Abstract
Background
Parkinson’s disease (PD) is a neurodegenerative disorder characterized by various motor symptoms including balance and gait impairment. Several studies have shown that physiotherapy, cueing techniques, treadmill training, and cognitive movement strategies are useful in improving balance and gait in patients with PD. Devices employing virtual reality (VR) have been shown to be promising in neurorehabilitation as they can provide the patients with multisensory stimulation creating a realistic environment and improve the motivation and the adhesion of patients to the rehabilitation program. This preliminary study is aimed at testing the efficacy and feasibility of gait training based on the computer-assisted virtual reality environment (CAREN) in a sample of PD.
Methods
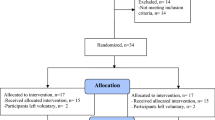
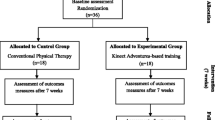
In this preliminary study, 22 outpatients affected by PD who attended the Behavioral and Robotic Neurorehab Laboratory of the IRCCS Neurolesi between August 2017 and October 2018 were enrolled. All PD patients underwent 20 conventional physiotherapy sessions followed by 3-month of rest. Then, the patients were provided with 20 sessions of CAREN training. Gait and balance performances were rated before, after each training protocol, and 3 months later. Gait analysis was also performed before and after CAREN training.
Results
All patients completed both of the rehabilitation trainings without any adverse event. All considered scales improved significantly at the end of both rehabilitation treatments. However, patients presented with a greater clinical improvement after the CAREN training, compared with conventional physiotherapy. In particular, patients walked faster and with more stability, with wider, longer steps.
Conclusions
Even though further neurophysiological details are required to identify the patients who may benefit from CAREN training, our findings suggest that this innovative device is an effective and feasible tool to train balance and gait in patients with PD.




Similar content being viewed by others
References
Shulman LM (2010) Understanding disability in Parkinson's disease. Mov Disord 25(Suppl 1):S131–S135
McNeely ME, Duncan RP, Earhart GM (2012) Medication improves balance and complex gait performance in Parkinson disease. Gait Posture 36(1):144–148
Burleigh-Jacobs A, Horak FB, Nutt JG, Obeso JA (1997) Step initiation in Parkinson's disease: influence of levodopa and external sensory triggers. Mov Disord 12(2):206–215
Wood BH, Bilclough JA, Bowron A, Walker RW (2002) Incidence and prediction of falls in Parkinson's disease: a prospective multidisciplinary study. J Neurol Neurosurg Psychiatry 72(6):721–725
Bloem BR, Hausdorff JM, Visser JE, Giladi N (2004) Falls and freezing of gait in Parkinson's disease: a review of two interconnected, episodic phenomena. Mov Disord 19(8):871–884
Bonnet AM, Loria Y, Saint-Hilaire MH, Lhermitte F, Agid Y (1987) Does long-term aggravation of Parkinson's disease result from nondopaminergic lesions? Neurology. 37(9):1539–1542
Frazzitta G, Bertotti G, Uccellini D, Boveri N, Rovescala R, Pezzoli G, Maestri R (2013) Short- and long-term efficacy of intensive rehabilitation treatment on balance and gait in parkinsonian patients: a preliminary study with a 1-year followup. Parkinsons Dis. 2013:583278
Frazzitta G, Maestri R, Uccellini D, Bertotti G, Abelli P (2009) Rehabilitation treatment of gait in patients with Parkinson's disease with freezing: a comparison between two physical therapy protocols using visual and auditory cues with or without treadmill training. Mov Disord 24(8):1139–1143
Frazzitta G, Maestri R, Bertotti G, Riboldazzi G, Boveri N, Perini M, Uccellini D, Turla M, Comi C, Pezzoli G, Ghilardi MF (2015) Intensive rehabilitation treatment in early Parkinson's disease: a randomized pilot study with a 2-year follow-up. Neurorehabil Neural Repair 29(2):123–131
Papagno C, Trojano L (2018) Cognitive and behavioral disorders in Parkinson's disease: an update. I: cognitive impairments. Neurol Sci 39(2):215–223
Tachibana H (2013) Cognitive impairment in Parkinson's disease. Seishin Shinkeigaku Zasshi 115(11):1142–1149
Maggio MG, Russo M, Cuzzola MF, Destro M, La Rosa G, Molonia F, Bramanti P, Lombardo G, De Luca R, Calabrò RS (2019) Virtual reality in multiple sclerosis rehabilitation: A review on cognitive and motor outcomes. J Clin Neurosci pii:S0967–5868(19)30185–7
Maggio MG, Maresca G, Scarcella I, Latella D, De Domenico C, Destro M, De Luca R, Calabro RS (2019) Virtual reality-based cognitive rehabilitation in progressive supranuclear palsy. Psychogeriatrics. https://doi.org/10.1111/psyg.12431
De Luca R, Portaro S, Le Cause M, De Domenico C, Maggio MG, Cristina Ferrera M, Giuffrè G, Bramanti A, Calabrò RS (2019) Cognitive rehabilitation using immersive virtual reality at young age: a case report on traumatic brain injury. Appl Neuropsychol Child 6:1–6
Albiol-Pérez S, Gil-Gómez JA, Muñoz-Tomás MT, Gil-Gómez H et al (2017) The effect of balance training on postural control in patients with Parkinson's disease using a virtual rehabilitation system. Methods Inf Med 56(2):138–144
Laver KE, George S, Thomas S, Deutsch JE, Crotty M (2015) Virtual reality for stroke rehabilitation. Cochrane Database Syst Rev 12:CD008349
Kalron A, Fonkatz I, Frid L, Baransi H, Achiron A (2016) The effect of balance training on postural control in people with multiple sclerosis using the CAREN virtual reality system: a pilot randomized controlled trial. J Neuroeng Rehabil 13:13
Sessoms PH, Gottshall KR, Collins JD, Markham AE, Service KA, Reini SA (2015) Improvements in gait speed and weight shift of persons with traumatic brain injury and vestibular dysfunction using a virtual reality computer-assisted rehabilitation environment. Mil Med 180(3 Suppl):143–149
Freitag F, Brucki SMD, Barbosa AF, Chen J, Souza CO, Valente DF, Chien HF, Bedeschi C, Voos MC (2019) Is virtual reality beneficial for dual-task gait training in patients with Parkinson's disease? A systematic review. Dement Neuropsychol 13(3):259–267
Cano Porras D, Sharon H, Inzelberg R, Ziv-Ner Y, Zeilig G, Plotnik M (2019) Advanced virtual reality-based rehabilitation of balance and gait in clinical practice. Ther Adv Chronic Dis 10:2040622319868379
Mehrholz J, Kugler J, Storch A, Pohl M, Elsner B, Hirsch K (2015) Treadmill training for patients with Parkinson's disease. Cochrane Database Syst Rev 8:CD007830
Maggio MG, Maresca G, De Luca R, Stagnitti MC, Porcari B, Ferrera MC, Galletti F, Casella C, Manuli A, Calabrò RS (2019) The growing use of virtual reality in cognitive rehabilitation: fact, fake or vision? A Scoping Review. J Natl Med Assoc pii: S0027–9684(18)30346–8
Santos P, Machado T, Santos L, Ribeiro N, Melo A (2019) Efficacy of the Nintendo Wii combination with conventional exercises in the rehabilitation of individuals with Parkinson's disease: a randomized clinical trial. NeuroRehabilitation. https://doi.org/10.3233/NRE-192771
Kastavelis D, Mukherjee M, Decker LM, Stergiou N (2010) The effect of virtual reality on gait variability. Biomech Res Build 14(3):239–256
Zimmerli L, Duschau-Wicke A, Riener R, Mayr A, Lünenburger L (2009) Virtual reality and gait rehabilitation augmented feedback for the Lokomat. Virtual Rehabilitation International Conference:150–153
Doniger GM, Beeri MS, Bahar-Fuchs A et al (2018) Virtual reality-based cognitive-motor training for middle-aged adults at high Alzheimer's disease risk: a randomized controlled trial. Alzheimers Dement (NY) 4:118–129
Cheung KL, Tunik E, Adamovich SV, Boyd LA (2014) Neuroplasticity and virtual reality. In: Keshner E, Levin M (eds) Weiss P. Virtual reality for physical and motor rehabilitation. Virtual Reality Technologies for Health and Clinical Applications, Springer, New York, NY, pp 5–24
Nieuwboer A, Kwakkel G, Rochester L et al (2007) Cueing training in the home improves gait-related mobility in Parkinson's disease: the RESCUE trial. J Neurol Neurosurg Psychiatry 78:134–140
Siegert RJ, Taylor KD, Weatherall M, Abernethy DA (2006) Is implicit sequence learning impaired in Parkinson's disease? A meta-analysis. Neuropsychology 20:490–495
Vakil E, Kahan S, Huberman M, Osimani A (2000) Motor and non-motor sequence learning in patients with basal ganglia lesions: the case of serial reaction time (SRT). Neuropsychologia 38:1–10
Calabrò RS, Naro A, Filoni S, Pullia M, Billeri L, Tomasello P, Portaro S, Di Lorenzo G, Tomaino C, Bramanti P (2019) Walking to your right music: a randomized controlled trial on the novel use of treadmill plus music in Parkinson's disease. J Neuroeng Rehabil. 16(1):68
Allen NE, Schwarzel AK, Canning CG (2013) Recurrent falls in Parkinson's disease: a systematic review. Parkinsons Dis 2013:906274
Bloem BR, Grimbergen YA, Cramer M, Willemsen M, Zwinderman AH (2001) Prospective assessment of falls in Parkinson’s disease. J Neurol 248:950–958
Stolze H, Klebe S, Zechlin C, Baecker C, Friege L, Deuschl G (2004) Falls in frequent neurological diseases--prevalence, risk factors and aetiology. J Neurol 251(1):79–84
Rahman S, Griffin HJ, Quinn NP, Jahanshahi M (2008) Quality of life in Parkinson's disease: the relative importance of the symptoms. Mov Disord 23(10):1428–1434
Koay L, Rose J, Abdelhafiz AH (2018) Factors that lead to hospitalisation in patients with Parkinson disease-a systematic review. Int J Clin Pract 72(1)
Karadsheh MS, Rodriguez EK, Harris MB, Zurakowski D, Lucas R, Weaver MJ (2015) Mortality and revision surgery are increased in patients with Parkinson's disease and fractures of the femoral neck. Clin Orthop Relat Res 473(10):3272–3279
Calabrò RS, De Cola MC, Leo A, Reitano S, Balletta T, Trombetta G, Naro A, Russo M, Bertè F, De Luca R, Bramanti P (2015) Robotic neurorehabilitation in patients with chronic stroke: psychological well-being beyond motor improvement. Int J Rehabil Res 38(3):219–225
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The local Ethics Committee of the IRCCS Centro Neurolesi Bonino Pulejo (Messina, Italy) approved the study.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Calabrò, R.S., Naro, A., Cimino, V. et al. Improving motor performance in Parkinson’s disease: a preliminary study on the promising use of the computer assisted virtual reality environment (CAREN). Neurol Sci 41, 933–941 (2020). https://doi.org/10.1007/s10072-019-04194-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-04194-7