Abstract
Background
Although hemorrhagic complications are major complications of percutaneous renal biopsy (PRB), the relationship between procedure volume and morbidity remains unclear for PRB. The present study investigated the impact of hospital volume on the occurrence of hemorrhagic complications after PRB.
Methods
Using large claims-based data in the diagnosis procedure combination database in Japan, we identified inpatients with renal disorders who underwent PRB within 4 days after admission during July to December 2007 to 2010. We assessed patient age, sex, clinical syndromes, hemorrhagic complications and diagnoses, and annual hospital volume of PRB divided into quintiles. Multivariate logistic regression analyses fitted with a generalized estimation equation were performed accounting for within-hospital clustering.
Results
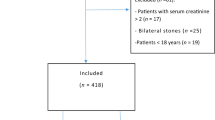
A total of 15,191 patients were identified from 942 hospitals. The overall proportion of hemorrhagic complications was 2.1 %, including diagnoses of hemorrhagic events (1.6 %), red blood cell transfusion (0.5 %), and requiring angiography or endovascular procedure (0.1 %). In-hospital deaths attributable to the complications occurred in 0.06 % of the patients. Patients with rapidly progressive nephritic syndrome (odds ratio 3.41, 95 % confidence interval 2.22–5.25) had significantly higher incidence than those with chronic nephritic syndrome. No significant association was observed between hospital volume and hemorrhagic complications, with odds ratios for the low-intermediate, intermediate, intermediate-high, and high-volume groups relative to the low-volume group of 0.74 (0.43–1.26), 1.19 (0.74–1.92), 1.16 (0.67–2.00), and 1.35 (0.78–2.34), respectively.
Conclusions
No significant relationship was observed between hemorrhagic complication incidence and hospital volume regarding PRB.

Similar content being viewed by others
References
Iversen P, Brun C. Aspiration biopsy of the kidney. Am J Med. 1951;11(3):324–30.
Alwall N. Aspiration biopsy of the kidney, including i.a. a report of a case of amyloidosis diagnosed through aspiration biopsy of the kidney in 1944 and investigated at an autopsy in 1950. Acta Med Scand. 1952;143(6):430–5.
Madaio MP. Renal biopsy. Kidney Int. 1990;38(3):529–43.
Whittier WL, Korbet SM. Timing of complications in percutaneous renal biopsy. J Am Soc Nephrol. 2004;15(1):142–7.
Parrish AE. Complications of percutaneous renal biopsy: a review of 37 years’ experience. Clin Nephrol. 1992;38(3):135–41.
Mendelssohn DC, Cole EH. Outcomes of percutaneous kidney biopsy, including those of solitary native kidneys. Am J Kidney Dis. 1995;26(4):580–5.
Marwah DS, Korbet SM. Timing of complications in percutaneous renal biopsy: what is the optimal period of observation? Am J Kidney Dis. 1996;28(1):47–52.
Khajehdehi P, Junaid SM, Salinas-Madrigal L, Schmitz PG, Bastani B. Percutaneous renal biopsy in the 1990s: safety, value, and implications for early hospital discharge. Am J Kidney Dis. 1999;34(1):92–7.
Shidham GB, Siddiqi N, Beres JA, Logan B, Nagaraja HN, Shidham SG, et al. Clinical risk factors associated with bleeding after native kidney biopsy. Nephrology (Carlton). 2005;10(3):305–10.
Manno C, Strippoli GFM, Arnesano L, Bonifati C, Campobasso N, Gesualdo L, et al. Predictors of bleeding complications in percutaneous ultrasound-guided renal biopsy. Kidney Int. 2004;66(4):1570–7.
Stratta P, Canavese C, Marengo M, Mesiano P, Besso L, Quaglia M, et al. Risk management of renal biopsy: 1387 cases over 30 years in a single centre. Eur J Clin Invest. 2007;37(12):954–63.
Tondel C, Vikse BE, Bostad L, Svarstad E. Safety and complications of percutaneous kidney biopsies in 715 children and 8573 adults in Norway 1988-2010. Clin J Am Soc Nephrol. 2012;7(10):1591–7.
Fish R, Pinney J, Jain P, Addison C, Jones C, Jayawardene S, et al. The incidence of major hemorrhagic complications after renal biopsies in patients with monoclonal gammopathies. Clin J Am Soc Nephrol. 2010;5(11):1977–80.
Alsfasser G, Kittner J, Eisold S, Klar E. Volume–outcome relationship in pancreatic surgery: the situation in Germany. Surgery. 2012;152(3 Suppl 1):S50–5.
Barocas DA, Mitchell R, Chang SS, Cookson MS. Impact of surgeon and hospital volume on outcomes of radical prostatectomy. Urol Oncol. 2010;28(3):243–50.
Miyata H, Motomura N, Ueda Y, Tsukihara H, Tabayashi K, Takamoto S. Toward quality improvement of thoracic aortic surgery: estimating volume–outcome effect from nationwide survey. Eur J Cardiothorac Surg. 2009;36(3):517–21.
Yasunaga H, Matsuyama Y, Ohe K. Effects of hospital and surgeon volumes on operating times, postoperative complications, and length of stay following laparoscopic colectomy. Surg Today. 2009;39(11):955–61.
Yasunaga H, Tsuchiya K, Matsuyama Y, Ohe K. High-volume surgeons in regard to reductions in operating time, blood loss, and postoperative complications for total hip arthroplasty. J Orthop Sci. 2009;14(1):3–9.
Sugihara T, Yasunaga H, Horiguchi H, Nishimatsu H, Kume H, Matsuda S, et al. Impact of hospital volume and laser use on postoperative complications and in-hospital mortality in cases of benign prostate hyperplasia. J Urol. 2011;185(6):2248–53.
Yasunaga H, Horiguchi H, Matsuda S, Fushimi K, Hashimoto H, Ohe K, et al. Relationship between hospital volume and operative mortality for liver resection: data from the Japanese Diagnosis Procedure Combination database. Hepatol Res. 2012;42(11):1073–80.
Yasunaga H, Yanaihara H, Fuji K, Horiguchi H, Hashimoto H, Matsuda S. Impact of hospital volume on postoperative complications and in-hospital mortality after renal surgery: data from the Japanese Diagnosis Procedure Combination Database. Urology. 2010;76(3):548–52.
Sugiyama H, Yokoyama H, Sato H, Saito T, Kohda Y, Nishi S, et al. Japan Renal Biopsy Registry: the first nationwide, web-based, and prospective registry system of renal biopsies in Japan. Clin Exp Nephrol. 2011;15(4):493–503.
Corapi KM, Chen JL, Balk EM, Gordon CE. Bleeding complications of native kidney biopsy: a systematic review and meta-analysis. Am J Kidney Dis. 2012;60(1):62–73.
Hirakata H. Questionnaire-based survey on renal biopsy in Japan. Nihon Jinzo Gakkai Shi. 2003;45(8):731–8.
Panageas KS, Schrag D, Localio AR, Venkatraman ES, Begg CB. Properties of analysis methods that account for clustering in volume–outcome studies when the primary predictor is cluster size. Stat Med. 2007;26(9):2017–35.
Zeger SL, Liang KY. Longitudinal data analysis for discrete and continuous outcomes. Biometrics. 1986;42(1):121–30.
Hirakata H. Indication and contraindication in renal biopsy. Nihon Jinzo Gakkai Shi. 2005;47(2):73–5.
Ross JS, Normand S-LT, Wang Y, Ko DT, Chen J, Drye EE, et al. Hospital volume and 30-day mortality for three common medical conditions. N Engl J Med. 2010;362(12):1110–8.
Acknowledgments
This work was accepted as a poster presentation at Kidney Week 2013, Annual Meeting of the American Society of Nephrology, November 5–10, 2013, Atlanta, GA. This study was supported by Grants-in-Aid for Scientific Research from the Ministry of Health, Labour and Welfare, Japan (H22-Policy-031 and, in part, H22-Policy-033); by a Grant-in-Aid for Scientific Research B (No. 22390131) from the Ministry of Education, Culture, Sports, Science and Technology, Japan; and by the Funding Program for World-Leading Innovative R&D on Science and Technology (FIRST program) from the Council for Science and Technology Policy, Japan (No. 0301002001001).
Conflict of interest
All the authors have declared no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Yamamoto, H., Hashimoto, H., Nakamura, M. et al. Relationship between hospital volume and hemorrhagic complication after percutaneous renal biopsy: results from the Japanese diagnosis procedure combination database. Clin Exp Nephrol 19, 271–277 (2015). https://doi.org/10.1007/s10157-014-0986-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-014-0986-x