Abstract
Purpose
Various aspects of diet, including specific food items and nutrients, have been shown to modulate inflammation and have been implicated in the etiology of prostate cancer (PrCA). No study examining the role of diet-associated inflammation in PrCA has been conducted in Latin America.
Method
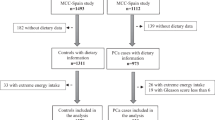
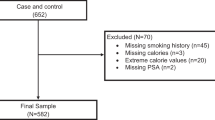
We examined the association between the Dietary Inflammatory Index (DII®) and PrCA in a population-based case–control study in Córdoba, Argentina. A total of 153 incident cases of PrCA and 309 controls frequency matched on sex, age (± 5 years), and place of residence were recruited from 2008 to 2015. The DII was developed to determine the inflammatory potential of individuals’ diets and was computed from a validated food frequency questionnaire using nutrient data from diet only. Multi-level logistic regression models were fit to evaluate the association between DII scores and PrCA, adjusting for age, body mass index, energy intake, and occupational exposure as first-level covariates and family history of prostate cancer as the second-level variable. Odds ratios were estimated in all subject and stratified by BMI (< 30 vs. ≥ 30 kg/m2).
Results
Men in the most pro-inflammatory group (tertile 3) had 50% higher odds of having PrCA compared to men in the most anti-inflammatory group (tertile 1) (ORtertile3 vs. tertile1 1.50; 95% CI 1.24–1.80). The odds of prostate cancer were higher in obese men (n = 109, ORtertile3 vs. tertile1 1.81; 95% CI 1.45–2.27), while no association was found among non-obese men (n = 375, ORtertile3 vs. tertile1 0.93; 95% CI 0.25–3.51).
Conclusions
A pro-inflammatory diet, reflected by higher DII scores, was positively associated with PrCA occurrence. Based on these results and those from other studies, steps should be taken to promote a diet rich in anti-inflammatory foods, in order to reduce risk of PrCA and other chronic diseases. Future studies should explore this association in a prospective setting.

Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61(2):69–90. https://doi.org/10.3322/caac.20107
Ferlay JSI, Ervik M, Dikshit R, Eser S, Mathers C et al (2013) GLOBOCAN 2012 v1.0, cancer incidence and mortality worldwide: IARC Cancer Base No. 11. Lyon. http://globocan.iarc.fr. Accessed June 2016
Diaz Mdel P, Osella AR, Aballay LR, Munoz SE, Lantieri MJ, Butinof M, Paz RM, Pou S, Eynard AR, La Vecchia C (2009) Cancer incidence pattern in Cordoba, Argentina. Eur J Cancer Prev 18(4):259–266. https://doi.org/10.1097/CEJ.0b013e3283152030
Coussens LM, Werb Z (2002) Inflammation and cancer. Nature 420(6917):860–867
Philip M, Rowley DA, Schreiber H (2004) Inflammation as a tumor promoter in cancer induction. Semin Cancer Biol 14(6):433–439
Keibel A, Singh V, Sharma MC (2009) Inflammation, microenvironment, and the immune system in cancer progression. Curr Pharm Des 15(17):1949–1955
Kopp TI, Friis S, Christensen J, Tjonneland A, Vogel U (2013) Polymorphisms in genes related to inflammation, NSAID use, and the risk of prostate cancer among Danish men. Cancer Genet 20(13):00084–00087
Cross AJ, Peters U, Kirsh VA, Andriole GL, Reding D, Hayes RB, Sinha R (2005) A prospective study of meat and meat mutagens and prostate cancer risk. Cancer Res 65(24):11779–11784
Nakai Y, Nonomura N (2013) Inflammation and prostate carcinogenesis. Int J Urol 20(2):150–160
De Nunzio C, Kramer G, Marberger M, Montironi R, Nelson W, Schroder F, Sciarra A, Tubaro A (2011) The controversial relationship between benign prostatic hyperplasia and prostate cancer: the role of inflammation. Eur Urol 60(1):106–117. https://doi.org/10.1016/j.eururo.2011.03.055
Guo YZ, Pan L, Du CJ, Ren DQ, Xie XM (2013) Association between C-reactive protein and risk of cancer: a meta-analysis of prospective cohort studies. Asian Pac J Cancer Prev 14(1):243–248
Toriola AT, Laukkanen JA, Kurl S, Nyyssonen K, Ronkainen K, Kauhanen J (2013) Prediagnostic circulating markers of inflammation and risk of prostate cancer. Int J Cancer 133(12):2961–2967. https://doi.org/10.1002/ijc.28313
Kaaks R, Lukanova A (2001) Energy balance and cancer: the role of insulin and insulin-like growth factor-I. Proc Nutr Soc 60(1):91–106
de Mello VD, Schwab U, Kolehmainen M, Koenig W, Siloaho M, Poutanen K, Mykkanen H, Uusitupa M (2011) A diet high in fatty fish, bilberries and wholegrain products improves markers of endothelial function and inflammation in individuals with impaired glucose metabolism in a randomised controlled trial: the Sysdimet study. Diabetologia 54(11):2755–2767
Khoo J, Piantadosi C, Duncan R, Worthley SG, Jenkins A, Noakes M, Worthley MI, Lange K, Wittert GA (2011) Comparing effects of a low-energy diet and a high-protein low-fat diet on sexual and endothelial function, urinary tract symptoms, and inflammation in obese diabetic men. J Sex Med 8(10):2868–2875
Luciano M, Mottus R, Starr JM, McNeill G, Jia X, Craig LC, Deary IJ (2012) Depressive symptoms and diet: their effects on prospective inflammation levels in the elderly. Brain Behav Immun 26(5):717–720
Michaud DS, Fuchs CS, Liu S, Willett WC, Colditz GA, Giovannucci E (2005) Dietary glycemic load, carbohydrate, sugar, and colorectal cancer risk in men and women. Cancer Epidemiol Biomarkers Prev 14(1):138–147
Lin PH, Aronson W, Freedland SJ (2015) Nutrition, dietary interventions and prostate cancer: the latest evidence. BMC Med 13:3. https://doi.org/10.1186/s12916-014-0234-y
Labbe DP, Zadra G, Ebot EM, Mucci LA, Kantoff PW, Loda M, Brown M (2015) Role of diet in prostate cancer: the epigenetic link. Oncogene 34(36):4683–4691. https://doi.org/10.1038/onc.2014.422
Patel VH (2014) Nutrition and prostate cancer: an overview. Exp Rev Anticancer Ther 14(11):1295–1304. https://doi.org/10.1586/14737140.2014.972946
Second expert report food, nutrition, physical activity and the prevention of cancer: a global perspective (2007) http://www.dietandcancerreport.org/cancer_resource_center/downloads/Second_Expert_Report_full.pdf. World Cancer Research Fund/American Institute for Cancer Research
Shivappa N, Steck SE, Hurley TG, Hussey JR, Hebert JR (2014) Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr 17(8):1689–1696. https://doi.org/10.1017/S1368980013002115
Shivappa N, Steck SE, Hurley TG, Hussey JR, Ma Y, Ockene IS, Tabung F, Hebert JR (2014) A population-based dietary inflammatory index predicts levels of C-reactive protein in the Seasonal Variation of Blood Cholesterol Study (SEASONS). Public Health Nutr 17(8):1825–1833. https://doi.org/10.1017/S1368980013002565
Wirth MD, Burch J, Shivappa N, Violanti JM, Burchfiel CM, Fekedulegn D, Andrew ME, Hartley TA, Miller DB, Mnatsakanova A, Charles LE, Steck SE, Hurley TG, Vena JE, Hebert JR (2014) Association of a dietary inflammatory index with inflammatory indices and metabolic syndrome among police officers. J Occup Environ Med 56(9):986–989
Wood L, Shivappa N, Berthon BS, Gibson PG, Hebert JR (2014) Dietary inflammatory index is related to asthma risk, lung function and systemic inflammation in asthma. Clin Exp Allergy. https://doi.org/10.1111/cea.12323
Tabung FK, Steck SE, Zhang J, Ma Y, Liese AD, Agalliu I, Hingle M, Hou L, Hurley TG, Jiao L, Martin LW, Millen AE, Park HL, Rosal MC, Shikany JM, Shivappa N, Ockene JK, Hebert JR (2015) Construct validation of the dietary inflammatory index among postmenopausal women. Ann Epidemiol 25(6):398–405. https://doi.org/10.1016/j.annepidem.2015.03.009
Vahid F, Shivappa N, Faghfoori Z, Khodabakhshi A, Zayeri F, Hebert JR, Davoodi SH (2018) Validation of a dietary inflammatory index (DII) and association with risk of gastric cancer: a case-control study. Asian Pac J Cancer Prev 19(6):1471–1477. https://doi.org/10.22034/APJCP.2018.19.6.1471
Vahid F, Shivappa N, Hekmatdoost A, Hebert JR, Davoodi SH, Sadeghi M (2017) Association between maternal dietary inflammatory index (DII) and abortion in Iranian women and validation of DII with serum concentration of inflammatory factors: case-control study. Appl Physiol Nutr Metab 42(5):511–516. https://doi.org/10.1139/apnm-2016-0274
Shivappa N, Hebert JR, Rietzschel ER, De Buyzere ML, Langlois M, Debruyne E, Marcos A, Huybrechts I (2015) Associations between dietary inflammatory index and inflammatory markers in the Asklepios Study. Br J Nutr 113(4):665–671. https://doi.org/10.1017/S000711451400395X
Wirth MD, Burch J, Shivappa N, Steck SE, Hurley TG, Vena JE, Hebert JR (2014) Dietary inflammatory index scores differ by shift work status: NHANES 2005 to 2010. J Occup Environ Med 56(2):145–148. https://doi.org/10.1097/JOM.0000000000000088
Shivappa N, Godos J, Hebert JR, Wirth MD, Piuri G, Speciani AF, Grosso G (2018) Dietary inflammatory index and cardiovascular risk and mortality—a meta-analysis. Nutrients. https://doi.org/10.3390/nu10020200
Tabung FK, Steck SE, Ma Y, Liese AD, Zhang J, Caan B, Hou L, Johnson KC, Mossavar-Rahmani Y, Shivappa N, Wactawski-Wende J, Ockene JK, Hebert JR (2015) The association between dietary inflammatory index and risk of colorectal cancer among postmenopausal women: results from the Women’s Health Initiative. Cancer Causes Control 26(3):399–408. https://doi.org/10.1007/s10552-014-0515-y
Wirth MD, Shivappa N, Steck SE, Hurley TG, Hebert JR (2015) The dietary inflammatory index is associated with colorectal cancer in the National Institutes of Health-American Association of Retired Persons Diet and Health Study. Br J Nutr 113(11):1819–1827. https://doi.org/10.1017/S000711451500104X
Shivappa N, Godos J, Hebert JR, Wirth MD, Piuri G, Speciani AF, Grosso G (2017) Dietary inflammatory index and colorectal cancer risk—a meta-analysis. Nutrients. https://doi.org/10.3390/nu9091043
Shivappa N, Hebert JR, Ferraroni M, La Vecchia C, Rossi M (2016) Association between dietary inflammatory index and gastric cancer risk in an Italian case-control study. Nutr Cancer 68(8):1262–1268. https://doi.org/10.1080/01635581.2016.1224367
Shivappa N, Bosetti C, Zucchetto A, Serraino D, La Vecchia C, Hebert JR (2014) Dietary inflammatory index and risk of pancreatic cancer in an Italian case-control study. Br J Nutr. https://doi.org/10.1017/S0007114514003626
Niclis C, Roman MD, Osella AR, Eynard AR, Diaz Mdel P (2015) Traditional dietary pattern increases risk of prostate cancer in Argentina: results of a multilevel modeling and bias analysis from a case-control study. J Cancer Epidemiol 2015:179562. https://doi.org/10.1155/2015/179562
Shivappa N, Bosetti C, Zucchetto A, Montella M, Serraino D, La Vecchia C, Hebert JR (2015) Association between dietary inflammatory index and prostate cancer among Italian men. Br J Nutr 113(2):278–283. https://doi.org/10.1017/S0007114514003572
Shivappa N, Jackson MD, Bennett F, Hebert JR (2015) Increased dietary inflammatory index (DII) is associated with increased risk of prostate cancer in Jamaican men. Nutr Cancer 67(6):941–948. https://doi.org/10.1080/01635581.2015.1062117
Shivappa N, Hebert JR, Askari F, Kardoust Parizi M, Rashidkhani B (2017) Increased inflammatory potential of diet is associated with increased risk of prostate cancer in Iranian men. Int J Vitam Nutr Res. https://doi.org/10.1024/0300-9831/a000395
Vazquez-Salas RA, Shivappa N, Galvan-Portillo M, Lopez-Carrillo L, Hebert JR, Torres-Sanchez L (2016) Dietary inflammatory index and prostate cancer risk in a case-control study in Mexico. Br J Nutr 116(11):1945–1953. https://doi.org/10.1017/S0007114516003986
Graffouillere L, Deschasaux M, Mariotti F, Neufcourt L, Shivappa N, Hebert JR, Wirth MD, Latino-Martel P, Hercberg S, Galan P, Julia C, Kesse-Guyot E, Touvier M (2016) The dietary inflammatory index is associated with prostate cancer risk in French middle-aged adults in a prospective study. J Nutr. https://doi.org/10.3945/jn.115.225623
Shivappa N, Miao Q, Walker M, Hebert J, Aronson K Association between a dietary inflammatory index and prostate cancer risk in Ontario, Canada. Nutr Cancer. https://doi.org/10.1080/01635581.2017.1339095
Shivappa N, Jalilpiran JRH, Faghih YS (2018) Association between dietary inflammatory index and prostate cancer in Shiraz Province of Iran. Asian Pac J Cancer Prev 19(2):415–420. https://doi.org/10.22034/APJCP.2018.19.2.415
Bermudez OI, Tucker KL (2003) Trends in dietary patterns of Latin American populations. Cadernos de saude publica 19(Suppl 1):S87–S99
Niclis C, Diaz Mdel P, Eynard AR, Roman MD, La Vecchia C (2012) Dietary habits and prostate cancer prevention: a review of observational studies by focusing on South America. Nutr Cancer 64(1):23–33. https://doi.org/10.1080/01635581.2012.630163
Navarro A, Munoz SE, Lantieri MJ, del Pilar Diaz M, Cristaldo PE, de Fabro SP, Eynard AR (2004) Meat cooking habits and risk of colorectal cancer in Cordoba. Argent Nutr 20(10):873–877. https://doi.org/10.1016/j.nut.2004.06.008
Navarro A, Osella A, Guerra V, Muñoz S, Lantieri M, Eynard A (2001) Reproducibility and validity of a food-frequency questionnaire in assessing dietary intakes and food habits in epidemiological cancer studies in Argentina. J Exp Clin Cancer Res CR 20(3):365–370
Navarro A, Cristaldo P, Diaz M, Eynard A (1999) Food photography atlas: its suitability for quantifying food and nutrient consumption in nutritional epidemiological research in Cordoba, Argentina. Revista de la Facultad de Ciencias Medicas (Cordoba, Argentina) 57(1):67–74
IPAQ Group (2012) International Physical Activity Questionnaire. http://www.ipaq.ki.se
Niclis C, Pou SA, Shivappa N, Hebert JR, Steck SE, Diaz MDP (2018) Proinflammatory dietary intake is associated with increased risk of colorectal cancer: results of a case-control study in Argentina using a multilevel modeling approach. Nutr Cancer 70(1):61–68. https://doi.org/10.1080/01635581.2018.1397710
Cao Y, Giovannucci E (2016) Obesity and prostate cancer. Recent results in cancer research. Fortschritte der Krebsforschung Progres dans les recherches sur le cancer 208:137–153. https://doi.org/10.1007/978-3-319-42542-9_8
Divella R, De Luca R, Abbate I, Naglieri E, Daniele A (2016) Obesity and cancer: the role of adipose tissue and adipo-cytokines-induced chronic inflammation. J Cancer 7(15):2346–2359. https://doi.org/10.7150/jca.16884
Jackson M, Tulloch-Reid M, Walker S, McFarlane-Anderson N, Bennett F, Francis D, Coard K (2013) Dietary patterns as predictors of prostate cancer in Jamaican men. Nutr Cancer 65(3):367–374
Bosire C, Stampfer MJ, Subar AF, Park Y, Kirkpatrick SI, Chiuve SE, Hollenbeck AR, Reedy J (2013) Index-based dietary patterns and the risk of prostate cancer in the NIH-AARP diet and health study. Am J Epidemiol 177(6):504–513. https://doi.org/10.1093/aje/kws261
Esmaillzadeh A, Kimiagar M, Mehrabi Y, Azadbakht L, Hu FB, Willett WC (2007) Dietary patterns and markers of systemic inflammation among Iranian women. J Nutr 137(4):992–998
Festa A, D’Agostino R, Howard G, Mykkänen L, Tracy RP, Haffner SM (2000) Chronic subclinical inflammation as part of the insulin resistance syndrome: the Insulin Resistance Atherosclerosis Study (IRAS). Circulation 102(1):42–47. https://doi.org/10.1161/01.cir.102.1.42
Whittemore AS, Kolonel LN, Wu AH, John EM, Gallagher RP, Howe GR, Burch JD, Hankin J, Dreon DM, West DW et al (1995) Prostate cancer in relation to diet, physical activity, and body size in blacks, whites, and Asians in the United States and Canada. J Natl Cancer Inst 87(9):652–661
Gronberg H (2003) Prostate cancer epidemiology. Lancet 361(9360):859–864. https://doi.org/10.1016/S0140-6736(03)12713-4
Merlo J (2003) Multilevel analytical approaches in social epidemiology: measures of health variation compared with traditional measures of association. J Epidemiol Commun Health 57(8):550–552
Shivappa N, Prizment AE, Blair CK, Jacobs DR Jr, Steck SE, Hebert JR (2014) Dietary inflammatory index and risk of colorectal cancer in the Iowa Women’s Health Study. Cancer Epidemiol Biomarkers Prev 23(11):2383–2392. https://doi.org/10.1158/1055-9965.EPI-14-0537
Peres LC, Bandera EV, Qin B, Guertin KA, Shivappa N, Hebert JR, Abbott SE, Alberg AJ, Barnholtz-Sloan J, Bondy M, Cote ML, Funkhouser E, Moorman PG, Peters ES, Schwartz AG, Terry PD, Camacho F, Wang F, Schildkraut JM (2017) Dietary inflammatory index and risk of epithelial ovarian cancer in African American women. Int J Cancer 140(3):535–543. https://doi.org/10.1002/ijc.30467
Zheng J, Tabung FK, Zhang J, Liese AD, Shivappa N, Ockene JK, Caan B, Kroenke CH, Hebert JR, Steck SE (2018) Association between post-cancer diagnosis dietary inflammatory potential and mortality among invasive breast cancer survivors in the Women’s Health Initiative. Cancer Epidemiol Biomarkers Prev 27(4):454–463. https://doi.org/10.1158/1055-9965.EPI-17-0569
Breslow NE, Day NE (1987) Statistical methods in cancer research, the design and analysis of cohort studies, vol 2. IARC Scientific Publications, Lyon, p 82
Lopez Fontana CM, Recalde Rincon GM, Messina Lombino D, Uvilla Recupero AL, Perez Elizalde RF, Lopez Laur JD (2009) [Body mass index and diet affect prostate cancer development]. Actas urologicas espanolas 33(7):741–746
Messina D, Perez Elizalde R, Soto C, Uvilla A, Lopez Laur JD, Lopez Fontana C (2012) High intake of lycopene together with low intake of red meat increases the total antioxidant status. Archivos latinoamericanos de nutricion 62(1):15–22
Vykhovanets EV, Shankar E, Vykhovanets OV, Shukla S, Gupta S (2011) High-fat diet increases NF-kappaB signaling in the prostate of reporter mice. Prostate 71(2):147–156
Pandey M, Gupta S (2009) Green tea and prostate cancer: from bench to clinic. Front Biosci (Elite Ed) 1:13–25
Acknowledgments
We are grateful to all field investigators, staffs, and participants of the present study. Drs. Shivappa and Hébert were supported by Grant Number R44DK103377 from the United States National Institute of Diabetes and Digestive and Kidney Diseases. Also, we would like to thank the Science and Technology National Agency, FONCyT Grant PICT 2012-1019 for financial support of this study in Argentina and the National Scientific and Technical Research Council (CONICET) for CN, JBC, and MDR fellowships.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. James R. Hébert owns controlling interest in Connecting Health Innovations LLC (CHI), a company planning to license the right to his invention of the DII® from the University of South Carolina in order to develop computer and smart phone applications for patient counseling and dietary intervention in clinical settings. Dr Nitin Shivappa is an employee of CHI.
Rights and permissions
About this article
Cite this article
Shivappa, N., Niclis, C., Coquet, J.B. et al. Increased inflammatory potential of diet is associated with increased odds of prostate cancer in Argentinian men. Cancer Causes Control 29, 803–813 (2018). https://doi.org/10.1007/s10552-018-1056-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-018-1056-6