Abstract
Background
In adult chronic kidney disease (CKD) patients, there is a positive association between inflammation and progressive renal dysfunction. Higher levels of soluble receptors of tumor necrosis factor (sTNFR) have been related to worst prognosis of adult CKD patients. Therefore, the present study aimed to evaluate soluble TNF receptors in children and adolescents with CKD and to search for an association with clinical and laboratory features.
Methods
Demographic, clinical, anthropometric, and laboratory data were evaluated in 34 pediatric patients with CKD and in 34 healthy sex- and age-matched controls. Blood samples were collected in both groups to measure sTNFR by enzyme-linked immunosorbent assay. The modified Schwartz formula was used to estimate glomerular filtration rate (GFR).
Results
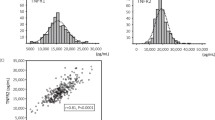
Pediatric patients with CKD had significantly higher plasma concentrations of soluble TNF receptors types 1 and 2 (sTNFR1 and sTNFR2) in comparison to sex- and age-matched healthy controls. Plasma levels of sTNFR1 and sTNFR2 increased progressively as renal function worsened, being inversely and significantly correlated with GFR (r = − 0.853 for sTNFR1 and GFR, r = − 0.729 for sTNFR2 and GFR).
Conclusions
Children and adolescents with CKD exhibited higher plasma levels of sTNFR1 and sTNFR2 than healthy controls, which increased in relation to renal function deterioration. Plasma levels of sTNFR1 and sTNFR2 emerge as markers of progressive CKD in pediatric patients.

Similar content being viewed by others
References
Gohda T, Maruyama S, Kamei N, Yamaguchi S, Shibata T, Murakoshi M, Horikoshi S, Tomino Y, Ohsawa I, Gotoh H, Nojiri S, Suzuki Y (2017) Circulating TNF receptors 1 and 2 predict mortality in patients with end-stage renal disease undergoing dialysis. Sci Rep 7:43520. https://doi.org/10.1038/srep43520
Bae E, Cha RH, Kim YC, An JN, Kim DK, Yoo KD, Lee SM, Kim MH, Park JT, Kang SW, Park JY, Lim CS, Kim YS, Yang SH, Lee JP (2017) Circulating TNF receptors predict cardiovascular disease in patients with chronic kidney disease. Medicine (Baltimore) 96:e6666. https://doi.org/10.1097/MD.0000000000006666
Baker NL, Hunt KJ, Stevens DR, Jarai G, Rosen GD, Klein RL, Virella G, Lopes-Virella MF, DCCT/EDIC Research Group (2018) Association between inflammatory markers and progression to kidney dysfunction: examining different assessment windows in patients with type 1 diabetes. Diabetes Care 41:128–135
Huang YS, Fu SH, Lu KC, Chen JS, Hsieh HY, Sytwu HK, Wu CC (2017) Inhibition of tumor necrosis factor signaling attenuates renal immune cell infiltration in experimental membranous nephropathy. Oncotarget 8:111631–111641. https://doi.org/10.18632/oncotarget.22881
Ortega LM, Fornoni A (2010) Role of cytokines in the pathogenesis of acute and chronic kidney disease, glomerulonephritis, and end-stage kidney disease. Int J Interferon Cytokine Mediat Res 2:49–62
Simões e Silva AC, Pereira AB, Teixeira MM, Teixeira AL (2014) Chemokines as potential markers in pediatric renal diseases. Dis Markers 2014:278715. https://doi.org/10.1155/2014/278715
Yang S, Wang J, Brand DD, Zheng SG (2018) Role of TNF-TNF receptor 2 signal in regulatory T cells and its therapeutic implications. Front Immunol 9:784
Al-Lamki RS, Mayadas TN (2015) TNF receptors: signaling pathways and contribution to renal dysfunction. Kidney Int 87:281–296
Steubl D, Kumar SV, Tato M, Mulay SR, Larsson A, Lind L, Risérus U, Renders L, Heemann U, Carlsson AC, Ärnlöv J, Anders HJ (2017) Circulating cathepsin-S levels correlate with GFR decline and sTNFR1 and sTNFR2 levels in mice and humans. Sci Rep 7:43538. https://doi.org/10.1038/srep43538
Patel M, Oni L, Midgley A, Smith E, Tullus K, Marks SD, Jones CA, Pilkington C, Beresford MW (2016) Increased concentration of plasma TNFR1 and TNFR2 in paediatric lupus nephritis. Lupus 25:1040–1044
Hogg RJ, Furth S, Lemley KV, Portman R, Schwartz GJ, Coresh J, Balk E, Lau J, Levin A, Kausz AT, Eknoyan G, Levey AS, National Kidney Foundation’s Kidney Disease Outcomes Quality Initiative (2003) Clinical practice guidelines for chronic kidney disease in children and adolescents: evaluation, classification, and stratification. Pediatrics 111:1416–1421
Schwartz GJ, Muñoz A, Schneider MF, Mak RH, Kaskel F, Warady BA, Furth SL (2009) New equations to estimate GFR in children with CKD. J Am Soc Nephrol 20:629–637
Kato M, Ayusawa M, Watanabe H, Komori A, Abe Y, Nakamura T, Kamiyama H, Takahashi S (2018) Cardiac function on 3-D speckle tracking imaging and cytokines in Kawasaki disease. Pediatr Int 60:342–348
Narverud I, Ueland T, Nenseter MS, Retterstøl K, Telle-Hansen VH, Halvorsen B, Ose L, Aukrust P, Holven KB (2011) Children with familial hypercholesterolemia are characterized by an inflammatory imbalance between the tumor necrosis factor α system and interleukin-10. Atherosclerosis 214:163–168
Campion CG, Sanchez-Ferras O, Batchu SN (2017) Potential role of serum and urinary biomarkers in diagnosis and prognosis of diabetic nephropathy. Can J Kidney Health Dis 4:2054358117705371. https://doi.org/10.1177/2054358117705371
Funding
This study was partially supported by PRPQ-UFMG (Programa Institucional de Auxílio à Pesquisa de Docentes Recém-Contratados), CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico, Brazil), FAPEMIG (Fundação de Amparo à Pesquisa do Estado de Minas Gerais, Brazil), and CAPES (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior). Dr. A.L. Teixeira and Dr. A.C. Simões e Silva receive a research productivity grant from CNPq.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Moreira, J.M., da Silva, A.N., Marciano Vieira, É.L. et al. Soluble tumor necrosis factor receptors are associated with severity of kidney dysfunction in pediatric chronic kidney disease. Pediatr Nephrol 34, 349–352 (2019). https://doi.org/10.1007/s00467-018-4124-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-018-4124-y