Abstract
Aims
To observe the effects of saxagliptin on the expression of mitogen-activated protein kinase 38 (p38MAPK), nephrin and podocin in renal tissue in type 2 diabetic (T2DM) rats, and to explore the possible mechanism of its renal protection.
Methods
Forty-eight male Sprague–Dawley rats were used for the study and divided into four different groups: normal controls (Group NC), DM controls (Group DM), DM + glibenclamide (Group Su) and DM + saxagliptin (Group Sa). The day drug administration started was defined as week 0. After 12 weeks, hemoglobin A1c (HbA1c), total cholesterol (TC), triglyceride (TG), urea nitrogen (BUN) and creatinine (Cr) in serum were detected, simultaneously albumin and creatinine in urine were measured, respectively, and then urinary albumin/creatinine ratio (UACR) was calculated. The pathological morphology of kidney tissue in different groups was observed, and the expression of nephrin and podocin mRNA and protein in kidney tissue were detected.
Results
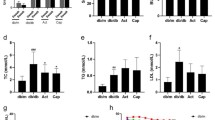
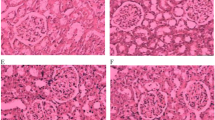
(1) After 12 weeks, FBG and HbA1c in Group Su and Group Sa were significantly lower than those in Group DM (both P < 0.05), while there was no significant difference between Group Su and Group Sa. TC, TG and UACR in Group Sa were significantly decreased than those in Group DM. (2) When compared with Group DM, the kidney weight/body weight ratios, the average width of glomerular basement membrane and foot process fusion ratio were all improved in Group Sa after 12 weeks. (3) The expression of p38MAPK mRNA and protein was significantly decreased, while nephrin and podocin mRNA and protein were significantly higher in Group Sa than those in Group DM after 12 weeks. (4) A significant negative correlation was detected between p38MAPK mRNA and nephrin (r = − 0.421, P = 0.009) and podocin mRNA (r = − 0.570, P = 0.000), respectively.
Conclusions
Saxagliptin can reduce urinary albumin excretion and exert renal protective effect, especially on podocytes in T2DM rats. The mechanism may be related to its inhibition of renal p38MAPK signaling pathway and the increase in the expression of nephrin and podocin in renal tissue, which is independent of its hypoglycemic effect.




Similar content being viewed by others
References
Fechete R, Heinzel A, Perco P et al (2011) Mapping of molecular pathways, biomarkers and drug targets for diabetic nephropathy. Proteomics Clin Appl 5:354–366
Morita M, Uchigata Y, Hanai K et al (2011) Association of urinary type IV collagen with GFR decline in young patients with type 1 diabetes. Am J Kidney Dis 58:915–920
Siu B, Saha J, Smoyer WE et al (2006) Reduction in podocyte density as a pathologic feature in early diabetic nephropathy in rodents: prevention by lipoic acid treatment. BMC Nephrol 15:6
Lian H, Cheng Y, Wu X (2017) TMEM16A exacerbates renal injury by activating P38/JNK signaling pathway to promote podocyte apoptosis in diabetic nephropathy mice. Biochem Biophys Res Commun 487:201–208
Komers R, Lindsley JN, Oyama TT et al (2007) Renal p38 MAP kinase activity in experimental diabetes. Lab Invest 87:548–558
Adhikary L, Chow F, Nikolic-Paterson DJ et al (2004) Abnormal p38 mitogen-activated protein kinase signalling in human and experimental diabetic nephropathy. Diabetologia 47:1210–1222
Gonçalves GL, Costa-Pessoa JM, Thieme K et al (2018) Intracellular albumin overload elicits endoplasmic reticulum stress and PKC-delta/p38 MAPK pathway activation to induce podocyte apoptosis. Sci Rep 8:18012
Duvnjak L, Perković MN, Blaslov K (2017) Dipeptidyl peptidase-4 activity is associated with urine albumin excretion in type 1 diabetes. J Diabetes Complications 31:218–222
Mosenzon O, Leibowitz G, Bhatt DL et al (2017) Effect of Saxagliptin on Renal Outcomes in the SAVOR-TIMI 53 Trial. Diabetes Care 40:69–76
Herman-Edelstein M, Thomas MC, Thallas-Bonke V et al (2011) Dedifferentiation of immortalized human podocytes in response to transforming growth factor-β: a model for diabetic podocytopathy. Diabetes 60:1779–1788
Ziyadeh FN, Wolf G (2008) Pathogenesis of the podocytopathy and proteinuria in diabetic glomerulopathy. Curr Diabet Rev 4:39–45
Welsh GI, Saleem MA (2010) Nephrin-signature molecule of the glomerular podocyte? J Pathol 220:328–337
Denhez B, Geraldes P (2017) Regulation of Nephrin Phosphorylation in Diabetes and Chronic Kidney Injury. Adv Exp Med Biol 966:149–161
Li X, Gao Z, Gao H et al (2017) Nephrin loss is reduced by grape seed proanthocyanidins in the experimental diabetic nephropathy rat model. Mol Med Rep 16:9393–9400
Wadie W, El-Tanbouly DM (2017) Vinpocetine mitigates proteinuria and podocytes injury in a rat model of diabetic nephropathy. Eur J Pharmacol 814:187–195
Acknowledgements
This study was supported by the National Natural Science Foundation of China (81800731) and Local Scientific and Technological Development Project guided by Central Government of China (No: 2017070802D147).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
The study protocol was approved by the Ethics Committee of Anhui provincial hospital, Medical Institution Animal Care and Research Advisory Committee (Hefei, China).
Additional information
Managed by Giuseppe Pugliese.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hu, Y., Ye, S., Xing, Y. et al. Saxagliptin attenuates glomerular podocyte injury by increasing the expression of renal nephrin and podocin in type 2 diabetic rats. Acta Diabetol 57, 279–286 (2020). https://doi.org/10.1007/s00592-019-01421-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-019-01421-7