Abstract
Purpose
The University Hospital of North Norway (UNN) is a tertiary-level hospital and has the main responsibility of providing specialized cancer health care in the remote area of Northern Norway. Weekly videoconferences (VCs) have been established to enable clinicians at a local hospital and primary cancer health care providers in five different communities to discuss cases with specialist cancer care services at UNN. In this study, we aimed to evaluate the feasibility of these VCs.
Methods
This is a prospective registration study. Descriptive data were collected at UNN, and for each patient discussed at the VC, a survey was completed by the local health care provider responsible for the patient.
Results
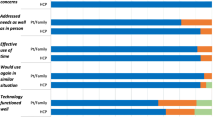
During an 18-month period, 167 cases were discussed (101 patients). A median of 7 health care providers participated in each VC. According to the local physicians and nurses, the VCs contributed in 96% of cases to give “quite a bit” or “very much” confidence in adequate patient care. They reported that patient care in 85% of cases would be improved “quite a bit” or “very much” due to the VC. The mean number of days waiting for VC were 2.0 days (range, 0–7; SD, 2.0) and was significantly shorter (P < 0.001) than the estimated time waiting if alternative consultations were to be used (mean, 10.2 days (range, 0–30; SD, 5.8)).
Conclusion
VC may be a useful supplemental tool to support primary health care providers at local hospitals and remote communities in their effort to offer efficient and high-quality cancer care.
Similar content being viewed by others
References
Cancer Registry of Norway (2009) Cancer in Norway 2008–cancer incidence, mortality, survival and prevalence in Norway. Oslo
Godden DJ (2005) Rural health care in the U.K.: a rapidly changing scene. J Agric Saf Health 11:205–210
Maserat E (2008) Information communication technology: new approach for rural cancer care improvement. Asian Pac J Cancer Prev 9:811–814
Coelho JJ, Arnold A, Nayler J, Tischkowitz M, MacKay J (2005) An assessment of the efficacy of cancer genetic counselling using real-time videoconferencing technology (telemedicine) compared to face-to-face consultations. Eur J Cancer 41:2257–2261
Doorenbos AZ, Kundu A, Eaton LH, et al (2011) Enhancing access to cancer education for rural healthcare providers via Telehealth. J Cancer Educ (in press)
Kitamura C, Zurawel-Balaura L, Wong RK (2010) How effective is video consultation in clinical oncology? A systematic review. Curr Oncol 17:17–27
Doolittle GC, Allen A (1997) Practising oncology via telemedicine. J Telemed Telecare 3:63–70
Allen A, Hayes J (1994) Patient satisfaction with telemedicine in a rural clinic. Am J Public Health 84:1693
Brigden M, Minty A, Pilatzke S, Della VL, Sherrington L, McPhail K (2008) A survey of recipient client physician satisfaction with teleoncology services originating from Thunder Bay Regional Health Sciences Centre. Telemed J E Health 14:250–254
Gagliardi A, Smith A, Goel V, DePetrillo D (2003) Feasibility study of multidisciplinary oncology rounds by videoconference for surgeons in remote locales. BMC Med Inf Decis Mak 3:7
Kidd L, Cayless S, Johnston B, Wengstrom Y (2010) Telehealth in palliative care in the UK: a review of the evidence. J Telemed Telecare 16:394–402
Weinerman B, den DJ, Hughes A, Robertson S (2005) Can subspecialty cancer consultations be delivered to communities using modern technology?–A pilot study. Telemed J E Health 11:608–615
Kunkler IH, Rafferty P, Hill DM, Henry M, Foreman D (1997) Telemedicine. Proved acceptable in pilot study in oncology in Scotland. BMJ 314:521
Olver IN, Selva-Nayagam S (2000) Evaluation of a telemedicine link between Darwin and Adelaide to facilitate cancer management. Telemed J 6:213–218
Norum J, Pedersen S, Stormer J et al (2007) Prioritisation of telemedicine services for large scale implementation in Norway. J Telemed Telecare 13:185–192
Norum J, Grev A, Moen MA, Balteskard L, Holthe K (2003) Information and communication technology (ICT) in oncology. Patients’ and relatives’ experiences and suggestions. Support Care Cancer 11:286–293
Norum J, Bruland OS, Spanne O et al (2005) Telemedicine in radiotherapy: a study exploring remote treatment planning, supervision and economics. J Telemed Telecare 11:245–250
Norum J, Jordhoy MS (2006) A university oncology department and a remote palliative care unit linked together by email and videoconferencing. J Telemed Telecare 12:92–96
Statistics Norway (2011) Estimated population per 1 January 2011 and estimated population growth in 2010. Counties and municipalities. http://www.ssb.no/folkber_en/. Accessed 16 Dec 2010
Andrusyszyn MA, Cragg B, Humbert J (2001) Nurse practitioner preferences for distance education methods related to learning style, course content and achievement. J Nurs Educ 40:163–170
Donnem T, Nordoy T, Ervik B, Jordhoy MS (2006) Centralized inpatient palliative care units in remote areas: an obstacle to future home care? Palliat Med 20:116–117
Acknowledgments
We thank all the study participants who took the time to complete the questionnaires and provided valuable feedback.
Conflict of interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Donnem, T., Ervik, B., Magnussen, K. et al. Bridging the distance: a prospective tele-oncology study in Northern Norway. Support Care Cancer 20, 2097–2103 (2012). https://doi.org/10.1007/s00520-011-1319-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-011-1319-1