034 (discussion 1829–1830)
Du Rand IA, Barber PV, Goldring J et al (2011) British Thoracic Society guideline for advanced diagnostic and therapeutic flexible bronchoscopy in adults. Thorax 66(3):1–21. doi:10.1136/thoraxjnl-2011-200713
Garcia-Olivé I, Monsó E, Andreo F et al (2009) Sensitivity of linear endobronchial ultrasonography and guided transbronchial needle aspiration for the identification of nodal metastasis in lung cancer staging. Ultrasound Med Biol 35:1271–1277. doi:10.1016/j.ultrasmedbio.2009.03.007
Lee HS, Lee GK, Lee H-S et al (2008) Real-time endobronchial ultrasound-guided transbronchial needle aspiration in mediastinal staging of non-small cell lung cancer: how many aspirations per target lymph node station? Chest 134:368–374. doi:10.1378/chest.07-2105
Nayak A, Sugrue C, Koenig S et al (2012) Endobronchial ultrasound-guided transbronchial needle aspirate (EBUS-TBNA): a proposal for on-site adequacy criteria. Diagn Cytopathol 40:128–137. doi:10.1002/dc.21517
Alsharif M, Andrade RS, Groth SS et al (2008) Endobronchial ultrasound-guided transbronchial fine-needle aspiration: the University of Minnesota experience, with emphasis on usefulness, adequacy assessment, and diagnostic difficulties. Am J Clin Pathol 130:434–443. doi:10.1309/BLLQF8KDHWW6MJNQ
Du Rand IA, Blaikley J, Booton R et al (2013) British thoracic society guideline for diagnostic flexible bronchoscopy in adults: accredited by NICE. Thorax 68(Suppl 1):i1–i44. doi:10.1136/thoraxjnl-2013-203618
Nakajima T, Yasufuku K (2011) How I do it–optimal methodology for multidirectional analysis of endobronchial ultrasound-guided transbronchial needle aspiration samples. J Thorac Oncol 6:203–206. doi:10.1097/JTO.0b013e318200f496
Sanz-Santos J, Serra P, Andreo F et al (2012) Contribution of cell blocks obtained through endobronchial ultrasound-guided transbronchial needle aspiration to the diagnosis of lung cancer. BMC Cancer 12:34. doi:10.1186/1471-2407-12-34
Esterbrook G, Anathhanam S, Plant PK (2013) Adequacy of endobronchial ultrasound transbronchial needle aspiration samples in the subtyping of non-small cell lung cancer. Lung Cancer 80:30–34. doi:10.1016/j.lungcan.2012.12.017
Navani N, Brown JM, Nankivell M et al (2012) Suitability of endobronchial ultrasound-guided transbronchial needle aspiration specimens for subtyping and genotyping of non-small cell lung cancer: a multicenter study of 774 patients. Am J Respir Crit Care Med 185:1316–1322. doi:10.1164/rccm.201202-0294OC
Goldstraw P (2009) Staging manual in thoracic oncology. RX Press, Orange Park
Goldstraw P, Crowley J, Chansky K et al (2007) The IASLC lung cancer staging project: proposals for the revision of the TNM stage groupings in the forthcoming (seventh) edition of the TNM classification of malignant tumours. J Thorac Oncol 2:706–714. doi:10.1097/JTO.0b013e31812f3c1a
Yung RCW, Otell S, Illei P et al (2012) Improvement of cellularity on cell block preparations using the so-called tissue coagulum clot method during endobronchial ultrasound-guided transbronchial fine-needle aspiration. Cancer Cytopathol 120:185–195. doi:10.1002/cncy.20199
Hirsch FR, Wynes MW, Gandara DR, Bunn PA (2010) The tissue is the issue: personalized medicine for non-small cell lung cancer. Clin Cancer Res 16:4909–4911. doi:10.1158/1078-0432.CCR-10-2005
Almeida FA (2012) Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer. Cleve Clin J Med 79(1):S11–S16. doi:10.3949/ccjm.79.s2.03
Plönes T, Elze M, Kayser G et al (2014) mRNA and miRNA analyses in cytologically positive endobronchial ultrasound-guided transbronchial needle aspiration: implications for molecular staging in lung cancer patients. Cancer Cytopathol 122:292–298. doi:10.1002/cncy.21398
Kinsey CM, Arenberg DA (2014) Endobronchial ultrasound-guided transbronchial needle aspiration for non-small cell lung cancer staging. Am J Respir Crit Care Med 189:640–649. doi:10.1164/rccm.201311-2007CI
Leiro-Fernández V, De Chiara L, Botana-Rial M et al (2014) Viability of lymph node samples obtained by echobronchoscopy in the study of epigenetic alterations in patients with lung cancer. Arch Bronconeumol 50:213–220. doi:10.1016/j.arbres.2013.11.017
Nakajima T, Yasufuku K, Suzuki M et al (2009) Assessment of chemosensitivity-related aberrant methylation of nonsmall cell lung cancer by EBUS-TBNA. J Bronchol Interv Pulmonol 16:10–14. doi:10.1097/LBR.0b013e318195d930
Schuurbiers OCJ, Looijen-Salamon MG, Ligtenberg MJL, van der Heijden HFM (2010) A brief retrospective report on the feasibility of epidermal growth factor receptor and KRAS mutation analysis in transesophageal ultrasound- and endobronchial ultrasound-guided fine needle cytological aspirates. J Thorac Oncol 5:1664–1667. doi:10.1097/JTO.0b013e3181f0bd93
Reynolds JP, Tubbs RR, Minca EC et al (2014) EGFR mutational genotyping of liquid based cytology samples obtained via fine needle aspiration (FNA) at endobronchial ultrasound of non-small cell lung cancer (NSCLC). Lung Cancer. doi:10.1016/j.lungcan.2014.09.003
Folch E, Yamaguchi N, VanderLaan PA et al (2013) Adequacy of lymph node transbronchial needle aspirates using convex probe endobronchial ultrasound for multiple tumor genotyping techniques in non-small-cell lung cancer. J Thorac Oncol 8:1438–1444. doi:10.1097/JTO.0b013e3182a471a9
Pellisé M, Castells A, Ginès A et al (2004) Detection of lymph node micrometastases by gene promoter hypermethylation in samples obtained by endosonography-guided fine-needle aspiration biopsy. Clin Cancer Res 10:4444–4449. doi:10.1158/1078-0432.CCR-03-0600
Toyooka S, Toyooka KO, Maruyama R et al (2001) DNA methylation profiles of lung tumors. Mol Cancer Ther 1:61–67
Yanagawa N, Tamura G, Oizumi H et al (2003) Promoter hypermethylation of tumor suppressor and tumor-related genes in non-small cell lung cancers. Cancer Sci 94:589–592
Harden SV, Tokumaru Y, Westra WH et al (2003) Gene promoter hypermethylation in tumors and lymph nodes of stage I lung cancer patients. Clin Cancer Res 9:1370–1375
Gu J, Berman D, Lu C et al (2006) Aberrant promoter methylation profile and association with survival in patients with non-small cell lung cancer. Clin Cancer Res 12:7329–7338. doi:10.1158/1078-0432.CCR-06-0894
Hawes SE, Stern JE, Feng Q et al (2010) DNA hypermethylation of tumors from non-small cell lung cancer (NSCLC) patients is associated with gender and histologic type. Lung Cancer 69:172–179. doi:10.1016/j.lungcan.2009.11.002
Yanagawa N, Tamura G, Oizumi H et al (2007) Promoter hypermethylation of RASSF1A and RUNX3 genes as an independent prognostic prediction marker in surgically resected non-small cell lung cancers. Lung Cancer 58:131–138. doi:10.1016/j.lungcan.2007.05.011
Zöchbauer-Müller S, Fong KM, Virmani AK et al (2001) Aberrant promoter methylation of multiple genes in non-small cell lung cancers. Cancer Res 61:249–255
Belinsky SA, Palmisano WA, Gilliland FD et al (2002) Aberrant promoter methylation in bronchial epithelium and sputum from current and former smokers. Cancer Res 62:2370–2377
Kim DH, Nelson HH, Wiencke JK et al (2001) p16(INK4a) and histology-specific methylation of CpG islands by exposure to tobacco smoke in non-small cell lung cancer. Cancer Res 61:3419–3424
Guo S, Tan L, Pu W et al (2014) Quantitative assessment of the diagnostic role of APC promoter methylation in non-small cell lung cancer. Clin Epigenetics 6:5. doi:10.1186/1868-7083-6-5
Usadel H, Brabender J, Danenberg KD et al (2002) Quantitative adenomatous polyposis coli promoter methylation analysis in tumor tissue, serum, and plasma DNA of patients with lung cancer. Cancer Res 62:371–375
Toyooka S, Suzuki M, Maruyama R et al (2004) The relationship between aberrant methylation and survival in non-small-cell lung cancers. Br J Cancer 91:771–774. doi:10.1038/sj.bjc.6602013
Wang J, Lee JJ, Wang L et al (2004) Value of p16INK4a and RASSF1A promoter hypermethylation in prognosis of patients with resectable non-small cell lung cancer. Clin Cancer Res 10:6119–6125. doi:10.1158/1078-0432.CCR-04-0652
Brabender J, Usadel H, Danenberg KD et al (2001) Adenomatous polyposis coli gene promoter hypermethylation in non-small cell lung cancer is associated with survival. Oncogene 20:3528–3532. doi:10.1038/sj.onc.1204455
Drilon A, Sugita H, Sima CS et al (2014) A prospective study of tumor suppressor gene methylation as a prognostic biomarker in surgically resected stage I to IIIA non-small-cell lung cancers. J Thorac Oncol 9:1272–1277. doi:10.1097/JTO.0000000000000256
Esteller M, Sanchez-Cespedes M, Rosell R et al (1999) Detection of aberrant promoter hypermethylation of tumor suppressor genes in serum DNA from non-small cell lung cancer patients. Cancer Res 59:67–70
Laird PW (2003) The power and the promise of DNA methylation markers. Nat Rev Cancer 3:253–266. doi:10.1038/nrc1045
Begum S, Brait M, Dasgupta S et al (2011) An epigenetic marker panel for detection of lung cancer using cell-free serum DNA. Clin Cancer Res 17:4494–4503. doi:10.1158/1078-0432.CCR-10-3436
Hubers AJ, Prinsen CFM, Sozzi G et al (2013) Molecular sputum analysis for the diagnosis of lung cancer. Br J Cancer 109:530–537. doi:10.1038/bjc.2013.393
Hubers AJ, Heideman DAM, Burgers SA et al (2015) DNA hypermethylation analysis in sputum for the diagnosis of lung cancer: training validation set approach. Br J Cancer 112:1105–1113. doi:10.1038/bjc.2014.636
Acknowledgments
We thank Michael Maudsley for providing an outline for this manuscript and support in editing and journal styling. This work has been supported by Fondo de Investigación Sanitaria 09/01612, Sociedad Española de Neumología y Cirugía Torácica (SEPAR), Fundació Catalana de Pneumologia (FUCAP) and Centro de Investigación Biomédica en Red de Enfermedades Respiratorias (CIBERES). CIBERES is an initiative of Instituto de Salud Carlos III.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Millares, L., Serra, M., Andreo, F. et al. Assessment of methylation status of locoregional lymph nodes in lung cancer using EBUS-NA. Clin Exp Metastasis 32, 637–646 (2015). https://doi.org/10.1007/s10585-015-9733-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-015-9733-2