Abstract
Background
Abnormalities of the complement system in Henoch–Schönlein purpura (HSP) have been reported, but how this abnormality in the complement system impacts on the prognosis of HSP remains unknown.
Methods
We retrospectively studied patients hospitalized for HSP in the Children’s Hospital Affiliated to Soochow University between October 2010 and May 2011. Patients with HSP and hypocomplementemia were the cases, and those without hypocomplementemia were the HSP controls. Another group of children (n = 50) with upper respiratory tract infections, but without HSP acted as negative controls.
Results
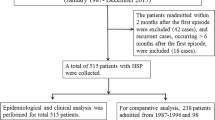
A total number of 338 HSP patients were included in this study (n = 53 cases, n = 285 controls). In the cases, C3 and C4 levels decreased in 29 patients, C3 was low in 6, and C4 in 18. Complement levels returned to normal within 3 months in all HSP patients except one. Case group patients had higher levels of serum IgG and arthralgia, as well as positive titers of antistreptolysin-O. Rates of abdominal pain, gastrointestinal bleeding, Henoch–Schönlein purpura nephritis (HSPN), and serum IgA and IgM levels were similar in the two HSP groups.
Conclusion
Hypocomplementemia associated with HSP is a transient phenomenon. The incidence of significant sequelae such as HSPN between patients with and without hypocomplementemia does not differ.
Similar content being viewed by others
References
Avner ED (2009) Pediatric nephrology, 6th edn. Springer, Berlin, pp 1111–1126
Lau KK, Suzuki H, Novak J, Wyatt RJ (2009) Pathogenesis of Henoch-Schönlein purpura nephritis. Pediatr Nephrol 25:19–26
Garcia-Fuentes M, Martin A, Chantler C, Williams DG (1978) Serum complement components in Henoch-Schonlein purpura. Arch Dis Child 53:417–419
Hisano S, Matsushita M, Fujita T, Iwasaki H (2005) Activation of the lectin complement pathway in Henoch-Schönlein purpura nephritis. Am J Kidney Dis 45:295–302
Motoyama O, Iitaka K (2005) Henoch-Schönlein purpura with hypocomplementemia in children. Pediatr Int 47:39–42
Islek I, Muslu A, Dagdemir A, Dilber C (2001) Is low serum complement 3 in Henoch-Schonlein purpura unusual and of prognostic value? Eur J Pediatr 160:397–398
Krause I, Garty BZ, Davidovits M, Cleper R, Tamary H, Rosenmann E, Eisenstein B (1999) Low serum C3, leukopenia, and thrombocytopenia: unusual features of Henoch-Schonlein purpura. Eur J Pediatr 158:906–909
Rivera F, Anaya S, Pérez-Álvarez J, Sánchez de la Nieta MD, Vozmediano MC, Blanco J (2010) Henoch-Schönlein nephritis associated with streptococcal infection and persistent hypocomplementemia: a case report. J Med Case Report 4:50
Levy M, Broyer M, Arsan A, Levy-Bentolila D, Habib R (1976) Anaphylactoid purpura nephritis in childhood: natural history and immunopathology. Adv Nephrol Necker Hosp 6:183–228
Zhang BL, Wang WH, Fang SY (2001) Clinical analysis of 575 cases with Henoch Schönlein purpura. Chin J Pediatr 39:646–649
Ozen S, Pistorio A, Iusan SM, Bakkaloglu A, Herlin T, Brik R, Buoncompagni A, Lazar C, Bilge I, Uziel Y, Rigante D, Cantarini L, Hilario MO, Silva CA, Alegria M, Norambuena X, Belot A, Berkun Y, Estrella AI, Olivieri AN, Alpigiani MG, Rumba I, Sztajnbok F, Tambic-Bukovac L, Breda L, Al-Mayouf S, Mihaylova D, Chasnyk V, Sengler C, Klein-Gitelman M, Djeddi D, Nuno L, Pruunsild C, Brunner J, Kondi A, Pagava K, Pederzoli S, Martini A, Ruperto N; Paediatric Rheumatology International Trials Organisation (PRINTO) (2010) EULAR/PRINTO/PRES criteria for Henoch–Schönlein purpura, childhood polyarteritis nodosa, childhood Wegener granulomatosis and childhood Takayasu arteritis: Ankara (2008) Part II: final classification criteria. Ann Rheum Dis 69:798–806
McCarthy HJ, Tizard EJ (2010) Diagnosis and management of Henoch–Schönlein purpura. Eur J Pediatr 169:643–650
Ninchoji T, Kaito H, Nozu K, Hashimura Y, Kanda K, Kamioka I, Shima Y, Hamahira K, Nakanishi K, Tanaka R, Yoshikawa N, Iijima K, Matsuo M (2011) Treatment strategies for Henoch-Schönlein purpura nephritis by histological and clinical severity. Pediatr Nephrol 26:563–569
Brogan P, Eleftheriou D, Dillon M (2010) Small vessel vasculitis. Pediatr Nephrol 25:1025–1035
Smith GC, Davidson JE, Hughes DA, Holme E, Beattie TJ (1997) Complement activation in Henoch-Schönlein purpura. Pediatr Nephrol 11:477–480
Chen WF (2005) Medical immunology, 4th edn. People’s Medical Publishing House, Beijing, pp 49–59
Hisano S, Matsushita M, Fujita T, Takeshita M, Iwasaki H (2007) Activation of the lectin complement pathway in post-streptococcal acute glomerulonephritis. Pathol Int 57:351–357
Zhao MH (2009) The roles of complement and complement regulators in the kidney diseases. In: Wang HY, Li XM, Zhao MH, Zhang YK, Wang M, Wang T (eds) Nephrology, 3rd edn. People’s Medical Publishing House, Beijing, pp 712–731
Sjöberg AP, Trouw LA, Blom AM (2009) Complement activation and inhibition: a delicate balance. Trends Immunol 30:83–90
Botto M, Kirschfink M, Macor P, Pickering MC, Wurzner R, Tedesco F (2009) Complement in human diseases: lessons from complement deficiencies. Mol Immunol 46:2774–2783
Garcia-Fuentes M, Chantler C, Williams DG (1977) Cryoglobulinaemia in Henoch–Schönlein purpura. Br Med J 2:163–165
Wang HY (2009) Acute poststreptococcal glomerulonephritis. In: Wang HY, Li XM, Zhao MH, Zhang YK, Wang M, Wang T (eds) Nephrology, 3rd edn. People’s Medical Publishing House, Beijing, pp 961–978
Xia YH, Mao JH, Chen YF, Wang DY, Cao L, Yao SH, Fu HD, Du LZ, Liu AM (2011) Clinical outcomes in children with Henoch–Schönlein purpura nephritis grade IIIa or IIIb. Pediatr Nephrol 26:1083–1088
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents (2004) The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114:555–576
Author information
Authors and Affiliations
Corresponding author
Additional information
Qiang Lin and Yue Min contributed equally to this work and share first authorship
Rights and permissions
About this article
Cite this article
Lin, Q., Min, Y., Li, Y. et al. Henoch–Schönlein purpura with hypocomplementemia. Pediatr Nephrol 27, 801–806 (2012). https://doi.org/10.1007/s00467-011-2070-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-011-2070-z