Abstract
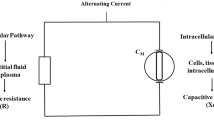
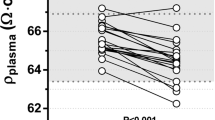
Bio-electrical impedance analysis (BIA) is frequently used to assess body composition in man. Its accuracy in patients is limited, possibly because the employed algorithms are based on the assumption that total body electrical resistance (TBER) is exclusively related to body water volume, and that variation in fluid composition and its effect on fluid resistivity can be ignored. This may introduce substantial calculation errors. The aim of this study was to develop an objective method to assess plasma resistivity (ρplasma) based on measurements by a conductivity probe, as a surrogate for extracellular fluid resistivity (ρe). Sample measurements were standardized at body temperature. Analytical variation was 0.6% within runs and 0.9% between runs. The critical difference, i.e. the smallest difference needed to consider changes within individuals significant, was 1.8% for measurements within runs and 4.3% for measurements between runs. The normal range was defined by a mean ± SD of 66.9 ± 1.8 Ω cm. Multiple regression demonstrated that ρplasma was inversely related to plasma sodium and chloride concentrations, and positively related to total protein (overall R2 = 0.92, p < 0.001). In conclusion, ρplasma measurements were sufficiently robust to be useful as a tool to examine and improve the validity of BIA in clinical settings.



Similar content being viewed by others
References
Bhattacharya, C. A simple method of resolution of a distribution into Gaussian components. Biometrics 23:115–135, 1967.
Boron, W. F., and E. L. Boulpaep. Medical Physiology. Amsterdam: Elsevier, 2008.
Donnan, F. G. Theorie der Membrangleichgewichte und Membranpotentiale bei Vorhandensein von nicht dialysierenden Elektrolyten. Ein Beitrag zur physikalisch‐chemischen Physiologie. Z. Elektrochem. Angew. Phys. Chem. 17:572–581, 1911.
Fogh-Andersen, N., B. M. Altura, B. T. Altura, and O. Siggaard-Andersen. Composition of interstitial fluid. Clin. Chem. 41:1522–1525, 1995.
Fraser, C. G. Biological Variation: From Principles to Practice. Washington, DC: American Association for Clinical Chemistry, 2001.
Fuller, H. The electrical impedance of plasma: a laboratory simulation of the effect of changes in chemistry. Ann. Biomed. Eng. 19:123–129, 1991.
Gilanyi, M., C. Ikrenyi, J. Fekete, K. Ikrenyi, and A. Kovach. Ion concentrations in subcutaneous interstitial fluid: measured versus expected values. Am. J. Physiol. Renal Physiol. 255:F513–F519, 1988.
He, B. Modeling & Imaging of Bioelectrical Activity: Principles and Applications. Boston: Springer, 2010.
Kyle, U. G., I. Bosaeus, A. D. De Lorenzo, P. Deurenberg, M. Elia, J. M. Gómez, B. L. Heitmann, L. Kent-Smith, J.-C. Melchior, and M. Pirlich. Bioelectrical impedance analysis—Part I: Review of principles and methods. Clin. Nutr. 23:1226–1243, 2004.
Lukaski, H. C., and W. A. Siders. Validity and accuracy of regional bioelectrical impedance devices to determine whole-body fatness. Nutrition 19:851–857, 2003.
Malbrain, M. L., J. Huygh, W. Dabrowski, J. J. De Waele, A. Staelens, and J. Wauters. The use of bio-electrical impedance analysis (BIA) to guide fluid management, resuscitation and deresuscitation in critically ill patients: a bench-to-bedside review. Resuscitation 8:15, 2014.
Miller, R. M., T. L. Chambers, S. P. Burns, and M. P. Godard. Validating InBody® 570 multi-frequency bioelectrical impedance analyzer versus DXA for body fat percentage analysis. Med. Sci. Sports Exerc. 48:991, 2016.
Ricos, C. A. V., F. Cava, J. V. Garcia-Lario, A. Hernandez, and C. V. Jimenez. Desirable Biological Variation Database Specifications. Madison: Westgard QC, 2009.
Scharfetter, H., G. Wirnsberger, H. Holzer, and H. Hutten. Influence of ionic shifts during dialysis on volume estimations with multifrequency impedance analysis. Med. Biol. Eng. Comput. 35:96–102, 1997.
Ward, L. C. Segmental bioelectrical impedance analysis: an update. Curr. Opin. Clin. Nutr. Metab. Care 15:424–429, 2012.
Zoccali, C., U. Moissl, C. Chazot, F. Mallamaci, G. Tripepi, O. Arkossy, P. Wabel, and S. Stuard. Chronic fluid overload and mortality in ESRD. J. Am. Soc. Nephrol. 28:2491–2497, 2017.
Acknowledgments
The authors want to thank Kurt Quarz, Damir Djulbic, and Huub Lievestro for their help with plasma resistivity measurements at the Rijnstate Hospital laboratory. This study was financed by the Radboud-Rijnstate Ph.D. funding.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Joel Stitzel oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schotman, J.M., van Borren, M.M.G.J., Wetzels, J.F.M. et al. Assessment of Plasma Resistivity as a Surrogate for Extracellular Fluid Resistivity: Analytical Performance and Impact of Fluid Composition. Ann Biomed Eng 47, 1463–1469 (2019). https://doi.org/10.1007/s10439-019-02246-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-019-02246-9