Abstract
Background
Transumbilical incision has been applied in single-incision laparoscopy. Evidence for the effect of transumbilical incision on postoperative pain compared with infraumbilical incision is still lacking.
Methods
A randomized controlled trial (RCT) was conducted in a university hospital. Patients who underwent conventional laparoscopic cholecystectomy were randomized to have transumbilical or infraumbilical incision. Postoperative pain was measured using visual analog score at 6, 24 h, and 7 days post operation. Secondary outcomes were analgesic usage, length of stay, superficial surgical site infection (SSI), wound numbness, and hypersensitivity. Risk ratio and mean difference (MD) along with their 95% confidence intervals (CIs) were estimated. Adjusted analysis was done, if clinical unbalanced characteristics presented. The study was registered at http://ClinicalTrial.gov (ID NCT02738710).
Results
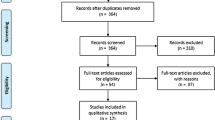
A total of 102 patients were enrolled in which 51 patients were randomized to each interventional group. Postoperative pain was not significantly different between the groups with the MD of − 0.07 (95% CI − 0.47, 0.35). Paracetamol usage was significantly 1 tab (95% CI − 1.9, − 0.1) less after transumbilical incision, but this was not significant after adjusting for unbalanced characteristics. Superficial SSI rate was much higher in the transumbilical than the infraumbilical group, i.e., 16 versus 4%, but this was not significant (p = 0.070). Satisfaction scores at 3 months were not different between the groups, with the corresponding means of 8.9 [standard deviation (SD) 1.3] and 9.0 (SD 1.0).
Conclusions
Transumbilical incision had non-significant different pain compared to infraumbilical incision. Most patients in both groups were satisfied with the operation at 3 months. A further large RCT is required for comparing SSI between the two incisions.

Similar content being viewed by others
References
Lu P, Yang NP, Chang NT, Lai KR, Lin KB, Chan CL (2018) Effect of socioeconomic inequalities on cholecystectomy outcomes: a 10-year population-based analysis. Int J Equity Health 17(1):22. https://doi.org/10.1186/s12939-018-0739-7
Saber AA, Elgamal MH, El-Ghazaly TH, Dewoolkar AV, Akl A (2010) Simple technique for single incision transumbilical laparoscopic appendectomy. Int J Surg (Lond Engl) 8(2):128–130. https://doi.org/10.1016/j.ijsu.2009.12.001
Abdel Azeez T, Mahran KM (2011) Transumbilical laparoscopic cholecystectomy: towards a scarless abdominal surgery. Hepato-gastroenterology 58(106):298–300
Noguera JF, Cuadrado A, Dolz C, Olea JM, Garcia JC (2012) Prospective randomized clinical trial comparing laparoscopic cholecystectomy and hybrid natural orifice transluminal endoscopic surgery (NOTES) (NCT00835250). Surg Endosc 26(12):3435–3441. https://doi.org/10.1007/s00464-012-2359-4
Bucher P, Ostermann S, Pugin F, Morel P (2011) Female population perception of conventional laparoscopy, transumbilical LESS, and transvaginal NOTES for cholecystectomy. Surg Endosc 25(7):2308–2315. https://doi.org/10.1007/s00464-010-1554-4
Bouffard-Cloutier A, Pare A, McFadden N (2017) Periumbilical vs transumbilical laparoscopic incision: a patients’ satisfaction-centered randomised trial. Int J Surg (Lond Engl) 43:86–91. https://doi.org/10.1016/j.ijsu.2017.05.040
Trastulli S, Cirocchi R, Desiderio J, Guarino S, Santoro A, Parisi A, Noya G, Boselli C (2013) Systematic review and meta-analysis of randomized clinical trials comparing single-incision versus conventional laparoscopic cholecystectomy. Br J Surg 100(2):191–208. https://doi.org/10.1002/bjs.8937
Haueter R, Schutz T, Raptis DA, Clavien PA, Zuber M (2017) Meta-analysis of single-port versus conventional laparoscopic cholecystectomy comparing body image and cosmesis. Br J Surg 104(9):1141–1159. https://doi.org/10.1002/bjs.10574
Pan MX, Jiang ZS, Cheng Y, Xu XP, Zhang Z, Qin JS, He GL, Xu TC, Zhou CJ, Liu HY, Gao Y (2013) Single-incision vs three-port laparoscopic cholecystectomy: prospective randomized study. World J Gastroenterol 19(3):394–398. https://doi.org/10.3748/wjg.v19.i3.394
Sinha R, Yadav AS (2014) Transumbilical single incision laparoscopic cholecystectomy with conventional instruments: a continuing study. J Minimal Access Surg 10(4):175–179. https://doi.org/10.4103/0972-9941.141502
Kim HO, Yoo CH, Lee SR, Son BH, Park YL, Shin JH, Kim H, Han WK (2012) Pain after laparoscopic appendectomy: a comparison of transumbilical single-port and conventional laparoscopic surgery. J Korean Surg Soc 82(3):172–178. https://doi.org/10.4174/jkss.2012.82.3.172
Lirici MM, Califano AD, Angelini P, Corcione F (2011) Laparo-endoscopic single site cholecystectomy versus standard laparoscopic cholecystectomy: results of a pilot randomize trial. Am J Surg 202(1):45–52. https://doi.org/10.1016/j.amjsurg.2010.06.019
Horan TC, Andrus M, Dudeck MA (2008) CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control 36(5):309–332. https://doi.org/10.1016/j.ajic.2008.03.002
Kelly AM (1998) Does the clinically significant difference in visual analog scale pain scores vary with gender, age, or cause of pain? Acad Emerg Med Off J Soc Acad Emerg Med 5(11):1086–1090
Kleeff J, Erkan M, Jager C, Menacher M, Gebhardt F, Hartel M (2015) Umbilical microflora, antiseptic skin preparation, and surgical site infection in abdominal surgery. Surg Infect 16(4):450–454. https://doi.org/10.1089/sur.2014.163
Acknowledgements
We would like to thank Dr. Amornpon Kanlerd and Dr. Pakkavuth Chanwangphuvana for helping us to enroll patients and support the study.
Funding
This study was funded by Faculty of Medicine, Thammasat University Hospital with Grant Number of 1-08/2559.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
The study was funded by Faculty of Medicine, Thammasat University with Grant Number of 1-08/2559. Boonying Siribumrungwong,Trirat Chunsirisub, Palin Limpavitayaporn, Assanee Tongyoo, Ekkapak Sriussadaporn, Chatchai Mingmalairak, Weerayut Thowprasert, Ammarin Thakkinstian have no conflict of interests or financial ties to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Siribumrungwong, B., Chunsirisub, T., Limpavitayaporn, P. et al. Comparison of postoperative pain at umbilical wound after conventional laparoscopic cholecystectomy between transumbilical and infraumbilical incisions: a randomized control trial. Surg Endosc 33, 1578–1584 (2019). https://doi.org/10.1007/s00464-018-6447-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6447-y